A 66-year-old female presented to our office with complaints of worsening pain in her left knee since last year. She first noticed the pain two years ago but didn’t seek any medical treatment then. She saw a physician last year who suggested her a knee replacement but she didn’t go ahead with it.
The pain started insidiously without any history of trauma/twisting injury. The pain was primarily located along the inner side of the left knee. The pain was a dull aching in character and non-radiating. The severity was described as moderate (6/10).
She was a registered nurse working at a hospital but currently out of work due to pain. She reported the pain limited her walking tolerance to less than a block. She found it extremely difficult to go up and down the stairs. Her work demanded her to frequently move, stand for a prolonged time, bend, and lift patients of the beds. She expressed discomfort at performing even her daily tasks at home.
She had previously tried physical therapy, pain modalities such as transcutaneous electrical nerve stimulation (TENS), ice packs and cortisone knee injections. The relief from all forms of conservative management was only temporary. She felt she had exhausted all her conservative treatment options.
She was a nonsmoker and nondrinker. Her past medical history was only positive for hyperlipidemia and hypertension, both well controlled with medications. She had a tubal ligation and right shoulder arthroscopic rotator cuff repair in the past.
On physical examination, her gait was antalgic, with a reduced stance phase on the left side. There as mild swelling in the left knee. Tenderness was present along the medial and lateral joint line, as well as on the patellar facets.
The range of motion was full of joint crepitus and restricted secondary to pain (20 degrees to 80 degrees). The skin overlying the left knee was normal with no scar marks or sinus tracts. There was no local rise in temperature.
The examination of the right knee, bilateral hips and ankles were normal. There was no evidence of distal neurological deficit. The bilateral lower extremity pulses were good volume and comparable.
The images studies revealed tricompartmental osteoarthritis of the left knee. Considering lifestyle limiting knee pain, the patient was advised to undergo customized left knee replacement. Risks, benefits, and alternatives were discussed with the patient and her family. They all agreed to go ahead with the surgery.
A few weeks prior to the procedure, a CT scan of the lower extremities was obtained. Using the accurate anatomy and biomechanics data, unique patient-specific implants and instruments were made. They ensured less invasive procedure work minimum bone loss. A preoperative plan was also made to aid in the surgery.
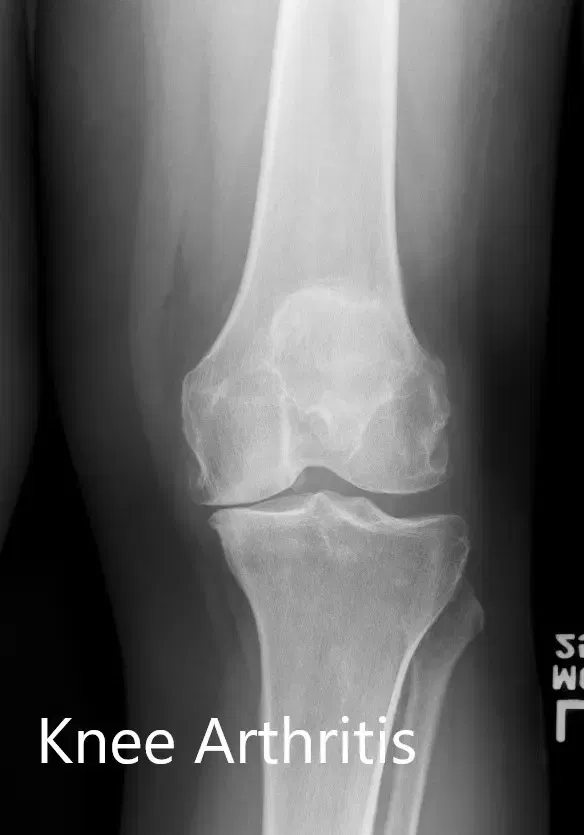
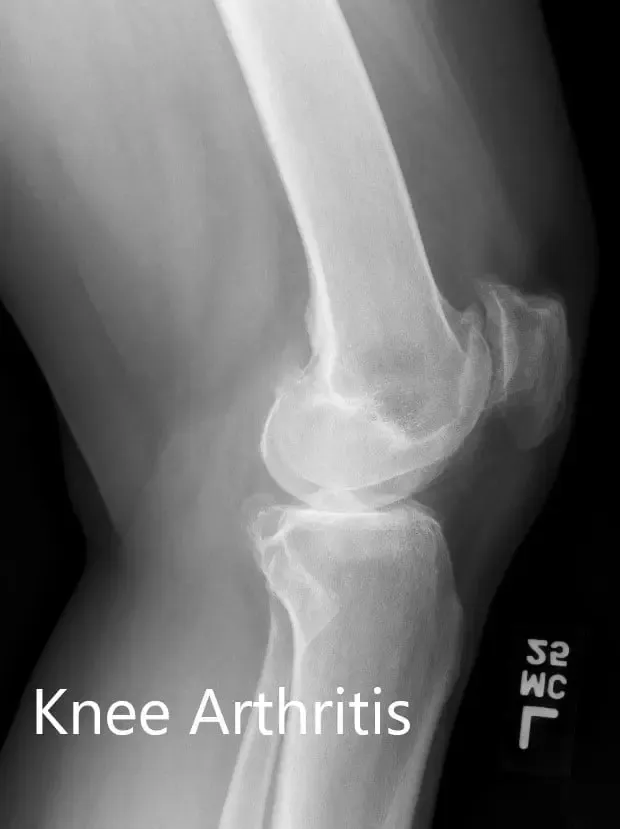
Preoperative X-ray of the left knee showing AP and lateral views
OPERATION: Left total knee arthroplasty.
IMPLANTS USED: Customized tibial tray with a custom femoral component with 6-mm polyethylene insert with 32-mm patella.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after performing an informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient was then anesthetized and the left lower extremity was then draped and prepped in the usual sterile manner. A tourniquet was used to exsanguinate the extremity.
A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were then divided. Medial parapatellar arthrotomy was then performed. The tibia was then prepared with a cutting guide and attention was then turned towards the femur. The femur was prepared using the customized cutting guides.
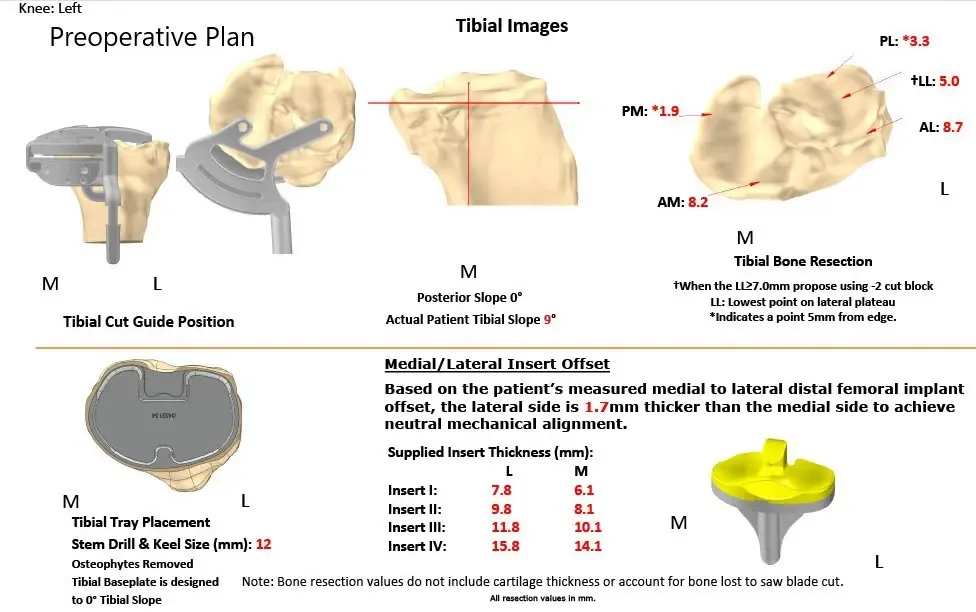
Complete Orthopedics patient-specific surgical plan for a customized left knee total replacement in a 66-year-old female.

Complete Orthopedics patient-specific surgical plan for a customized left knee total replacement in a 66-year-old female (scan 2)
Notch cut was then performed. Lamina spreaders were used medially and laterally. The remainder of the meniscus and the cruciate were then divided. Gap balancing was performed and was found to be correct.
Attention was then turned towards the patella. Patellar resection was then performed. Drill holes were made in the patella.
The trial patella was then placed into position. Attention was then turned towards the femur. The trial femur was then placed into position followed by the trial tibia and the trial poly. The knee was then reduced and trialed through a full physiological range of motion. There was no instability.
Gap balancing was found to be perfect. Patellar tracking was also found to be perfect. Trial components were then removed. The femur was then cemented into position. Excess cement was removed.
The tibia was cemented into position. Excess cement was removed. Poly was then placed over the tibia and the knee was then reduced and held in full extension with a bump under the ankle.
The patella was cemented into position and held with a patellar clamp. After the cement hardened, the patellar clamp was removed. Medial patellar arthrotomy was closed with Vicryl and Stratafix.
The wound was then closed in layers. A tourniquet was then let down and the patient was then transferred to the postoperative care unit in stable condition.

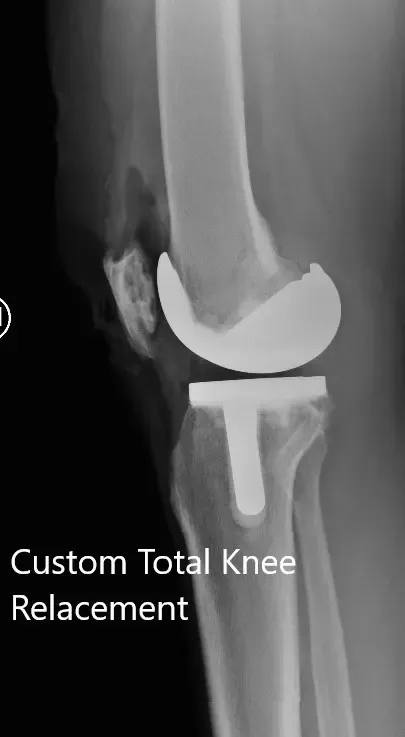
Postoperative X-ray showing the AP and lateral views of the left knee.
Post-op she had an excellent recovery. She was able to walk for 50 feet with support the same day of the surgery. The pain was managed with medications and aspirin was given for deep vein thrombosis prophylaxis.
Sutures were removed uneventfully. Physical therapy was started to rebuild muscle strength and gain range of motion. Three months post-op she had a full range of motion with zero pain. She was able to get back to her baseline and return to her job without any discomfort. She was extremely happy with the outcome.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


