A cartilage component called meniscus, aids in the appropriate function of your knee. Meniscal tears, a frequent knee ailment, are commonly treated by a meniscectomy. The purpose of the procedure is to eliminate meniscus pieces that protrude into the joint. Your knee may lock as a result of these pieces obstructing joint mobility.
Patient presented today is a 24 year-old female who complains of still having pain on her left knee even after the surgery, three months ago. The patient who had a twisting injury to the left knee while she was exercising. Her X-ray showed no significant degenerative changes and no acute fractures.
We agreed to have an MRI which showed status post meniscal repair of bucket-handle tear seen previously with appearance is recurrent tear and disruption of anterior horn associated with displacement of a large flap and focal disruption of posterior horn into proximity of tibial attachment.
Postsurgical changes are present at the meniscocapsular junction and through the subcutaneous tissue. Arthroscopic portals are also visualized to infrapatellar fat. Mild lateral compartment degenerative disease and small joint effusion were also observed.
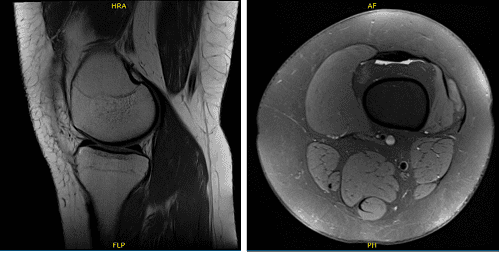
X-ray of left knee
The patient was taken to the operating room where she was placed on a well-padded operating table. General anesthesia was induced. The left lower extremity was prepped and draped aseptically in the usual sterile fashion and inflated to 300 mmHg.
Tourniquet time of more than 30 minutes was used for the surgery. Timeout was called. Preoperative antibiotic was given. Lateral entry portal was made and an arthroscope was entered. A medical entry portal was also made.
Examination of the medial compartment showed intact meniscus and cartilage. Examination of the intercondylar notch showed intact ACL as well as cartilage.
Examination of the lateral compartment showed tearing of the lateral meniscus and sutures were present. The lateral meniscus was debrided with the use of upbiter, straight biter, and shaver. A thorough debridement was performed. There was some amount of arthritis of the tibial cartilage.
Balanced margins were achieved. Almost 40% of lateral meniscus was resected in the procedure to achieve balanced margins. Final pictures were taken and saved. The examination of the compartment showed no arthritis. Final pictures were taken and saved. The knee was thoroughly irrigated and drained.
Closure was done with # 3-0 nylon. Then, 30 cc of Marcaine 0.5% mixed with 40 mg of Depo-Medrol was injected into the knee. Dressing was done with the use of Xeroform, 4×8, ABD, Webril, Ace wrap. The patient was extubated and moved to recovery in stable condition.
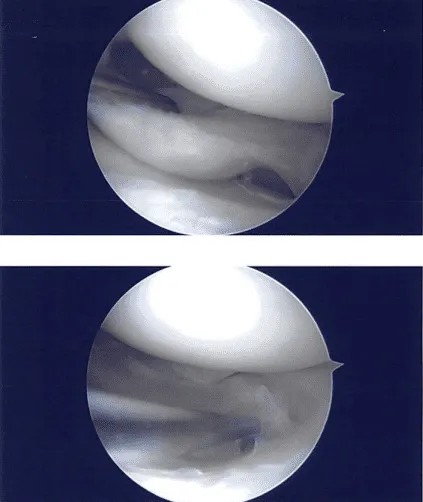
Intraoperative images
The patient underwent postoperative evaluation and was determined to move through with formal physical therapy as well as a home exercise program for knee rehabilitation. We’ll keep applying ice and elevating the knee to relieve pain and swelling while also lowering the risk of a deep vein thrombosis.
We’ll also use early mobilization and mechanical prophylaxis. As long as there are no contraindications to these meds, we will advance to anti-inflammatories and Tylenol after we have weaned them off of any narcotic medications. She will also continue taking aspirin. In three weeks, I’ll meet them again to assess their development.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


