A lateral meniscus tear affects the semicircular cartilage that lines the exterior of the knee joint. Through twisting or a traumatic injury, it can happen suddenly. Alternatively, it could come about gradually as a result of damage.
A 29 year-old female patient seen in the office with right knee pain after MVA. She has a history of right knee injury with lateral meniscus tear, tricompartmental AO in 2018 following a dancing accident.
She did not get surgery for it but recovered completely and was able to perform all usual activities without any pain of discomfort. We discussed treatment options including PT, MRI, Injection, surgery. We agreed to go with 3 Tesla MRIs.
The patient who has been seeing a doctor for right knee pain following a motor vehicle accident past summer. She had a similar car accident two years back when she had a lateral meniscus tear, which was treated non-operatively due to COVID pandemic. She had been doing fine before this recent accident.
She has been making her limp and not able to bear weight on the knee. She was advised surgical treatment, but could not undergo surgery earlier due to insurance issues. We discussed treatment options but she opted for surgical management.
We discussed risks and benefits including infection, bleeding, injury to adjacent nerves and vessels, re-injury, need for repeat surgery, failure of surgery, rehabilitation, stiffness, systemic complications including blood clot, cardiac, pulmonary, or neurological complications including death. The patient understood and signed informed consent.
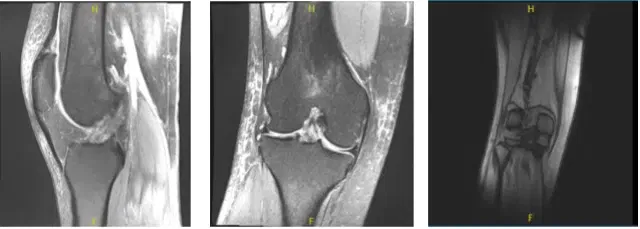
MRI-3T Right Knee non-contrast
The patient was taken to the operating room where she was placed on a well-padded operating room table. General anesthesia was induced. Low thigh tourniquet was applied. Esmarch was applied and the thigh was put on the tourniquet.
The right lower extremity was prepped and draped aseptically in usual surgical fashion. Time-out was called. Bony prominences were marked on the anterior and the lateral sides in case we had to do an open inside-out surgical repair.
A lateral incision was given and an arthroscopic was inserted. A medical entry portal was made with access to the central compartment. Probe was inserted. Examination of the medial tibiofemoral compartment showed injected cartilage as well as meniscus.
Examination of the intercondylar notch showed an injected ACL. Examination of the patellofemoral compartment showed grade 1 tearing of the trochlea with no cartilage loss of the patella. Debridement was done with the use of a shaver.
Examination of the lateral tibiofemoral compartment showed fraying and tearing of the lateral meniscus and the posterior horn as well as vertical tear of the body of the lateral meniscus. Debridement of lateral meniscus was performed.
There was a free edge tear of the anterior horn of the lateral meniscus also, which was debrided. Decision was made to repair the lateral meniscus considering that it was reducing very well.
Flexible FAST-FIX sutures were used to pass horizontal mattresses x2. A good repair was achieved. Spinal needle was done to fenestrate the capsule of the lateral meniscus in the region of the repair. Microfracture chondroplasty of the intercondylar notch was performed from the holes.
Final pictures were taken and saved. The knee was thoroughly irrigated. Then, 10 cc of 0.5% Marcaine was injected in the knee. Closure was done with the use of #3-0 nylon. Dressing was done with the use of Xeroform, 4 x 8, DSD, Webril, Ace wrap. A knee immobilizer was applied. The patient was extubated and moved to recovery in a stable condition.
After one week the patient was seen in the office and we discussed treatment options. She has been using knee braces and crutches. She denies fever, chills and Her pain is not well controlled and she is staying at home as well as here.
She and her friend feel that she has a low threshold for pain. We discussed the importance of avoiding opioids and also using NSAIDs for pain control. The patient referred to pain management for pain control.
We also discussed the importance of PT and movement. She will get a bledsoe which has to be used locked in extension. Knee should not be bent beyond 90 degrees. She will be PWB with brace locked in extension.
We have decided to proceed with formal physical therapy as well as a home exercise program for rehabilitation of the knee. We went over the arthroscopic pictures and removed the stitches during the visit. We will continue with ice and elevation of the knee to decrease swelling and pain.
We will continue to utilize early mobilization and mechanical prophylaxis to reduce the chances of a deep vein thrombosis. We will wean them off any narcotic medications and progress to anti-inflammatories and Tylenol as long as there are no contraindications to these medications.
We also discussed the risk and benefits and common side effects of taking these medications. The patient will be back in three weeks’ time to evaluate the progress
After a month of seeing the patient in the office, she has been using a knee brace and single crutch. She denies fever, chills. She has been using a knee brace and single crutch. Denies fever, chills. Her pain is well controlled.
She is working with PT and improving. With regular visits in the office, the patient did well after the surgery and continued physical therapy and rehabilitation for the knee.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


