Through surgery, a shattered bone’s fragments are fixed together in an open reduction and internal fixation (ORIF). The shattered bone is held together by rods, screws, plates, sutures, or other devices.
Choosing whether or not you can treat your injury at home or if you need to visit a doctor is one of the first steps. Visit an orthopedic urgent care center if your wrist is bent unnaturally or your hand is numb. It’s OK to wait to visit a doctor and take care of your wrist at home if you believe it to be sprained.
A 69 year-old patient was in our office with complaints regarding pain and deformity in right wrist. She got a sugar tong splint there and is now in NY. She got the pain due to falling. For aggravating factors, the patient reports pushing/pulling and weight bearing.
For associated symptoms, she reported weakness, swelling, tender to the touch, and pain with motion but reported no numbness, no tingling, no redness, no warmth, no ecchymosis, no catching/locking, no popping/clicking, no buckling, no grinding, no instability, no radiation, no drainage, no fever, no chills, no weight loss, and no change in bowel/bladder habits.
The patient presented an MRI result which contained Colles’ fracture with dorsal angulation.
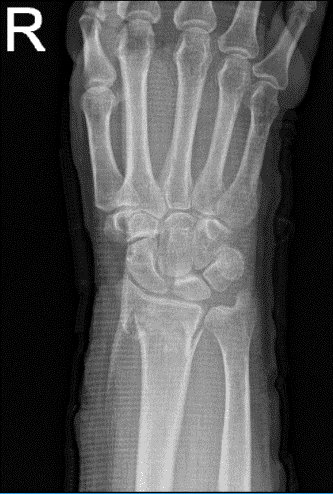
Right wrist X-ray 3 or more views
We discussed the treatment options for the patient’s diagnosis, which included non-surgical and surgical options. We also discussed the nature and purpose of the treatment options along with the expected risks and benefits.
I educated the patient regarding the inherent and unavoidable risks which include, but are not limited to anesthesia, infection, damage to nerves and blood vessels, blood loss, blood clots, and even death were discussed at length.
We also talked about the possibility of not being able to return to prior activities or employment, the need for future surgery, and complex regional pain syndrome. The patient also understands there is a long rehabilitative process that typically follows the surgical procedure.
We talked about the possibility of not being able to alleviate all of the discomfort. Also, I explained there is no guarantee all the function and strength will return. The patient also understands the risks of re-tear or failure to heal. The patient understands implants may be utilized during this surgery.
The patient expressed understanding of these risks and has elected to proceed with surgery. We have discussed the surgical procedure as well as the realistic expectations regarding the risks, outcome and post operative protocol.
The patient was taken to the operating room where general anesthesia was induced. The patient was put on with the right hand over the hand table. The right upper extremity was prepped and draped aseptically in the usual fashion. Tourniquet was applied. Tourniquet time was 58 minutes for the procedure.
A preoperative antibiotic was already given. Incision was given from the flexor carpi radialis tendon. The incision was carried down to the tendon sheath and the anterior sheath of the flexor carpi radialis was cut in the line of the incision. The tendon was reflected medially and also cut.
Pronator quadratus was exposed and cut in line with the incision. Periosteal elevator and Freer were used to elevate the muscle from the distal radius where the fracture site was exposed. The fracture was malreduced.
The fracture reduction was done with manipulation as well as use of the periosteum into the fracture site. Some soft callus as well as bone had to be removed. The fracture site was opened and cleaned with the use of curette. The fracture site was washed thoroughly.
All the pieces were shaved and morselized and mixed with Vitoss to be used later. There was a fracture cavity at the site of fracture. The fracture was reduced and held with the K-wire. The plate was put on the volar surface and held with K-wires and found to be in the acceptable position.
The plate was fixed proximally with the locking screws. Distal locking screw was also done to pull the wound to the plate, finding it in acceptable position. Final fixation of the plate was done with the use of locking screws distally and nonlocking screws proximally.
The nonlocking screw distally was also removed and exchanged with the locking screw. Before the fixation, the Vitoss mixed with bone fragments was packed into the fracture cavity. The wounds were thoroughly irrigated and hemostasis was achieved. Tourniquet was released.
Surgical was used to achieve hemostasis. Closure was done in layers using # 2-0 Vicryl for the subcu and # 3-0 Monocryl for the skin. Dressing was done with the use of Xeroform, 4 x 4, Webril. Short arm splint was applied with the volar and dorsal splints and application of Ace wrap. The patient was extubated and moved to recovery in a stable condition.
The patient was seen for post operative check up. We have decided to do formal physical therapy as well as a home exercise program for rehabilitation of the wrist. Patients regularly followed an office visit every 3-4 weeks.
Patient did well after the surgery and continued physical therapy. Patient checked in for a follow up visit after a month and saw significant improvement on her wrist.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


