A 60-year-old male presented with complaints of left hip pain for the past four years. The patient had a history of liver disease and was a former alcoholic. He wasn’t able to determine the exact onset of pain but denied any inciting event. A stated the pain had worsened to the point he was no longer able to walk for more than two blocks. He used a cane as an assistive device.
The pain was described as a sharp pain in the left groin which had gotten worse in the past six months. There was no radiation of the pain. The pain was moderate to severe in intensity. Activities such as standing for long, walking, navigating stairs and bending made the pain worse. The pain was present at night and he received minimal relief with pain medications.
He worked was employed as a store manager and was currently not working. His job required him to stand for prolonged periods of time. He was dismayed at his lack of ability to do daily activities due to pain.
He was a former smoker (20 pack-years) and a reformed alcoholic. He was admitted to a rehabilitation center three times in the past five years. He was told he had cirrhosis of the liver and was currently taking medications for cirrhosis. He was also on omeprazole for acid reflux. He denied any bleeding diathesis.
On his physical examination, he walked with an antalgic gait. The stance phase was reduced on the left side. There was tenderness on the left anterior joint line. The range of motion was moderately restricted in the abduction and internal rotation. The rotational movements were especially painful.
On standing, there was no evidence of any structural or functional scoliosis. There was no exaggerated lumbar lordosis. The bilateral shoulders, scapula, iliac spines, patella, and the malleolus were at the same level. On the supine examination, both the anterior superior iliac spines were at the same level. There was no evidence of any leg length discrepancy.
The skin overlying the left groin was normal. There was no broadening or thickening of the trochanter. The bulk and tone of the lower extremities were normal. There was no distal neurological deficit. The bowel and bladder movements were normal. There was no inguinal lymphadenopathy. The examination of the lower spine, right hip, bilateral knee, and ankles was normal.
A routine blood examination was done to estimate the levels of serum vitamin D and electrolytes. Imaging studies in the form of X-Ray revealed increased sclerosis of the left hip. A small radio-opacity was present just below the superior surface of the head of the femur. There were moderate acetabulum changes.
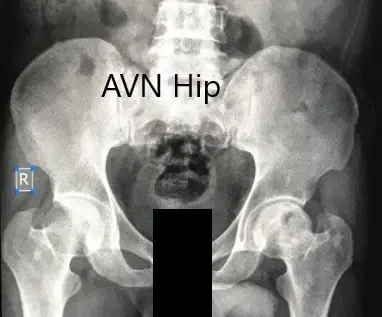
Preoperative X-ray of the pelvis with both hips in anteroposterior view showing AVN of the Left Hip.
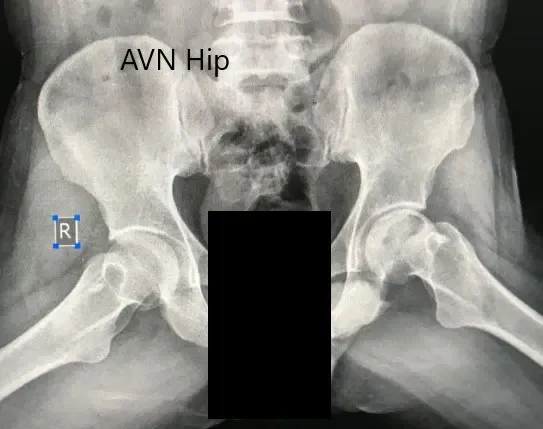
Preoperative X-ray of the pelvis with both hips in the frog-legged lateral view showing AVN of the Left Hip.
An MRI was obtained which suggested avascular necrosis of the left hip stage 3. There were altered signal intensity and bone marrow edema.
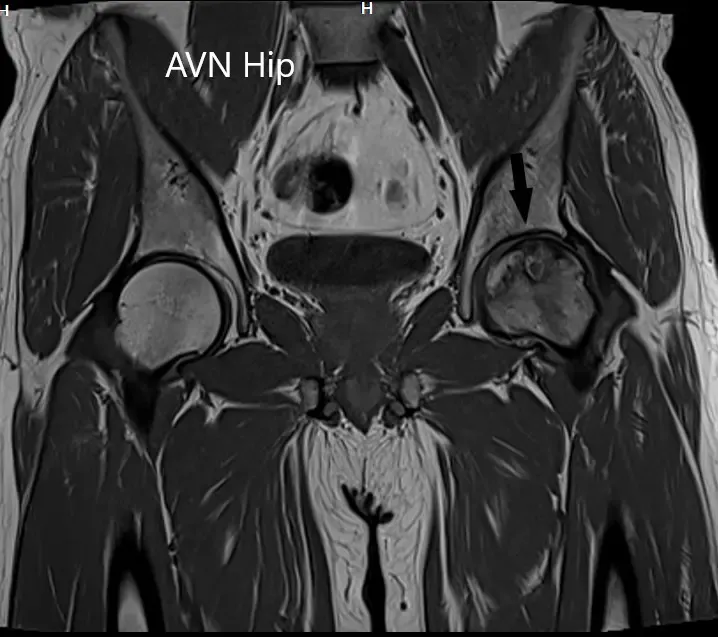
T1WI coronal section of MRI showing AVN hip.
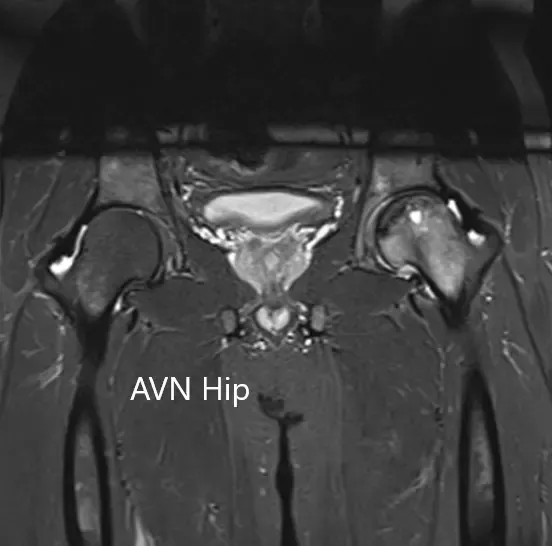
T2WI coronal section of MRI showing AVN hip.

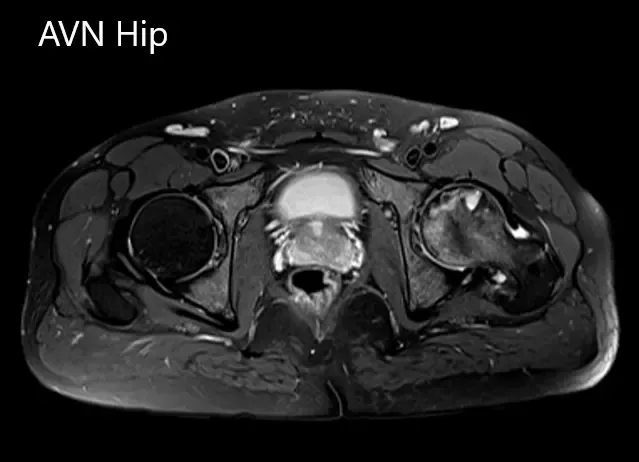
Axial sections of the T1WI and T2WI of MRI.
In view of lifestyle limiting hip pain due to avascular necrosis, the patient was advised a left total hip replacement. Risks, benefits, and alternatives were discussed with the patient at length. The patient was made aware of other hip preservation surgical techniques such as core decompression, vascular and nonvascular bone grafts, and rotational Osteotomy. He decided to go ahead with left total hip replacement.
Post-operative pain was managed with medications and aspirin was given for deep vein thrombosis prophylaxis. There was no distal neurological deficit and the vitals of the patients remained stable.
The patient was allowed to walk with support as tolerated. Physical therapy ensued and hip precautions were explained to the patient. The patient had an excellent recovery and was walking without support in three months. He had a full range of motion and reported zero pain. The patient was overjoyed with the results of the surgery. He follows as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


