A retired nurse presented to our office with complaints of worsening right knee pain for the past 15 years. She first noticed the pain while working but without any precipitating cause. She feels her long hours at work contributed to her knee pain. The pain had gradually progressed over the years and she recently went to the ER for excruciating knee pain.
The pain is located on the inner side of the knee described as a sharp pain. The intensity was described as moderate which would increase to severe on exacerbating activities. The pain was worse with activities such as bending, twisting, turning, kneeling, walking, and getting up from a chair. She was unable to climb stairs due to her knee pain. She denied any feeling of instability or giving away.
She was currently staying with her husband and enjoyed cooking. She stated she used to host her children and friends for food but in the past year, she had been unable to do so owing to pain. She tried treatment modalities such as cortisone injections, gel injections, and physical therapy. While they provided some relief but it never lasted for more than two weeks.
Her husband recently had a hip replacement surgery and was now enjoying pain-free mobility. She was enthusiastic about the results of replacement surgery and wanted to explore her options for knee pain.
She was an occasional smoker and social drinker. She was allergic to penicillin. Her medical history was positive for high blood pressure, hypothyroidism and gastroesophageal reflux disease. She was currently taking Toprol XL 25mg, Levothyroxine, and Omeprazole. She previously had a hysterectomy 25 years ago and carpal tunnel repair 6 years ago.
On physical examination, her gait was steady. There was mild swelling in the right knee. Tenderness was present on the medial and lateral joint line. Additionally, there was tenderness on patellar facets. There was mild genu varus deformity. The skin overlying the knee was normal with scar, sinus or redness.
There was no coronal, sagittal, and rotational instability or laxity. The range of motion was restricted due to pain (5 degrees to 90 degrees). There was ample joint crepitus on range of motion. The examination of the right hip revealed bursitis. The examination of the left hip left knee and bilateral ankles were normal.
There was no distal neurological deficit. The distal extremity pulses were palpable and comparable. Imaging revealed severe tricompartmental osteoarthritis of the right knee. Options discussed with her at length including surgical and nonsurgical methods. She was given the option of right custom knee replacement. She agreed to go ahead with it.
A preoperative CT scan was done a few weeks prior to the surgery. Detailed images of her unique knee anatomy and correct biochemical axis were obtained. The data was used to construct customized implants. Patient-specific unique bone jigs were 3D constructed to match the contour of the knee. A preoperative plan was made to aid in the surgery.
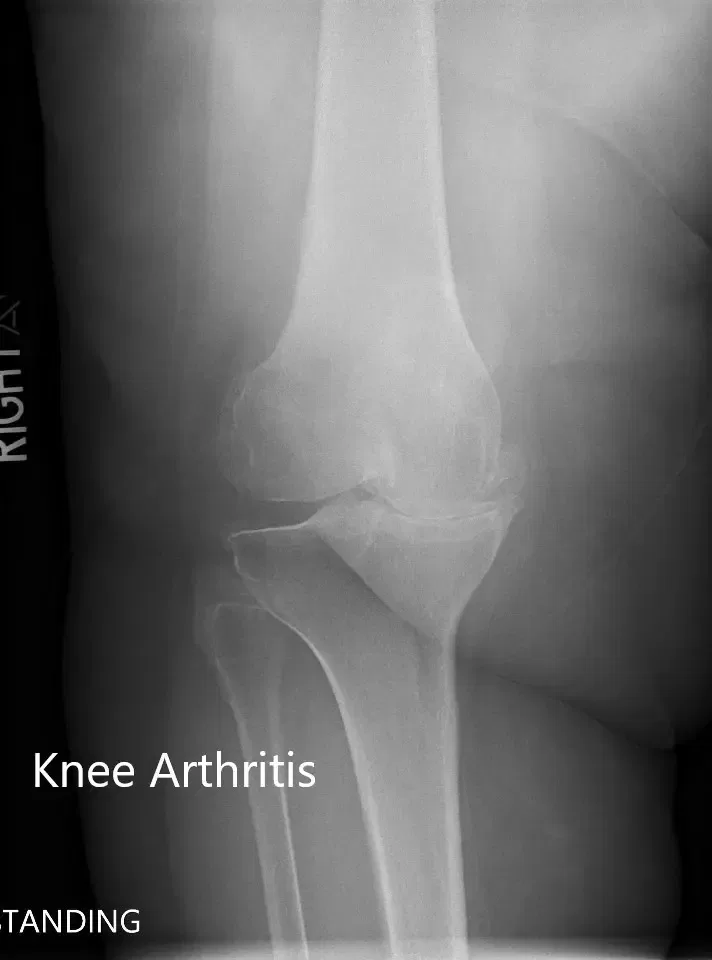

Preoperative X-ray of the right knee showing AP and lateral views.
OPERATION: Right total knee arthroplasty.
IMPLANTS USED: Customized Femur with a customized Tibia, posterior stabilized with 35mm patella with 14 mm polyethylene insert.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. Anesthesia was obtained by the anesthesiologist.
The patient was then definitively positioned and a cuff was placed over her right thigh. The limb was exsanguinated and the tourniquet was elevated. A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were incised. Medial parapatellar arthrotomy was performed and the tibia was exposed.

Complete Orthopedics patient-specific surgical plan for a customized right knee replacement in a 72-year-old patient.
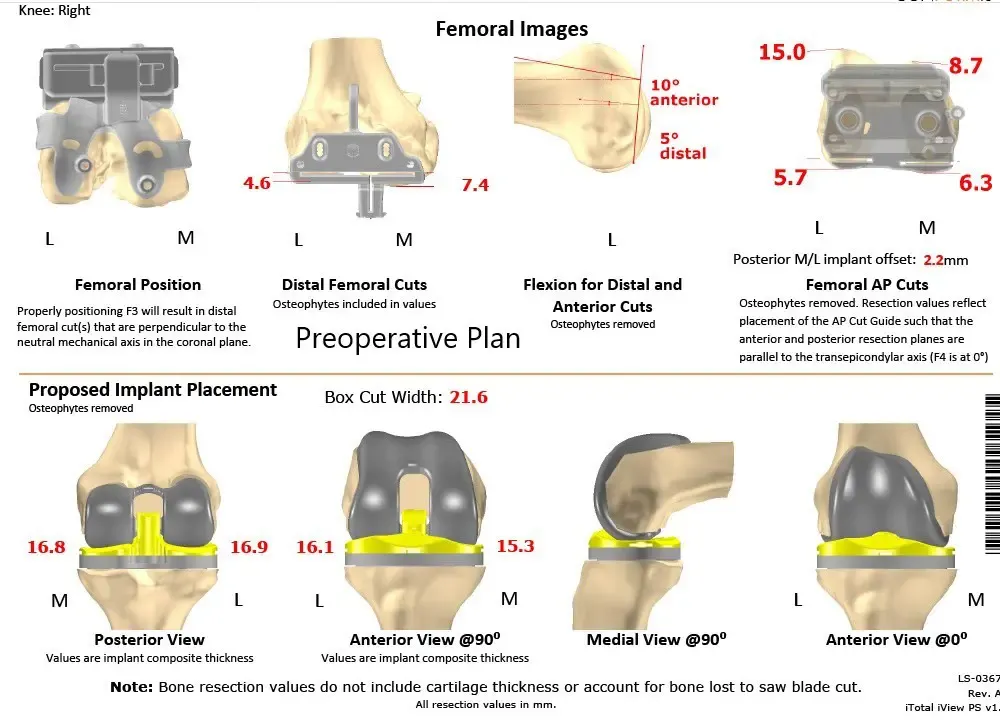
Complete Orthopedics patient-specific surgical plan for a customized right knee replacement in a 72-year-old patient (scan 2)
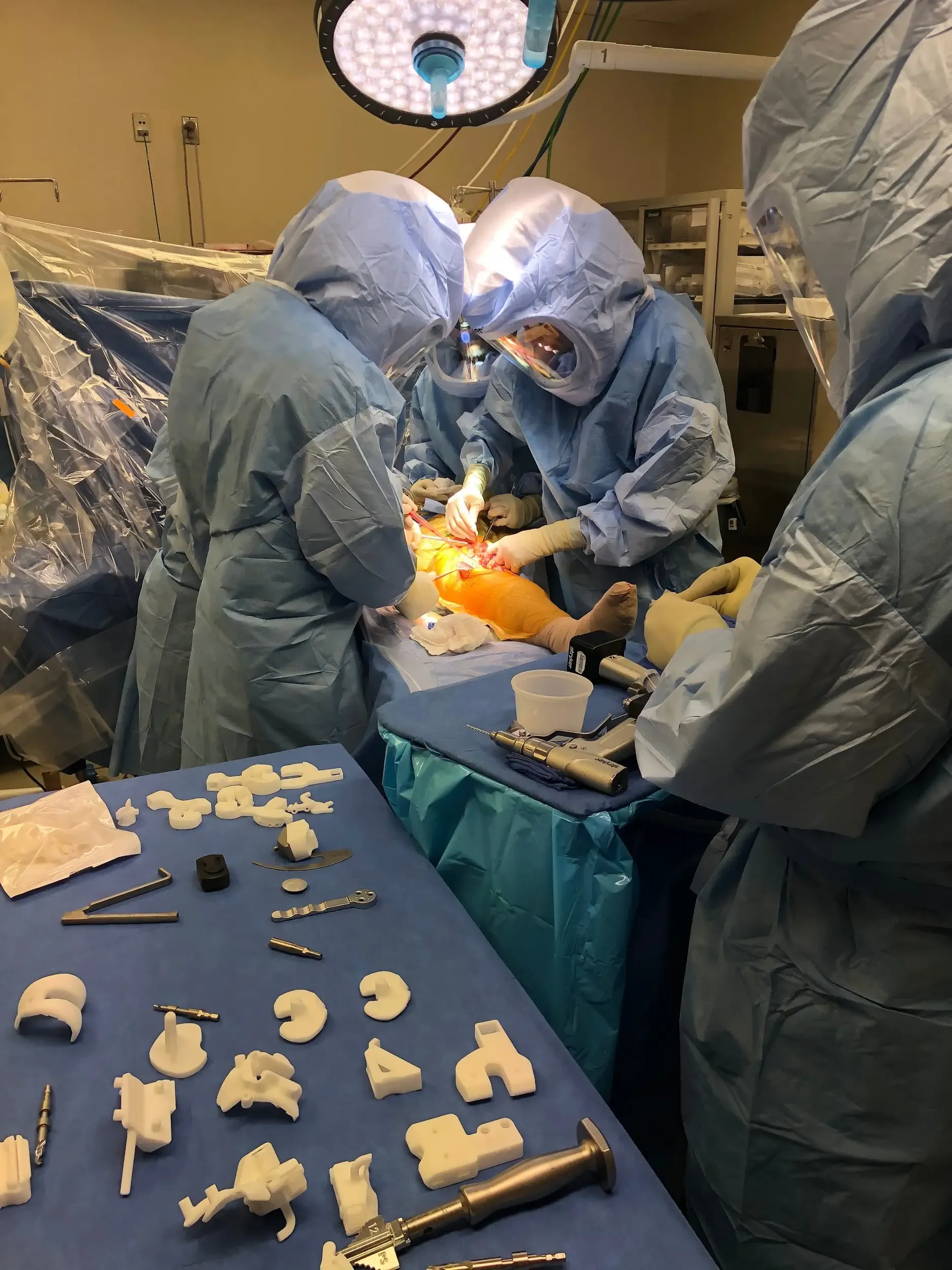
Doctors performing the actual surgery
The tibial cutting guide was placed and the tibial resection was then performed. Attention was then turned towards the femur and the distal cut and chamfer cuts and a notch cut were performed using the custom cutting guides. The medial release was done for balancing the knee joint. Flexion and extension gaps were balanced.
The tibia was prepared. The patellar resection was performed. The drill holes were made in the patella. The trial patella was placed into position. The trial femur was placed into position.
The trial tibia was placed into position. Poly was placed into position, and the knee was then trailed through a full range of motion. The knee was stable in the range of motion.
Trial components were then removed. The injection was given. The femur was cemented into position followed by the tibia. Poly was then placed into position and knee was then reduced and held in full extension with a bump on the back. The patella was then cemented into position. Excess cement was removed.
After the cement hardened, the patellar clamp was removed. The medial parapatellar arthrotomy was closed with #1 Vicryl and Stratafix. Cutaneous tissues were closed with O Vicryl. Subcuticulartissues were closed with 2-0 Vicryl.
The skin was closed using staples. Tourniquet was then let down. Sterile dressing was achieved, and the patient was transferred to the postoperative care unit in stable condition.
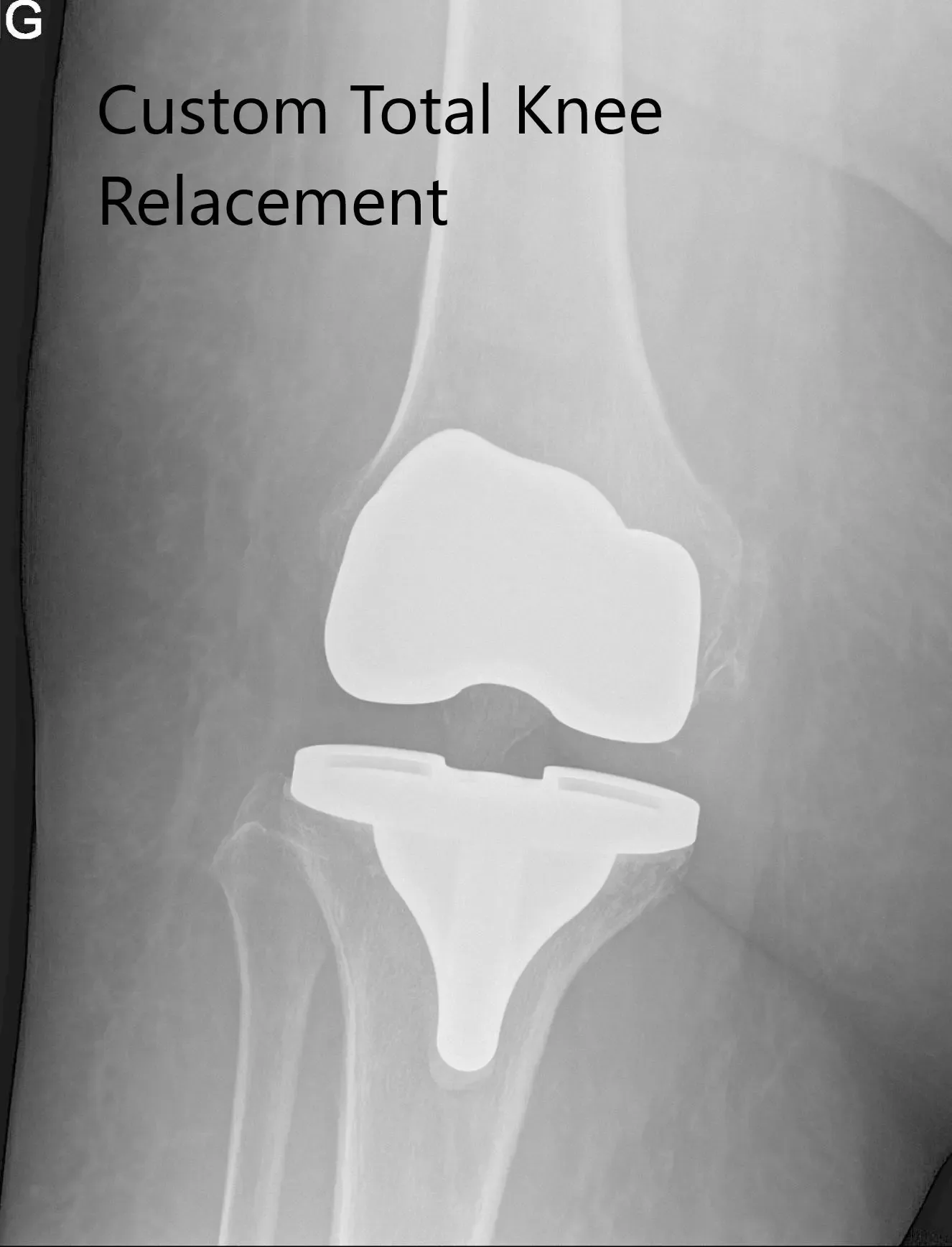
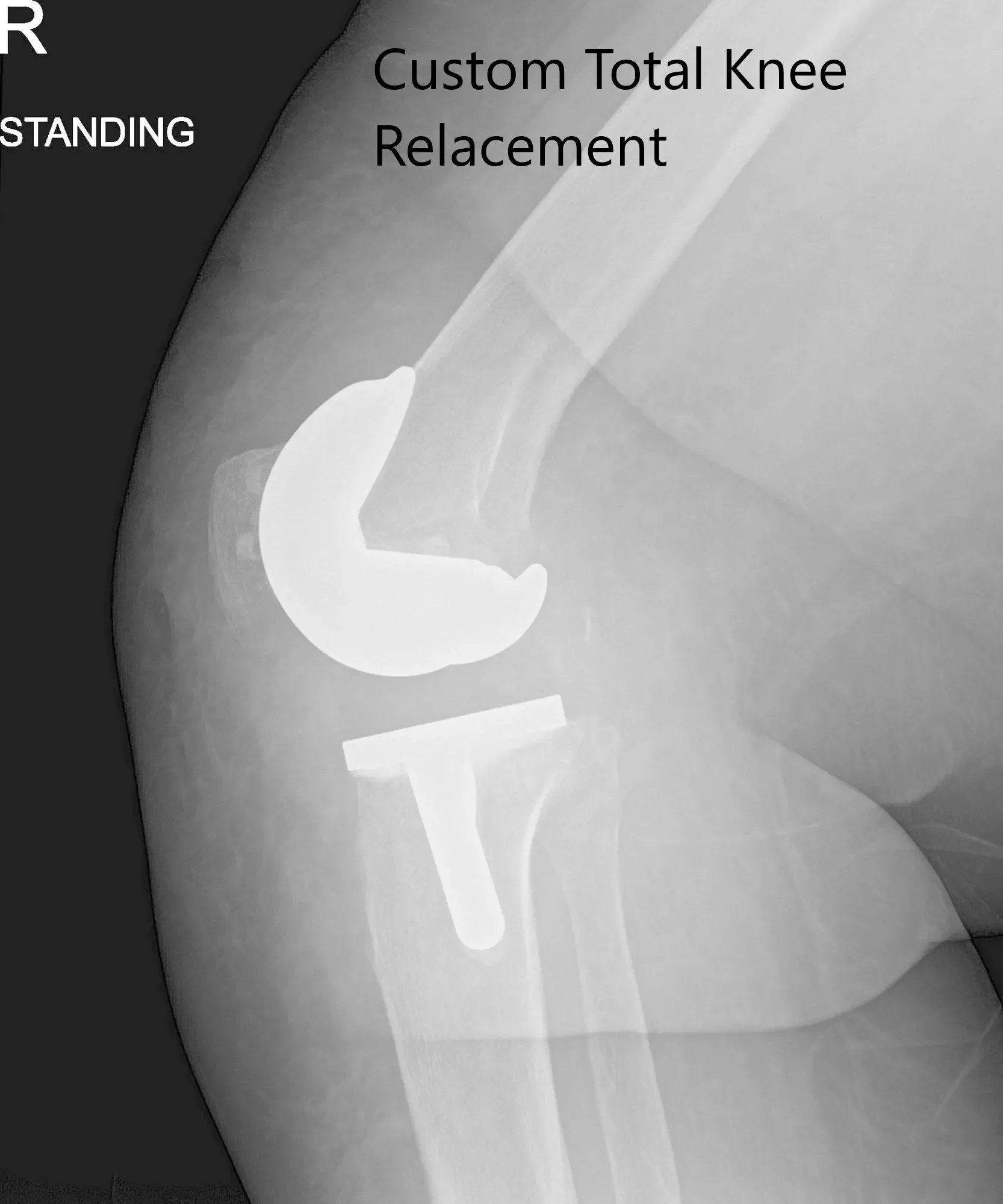
Postoperative x-ray images showing AP and lateral views of the right knee
She was able to walk bearing weight, the same day of the procedure. Her vitals were stable postoperative and she was discharged the next day. The pain was managed well with medications and aspirin was started for DVT (deep vein thrombosis) prophylaxis.
Her postoperative x-ray demonstrated excellent alignment. Outpatient physical therapy was started for increasing the range of motion and strengthening of muscle. On a subsequent follow-up visit, she reported zero pain with a full range of motion. She was back to her baseline activities and expressed satisfaction at the outcome of the surgery. She follows up as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


