A 83 year-old gentleman who had previously had a Total Hip Replacement performed at another institution approximately 13 years prior to being referred to us. He initially recovered well from the procedure and had been asymptomatic for much of this time, but in the last 18 months he had been experiencing feelings of instability and “giving way” in his hip.
He had not experienced a full dislocation during this time, but describes more than one occasion of “feeling like it was going to pop out of joint”. The surgeon that had performed the initial surgery had since retired from practice, so he was referred to us for further evaluation.
His medical history was significant for COPD, Hypertension, High Cholesterol, Benign Prostatic Hypertrophy and Gout. He took numerous regular medications pertaining to these diagnoses, but no anticoagulants or immunosuppressant drugs. He endorsed no known drug allergies, had previously smoked but quit over a decade ago.
Physical examination of his operative hip was largely unremarkable – range of motion was within normal limits and pain-free. Examination of his knees, lower back and gait revealed no additional pertinent information.
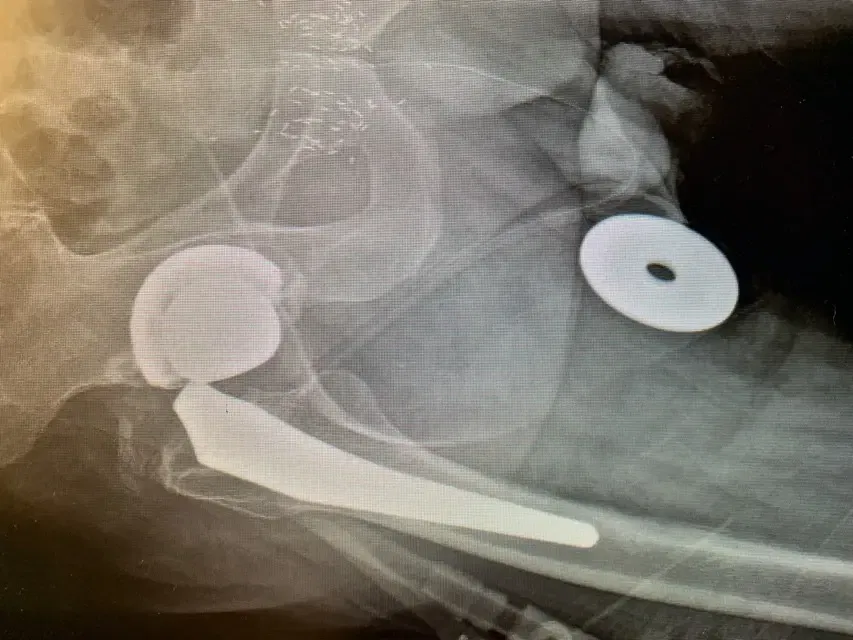
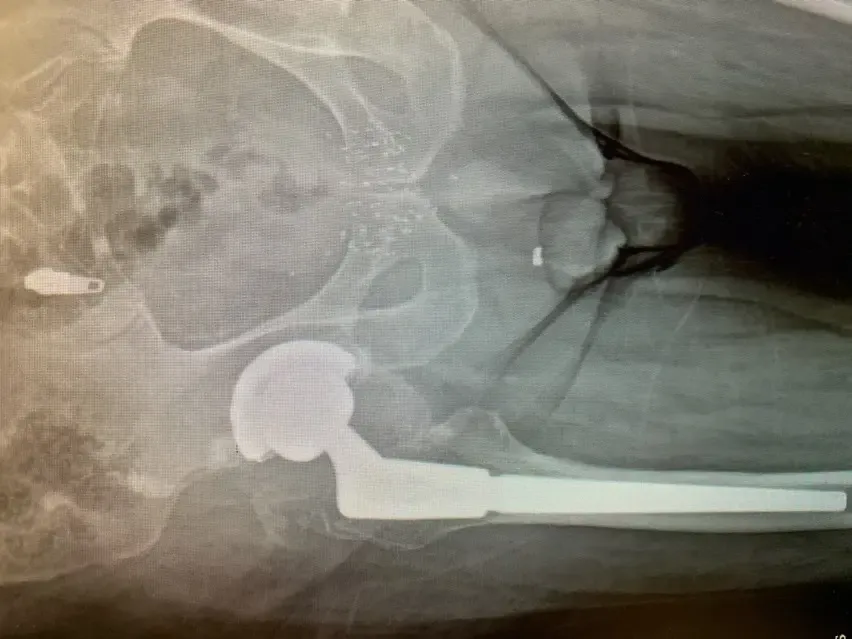
Plain film radiographs revealed thinning and “penciling” of the neck of the femoral component, indicating likely fretting corrosion at the trunion – also known as “trunnionosis”.
In fact the radiographs suggested the trunion had become so corroded that it had fractured. Further inquiry revealed the type of component used in the initial replacement surgery has since been shown to suffer from this phenomenon at a higher rate than others – though this was not known at the time.
I recommended to Mr. JF that we perform a revision surgery in a timely fashion to avoid further damage to the components, and possibly his native anatomy as a result. He consented to this, and we planned to perform a revision surgery in an expeditious manner.
We utilized the same surgical approach as the previous surgeon used – in this case the lateral approach – and exposed the hip joint in a careful and meticulous fashion.
Once this was completed, we dislocated hip and retrieved the femoral head component which revealed that the neck of the femoral component had been pistoning within the head component, leading it to have become eroded down to resemble the tip of a pencil.
We carefully removed the femoral component and the plastic liner of the acetabular component – testing of the metal shell revealed it to be stable so it was decided this part of the original procedure would remain intact.
We prepared and inserted the revision femoral component without event and trialed femoral head components with trial acetabular liner components to ensure the hip remained stable. Once we were satisfied with our component sizes, definitive components were placed and the procedure was completed.
6 weeks following surgery, Mr. JF had recovered most of his strength, had been returned to his former pain-free status and has not had any recurrent episodes or feelings of instability to date.