Chondroplasty is a procedure that involves smoothing degenerative cartilage and reducing unstable cartilage flaps in order to stabilize and treat chondral lesions. Trimming the unstable flaps of a torn meniscus to create a stable remnant meniscus is what a partial meniscectomy entails.
The patient is a 57 year-old woman who has been seen several times for pain on the inner side of her left knee. We had talked about therapy alternatives. Nonsurgical treatment in the form of physical therapy and anti-inflammatory medicines did not benefit the patient. An MRI was performed, which revealed a tear in the medial meniscus as well as suspected involvement of the root of the left knee.
We examined treatment alternatives and decided on surgical intervention. We examined the risks, advantages, and problems, which included infection, hemorrhage, nerve and vascular injury, the need for repeat surgery, the development of arthritis and the necessity for total knee replacement, and the need for rehabilitation, among other things.
The patient is a smoker, and we talked about quitting, especially if we were to make a repair. The patient finds it challenging, but he intends to try to quit smoking. We also talked about systemic concerns such as blood clots, cardiac, pulmonary, and neurological issues. The patient comprehended and signed an informed consent form.
The patient was transported to the operation room and given general anesthesia. The patient was placed on a comfortable operation table. As is customary, the left knee was prepped and draped aseptically. Then 3 grams of Ancef were administered as preoperative antibiotics. A timeout was issued.
The arthroscope was inserted through a lateral parapatellar incision. The superior border of the posterior aspect of the patella was found to have grade 2 osteoarthritic alterations during an examination of the patellofemoral compartment.
The scope was moved to the medial tibiofemoral compartment, where it revealed grade 4 osteoarthritic alterations of the majority of the medial femoral condyle as well as a complicated tear along the body and posterior horn of the medial meniscus.
A spinal needle was used to create a medial entrance hole. The root was found to be intact after a probing examination. The decision was made to debride the patella and meniscus using a shaver and biters. A margin balance was obtained. There was no repair.
Photographs were taken and preserved. The ACL was found to be intact when the intercondylar notch was examined. The lateral tibiofemoral compartment revealed healthy cartilage and meniscus.
The patellofemoral compartment was examined again and revealed grade 2 osteoarthritic alterations in the patella, which were debrided with a shaver. The scope was then placed through the medial entrance portal, and the medial meniscus was rebalanced using a shaver through the lateral portal.
The final photographs were shot and preserved. The knee was irrigated and drained extensively. Closure was accomplished with 3-0 nylon. The knee was then injected with 40 mg of Depo-Medrol combined with 20 mL of Marcaine. In stable condition, the patient was extubated and transported to recovery.
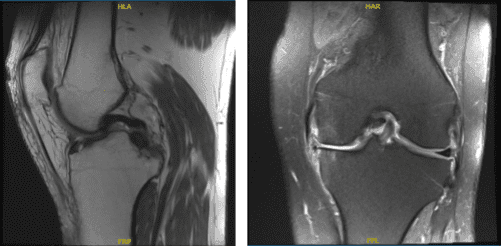
MRI-3T: left knee non-contrast.
After one week the patient is seen in the office for his post-operative visits, although he denies fever, chills and he did not start PT; however, his pain is improving and the Rt Radiculopathy also improved.
We decided to use cautious management for the time being. PT will start. To lessen discomfort and swelling, we will still utilize ice and elevation, and we will keep taking over-the-counter anti-inflammatory medications.
His follow-up 4 weeks later. The patient is still making improvement, albeit slowly, with help of monthly examinations and physical treatment and at home.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


