Debridement can be performed either arthroscopically (via two or three microscopic incisions) or openly (often through one larger incision). Surgery to repair the rotator cuff frequently includes it.
Shoulder injury may result in discomfort that develops suddenly or gradually, a sense that the shoulder is loose, or arm weakness. Surgery, physical therapy, and rest are all options for treatment. When the ligaments holding the clavicle to the acromion rupture, it results in a shoulder separation, also known as a sprain.
A 25-year-old patient was in our office with complaints regarding lower back pain (Left lower back), right shoulder, neck, left foot and bilateral knee pain due from MVA. Patient did not have pain in these body parts before the current injury except both knee pain which seems to have aggravated with the accident. Neck and left foot have improved. He is having tingling in left foot.
The patient presented MRI results for shoulder and knee, the shoulder has shown anterior and posterior labral tearing. The biceps tendon is hypoplastic, ill-defined. Synovitis of the patulous axillary pouch of the inferior glenohumeral ligament.
Cuff tendinosis/tendon with tendinopathy and thickening of the supraspinatus, subscapularis and infraspinatus portions of the cuff. Impingement. For the knee, joint effusion. Quadriceps tendinosis/tendonitis. Supra and infrapatellar plica. Patella alta or high positioned patella. Partial LCL tear. Heterogeneous and partially torn ACL.
We discussed the treatment options for the patient’s diagnosis, which included living with the extremity as it is, organized exercises, medicines, injections, and surgical options. I also discussed the nature and purpose of the treatment options along with the expected risks and benefits.
I educated the patient regarding the inherent and unavoidable risks which include, but are not limited to infection, stiffness, damage to nerves and blood vessels, blood loss possibly requiring transfusion, blood clots, persistent or worsening pain, loosening or failure of implants, instability, tingling or numbness, anesthesia and systemic complications including cardiac, pulmonary, neurological complications and even death were discussed at length.
I also talked about the possibility of not being able to return to prior activities or employment, the need for future surgery, and complex regional pain syndrome. The patient also understands there is a long rehabilitative process that typically follows the surgical procedure.
I talked about the possibility of not being able to alleviate all the discomfort. Also, I explained there is no guarantee all the function and strength will return. I discussed the type of implants that may be utilized during this surgery. The patient expressed understanding of these risks and has elected to proceed with surgery.
I discussed the patient’s medications and allergies and the possible need for medical and other clearances if needed. I have discussed the surgical procedure as well as the realistic expectations regarding the risks, outcome, and post operative protocol.
The patient was put in a left lateral position on a beanbag with the right shoulder up after informed consent and supraclavicular block was placed. All the bony prominences were well padded. The patient was placed in a secured position.
The right shoulder was prepped and draped aseptically in usual fashion. It was put on traction with 40 degrees of abduction and 20 degrees of flexion. Preoperative antibiotic was given. Anterior portal was made through the posterior soft spot into the glenohumeral joint.
The arthroscope was inserted. Anteroinferior portal was made with the use of a spinal needle just above the subscapularis tendon. Cannula was inserted. Examination of the glenohumeral joint was done, which showed fraying of the glenoid labrum.
There was no clear tear in the anterior or posterior labrum. Debridement of the glenoid labrum was done with the use of a shaver. Examination of the biceps showed intact biceps.
There was articular sided fraying of the rotator cuff in the region of the infraspinatus, which was debrided with the use of shaver. There was no articular lesion. The subscapularis was intact. The arthroscope was inserted into the subacromial region where synovitis was present, which was debrided with the use of shaver from the anterosuperior portal.
The glenohumeral joint was also examined with the arthroscope in the anteroinferior portal and the findings were confirmed. The subacromial bursa was removed with the use of a shaver from the subacromial space. There was no impingement. The AC joint was intact. Final pictures were taken and saved.
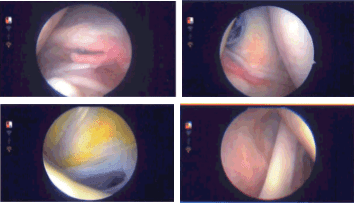
Intraoperative Arthroscopy Images
The shoulder was irrigated and drained. Closure was done with the use of nylon. Dressing was done with the use of Xeroform, 4×4, ABD, and tape. The patient was extubated and moved to Recovery in stable condition.
The patient was seen for post operative check up. We have decided to do formal physical therapy as well as a home exercise program for rehabilitation of the shoulder. Patients regularly followed an office visit every 3-4 weeks.
Patient did well after the surgery and continued physical therapy. Patient checked in for a follow up visit after a month and saw significant improvement on his shoulder.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


