A 72-year-old female presented to our office with complaints of right hip and right knee pain. The patient stated she had a slip and fall 6 years ago. She injured her right hip and right knee. The right hip was managed conservatively while she underwent a meniscal surgery for her right knee. She states the pain has since worsened affecting her daily activities.
The pain in the right hip was located in the groin and described as a dull ache radiating to her knee. The intensity varies from mild to severe depending upon the physical activity involved. The pain was exacerbated by activities such as walking, going up the stairs, sitting, squatting and bending. The pain was better on rest but recently had been disturbing her sleep.
The patient was running a local grocery store and her work including lifting, moving, bending and driving to get supplies. During the weekend, she enjoyed going to the park with her friends. Secondary to pain, she has reduced her working hours and was unable to do the activities she enjoyed. Her husband accompanied her to the office visit and was equally distressed.
She was a nonsmoker and social drinker. Her medical history included diabetes mellitus, dyslipidemia, and hypertension, all well controlled with medications. She reported her last HbA1C was 6.2 demonstrating good control. She was currently taking metformin 1000 mg, atorvastatin 20 mg, and amlodipine 10 mg. Her past surgical history involved right knee meniscal repair and posterior lumbar interbody fusion (PLIF).
The pain in the groin was managed conservatively in the form of physical therapy. She also received right hip cortisone injections from an outside physician with minimal relief. She was currently using a cane for ambulation.
On her physical examination, her gait was bipedal, coordinated, and antalgic with a reduced stance phase on the right side. On standing, both the shoulders, anterior superior iliac spines (ASIS), pastels and medial malleolus were at the same level. There was no evidence of increased lumbar lordosis and functional/structural scoliosis.
On the supine examination, both the ASIS were at the same level. There was no scar, sinus, erythema in the Scarpa’s triangle, laterally or posteriorly of the hip. There were no enlarged inguinal lymph nodes. The right hip range of motion was restricted terminally in abduction, extension, and internal rotation.
On digital palpation, there was no supra-trochanteric shortening. Tenderness was present on the right anterior joint line. The examination of the contralateral hip, bilateral knee and ankle were normal. There was no distal neurological deficit. The bilateral lower extremity pulses were palpable and good volume.
Imaging revealed osteoarthritis of the right hip with joint space reduction and osteophytes. The patient was advised right total hip robotic replacement. The risks, benefits, and alternatives were discussed with the patient at length and she agreed with the plan.
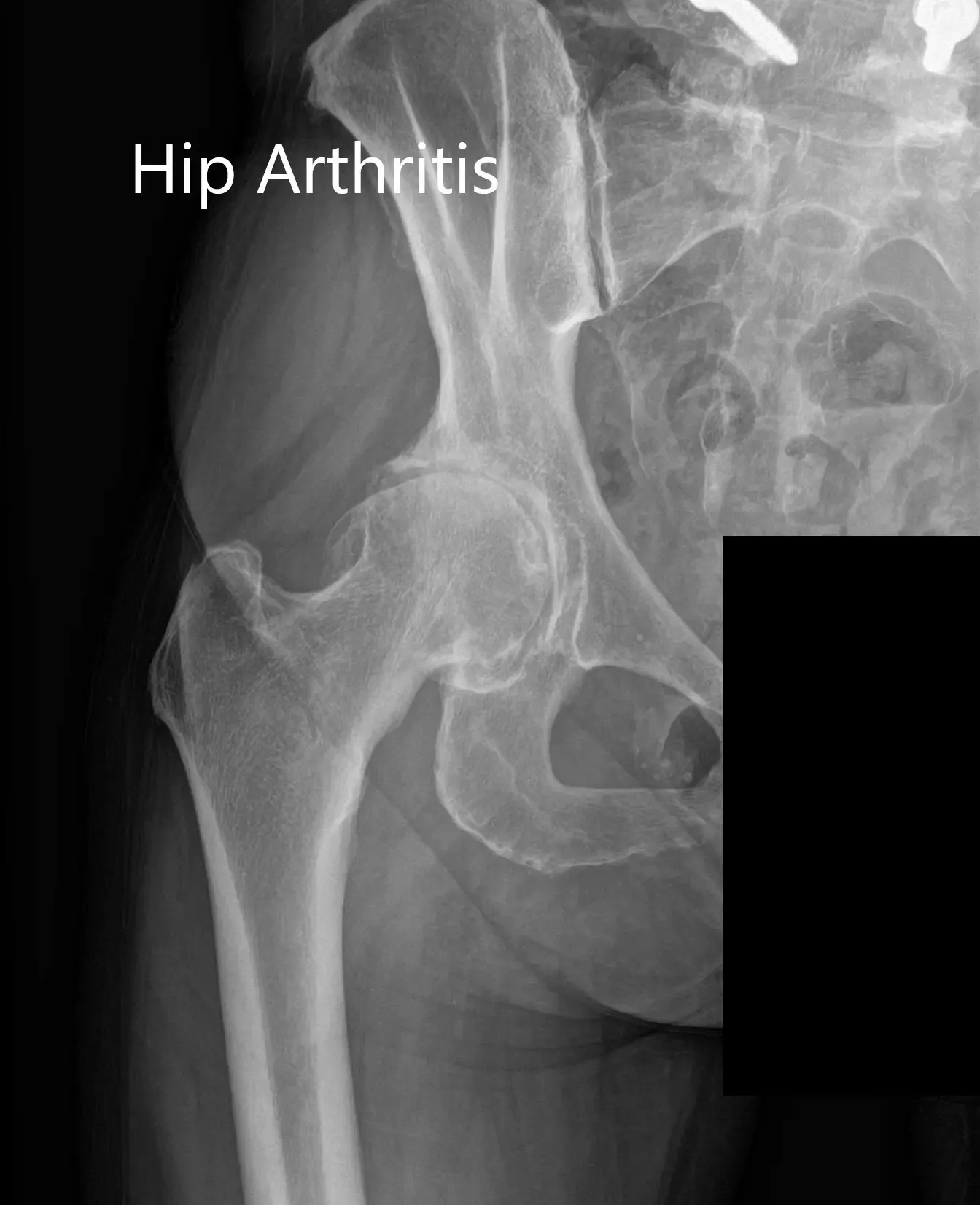
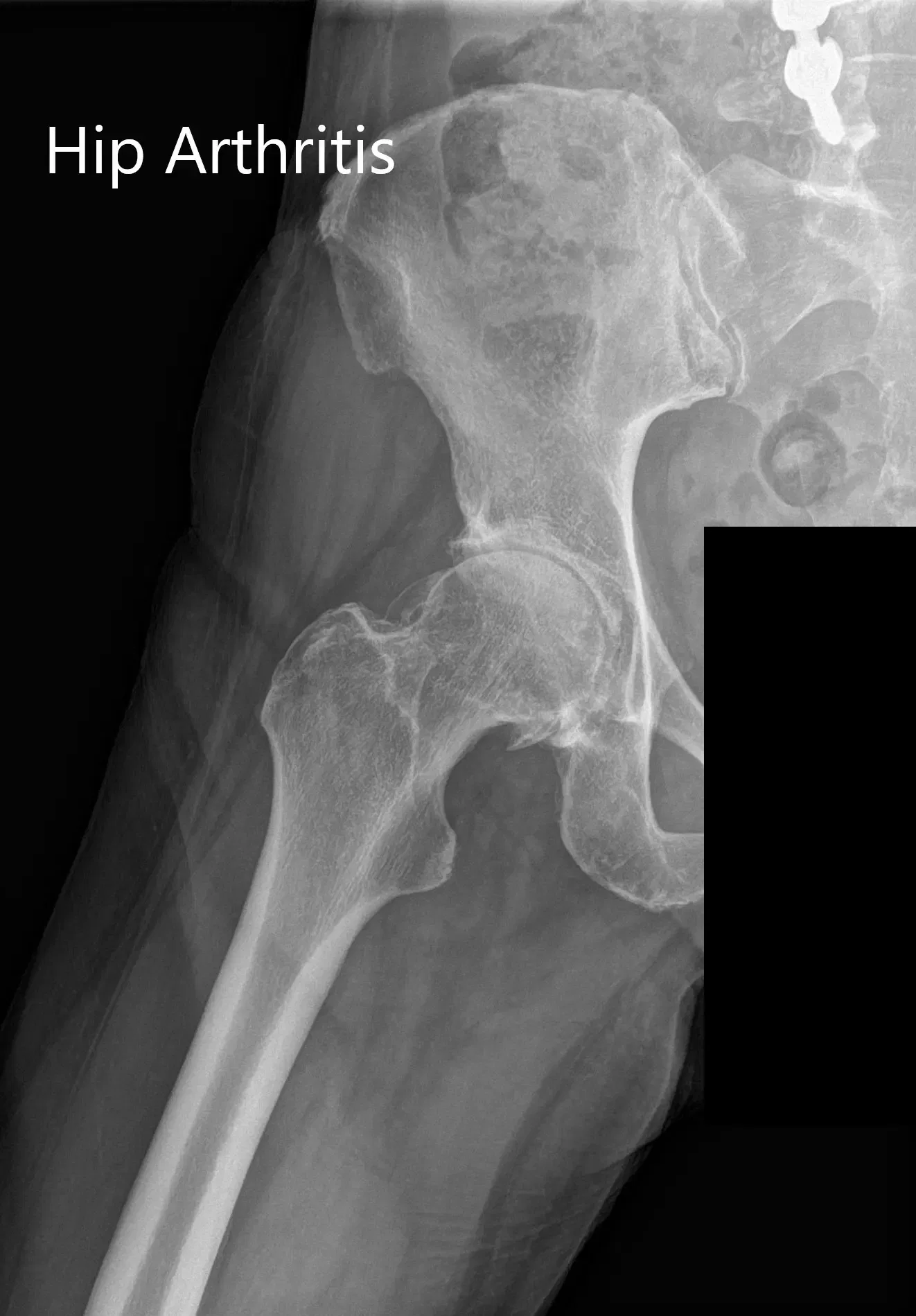
Preoperative X-ray Showing the AP and lateral views of the right hip.
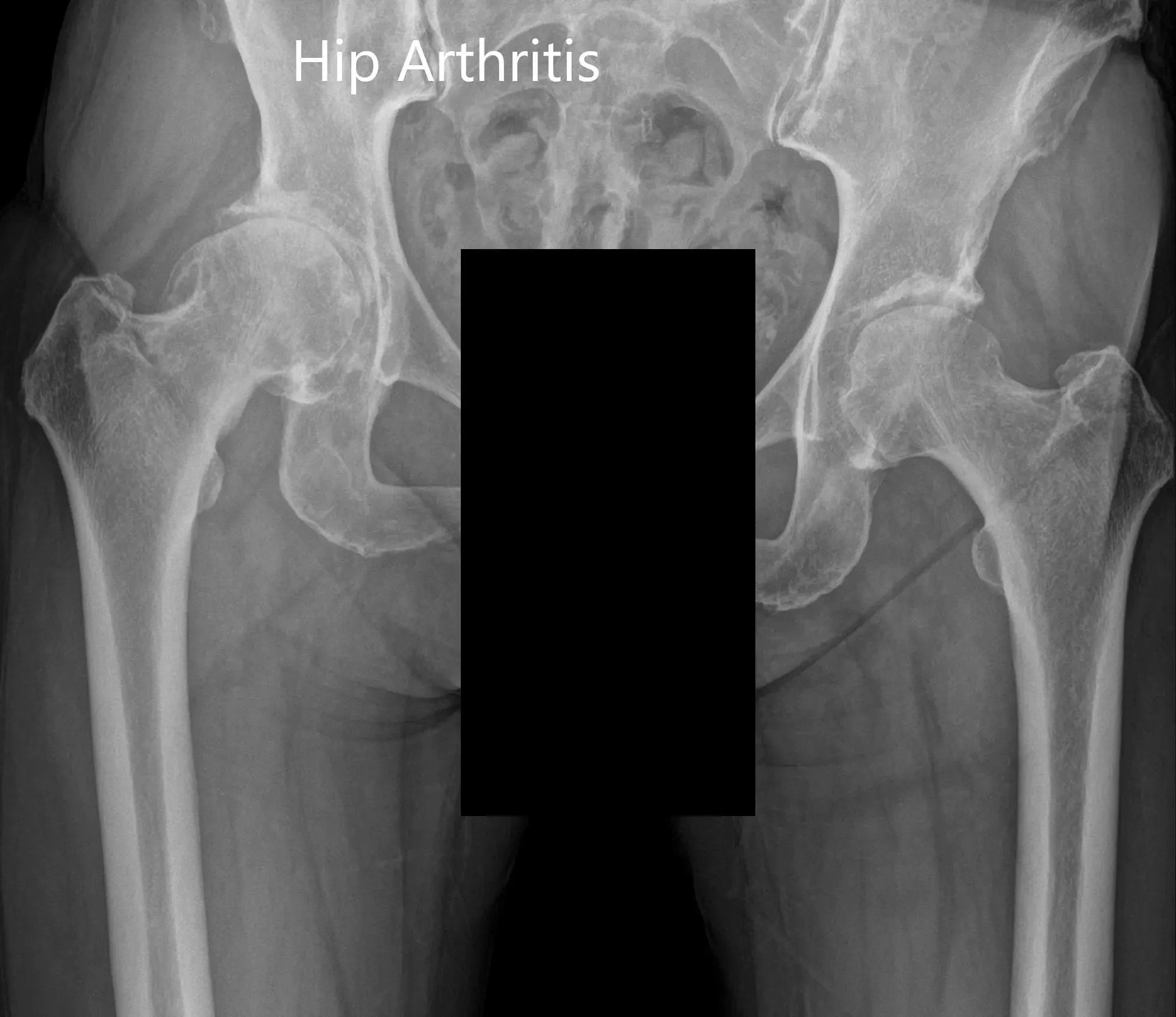
Preoperative X-ray showing the AP view of the pelvis with both hips.
OPERATION: Robotic right total hip replacement.
IMPLANTS USED: Tritanium cluster shell 52-mm with 6.5-mm x 30-mm screw with a Trident shell. Zero degrees poly with a 127-degree stem with a ceramic head, outer diameter 32-mm minus 4.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining the informed consent signing in the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist.
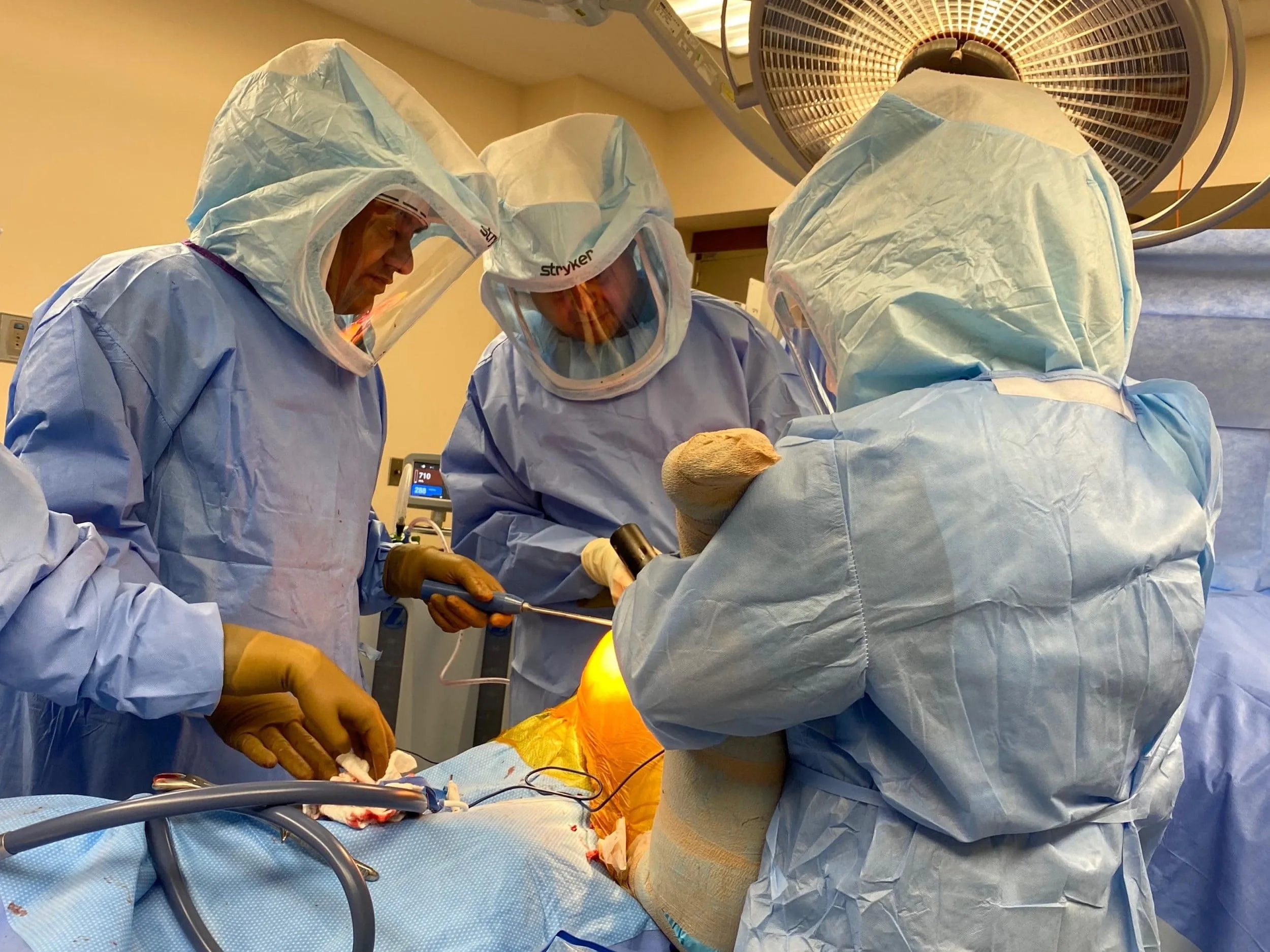
The patient was then definitively positioned, and the right hip was then draped and prepped in the usual sterile manner. The external fixator was placed over the right iliac crest and the arrays were then assembled.
The incision was then made centered over the greater trochanter, and skin and subcutaneous tissues were incised. The fascia was then divided.
The posterior soft tissue structures were then taken down and tagged for future repair. The marker was placed in the femur and over the acetabulum. Registration was performed for limb length.
The hip was then dislocated. Neck resection was made and the lesser trochanter to center measurement was measured before the neck resection. The acetabulum was then exposed. The remainder of the labrum was then debrided. The robot was then used for reaming the acetabulum.
The acetabulum was then measured and the cup was then placed into position in the correct abduction anteversion using the robot. The placement was then confirmed visually. The reaming was also confirmed visually before the placement of the implant. The screw was then placed into position in the correct place and the poly was then placed over the cup.
Attention was then turned towards the femur. The femur was then sequentially broached. The final broach was left into position. The head was placed in position. The lesser trochanter center distance was then measured and the hip was then relocated. The limb length was then confirmed with the robot and was found to be accurate.
The hip was then dislocated. Trial components were then removed. The final components were then placed into position. The confirmation of the limb length was then made again with the robot. Markers in the acetabulum and the femur were then removed and thorough lavage was given. The injection was given for pain control.
Posterior soft tissue structures were then tagged to the greater trochanter through transosseous tunnels. Fascia was then closed with Ethibond. Cutaneous tissues were closed with Vicryl. Subcuticular: tissues were closed with O Vicryl. The skin was closed with staples.
The external fixation was then removed and closure was performed again in layers. The skin was closed using staples. Sterile dressing was then applied to the wound, and the patient was then transferred to the postoperative care unit in stable condition.
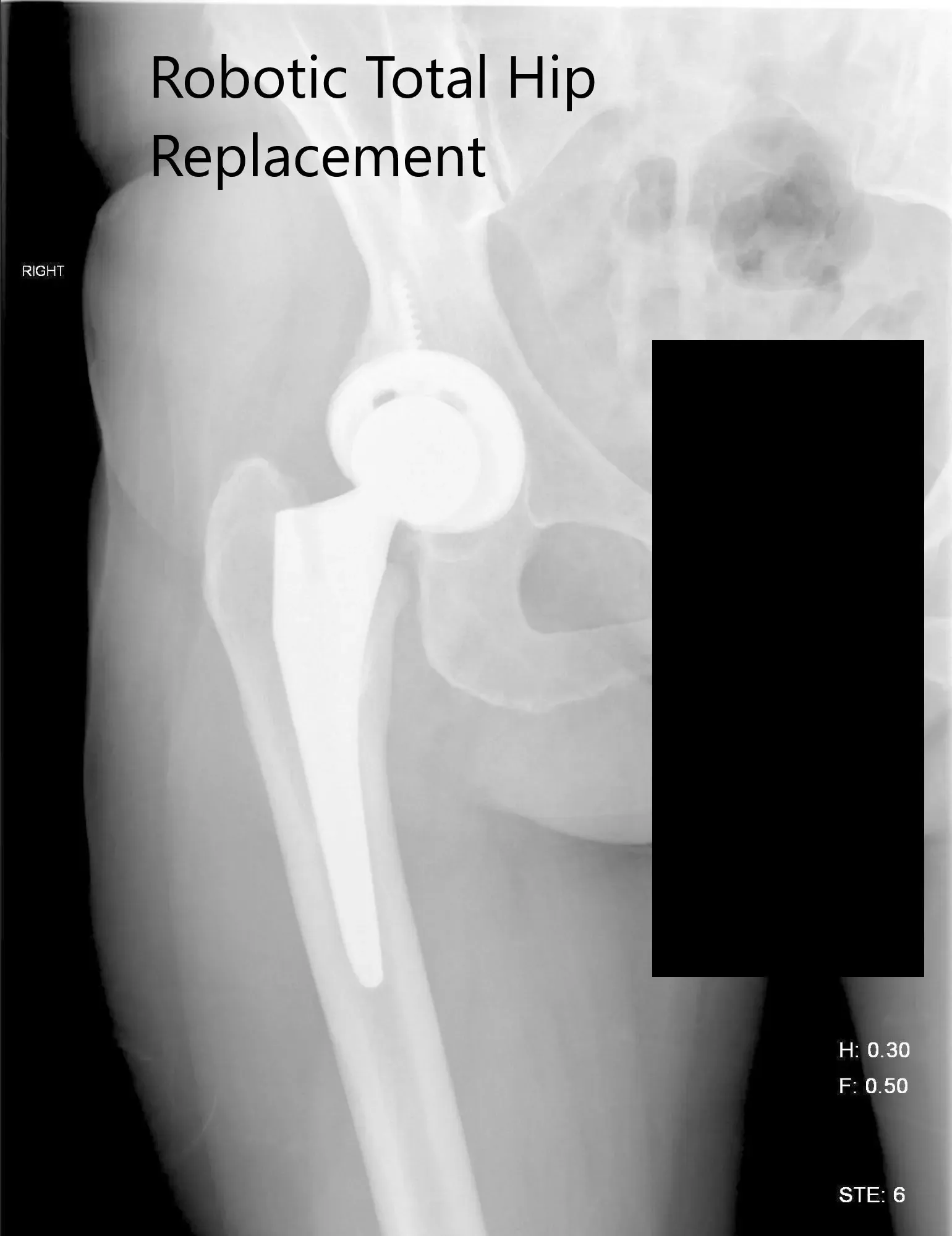
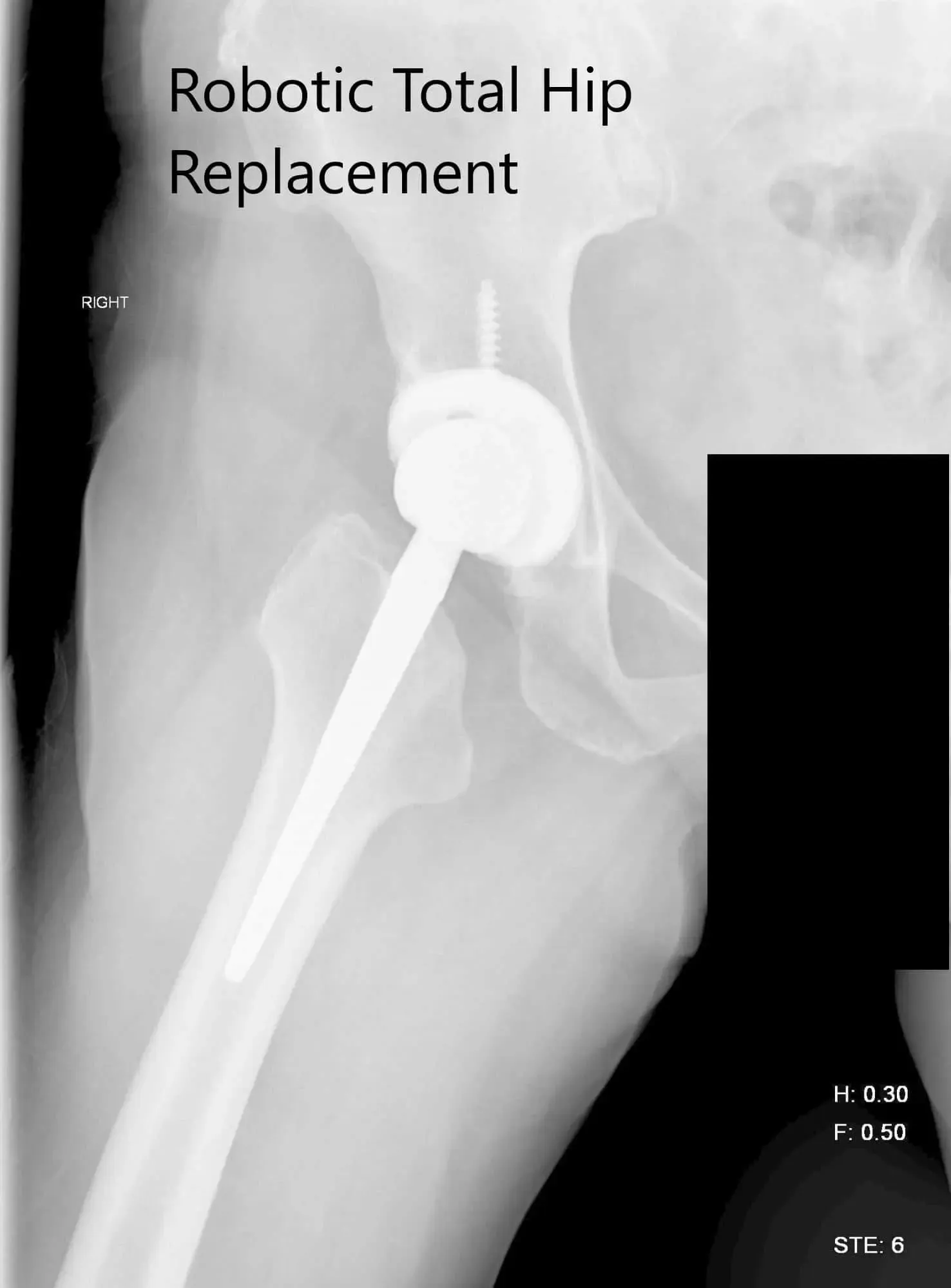
Postoperative X-ray of the right hip showing AP and lateral view.
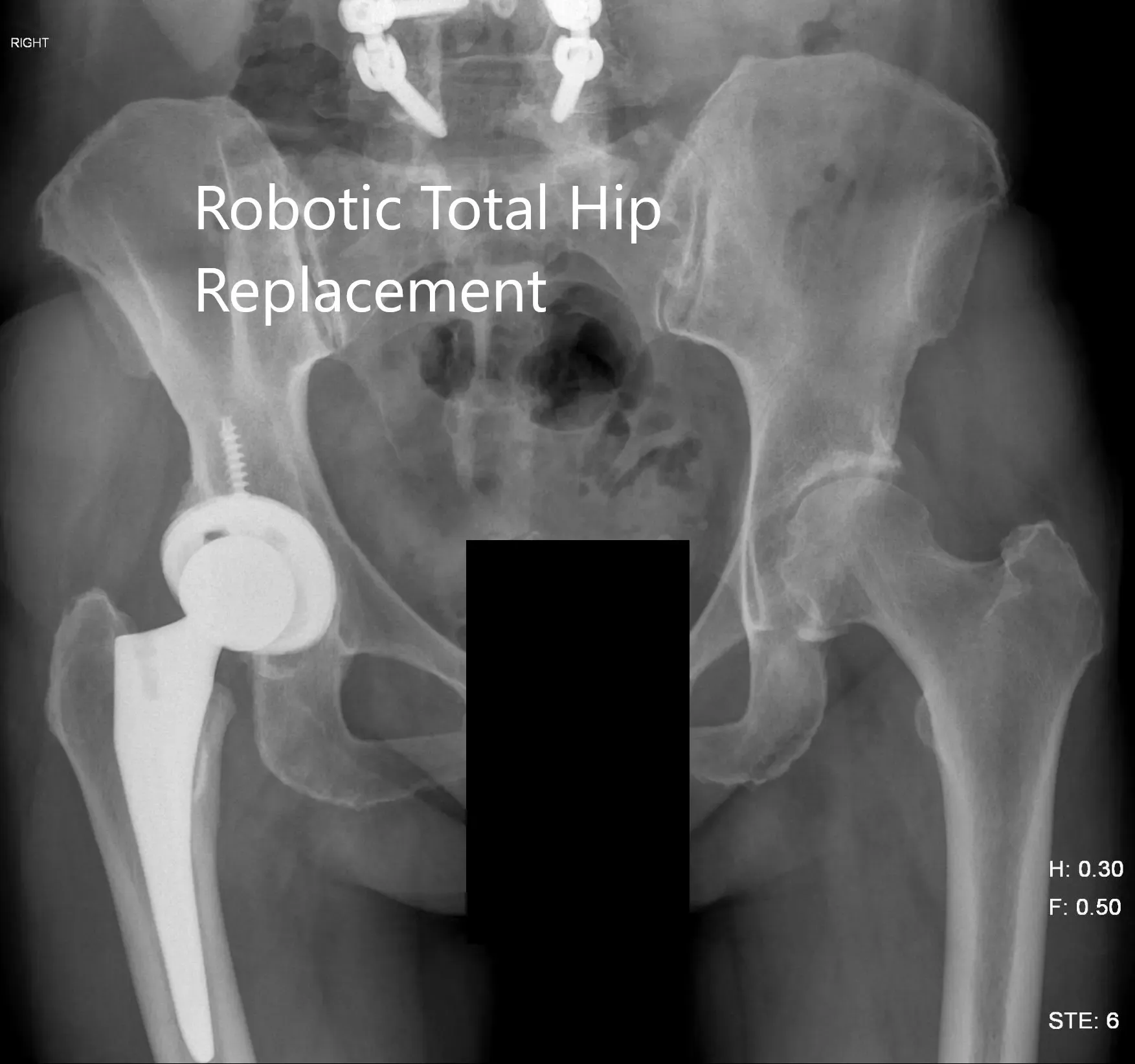
Postoperative X-ray of the pelvis showing AP view.
The patient had an excellent recovery postoperative. She was compliant with hip precautions and the use of an abduction pillow. The pain was well managed with oxycodone and acetaminophen. Deep vein thrombosis prophylaxis was started in the form of aspirin 325 mg BID for three months. Her vitals were stable postoperative and there was no neurological/vascular deficit in the right lower extremity postoperative.
The patient was allowed weight bearing as tolerated. The sutures were clean, dry, intact and were removed 15 days postoperative. She underwent physical therapy focusing on the range of motion exercises and muscle strengthening. She was educated about fall prevention and had gait training.
Three months later, she was driving her car, back to her business and was happily enjoying her weekends at the park. She had concluded her physical therapy and was gradually weaned off hip precautions. She was extremely happy with the outcome.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


