A 65-year-old former New York City Fire Department (FDNY) employee and a September 11 survivor presented to our office with complaints of worsening bilateral groin pain. The patient had sustained multiple injuries during the collapse of the north tower in 2001.
As a member of the FDNY, responded on 9/11/2001 immediately upon the first plane striking the North Tower of the World Trade Center. During the subsequent collapse of the North Tower, she was thrown down a flight of stairs and was covered in a large pile of debris.
Despite her injuries, she worked to free herself, an elderly woman she was carrying down and a co-worker who was assisting her in the removal. She and her colleagues were trapped in the stairwell of the North Tower for some 5 hours prior to self extricating themselves from the confines of the collapsed building.
She continued to work directly on the Ground Zero pile without being treated for her injuries, despite constant pain, for months in the immediate aftermath of the attack. She had previously received cortisone injections in the right hip and physical therapy along with heat pads. She had minimal relief with all forms of conservative management.
The pain was described as a dull ache in both groins, which radiates down the knees medially and anteriorly. The severity was mild to moderate initially which had increased to severe recently. She was unable to perform her daily activities without pain. Activities such as walking, navigating stairs, bending and getting up from a chair exacerbated her pain.
She was a nonsmoker and her medical ailments included hyperlipemia, asthma, and hypertension. She previously had arthroscopic meniscal debridement of the right knee. Open reduction and internal fixation of the left humerus. Left inguinal hernia repair and right rotator cuff repair.
On physical examination, she walked with an antalgic gait and used a cane for ambulation. There was no evidence of exaggerated lumbar lordosis. There was no spinal scoliosis and both the shoulders, iliac spines, and patella were at the same level.
There was no leg length discrepancy and the bilateral trochanters were at the same level. There was no fullness or induration in bilateral groins. There was no inguinal lymphadenopathy. There was no thickening or broadening of the trochanters. The range of motion was restricted terminally with painful rotatory movements.
There was no fixed deformity in the coronal, sagittal and axial plane. The bilateral lower extremity pulses were 2+ and comparable. There was no distal neurological deficit. Imaging revealed severe osteoarthritis of both hips with subchondral cysts, sclerosis, and osteophyte.
In view of the patient’s medical conditions and lifestyle limiting groin pain, she was advised bilateral total hip replacement with robotic assistance. Risks, benefits, and alternatives were discussed at length with the patient. She agreed with the plan.

Preoperative X-ray of the patient’s pelvis with both hips.
OPERATION: Bilateral hip replacement using the robot.
IMPLANTS USED: Cup size 56 with acetabular liner 36-mm inner diameter with a 127 degree neck angle size 6 stem with ceramic femoral head 36-mm plus O on both sides with a 6.5-mm bone cancellous screw.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining the informed consent, signing on the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as with her husband prior to the procedure.
The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist The patient was then definitely positioned with the right hip up and the right hip was then draped and prepped in the usual sterile manner.
The external fixator pins were then placed in the iliac crest and the tacking device was then set up. An incision was then made over the hip joint, centered over the greater trochanter, and the skin and subcutaneous tissues were then incised.
The fascia was then divided and the hip was then placed into internal rotation and the posterior soft tissue structures were then taken down and tagged for future repair. The acetabular was then exposed. The tracker was placed over the greater trochanter before the neck resection that was done before exposure of the acetabulum.
After exposing the acetabulum, the acetabular tacking device was then placed into position. The remainder of the labrum was then divided. The acetabulum was then reamed and the final shell was placed into position in the correct abduction and anteversion. A screw was placed for additional fixation. The liner was then placed over the shell.
The alignment was found to be satisfactory. Attention was then turned towards the femur. The remainder of the tissue and undersurface of the greater trochanter was then removed, and the femur was then sequentially broached. The final broach was left into position. The trial trunnion and the head were.then placed into position.
The lesser trochanter with the central distance was measured and was compared to the lesser trochanter to the.center distance prior to the hip dislocation. The lesser trochanter to the center distance was found to be correct. The hip was then reduced and then trialed through a full range of motion.
The hip was then dislocated and the trial femur was then removed. The final femur with the femoral head was placed into position. The hip was then reduced, thorough lavage was given. The tracking devices were then removed.
The fascia was closed with Ethibond, cutaneous tissues were closed with 2-0 Vicryl, subcutaneous tissues were closed with O Vicryl, subcuticular tissue was closed with 2-0 Vicryl, and the skin was closed using staples.
Sterile dressing was then applied over the wound. The patient was stable under anesthesia and it was decided to proceed with the other hip joint.
An x-ray was obtained before proceeding to the other hip joint and the hip joint was found to be in satisfactory position.
The patient was then placed with the left hip and the left hip was then draped and prepped in the usual sterile manner. A curved incision centered over the greater trochanter was used for the arthrotomy, skin and subcutaneous tissues were incised, fascia was then divided.
The hip was then placed under a trial rotation and the posterior soft tissue structures were then taken down and tied for future repair The hip was then dislocated. The lesser trochanter with center distance was then taken and the neck dissection was made at the correct level.
The head was then removed as the acetabulum was exposed and the labrum was then debrided. The acetabulum was then reamed and the final cup was then placed into position and the correct hip reduction in anteversion. The poly was then placed over the shell.
Attention was then turned towards the femur. The remainder of the tissue and the undersurface of the greater trochanter was removed, and the femur was then sequentially broached. The final broach was left into position. The.trunnion and the head were then placed over the femur the hip was then reduced.
The hip was then trialed through a full range of motion and the hip was found to be stable. The hip was then dislocated. Trial components were then removed. The final components were then placed into position. Thorough lavage was given. The soft tissue structures were then tagged to the greater trochanter through transverse tunnels.
The fascia was closed with Ethibond, cutaneous tissues were closed with 0 Vicryl, subcuticular tissues were closed with 2 0 Vicryl, and the skin was closed using staples. Sterile dressing was then applied over the wound and the patient was then placed in the supine position.
An x-ray was then obtained for confirmation of the placement of the prosthesis and for confirming proper alignment and limb length. The x-rays were found satisfactory. The patient was then transferred to the postoperative care unit in stable condition.
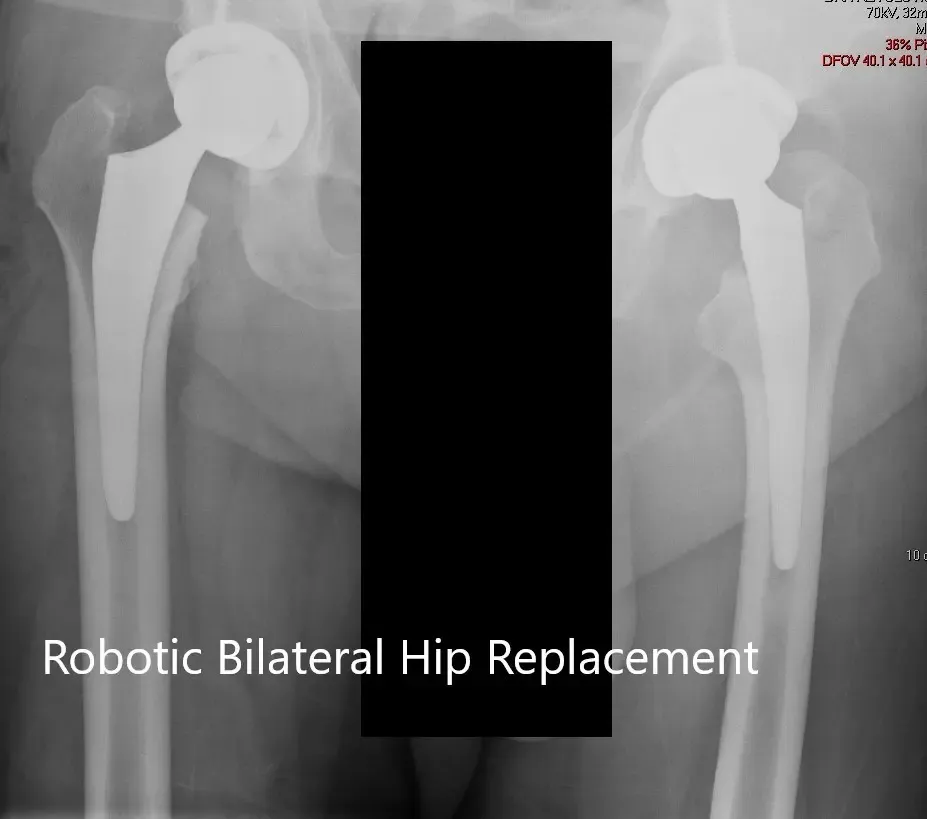
Postoperative X-ray of the patient’s pelvis with both hips.
Post-op her vitals remained stable and there was no distal neurological deficit. Hip precautions were advised to the patient at length. She was started on aspirin for deep vein thrombosis prophylaxis. The sutures were removed uneventfully. Physical therapy and rehabilitation were started with gait training and fall prevention education.
Three months post-op, she demonstrated an excellent range of motion and zero pain. She was able to walk without support and was able to carry on her daily activities without pain. She follows up as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


