A 50-year-old female presented to our office with complaints of worsening left hip pain. The patient did not recall any inciting event when the pain first started seven years ago. The pain gradually worsened over the years. She saw another physician who told her she had avascular necrosis of the left hip.
She was on medical therapy in the form of blood thinners, cholesterol-lowering agents and bisphosphonates. The pain was initially well managed with Tylenol and NSAIDs but recently the relief was not substantial.
She was working as a hairdresser and had recently stopped working as the pain was unbearable on standing for long. The pain was located in the left groin which was at times radiate to the inner side of the left knee. The pain was described as sharp pain and moderate to severe in intensity.
The pain was exacerbated on activities such as navigating stairs, walking, bending, squatting or getting up from a chair. The pain disturbed her sleep and she was distressed due to lack of proper sleep. She felt the medical therapy was initially helpful but now the pain was limiting her daily activities.
She was a nonsmoker and a nondrinker. She denied any known drug allergies. Her medical history was positive for dyslipidemia and pre-diabetes. She had right breast lumpectomy and a left shoulder arthroscopic surgery five years ago.
On physical examination, her gait was antalgic with a reduced stance phase on the left side. The bilateral shoulders, iliac spines, patella, and the malleolus were at the same level. There was no exaggeration of the lumbar lordosis. There was no evidence of any functional or structural scoliosis.
The skin overlying the left groin was normal with no evidence of any scar marks or sinus tracts. There was no swelling of the left groin or inguinal lymphadenopathy. Tenderness was present on the left anterior joint line. There was no broadening or thickening of the trochanter.
On digital palpation, both the greater trochanter were at the same level. The pelvis was squared and there was no evidence any leg length discrepancy. The range of motion was restricted in internal rotation and abduction. There was no evidence of any fixed deformity in coronal, sagittal and axial planes. There was a differential rotation of the left hip in flexion.
The power, bulk, and tone of the muscles of both the lower extremities were normal. There was no evidence of any distal neurological deficit. The examination of the lower spine, right hip, bilateral knee, and ankles was normal. The bilateral lower extremity pulses were palpable and comparable.
An X-Ray was obtained suggesting severe loss of joint space with acetabulum changes in the left hip. There was a loss of spherical contour of the left hip. Sclerosis and subchondral cysts were present in the left hip with a collapse.

Preoperative X-ray of the pelvis with both hips in anteroposterior view showing AVN changes in the left hip.
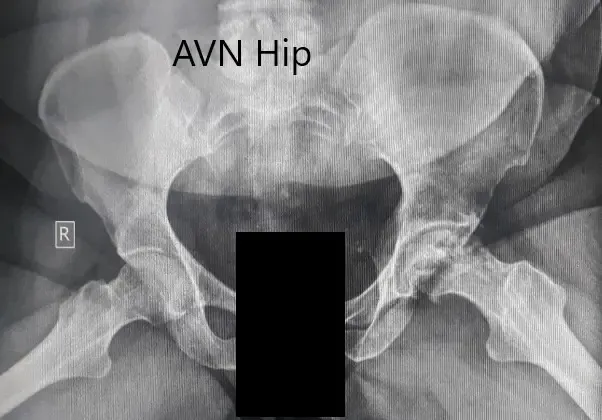
Preoperative X-ray of the pelvis with both hips in the frog-legged lateral view showing AVN changes in the left hip.
An MRI was obtained which showed altered signal intensity in both T1WI and T2WI. There was a subtle collapse of the left femoral head. A serpiginous hyperintense line was seen on T2WI demarcating an area of osteonecrosis in the left femoral head. This area involved the lateral and medial compartment and covered more than 50% of the surface area of the head.
Secondary osteoarthritic changes were visualized in the form of reduction of anterosuperior joint space and osteophyte formation. A small amount of fluid was seen in the joint cavity.
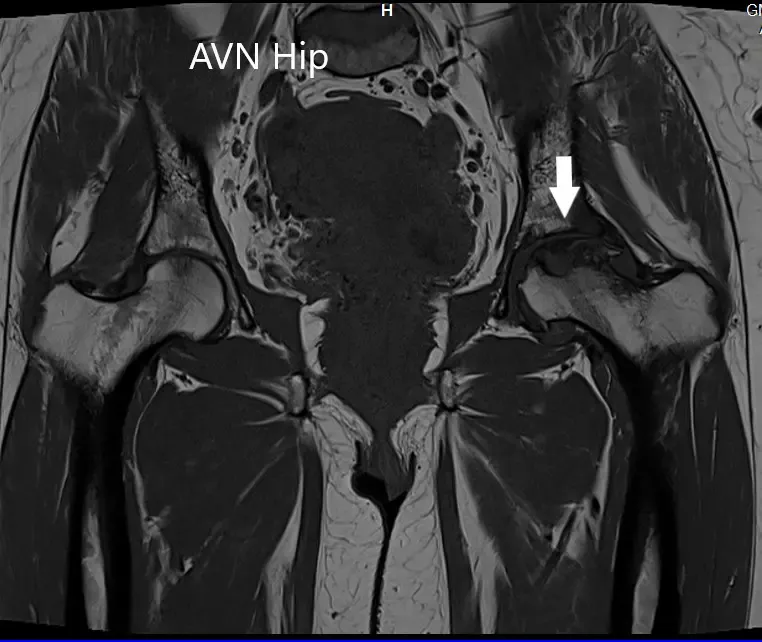
T1WI image of MRI showing the coronal section.
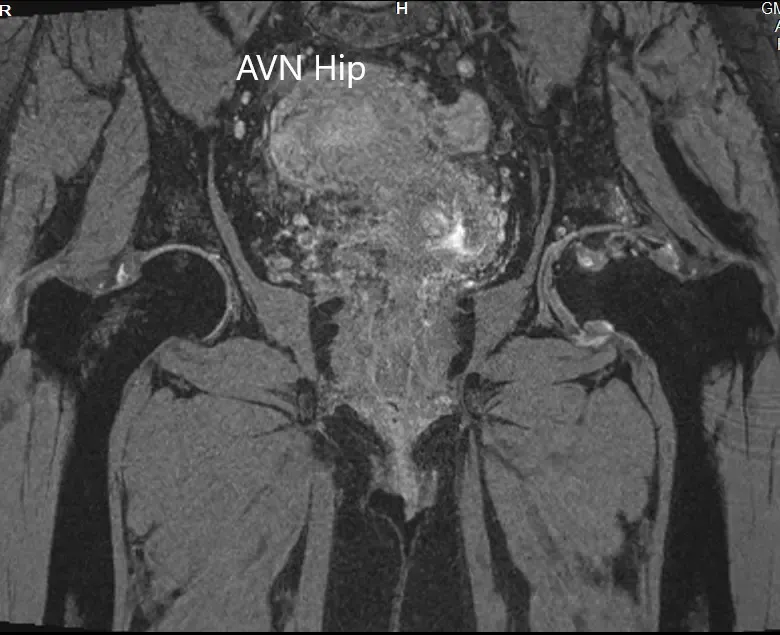
T2WI MRI image showing the coronal section.
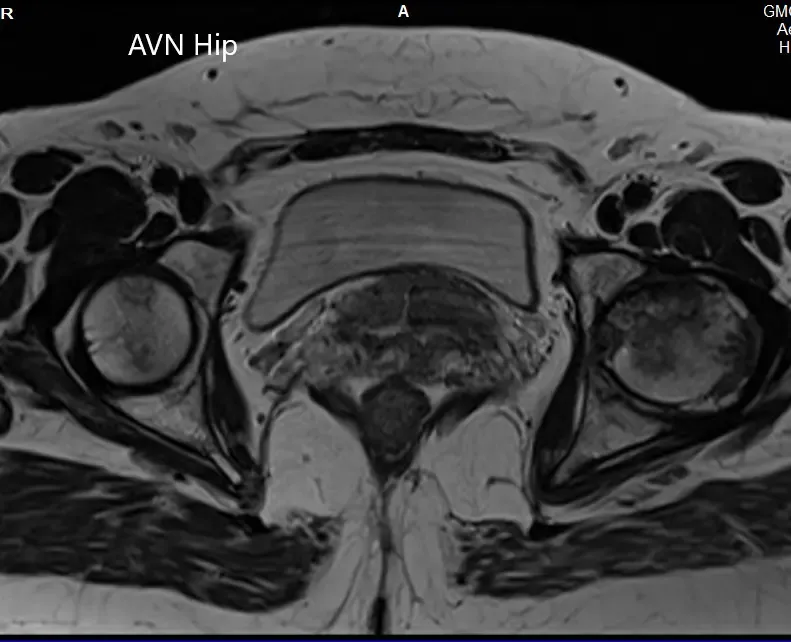
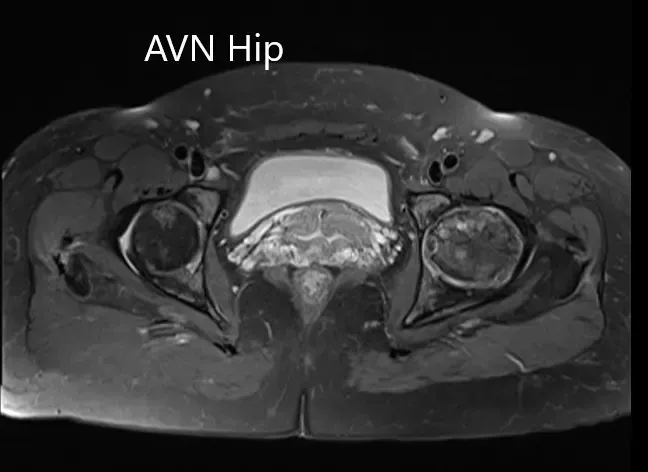
T1WI and T2WI of the MRI showing an axial section of the bilateral femoral head.
She had a unilateral left head of femur idiopathic avascular necrosis with acetabulum changes. She was advised a left total hip replacement. Risks, benefits, and alternatives were discussed with the patient at length. She agreed to go ahead with the procedure.
A left total hip replacement was performed on the patient. Post-op her vitals remained stable. The pain was managed well with medications and she was given aspirin for deep vein thrombosis prophylaxis.
Weight-bearing was allowed as tolerated with support. The sutures were removed uneventfully. She was compliant with hip precautions and physical therapy. Three months post-op she was walking without the support and reported no pain in the left hip.
She was back to her baseline activities and returned to her job as a hairdresser. She was extremely happy and relieved to be free from pain. She follows up regularly for surveillance of any avascular changes in the right hip.


