To repair a torn meniscus cartilage in the knee, arthroscopic meniscectomy is a minimally invasive outpatient surgical technique. Injuries sustained while playing sports frequently result in meniscus tears in athletes. Meniscus is only partially gone when it is torn.
Some individuals believe that meniscus tears will naturally heal with time. However, the truth is that there are various meniscus tears, and some tears cannot heal on their own. If your meniscus tear is on the outside third of the meniscus, it could mend naturally or need to be surgically fixed.
A 48-year-old patient was in our office with complaints regarding right knee pain. He has had a standing job for many years. He recently played soccer which seems to have worsened the pain.
MRIs were reviewed and discussed during the visit. The results have shown complex medial meniscus tear and reactive medial collateral ligament sprain. Very small joint effusion.
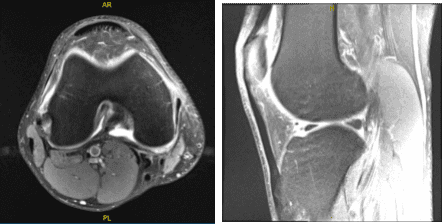
MRI-3T Right Knee non-contrast
We discussed the treatment options for the patient’s diagnosis, which included living with the extremity as it is, organized exercises, medicines, injections, and surgical options. We also discussed the nature and purpose of the treatment options along with the expected risks and benefits.
The patient has expressed a desire to proceed with surgery, and I think that is a reasonable option. I educated the patient regarding the inherent and unavoidable risks which include, but are not limited to anesthesia, infection, damage to nerves and blood vessels, blood loss, blood clots, and even death were discussed at length.
We also talked about the possibility of not being able to return to prior activities or employment, the need for future surgery, and complex regional pain syndrome. The patient also understands there is a long rehabilitative process that typically follows the surgical procedure.
We talked about the possibility of not being able to alleviate all of the discomfort. Also, I explained there is no guarantee all the function and strength will return. The patient also understands the risks of re-tear or failure to heal.
The patient understands implants may be utilized during this surgery. The patient expressed understanding of these risks and has elected to proceed with surgery. We have discussed the surgical procedure as well as the realistic expectations regarding the risks, outcome and post operative protocol.
The patient was taken to the operating room and he was placed on a well-padded operating room table. General anesthesia was induced. The right lower extremity was prepped and draped aseptically in the usual fashion after application of a lower thigh tourniquet and putting in a C-clamp.
Exsanguination and tourniquet elevation was done. The right lower extremity was prepped and draped as usual. Preoperative antibiotic was already given. An incision was given for entry portal. Arthroscope was inserted through the lateral entry portal.
A medial entry portal was made with the use of spinal needle. Examination of the medial compartment showed an injected cartilage of the femoral and medial condyle.
There was a complex tear of the posterior horn and body of the medial meniscus down to medial surface as well as the lateral free margin. Debridement of the tear was done with the use of biter as well as shaver and a stable margin was achieved.
Examination of the intercondylar notch showed intact ACL. Examination of the lateral tibiofemoral compartment showed intact cartilage as well as meniscus. Examination of the patellofemoral compartment showed intact cartilage and normal patellar tracking.
The arthroscope was inserted from the medial entry portal and the margin of the medial meniscus was cleaned to a balanced margin. Final pictures were taken and saved.
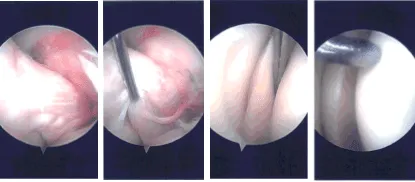
Intraoperative Arthroscopy Images
The knee was thoroughly irrigated and drained. Closure was done with the use of #3-0 nylon and 9 cc of 0.5% Marcaine mixed with 40 mg of Depo-Medrol was injected into the knee.
The dressing was done with the use of Adaptic, 4 x 8, ABD, and Webril, and Ace wrap. The patient was extubated and moved to recover in stable condition.
The patient was seen for a post-operative checkup. We have decided to do formal physical therapy as well as a home exercise program for rehabilitation of the knee. Patients regularly followed an office visit every 3-4 weeks.
The patient did well after the surgery and continued physical therapy. Patient checked in for a follow up visit after a month and saw significant improvement on his knee.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


