Knee arthroscopy may help with the excruciating symptoms of a variety of conditions that harm the soft tissues and cartilage surfaces around the joint. Injury to one or more of the ligaments, tendons, cartilage, bones, or muscles that make up the knee joint constitutes a knee injury.
These injuries can be caused by falling, twisting the knee violently, heavy impact from a car accident, or other forces.
A 69 year-old patient was in our office with complaints regarding left knee pain after twisting. For aggravating factors, patients reported standing, walking, twisting, weight bearing, upstairs, and downstairs.
For associated symptoms, she reported swelling, buckling, instability, tender to the touch, and pain with motion but reports no weakness, no numbness, no tingling, no redness, no warmth, no ecchymosis, no catching/locking, no popping/clicking, no grinding, no radiation, no drainage, no fever, no chills, no weight loss, and no change in bowel/bladder habits.
The patient also brought and presented X-Ray results for both of her knees. For the left, there are mild osteoarthritic degenerative changes. There are no acute fractures. However, for the right, there are moderate osteoarthritic degenerative changes. Joint effusion. There are no fractures.
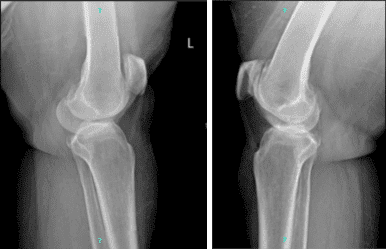
Left and right knee x-ray complete patella
We discussed the treatment options for the patient’s diagnosis, which included living with the extremity as it is, organized exercises, medicines, injections and surgical options. We also discussed the nature and purpose of the treatment options along with the expected risks and benefits.
I educated the patient regarding the inherent and unavoidable risks which include, but are not limited to anesthesia, infection, damage to nerves and blood vessels, blood loss, blood clots, and even death were discussed at length.
We also talked about the possibility of not being able to return to prior activities or employment, the need for future surgery, and complex regional pain syndrome. The patient also understands there is a long rehabilitative process that typically follows the surgical procedure.
We talked about the possibility of not being able to alleviate all of the discomfort. Also, I explained there is no guarantee all the function and strength will return. The patient also understands the risks of re-tear or failure to heal.
The patient understands implants may be utilized during this surgery. The patient expressed understanding of these risks and has elected to proceed with surgery. We have discussed the surgical procedure as well as the realistic expectations regarding the risks, outcome, and post operative protocol.
The patient was taken to the operating room where she was placed on a well-padded operating room table. General anesthesia was induced. Preoperative antibiotics were given. Left lower extremity was prepped and draped aseptically in the usual fashion.
A lateral entry portal was made and an arthroscope was inserted. Examination of the patellofemoral joint showed patches of grade 4 arthritis and grade 1 osteoarthritis on the rest of the patella and trochlea.
Examination of the medial tibiofemoral compartment showed tears involving the posterior horn of the medial meniscus with horizontal delamination. A medial entry portal was made with the use of a spinal needle.
Shaver was introduced through the medial portal and meniscectomy was performed with the use of shaver as well as upbiter and straight biter. Balance of margins was achieved.
Examination of the medial femoral condyle compartment showed grade 1 osteoarthritic changes of the medial femoral condyle. Examination of the intercondylar notch showed intact ACL. Examination of the lateral compartment showed intact meniscus as well as cartilage.
Another shaver was introduced from the lateral portal and camera from the medial portal and balancing of the margins of the medial meniscus was further performed with the use of shaver.
Chondroplasty of the patella and trochlea was also performed. The knee was thoroughly irrigated and drained. Closure was done with the use of # 3-0 nylon. Marcaine 0.5% 30 cc mixed with 40 mg of Depo-Medrol was injected into the knee. Dressing was done with the use of Xeroform, Webril, 4 x 8s, ABD, and Ace wrap. The patient was extubated and moved to recovery In a stable condition.
The patient wished to proceed with the injection to reduce pain and swelling. After a sterile prep, 7cc of 0.5% marcaine and 80mg of depo-medrol were injected into the left knee.
The patient tolerated the procedure well and there were no complications. Post injection pain, blood sugar elevation, skin discoloration, fatty atrophy and the signs of infection were discussed in detail.
The patient was seen for post operative check up. We have decided to do formal physical therapy as well as a home exercise program for rehabilitation of the knee.
The patient did well after the surgery and continued physical therapy. Patient checked in for a follow up visit after a month and saw significant improvement on her knee.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


