A meniscus tear is a common knee injury that causes pain, swelling, stiffness, and difficulty moving the knee. The meniscus is a C-shaped piece of fibrocartilage in the knee that helps with smooth motion and absorbs shock. Meniscus tears can happen from twisting, injuries, falls, or age-related wear.
How Common It Is and Who Gets It? (Epidemiology)
Meniscus tears happen in both young and older adults. In young people, they often occur during sports or accidents. In older adults, they may result from degeneration, which is normal aging of the meniscus. Degenerative tears may happen from small movements rather than a major injury.
Why It Happens – Causes (Etiology and Pathophysiology)
The meniscus can tear from twisting while the foot is planted. It can also tear when caught between the thigh bone and shin bone. Degeneration makes the meniscus weaker and more likely to tear, especially in older adults. Tears may also happen alongside ligament injuries, cartilage injuries, stress fractures, or bone bruises.
How the Body Part Normally Works? (Relevant Anatomy)
The knee joint is formed by the thigh bone above, the shin bone below, and the kneecap in front. Between the thigh and shin bone are two menisci—medial (inner) and lateral (outer). Each is a C-shaped fibrocartilage disc that helps absorb shock, spread load, support bending and rotation, and protect the joint surface.
The meniscus has good blood supply only on the outer edge. The inner part has almost no blood supply, which affects healing. The medial meniscus tears more often because it is less mobile and more firmly attached.
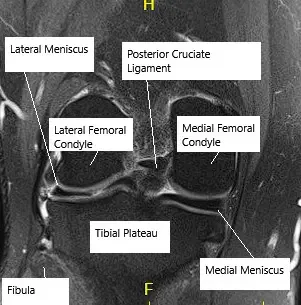
MRI showing knee meniscus.
What You Might Feel – Symptoms (Clinical Presentation)
Symptoms may include knee pain, swelling, stiffness, difficulty straightening the knee, locking, clicking, or the knee giving way. Swelling may appear within hours or overnight. Some patients hear a pop at the time of injury. A locked knee may get stuck in one position. Degenerative tears may cause recurring swelling and point tenderness.
How Doctors Find the Problem? (Diagnosis and Imaging)
A physical exam may show signs of a tear or other knee injuries. X-rays are done to rule out fractures or subluxations. An MRI is the test of choice because it confirms the tear and shows the tear pattern, which helps plan treatment.
Classification
Meniscal tears are classified by their location and pattern:
- Horizontal Tears: Parallel to the tibial plateau.
- Longitudinal (Vertical) Tears: Perpendicular to the tibial plateau.
- Radial Tears: Perpendicular to both the tibial plateau and the long axis of the meniscus.
- Complex Tears: Combination of different types.
- Displaced Tears: Detachment or flipping of a meniscus piece.
Other Problems That Can Feel Similar (Differential Diagnosis)
Symptoms of a meniscus tear can be similar to ligament injuries such as ACL or MCL tears, cartilage injuries, bone bruises, stress fractures, and knee arthritis, especially when swelling and pain recur.
Treatment Options
Non-Surgical Care
In the presence of arthritis, treatment starts with anti-inflammatory medicines, ice, elevation, compression, physical therapy, and sometimes a cortisone shot. These help decrease inflammation and swelling to restore function. If symptoms continue or return, MRI may be used to confirm the tear.
Surgical Care
In the younger population, MRI confirms the tear and looks for other knee injuries. It is best to keep the native meniscus when possible because meniscectomy can speed up arthritis later in life.
If repairable, the meniscus is repaired arthroscopically using stitches. If not repairable, a partial meniscectomy removes loose pieces causing pain, catching, and swelling.
Surgery is done arthroscopically. Patients go home the same day with pain medicine, ice, and sometimes a brace and crutches.
Treatment of a meniscal tear in presence of arthritis
Meniscal tear under degenerative setting can be initially treated conservatively with the use of antiinflammatory medications, elevation, icing, compression, use of physical therapy with or without the use of cortisone shot.
These all help in decreasing the inflammation and the swelling of the knee and helping in returning the function of the knee to normal. If the patient does not have relief from all these conservative measures or there is recurrence of the symptoms, then an MRI can be done to confirm diagnosis and a surgical treatment in the form of arthroscopic management of the meniscus can be done.
Treatment of meniscal tear in the younger population
Younger population usually presents with acute presentation of the meniscal tear. An MRI is usually performed in these patients to confirm the diagnosis as well as rule out other injuries to the knee. It is always advisable to keep the native meniscus in place especially in younger population because meniscectomy has been shown to enhance or accelerate the osteoarthritic changes in the knee in the future.
If the meniscal tear is repairable, it should be repaired with the use of sutures on the meniscus. This was usually performed arthroscopically and should be done as soon as possible to improve the chance of healing and full recovery. If the meniscus is non-repairable then a partial meniscectomy has to be performed to debride the meniscus and remove the loose flaps which are contributory to the pain, catching sensation and swelling in the knee.
Recovery and What to Expect After Treatment
Patients are usually seen one week after surgery. After a partial meniscectomy, no brace is needed and physical therapy helps improve motion and strength. Recovery may take three to six weeks. Most daily activities resume as tolerated, and full activity is usually allowed by six to ten weeks.
After meniscal repair, a knee brace and crutches are needed. Patients bear partial weight with the brace locked straight. Therapy begins early but without weightbearing. At six to eight weeks, weightbearing and motion increase as the brace is weaned off. Contact sports are avoided for four to six months.
Possible Risks or Side Effects (Complications)
Infection
Bleeding
Nerve or vessel injury
Failure of the repair to heal
Hemarthrosis
Long-Term Outlook (Prognosis)
Healing depends on tear type, location, age, and blood supply. Repairs in younger people generally do well when performed early. Degenerative tears may respond to conservative care but may recur. Keeping as much meniscus as possible helps protect the joint long-term.
Out-of-Pocket Costs
Medicare
CPT Code 29881 – Arthroscopic Partial Meniscectomy: $129.43
CPT Code 29882 – Arthroscopic Meniscal Repair: $163.86
CPT Code 29883 – Arthroscopic Meniscal Repair (Both Menisci): $199.40
Medicare generally covers most of the approved charge for these arthroscopic knee procedures, leaving you with the standard twenty percent co-insurance. Supplemental plans such as Medigap, AARP, or Blue Cross Blue Shield usually remove this remaining share entirely. These plans are designed to pair with Medicare, so when the surgery is a Medicare-approved treatment, patients commonly have little to no remaining responsibility.
If you also have secondary insurance, such as an employer-based policy, TRICARE, or the Veterans Health Administration, it becomes the payer after Medicare. Once any deductible under the secondary policy is met, which often ranges from one hundred to three hundred dollars, it may cover the rest of the remaining balance. This type of coverage frequently reduces or removes any expected out-of-pocket cost for meniscus surgery.
Workers’ Compensation
If the meniscus injury is the result of work-related activity, Workers’ Compensation pays the full cost of evaluation, surgery, and recovery. You will not have any out-of-pocket expenses under this coverage.
No-Fault Insurance
If the meniscus tear occurred in an automobile accident, No-Fault Insurance pays the entire cost of treatment. The only possible patient responsibility would be a small deductible based on your specific policy.
Example
A patient needed arthroscopic meniscal repair after twisting their knee during activity. With Medicare alone, the estimated out-of-pocket cost would have been 163.86 dollars. Because the patient also had a secondary insurance plan, the remaining twenty percent was covered, leaving them with no out-of-pocket expense.
Frequently Asked Questions (FAQ)
Q. Why does my knee swell after a meniscus tear?
A. Swelling happens because the knee becomes irritated or inflamed after the tear.
Q. Does a meniscus tear always need surgery?
A. No. Many degenerative tears improve with rest, therapy, and other conservative treatments.
Q. How long is recovery after meniscus surgery?
A. Partial meniscectomy may take three to six weeks. Meniscus repair takes longer because it must heal.
Q. Why is repair preferred in younger people?
A. Keeping the meniscus helps protect the knee joint and slows arthritis.
Q. Can a meniscus tear cause locking?
A. Yes. A displaced tear can get stuck between the bones and lock the knee.
Summary and Takeaway
A meniscus tear can cause pain, swelling, stiffness, and locking of the knee. Diagnosis is confirmed with MRI. Treatment can be conservative or surgical depending on the type of tear, age, and activity level. Meniscus repair preserves the knee long-term, while meniscectomy helps when the tear cannot be fixed. Recovery varies based on the procedure.
Clinical Insight and Recent Findings
A recent study examined the meniscus at a microscopic level and showed that its ability to cushion the knee depends on a precise balance between the tissue’s porous structure and the viscosity of synovial fluid, with even moderate increases in porosity causing large rises in fluid flow and a loss of normal shock-absorbing behavior.
These findings reinforce the clinical understanding described in your text: the meniscus functions as a fibrocartilaginous shock absorber that distributes load, protects the articular cartilage, and depends on healthy collagen architecture and adequate hydration to tolerate twisting or compression injuries.
When degeneration or tearing alters this microstructure, as occurs with aging, trauma, or an associated ligament injury, the tissue becomes less effective at controlling joint forces, leading to pain, swelling, mechanical symptoms, and a higher likelihood of additional joint damage.
This research highlights why preserving and repairing the native meniscus whenever possible is critical, particularly in younger patients, and supports current treatment approaches that prioritize protecting meniscal tissue to maintain long-term knee function. (“Study of meniscus microstructure and fluid mechanics – See PubMed.”)
Who Performs This Treatment? (Specialists and Team Involved)
Orthopedic surgeons specializing in knee and sports injuries perform meniscus surgery. Physical therapists guide recovery and strengthening.
When to See a Specialist?
You should see a specialist if pain, swelling, stiffness, or locking continues or returns. Sudden swelling after a twist or fall also needs evaluation.
When to Go to the Emergency Room?
Go to the emergency room if you experience severe swelling, intense pain, inability to move the knee, or symptoms that suddenly worsen after surgery.
What Recovery Really Looks Like?
Recovery includes decreasing swelling, regaining motion, and slowly rebuilding strength. Some patients recover in a few weeks, while others take months depending on whether repair or meniscectomy was done.
What Happens If You Ignore It?
Ignoring a meniscus tear may lead to recurring swelling, locking, or further damage to the cartilage or ligaments.
How to Prevent It?
To prevent meniscal tears:
- Strengthen leg muscles, especially the quadriceps.
- Warm-up before exercising.
- Avoid activities that involve sudden twists and turns.
Nutrition and Bone or Joint Health
Healthy nutrition supports healing after injury or surgery. Balanced meals and hydration help the knee recover.
Activity and Lifestyle Modifications
After treatment, activity should increase gradually. Follow therapy instructions, avoid sudden twisting movements, and delay contact sports until cleared.
Do you have more questions?
What is the function of the meniscus in the knee?
The meniscus acts as a shock absorber, distributes weight, provides joint stability, and aids in smooth knee movement.
How can I differentiate between a meniscal tear and other knee injuries?
Meniscal tears often present with specific symptoms like knee locking, inability to fully straighten the knee, and pain localized to the joint line. Diagnosis usually involves physical exams and MRI.
How effective are conservative treatments for meniscal tears?
Conservative treatments like RICE, physical therapy, and NSAIDs can be effective, especially for minor or degenerative tears.
When is surgery necessary for a meniscal tear?
Surgery is necessary when the tear is large, symptomatic, or unresponsive to conservative treatments, and particularly if the tear is in the red zone, which has better healing potential.
What types of surgical procedures are available for meniscal tears?
Surgical options include meniscectomy (removal of the damaged part) and meniscal repair (suturing the tear).
What are the risks associated with meniscal surgery?
Risks include infection, stiffness, continued pain, and potential for accelerated arthritis if the meniscus is removed.
How long does recovery take after meniscal surgery?
Recovery varies but typically takes several weeks to months. Full rehabilitation includes physical therapy to restore strength and mobility.
Can meniscal tears heal on their own without surgery?
Some tears, especially those in the red zone with a good blood supply, can heal with rest and conservative management.
What activities should be avoided with a meniscal tear?
Activities involving twisting, squatting, or heavy lifting should be avoided to prevent further damage.
How can I prevent meniscal tears?
Strengthening leg muscles, proper warm-up exercises, and avoiding sudden twists can help prevent tears.
What is the prognosis for a meniscal tear?
The prognosis depends on the tear’s location, size, and treatment method. Many people recover well with appropriate treatment.
Are there any long-term complications of untreated meniscal tears?
Untreated tears can lead to chronic pain, knee instability, and increased risk of developing osteoarthritis.
How does age affect meniscal tear treatment and recovery?
Older adults may have more degenerative tears and slower healing, often requiring a more conservative approach or surgery based on overall health.
Can physical therapy alone heal a meniscal tear?
Physical therapy can strengthen surrounding muscles and improve function, potentially aiding in the healing of minor tears.
What are the signs of a meniscal tear in athletes?
Athletes may experience knee pain, swelling, popping sensations, and difficulty moving the knee.
How common are meniscal tears?
Meniscal tears are common, especially among athletes and older adults due to injury and degenerative changes.
What is the difference between a partial and complete meniscectomy?
A partial meniscectomy removes only the damaged portion, while a complete meniscectomy removes the entire meniscus, which is rare due to high risk of arthritis.
Can meniscal tears occur alongside other knee injuries?
Yes, they often occur with ligament injuries like ACL tears.
What role does imaging play in diagnosing meniscal tears?
MRI is the most accurate imaging tool for diagnosing the type and extent of meniscal tears.
Can diet and supplements aid in meniscus healing?
A balanced diet rich in anti-inflammatory foods and supplements like glucosamine may support joint health, though evidence is mixed.
What are the potential complications of meniscal repair surgery?
Complications can include infection, blood clots, and the possibility that the repair doesn’t heal properly, necessitating further surgery.
How does weight affect meniscal tear risk and recovery?
Excess weight increases stress on the knee, raising the risk of tears and complicating recovery.
Are meniscal tears more common in certain sports?
Sports that involve a lot of twisting and pivoting, like soccer, basketball, and skiing, see higher rates of meniscal tears.
What is the likelihood of re-tearing the meniscus after surgery?
Re-tear risk depends on factors like the tear type, repair quality, and post-surgery care but can occur, especially if the knee is subjected to high stress too soon.


