Minimal Invasive Spine Surgery (MISS) is a cutting-edge approach to treating spine conditions through smaller incisions and specialized techniques.
This surgery is designed to address a variety of spinal issues while minimizing tissue damage, leading to faster recovery and less postoperative pain compared to traditional surgery. MISS can be performed on both the cervical and lumbar spine using different techniques such as tubular, endoscopic, microscopic, and percutaneous surgery.
How Common It Is and Who Gets It? (Epidemiology)
MISS has become increasingly common due to advancements in technology and its proven benefits in reducing recovery time and surgical complications. Patients who are candidates for this surgery typically have conditions such as herniated discs, spinal stenosis, degenerative disc disease, and fractures. It is particularly beneficial for those looking for quicker recovery, less blood loss, and smaller scars. Individuals with obesity, diabetes, or other chronic conditions may face higher risks, but MISS can still be an option depending on the patient’s health status.
Why It Happens – Causes (Etiology and Pathophysiology)
The primary reasons for spine surgery are degenerative conditions, trauma, or abnormalities that cause nerve compression. Conditions like disc herniation, where the intervertebral disc pushes out and compresses nerve roots, or spinal stenosis, which is the narrowing of the spinal canal, often lead to pain and mobility issues. These conditions can result in symptoms like radiating leg or arm pain, numbness, and weakness, all of which can be addressed through minimally invasive techniques.
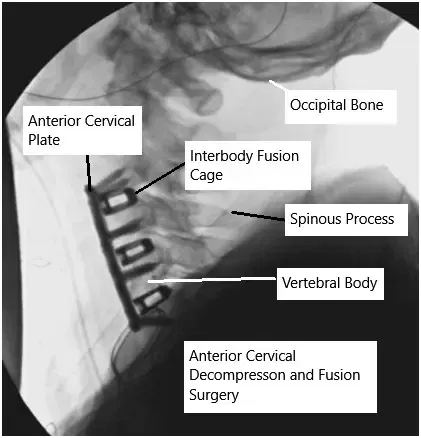
How the Body Part Normally Works? (Relevant Anatomy)
The spine is composed of 33 vertebrae that house and protect the spinal cord. Between the vertebrae are intervertebral discs that act as cushions. Nerves exit the spinal cord through openings between the vertebrae, known as foramen. When these structures are compressed or damaged, it can lead to pain, weakness, or even paralysis. In MISS, the goal is to access the spine with minimal disruption to surrounding tissues such as muscles, ligaments, and nerves.
What You Might Feel – Symptoms (Clinical Presentation)
Patients who may benefit from MISS typically experience symptoms such as chronic back pain, neck pain, leg pain (sciatica), weakness, numbness, and difficulty walking. These symptoms often result from nerve compression or damage in the spine. Patients may also have reduced range of motion, instability, and sometimes difficulty with bowel or bladder control if the nerves involved are impacted.
How Doctors Find the Problem? (Diagnosis and Imaging)
Spine conditions that warrant surgery are usually diagnosed through a combination of patient history, physical examinations, and imaging studies. Common diagnostic tools include X-rays, CT scans, and MRIs, which allow the doctor to visualize the spine’s structure and identify areas of compression, herniation, or other abnormalities. These tests help determine the severity and location of the problem, guiding the surgical approach.
Classification
MISS procedures are categorized by the technique used (e.g., tubular, endoscopic, microscopic). The severity of the spine condition, such as the level of disc herniation or stenosis, also plays a role in classifying the surgery. Each type of MISS surgery has its own set of indications based on the area of the spine affected, the type of surgery required (discectomy, laminectomy, fusion), and the complexity of the case.
Other Problems That Can Feel Similar (Differential Diagnosis)
Conditions such as muscle strain, ligament sprain, osteoarthritis, or peripheral neuropathy can present with symptoms similar to spine conditions like herniated discs or spinal stenosis. A thorough examination, including imaging, is crucial to differentiate between these conditions and ensure proper treatment.
Treatment Options
Non-Surgical Care
Non-surgical treatments for spine conditions include physical therapy, medications (e.g., pain relievers, anti-inflammatories), corticosteroid injections, and lifestyle changes such as weight loss and improved posture. These treatments aim to alleviate pain and improve mobility but may not address the underlying cause in cases of severe degeneration or herniation.
Surgical Care
When conservative treatments fail, surgery is often recommended. MISS allows surgeons to perform complex procedures such as discectomy (removal of a herniated disc), laminectomy (removal of part of the vertebra to relieve pressure), and spinal fusion (joining two or more vertebrae). MISS provides the advantage of smaller incisions, which leads to less muscle dissection and a faster recovery.
Recovery and What to Expect After Treatment
Patients undergoing MISS generally experience a shorter hospital stay, with many being discharged the same day. Recovery times vary depending on the surgery performed, but most patients are able to resume normal activities within a few weeks. Physical therapy may be recommended to improve strength and mobility. Pain management will continue post-surgery, and patients are encouraged to gradually increase their activity levels.
Possible Risks or Side Effects (Complications)
As for all surgeries there are certain but rare risks for anesthesia including cardiac arrest, stroke, paralysis, and rarely death.
- Risks of Spine surgery may include though not limited to:
- Hematoma or hemorrhage
- Damage to the major vessels which may result in excessive bleeding, even death
- Blindness
- Damage to the dura, resulting in a cerebrospinal fluid leak
- Damage to vital structures around the neck
- Failure, loosening or pull out of the cage, graft, rod or screws
- Wound infection
- Failure of fusion to happen
- Damage to the nerve root(s) resulting in new onset or deterioration of preexisting pain, weakness, paralysis, loss of sensation, loss of bowel or bladder function, impaired sexual function, etc., which may or may not recover.
- A few of these conditions may warrant repeat surgery
Certain patient population is at a higher risk for complication which include but are not limited to:
- Smoking
- Seizures
- Obstructive sleep apnea
- Obesity
- High blood pressure
- Diabetes
- Other medical conditions involving your heart, lungs or kidneys
- Medications, such as aspirin, that can increase bleeding
- History of heavy alcohol use
- Drug allergies
- History of adverse reactions to anesthesia
Long-Term Outlook (Prognosis)
The prognosis for patients undergoing MISS is generally positive, especially when the surgery is performed early in the disease process. Most patients experience significant pain relief and improvement in mobility, with a faster return to daily activities than traditional spine surgeries. However, the long-term success of the surgery depends on factors such as the severity of the condition, the patient’s overall health, and adherence to post-operative care.
Out-of-Pocket Costs
Medicare
CPT Code 63030 – Minimally Invasive Lumbar Discectomy (Tubular/Microdiscectomy): $225.06
CPT Code 63020 – Minimally Invasive Cervical Discectomy: $271.49
CPT Code 63040 – Minimally Invasive Thoracic Discectomy: $335.83
CPT Code 63047 – Minimally Invasive Lumbar Laminectomy (Decompression): $271.76
CPT Code 22612 – Minimally Invasive Lumbar Fusion (Posterior/Posterolateral): $382.85
CPT Code 22558 – Minimally Invasive Anterior Lumbar Interbody Fusion (ALIF)/OLIF/XLIF/FFLIF: $368.50
CPT Code 22630 – Minimally Invasive Transforaminal Lumbar Interbody Fusion (TLIF): $387.42
CPT Code 62380 – Endoscopic Lumbar Discectomy (Interlaminar/Transforaminal): $410.41
CPT Code 62287 – Percutaneous Disc Decompression / Nucleoplasty: $137.26
Under Medicare, 80% of the approved cost for these procedures is covered once your annual deductible has been met. The remaining 20% is typically the patient’s responsibility. Supplemental insurance plans—such as Medigap, AARP, or Blue Cross Blue Shield—usually cover this 20%, leaving most patients with little to no out-of-pocket expenses for Medicare-approved spine surgeries. These supplemental plans work directly with Medicare to ensure full coverage for the procedure.
If you have secondary insurance—such as Employer-Based coverage, TRICARE, or Veterans Health Administration (VHA)—it acts as a secondary payer once Medicare processes the claim. After your deductible is satisfied, these secondary plans may cover any remaining balance, including coinsurance or any uncovered charges. Secondary plans typically have a modest deductible, ranging from $100 to $300, depending on the policy and network status.
Workers’ Compensation
If your lumbar, cervical, or thoracic spine condition requiring these procedures is work-related, Workers’ Compensation will fully cover all treatment-related costs, including surgery, hospitalization, and rehabilitation. You will have no out-of-pocket expenses under an accepted Workers’ Compensation claim.
No-Fault Insurance
If your spine injury resulting in one of these procedures was caused by a motor vehicle accident, No-Fault Insurance will cover the full cost of the surgery, including discectomy, fusion, and decompression procedures. The only possible out-of-pocket cost may be a small deductible depending on your individual policy terms.
Example
Tom, a 62-year-old patient with a herniated lumbar disc, underwent minimally invasive lumbar discectomy (CPT 63030) and minimally invasive lumbar fusion (CPT 22612) to stabilize his spine. His estimated Medicare out-of-pocket costs were $225.06 for the discectomy and $382.85 for the fusion. Since Tom had supplemental insurance through AARP Medigap, the 20% not covered by Medicare was fully paid, leaving him with no out-of-pocket expenses for his procedures.
Frequently Asked Questions (FAQ)
Q. What is the recovery time for MISS?
A. Most patients are able to return to normal activities within a few weeks, though full recovery can take several months depending on the complexity of the surgery.
Q. Is MISS less painful than traditional spine surgery?
A. Yes, due to smaller incisions and less tissue disruption, MISS typically results in less pain and a faster recovery than traditional open spine surgery.
Q. Are there any long-term risks?
A. While MISS generally has a good prognosis, there are still risks of complications such as hardware failure, infection, or nerve damage.
Q. Can I return to work after MISS?
A. Many patients can return to work within a few weeks, though those with physically demanding jobs may need a longer recovery period.
Summary and Takeaway
Minimal Invasive Spine Surgery is a safe and effective option for many individuals with spine conditions. It offers the benefits of smaller incisions, faster recovery, and reduced risk of complications. However, it is important to consider the potential risks, costs, and recovery time when deciding whether MISS is the right choice. Patients should consult with their healthcare provider to determine the best treatment plan for their specific condition.
Who Performs This Treatment? (Specialists and Team Involved)
MISS is typically performed by spine surgeons, particularly those who specialize in minimally invasive techniques. The surgical team may also include anesthesiologists, surgical assistants, and nurses trained in spine surgery.
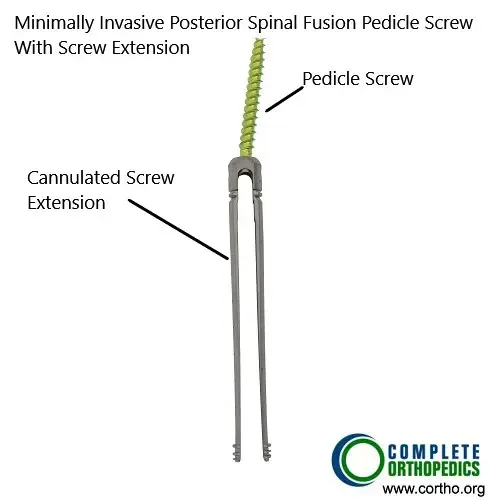
The image shows pedicle screws used in the minimally invasive posterior spinal fusion. The screw extensions aid in the insertion of the screw through key-hole incision.
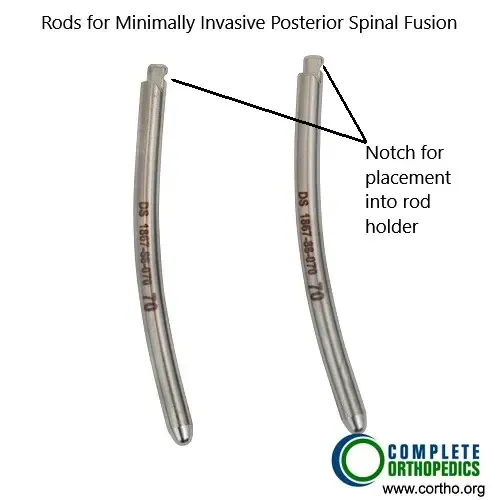
The rods are attached to the pedicle screws for achieving stability across the involved spinal segments. The rods in the image above are designed for minimally invasive posterior spinal fusion.
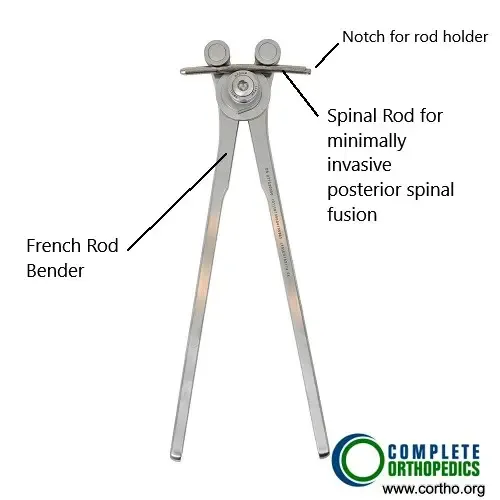
The rod bender in the image above is used to bend and contour the rod for insertion in the slot of the pedicle screws and to achieve maximum stability intra-operatively.
When to See a Specialist?
- temperature more than 101 degrees Fahrenheit
- increased pain or tenderness near the incision
- poor pain relief
- signs of infection: increased swelling, redness, increased drainage, increased warmth, pus, foul smell, bleeding at the incision, incision coming apart
• increased numbness, numbness in genital area - inability to feel or move fingers or toes
- pale blue, white or abnormally cold fingers or toes
- nausea (upset stomach) or vomiting (throwing up) that won’t stop
- increased tiredness
- a generally worse feeling than you had when you left the hospital
- problems urinating, severe constipation or severe diarrhea
- a concern about any other symptoms that seem unusual
When to Go to the Emergency Room?
- Suspected cardiac problem: severe chest pain or pressure, shortness of breath, tightness in chest, pain in left arm, jaw pain, dizziness or fainting, unexplained weakness or fatigue, rapid or irregular pulse, sweating, cool, clammy skin, and/or paleness\
- Suspected Stroke: trouble speaking, changes in vision, confusion or other change in mental status
- \Suspected venous thrombosis: swelling of the legs, ankles, or feet, discomfort, heaviness, pain, aching, throbbing, itching, or warmth in the legs, sudden shortness of breath, chest pain, coughing up blood, rapid or irregular heart rate
- Suspected Sepsis: high grade fever, with shivers associated with fatigue, dizziness, racing heart, pale or discolored skin, sleepy, difficult to rouse, confused, short of breath
• Heavy bleeding from the surgical site - Severe allergic reaction with trouble breathing, swelling, hives
What Recovery Really Looks Like?
Recovery after MISS typically involves limited pain, shorter hospital stays, and a quicker return to daily activities compared to traditional surgeries. Full recovery can take a few months depending on the complexity of the procedure.
What Happens If You Ignore It?
Ignoring spine issues can lead to worsening pain, permanent nerve damage, and loss of mobility. Early surgical intervention, particularly with MISS, can prevent these outcomes.
How to Prevent It?
Maintaining a healthy weight, exercising regularly, practicing good posture, and avoiding smoking can help prevent many spine conditions. Regular check-ups with a spine specialist can also detect problems early.
Nutrition and Bone or Joint Health
Eating a nutritious diet rich in calcium and vitamin D is essential for bone health. Proper nutrition supports healing after surgery and helps maintain the integrity of the spine.
Activity and Lifestyle Modifications
After surgery, it’s important to follow a gradual return-to-activity plan. Avoid heavy lifting, high-impact activities, and anything that puts undue stress on the spine. Staying active with low-impact exercises like walking or swimming can aid in the recovery process.
Do you have more questions?
What is minimally invasive spine surgery (MISS)?
Minimally Invasive Spine Surgery (MISS) is a surgical technique aimed at reducing tissue damage and recovery time compared to traditional open spine surgery. It uses smaller incisions and advanced technologies like endoscopes, navigation systems, and robotics.
What are the benefits of MISS over traditional open spine surgery?
MISS offers several benefits, including smaller incisions, reduced tissue damage, less blood loss, shorter hospital stays, quicker recovery times, and reduced postoperative pain and complications.
What conditions can be treated with MISS?
MISS can treat various conditions, including herniated discs, spinal stenosis, spondylolisthesis, spinal metastasis, spinal deformities, and spinal trauma.
How does endoscopic-assisted spinal surgery work?
Endoscopic-assisted spinal surgery involves using an endoscope to visualize the surgical area through small incisions. This approach minimizes tissue damage and preserves normal anatomy, leading to faster recovery.
What role do robotics play in MISS?
Robotics systems enhance the precision and reliability of spinal surgeries. They help surgeons perform delicate procedures more accurately and reduce physical and mental fatigue during long operations.
Are there any risks associated with MISS?
Like any surgery, MISS has risks, including infection, nerve damage, and complications related to anesthesia. However, these risks are generally lower compared to traditional open surgery.
How long is the recovery period after MISS?
Recovery time varies depending on the specific procedure and patient factors. Generally, patients undergoing MISS experience quicker recovery times and can return to normal activities sooner than those who have traditional open surgery.
Is MISS suitable for everyone?
Not all patients are candidates for MISS. Factors such as the type and severity of the spinal condition, patient health, and previous surgeries play a role in determiNot all patients are candidates for MISS. Factors such as the type and severity of the spinal condition, patient health, and previous surgeries play a role in determining eligibility.ing eligibility.
What advancements have been made in MISS technology?
Recent advancements include high-resolution endoscopic cameras, improved navigation and imaging systems, and robotic-assisted surgical tools. These technologies enhance the precision, safety, and outcomes of MISS.
How does MISS help in treating spinal deformities?
MISS is beneficial for spinal deformities as it reduces tissue damage, blood loss, and recovery time. Techniques like MI-TLIF and MI-LLIF provide sufficient correction while minimizing complications.
Can MISS be performed on patients with previous spinal surgeries?
MISS can be performed on patients with previous spinal surgeries, although careful evaluation and planning are required to address potential scar tissue and anatomical changes.
What are the advantages of using navigation technology during MISS?
Navigation technology provides real-time imaging and guidance, allowing for more precise and safer placement of instrumentation.
What kind of implants are used in MISS?
Specialized screws, rods, and other implants designed for insertion through small incisions are used in MISS.
How does the surgeon decide which type of MISS technique to use?
The choice of technique depends on the specific spinal condition, the location and severity of the issue, and the surgeon’s expertise and assessment of the best approach for the patient.


