The patient is a 59-year-old female who presented to our office with complaints of bilateral knee pain (left greater than right). She stated that the pain started 4 years back insidiously which has worsened over time. She is a former track and field athlete and feels her knees deteriorated due to her sporting career.
The patient is presently working in a consulting firm which requires her to be seated for long hours. She states that her knee pain is getting worse and she finds it difficult to stand from her sitting position. The patient states she previously enjoyed going for a stroll which she is now unable to do secondary to pain. She finds it difficult to bend her knees or climb stairs limiting her daily activities.
She had lower back surgery done 2 years ago with excellent relief from symptoms. The patient also stated she had an open reduction and internal fixation with a screw secondary to slip and fall in left upper tibia 20 years ago. She had an episode of myocardial infarction 5 years ago and is currently on coronary artery disease medications. Her hypertension is well controlled with medications.
The patient stated she had multiple knee gel injected but the initial pain relief didn’t last. She also had a trial of conservative management in the form of braces, pain medications, and physical therapy but with only temporary relief. She stated she now has lifestyle limiting knee pain.
The patient’s physical examination revealed a horizontal scar over the left tibial tubercle. There was mild swelling with genu varus and flexion deformity. The range of motion of the left knee was found to be 10-95 degrees. Medial joint line and medial patellar facet tenderness were elicited. The patient was visibly under distress due to pain. She stated she wanted to explore the options of knee arthroplasty.
Her imaging studies revealed tricompartmental osteoarthritis of the left knee with a retained hardware (bolt) in the left proximal tibia. After assessing her medical conditions and physical examination she was deemed as a candidate for custom knee replacement. She was advised to undergo only the left side in view of the previous history of myocardial infraction and then proceed for right knee.
Risks and benefits were explained at length to the patient. She was made aware of alternative treatment options. She decided to go ahead with a left custom knee replacement.
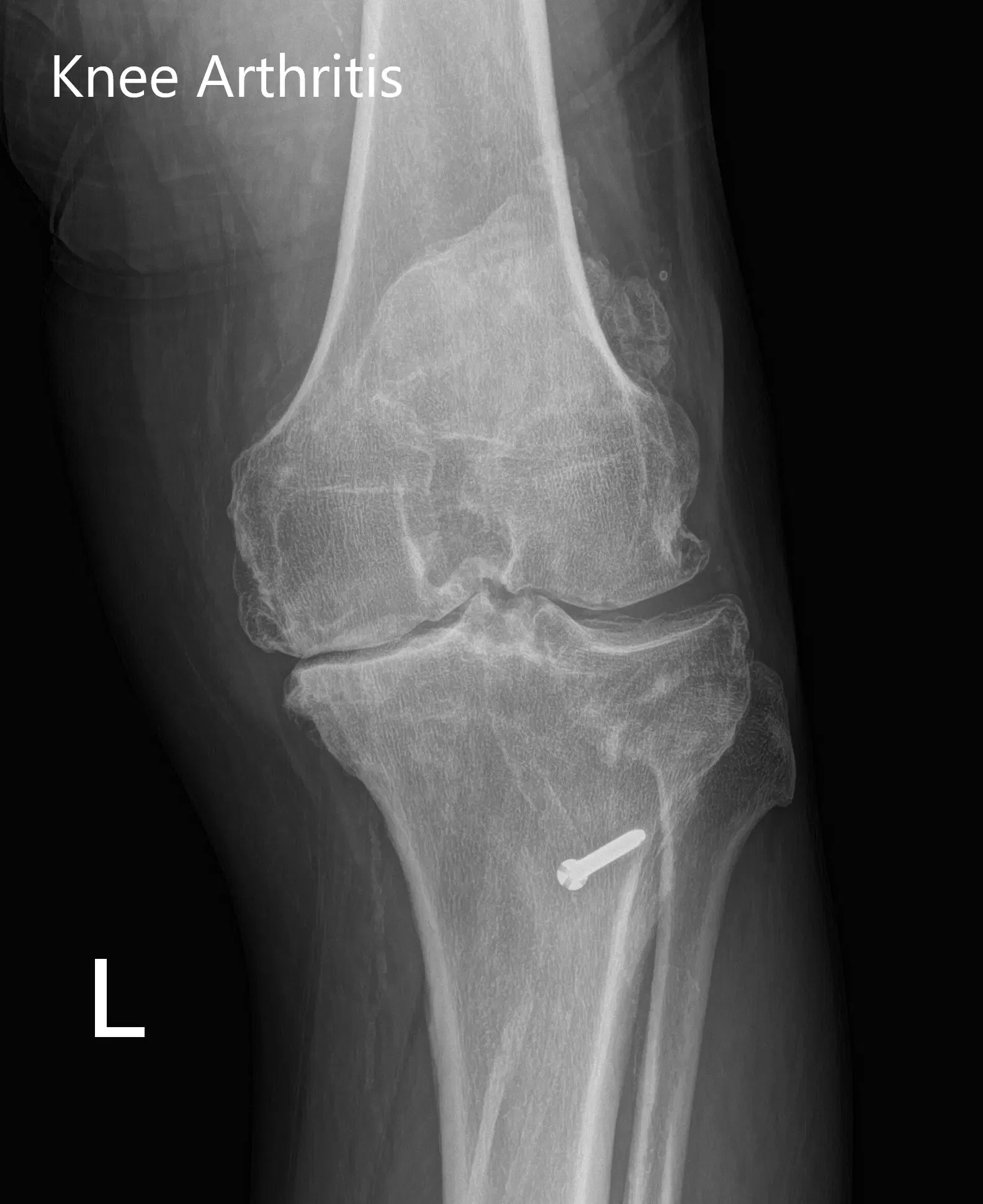
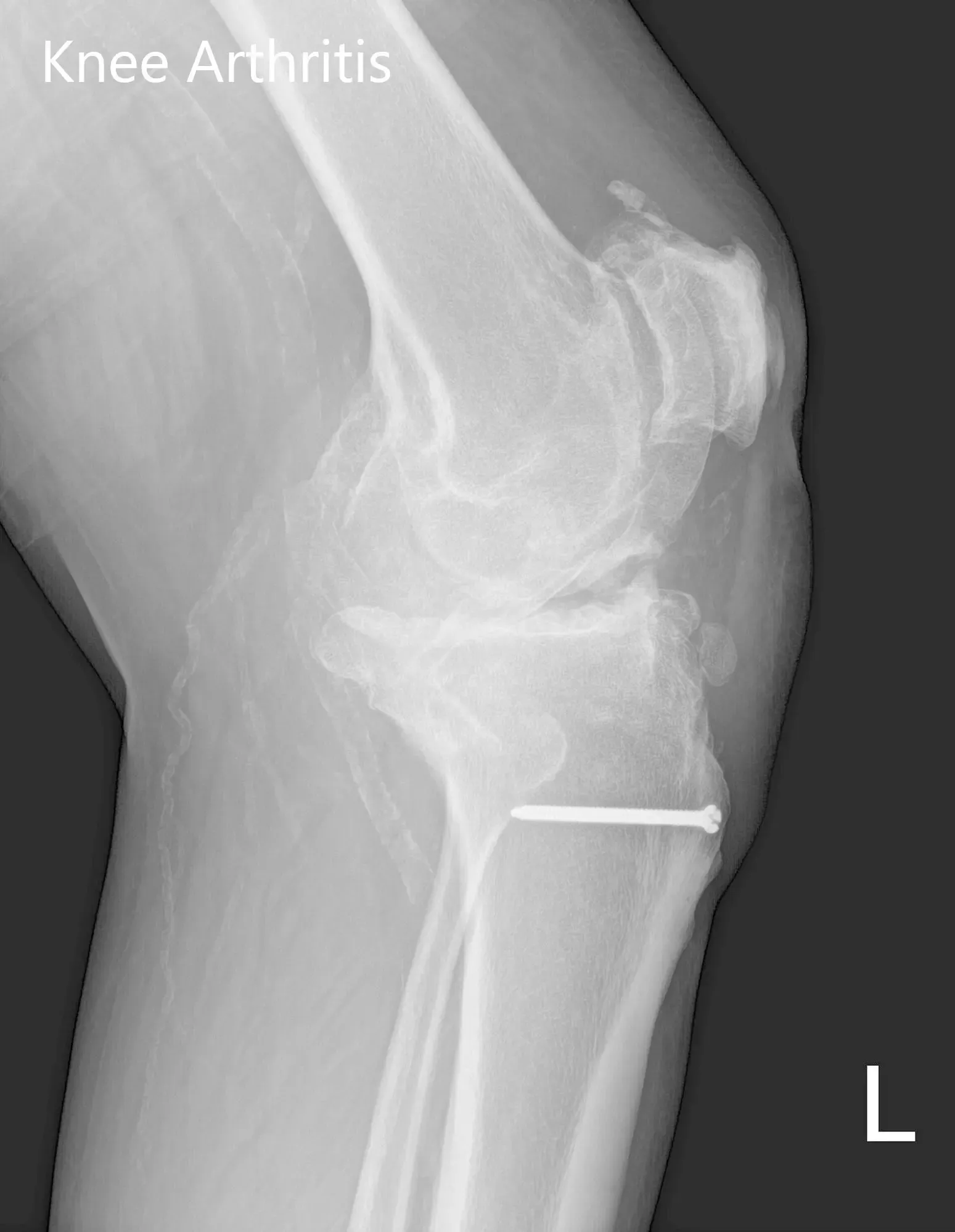
Preoperative X-ray of the left knee showing AP and lateral views with degenerative osteoarthritic changes and retained hardware in the proximal tibia.
The patient underwent a preoperative CT scan a few weeks before the surgery. The data was used to create custom 3D printed instruments and patient-specific unique implants. The data was utilized to create a preoperative plan outlining bone cuts and femoral offsets. The custom implants ensure that maximum bone is preserved and the biological biomechanics are recreated.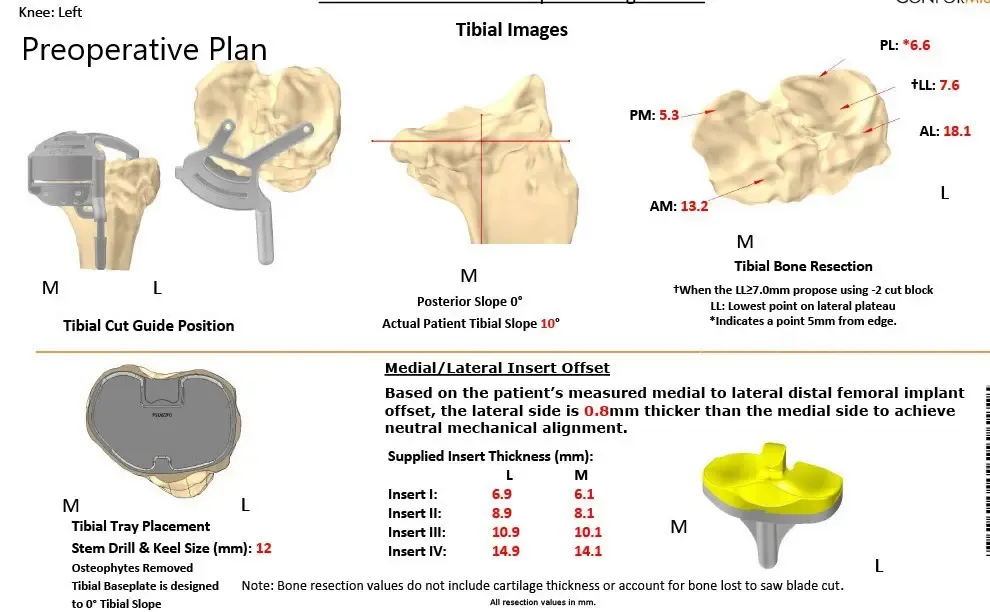
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement in a 59-year-old female.
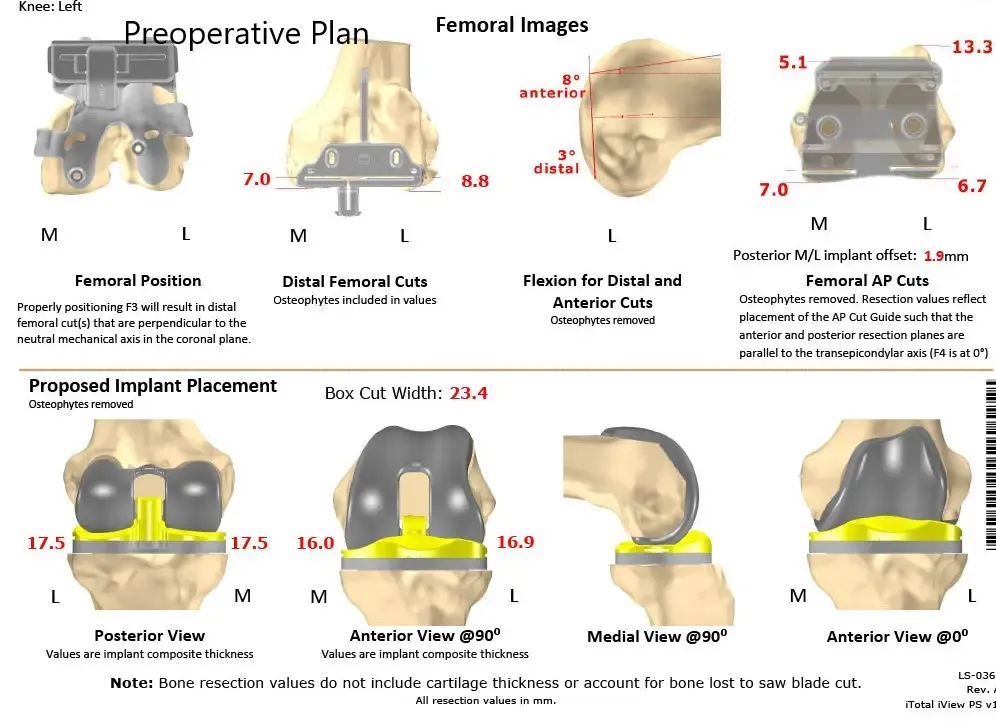
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement in a 59-year-old female (scan 2)
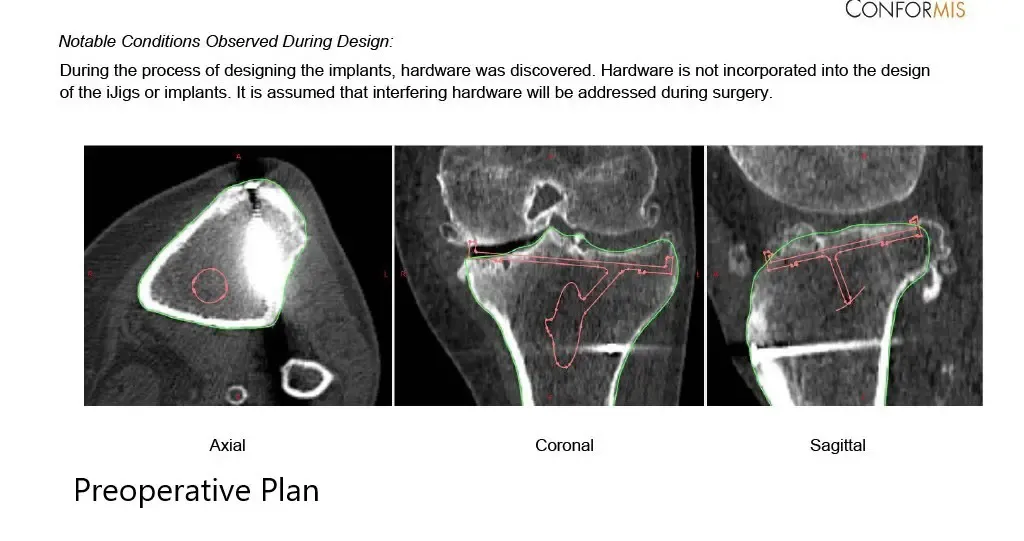
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement in a 59-year-old female (Scan 3)
Operative report:
Implant – Left total knee arthroplasty using custom femur, custom tibia, patella, and 6-mm polyethylene
The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, alternatives were extensively discussed with the patient prior to the procedure. The patient understands that the increased risk of medical issues considering his medical problems prior to the surgery.
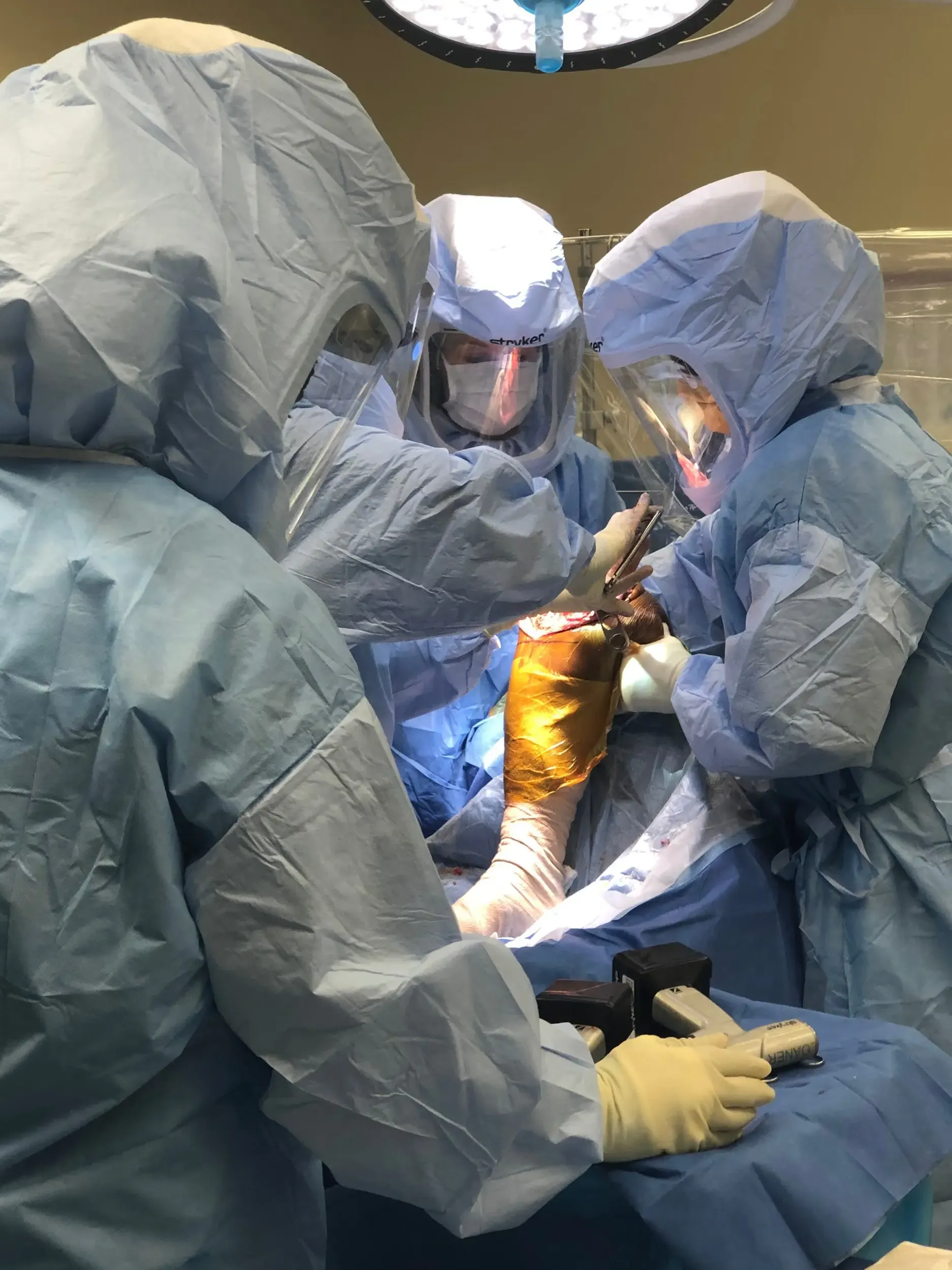
The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist. The patient was definitely positioned and the left lower extremity was then draped and prepped in the usual sterile manner. A cuff was placed and the Esmarch was used to exsanguinate the limb.
The straight incision was used for the arthrotomy. Skin and subcutaneous tissues were incised. The fascia was then divided. A medial parapatellar arthrotomy was performed and the knee was exposed. The tibia was subluxed and the tibia was prepared using the customized jig.
Attention was then turned towards the femur. Using the customized instrumentation, anterior, posterior, and chamfer cuts were then performed. Laminar spreaders were used medially and laterally, with medial and the lateral remainder of the meniscus, and the cruciates were then debrided. The posterior osteophytes were then removed.
Attention was then turned towards the patella. Patellar resection was performed. The drill holes were made in the patella. Trial patella was placed into position. Attention was then turned back towards the tibia.
The tibia was prepared. The femoral notch was prepared. Trial femur was placed into position followed by the trial poly. The knee was ranged through a full range of motion. There was no flexion contracture. Full-extension was achieved.
The trial components were then removed. Injection was given. Thorough lavage was given. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. Poly was placed into position and the knee was reduced and held in full extension with a bump on the back. The patella was then cemented into position and held in position with a patellar clamp. Excess cement was removed after the cement hardened. The patellar clamp was removed.
Thorough lavage was performed. Medial parapatellar arthrotomy was closed with Vicryl and with V-Loc. cutaneous tissues were closed with 0 Vicryl. Subcutaneous tissues were closed with 2-0 Vicryl. Skin was closed using staples. Sterile dressing was applied over the wound. The patient was then transferred to the postoperative care unit in stable condition.
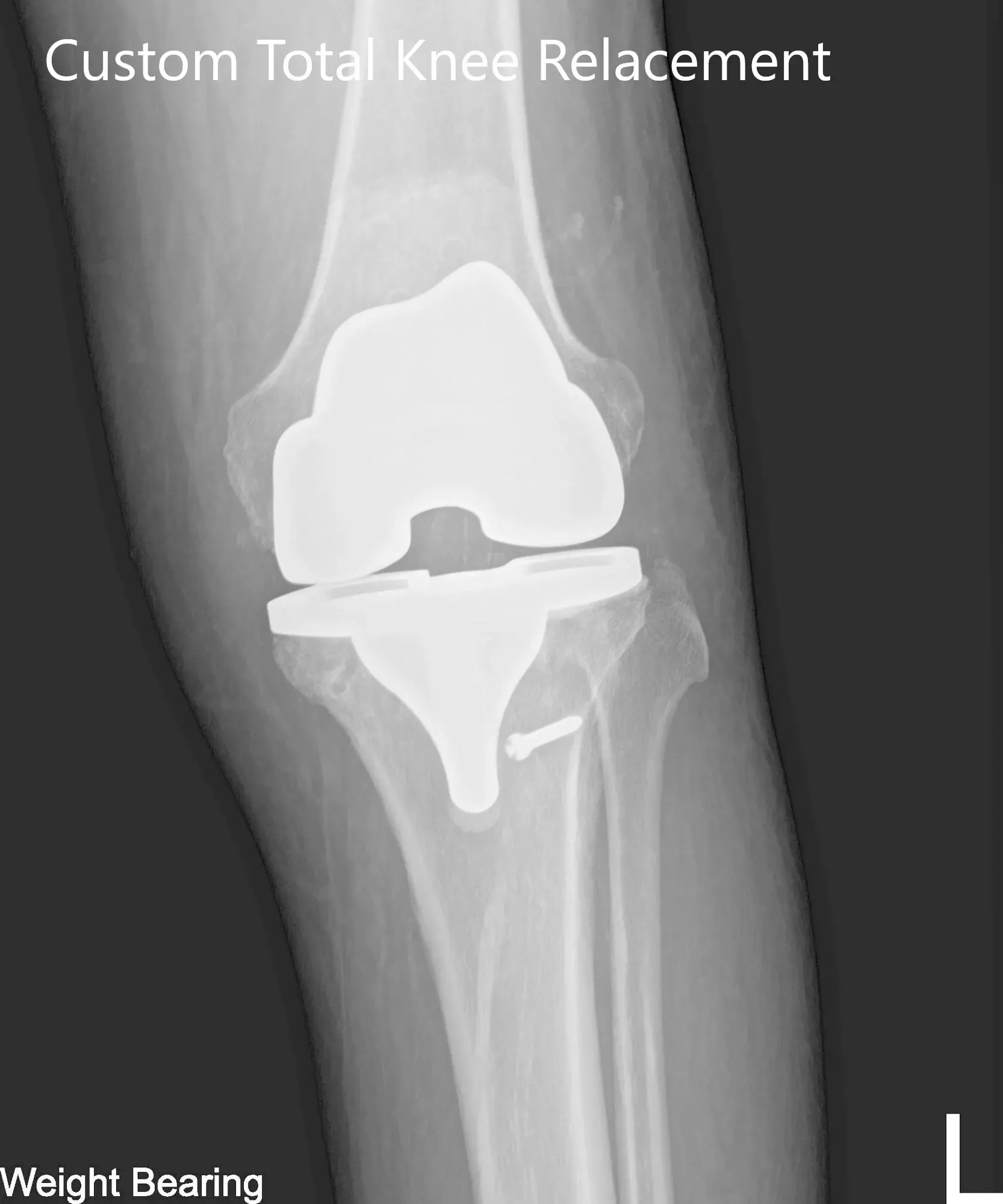
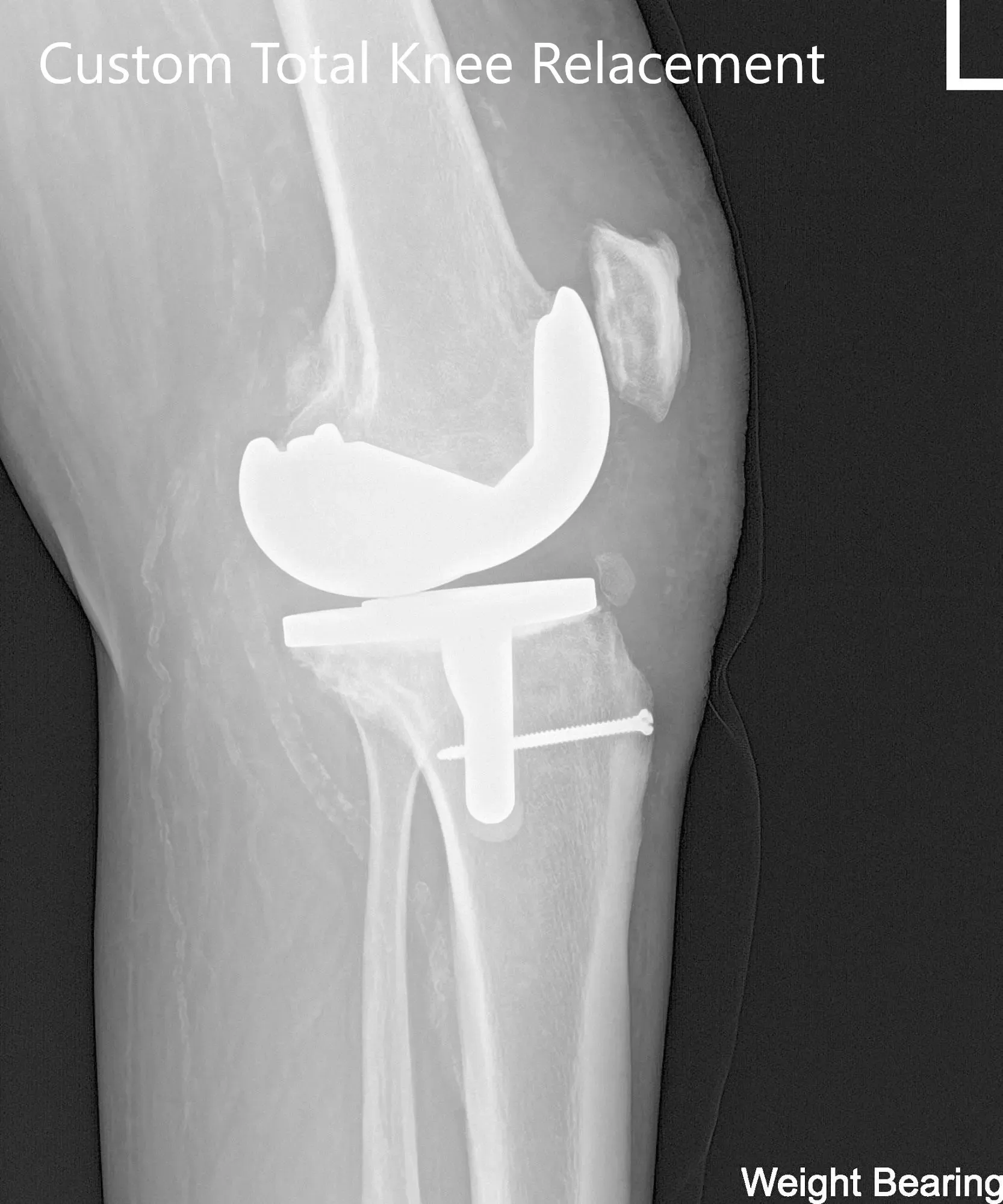
Postoperative X-ray of the left knee showing AP and lateral views
The patient had an expedited post-operative recovery. She was bearing weight walking with support the same day. Her pain was well managed on medications and she was started on aspirin 325mg BID for deep vein thrombosis prophylaxis. On her subsequent visits, she had her staples removed. Her surgical wound was clean, dry and intact.
She was started on physical therapy and home exercise program regime. The patient was compliant with the regime and demonstrated a full range of motion. She was happily back to work and enjoyed her visits to the supermarket walking. She was able to continue her daily activities and was enthusiastic about the results. She was advised to follow up for the replacement of the right knee.


