The patient was a 68-year-old male a retired banker presenting to our office with complaints of worsening bilateral knee pain (left greater than right) for the last 4 years. The pain was dull aching to sharp in character associated with joint crepitus. The pain was especially worse after getting up from a chair after sitting for a long time.
The patient stated the pain limited his daily activities such as walking, climbing stairs and getting up. He no longer enjoyed his hobbies of gardening and playing golf. The patient stated he was apprehensive about precipitating his knee pain with activities.
Recently he stated the pain was hampering his sleep which reduced his productivity during the day. The patient had previously tried conservative management in the form of physical therapy, pain medications, knee injections, and heat pads but with no relief.
His physical examination revealed tender joint movements with crepitus. There was tenderness on the medial joint line and medial patellar facet. Imaging studies revealed bicompartmental Osteoarthritis of the knee with joint space obliteration of the medial compartment and the patellofemoral compartment.
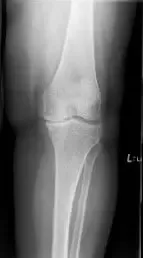
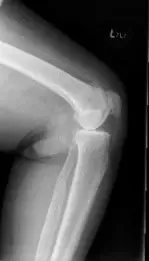
Pre operative X-Ray of the left knee showing AP and lateral views
The patient was a nonsmoker with comorbidities of hypertensive and hyperlipidemia controlled with medications. After assessing his medical conditions and requirements he was found to be a candidate for surgical intervention in the form of total knee replacement with custom implants and instruments.
Risks, benefits and potential complications were explained to the patient in detail as well as alternatives to surgery were discussed with him. The patient agreed to go ahead with the surgery.
A few weeks before the surgery CT scans of the patient’s knee, including the hip and knee was performed to assess his knee anatomy and correct biomechanics. The images were then used to construct unique patient-specific implants and instruments.
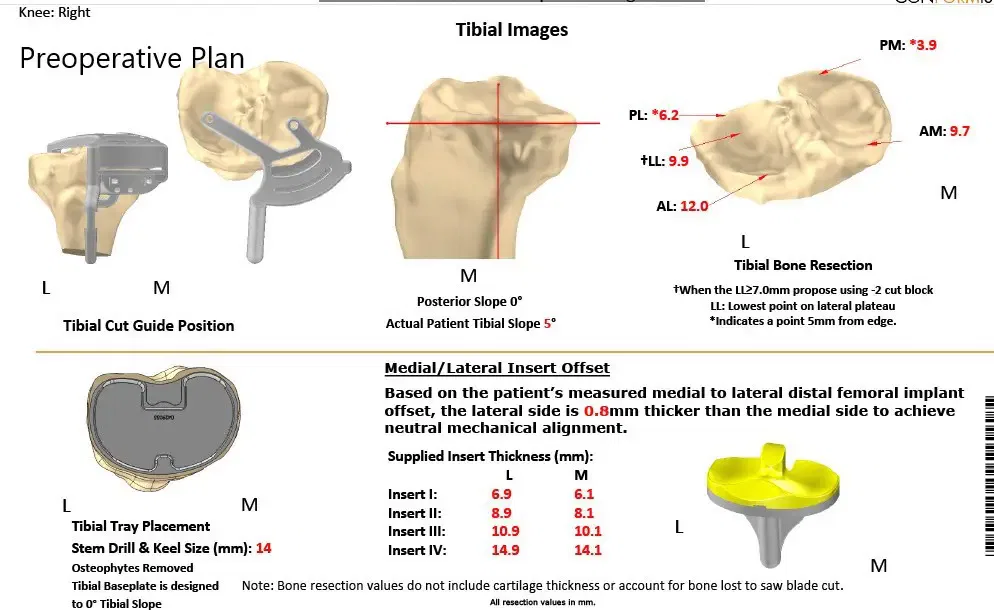
Complete Orthopedics patient-specific surgical plan for a left custom total knee arthroplasty in a 68-year-old male.
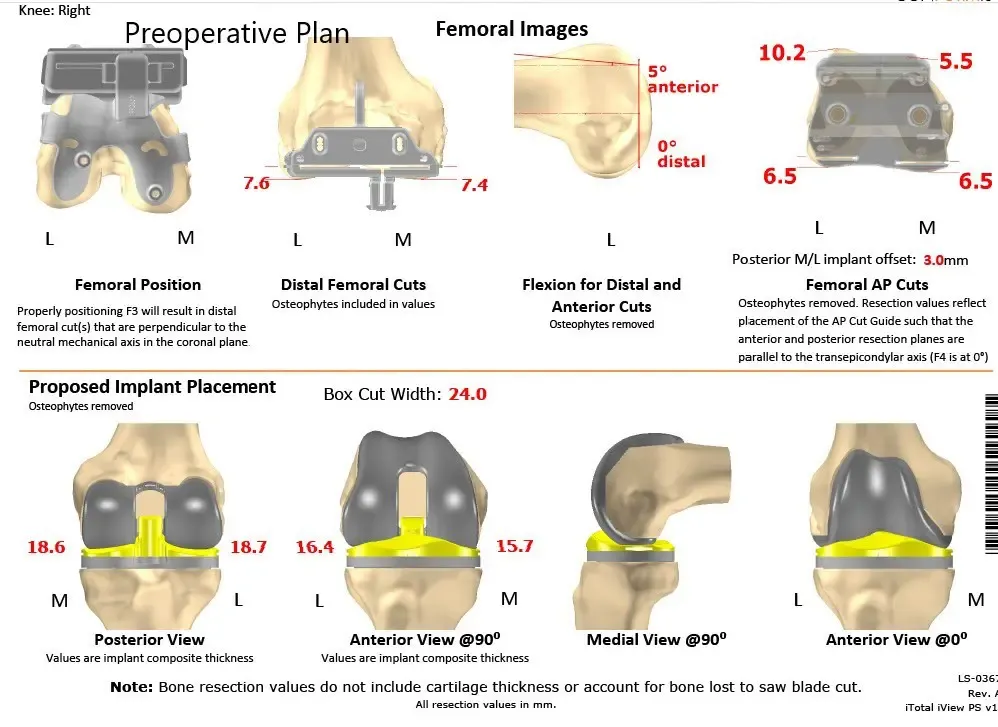
Complete Orthopedics patient-specific surgical plan for a left custom total knee arthroplasty in a 68-year-old male (scan 2)
Operative report:
The patient underwent custom left total knee replacement.
Implants used: 8 mm posterior stabilized polyethylene with tibial tray, femoral implant 32 mm, 6 mm thickness polyethylene with an 8 mm polyethylene insert.
Anesthesia was obtained by the anesthesiologist. The left lower extremity was then draped and prepped in the usual sterile manner. A straight incision was placed over the knee joint. Skin and subcutaneous tissues were incised and a medial parapatellar arthrotomy was then performed.
The medial site of the tibia was then exposed and fat pad was resected. The femoral guide was placed into position and the distal cut was then performed. Chamfer cuts were then performed using the chamfer cutting guides. Attention was then turned towards the tibia. The tibial cut was then performed using the tibial cutting guide. Bone was removed.
Lamina spreaders were used medially and laterally and the remainder of the meniscus was debrided. Balancing was performed. The notch cut was then performed. Attention was then turned towards the patella. The patellar resection was then performed and drill holes were made in the patella.
Trial patella was then placed into position. Trial femur was placed into position. Trial tibia was placed into position. The poly was placed over the tibia and the knee was then reduced.
Knee was trialed through a full range of motion and the knee was stable. The patellar tracking was excellent.Trial components were then removed. Injection was given.
Femur was cemented into position followed by the tibia. The poly was then placed over the tibia. The knee was then reduced and held in full extension with a bump under the ankle. Patella was then cemented into position. Excess cement was removed. The patella was held in place with the patella clamped. After the cement hardened, the clamp was removed.
Thorough lavage was given. Medial parapatellar arthrotomy was closed with Stratafix. Cutaneous tissues were closed with Vicryl. Subcuticular tissues were closed with Vicryl. The skin was closed using staples.
Sterile dressing was then applied over the wound and the patient was then transferred to the postoperative care unit in stable condition.
The patient was discharged from the postoperative care after 28 hours and was able to walk with support bearing weight. Patient-reported no complications and was given aspirin for DVT prophylaxis. There were no signs of infection on the surgical wound in the subsequent visits and the skin staples were removed.
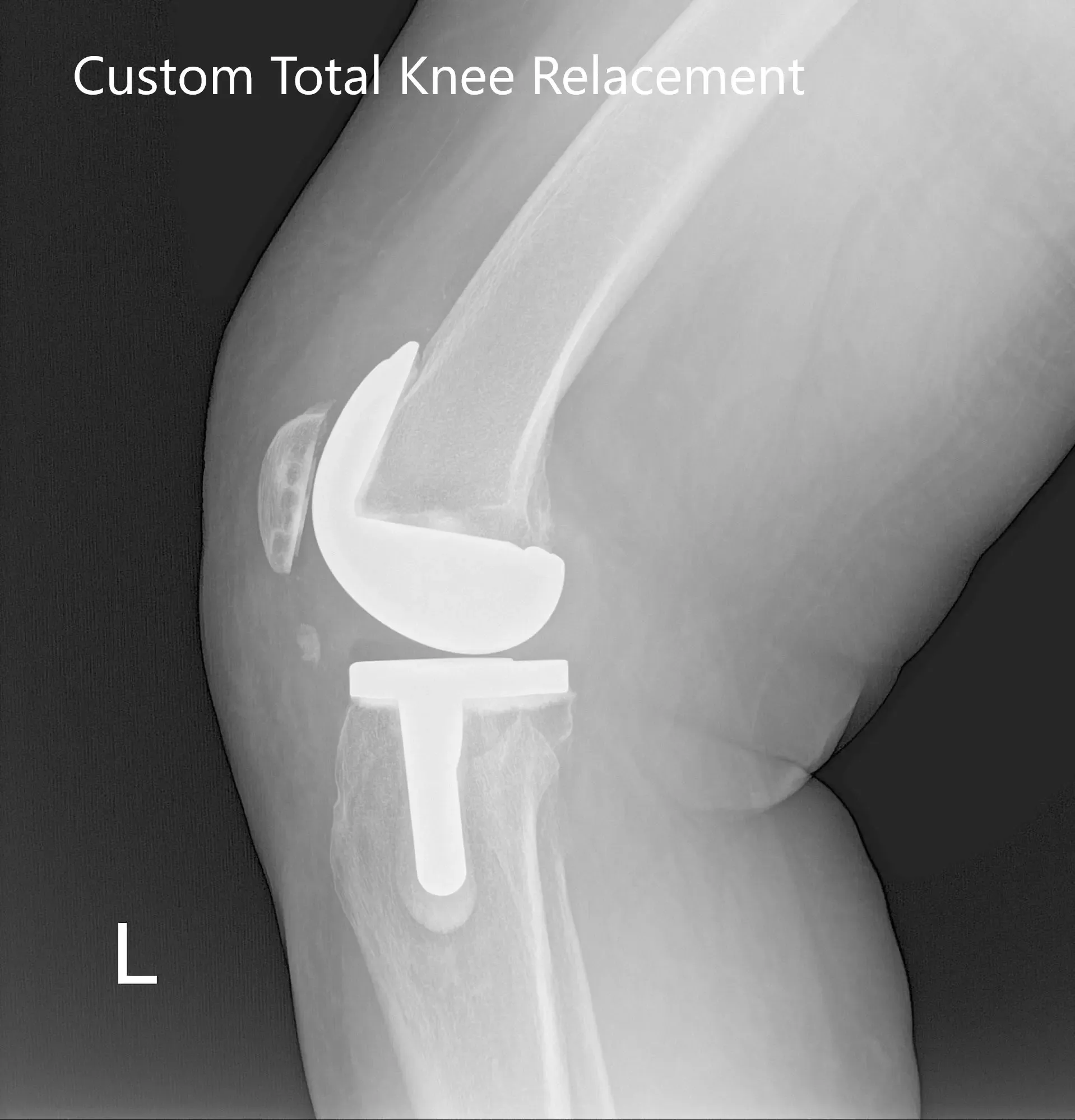
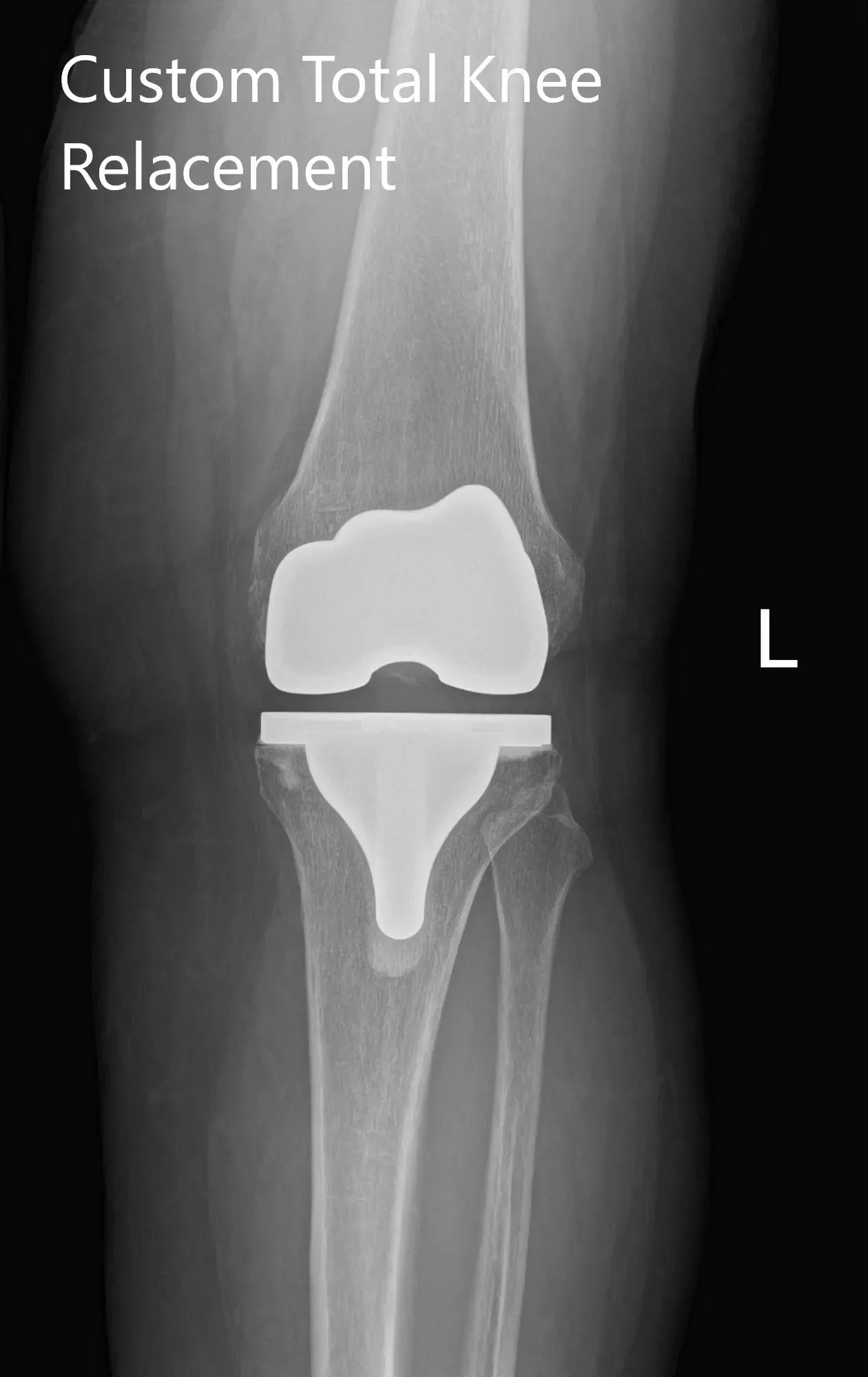
Post Operative X-Ray of the left knee showing AP and lateral view
In subsequent visits after 3 months, the patient demonstrated excellent pain free range of motion of the left knee. He stated he had been compliant with his home exercise program and physical therapy. The patient has since returned back to playing golf and feels no discomfort bending his knee while gardening.
He is happy with the outcome of the surgery and states he experiences less pain on the right knee due to offloading. The patient reports a natural feeling knee on the operated side. He follows up as needed.


