A 56-year-old male presented to our office with complaints of a worsening pain of the right hip with associated limp. The patient explained that he has had this pain since he was a child and he could live with it, but it has gotten worse. The pain was so unbearable that he had to go to the hospital and they told him there was nothing more they can do, but perform surgery.
The pain was associated with a limp and a lurch. He stated he used a shoe raise on the right side to avoid the limp. He felt his right leg was shorter than the left one. The patient stated he was able to sit, squat and sit cross-legged before but recently over the past year he was unable to do so.
The patient doesn’t recall the initial onset of the pain but denied any history of trauma. The limp was first noticed by his parents when he was in Columbia. He was managed conservatively for pain and limp in the form of traction and splint.
He denied any childhood infection/discharge from the right hip. He also denied any childhood endocrine disease or a history of tuberculosis.
The patient tried conservative management in the past year in the form of physical therapy and pain medications. The pain was located in the right groin radiating to the knee anteriorly. The pain was worse with walking and better with rest. Limping increased as the intensity of pain increased and he used a cane for ambulation.
The patient denies any family history of hip disease associated with limping and pain. He was currently on disability. The patient has had two arthroscopic surgery on both shoulders due to a work accident. The patient has no known allergies or is taking any medications.
On his physical examination, his gait was bipedal, antalgic, steady, unassisted with a lurch towards the right side. There was a presence of mild functional scoliosis with convexity towards the right side. Scoliosis disappeared on sitting or bending forward (Adam’s test).
There was no exaggeration of lumbar lordosis. The right anterior superior iliac spine was at a higher level than the left. On squaring the pelvis, both the apparent and true shortening were equal. There was no coronal or sagittal plane deformity. The rotational movements were restricted due to pain.
There was no distal neurological deficit. The bilateral lower extremity pulses were good volume and comparable. The skin overlying the hip joint was normal with no scar or sinus. There was no fullness of scarpa’s triangle and three digit palpation of hip joint revealed the right greater trochanter higher than the left side.
There was no broadening or thickening of the trochanter. Telescopy was negative and there was no abnormal bony mass in the right gluteal region. Tenderness was present along the right anterior joint line. There were no enlarged lymph nodes in the inguinal region.
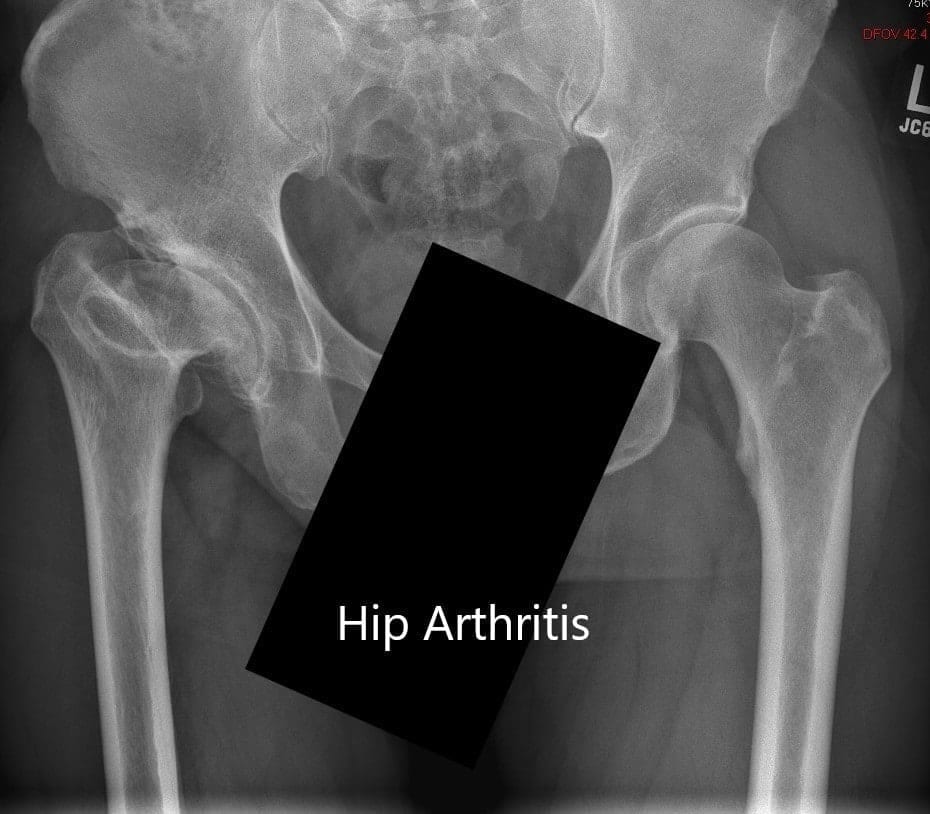
Preoperative X-ray showing the AP view of the pelvis with both hip joints
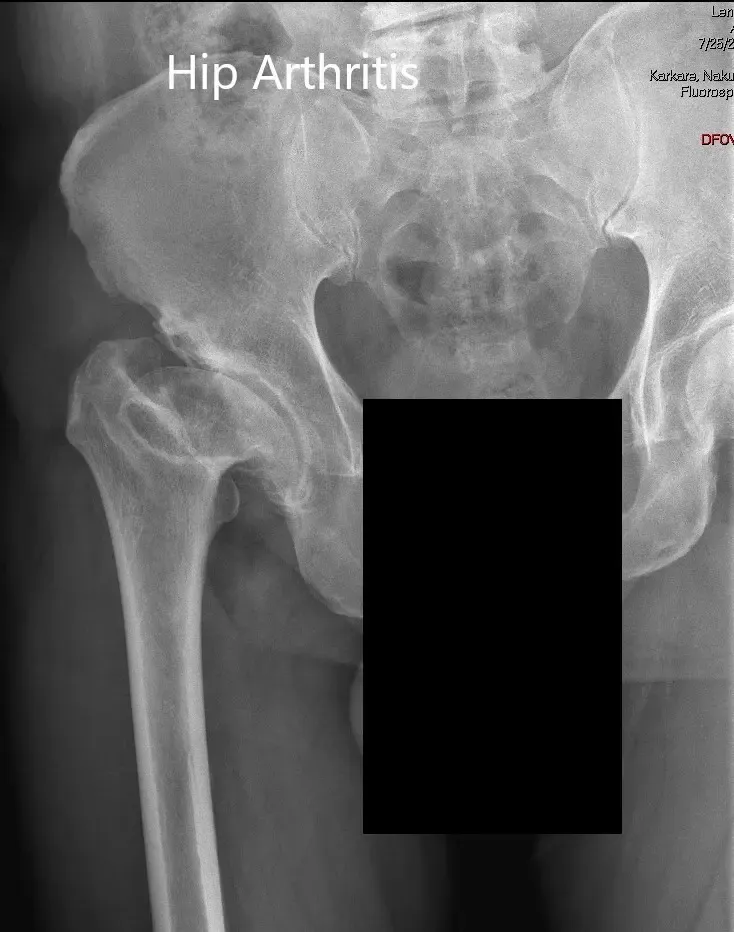
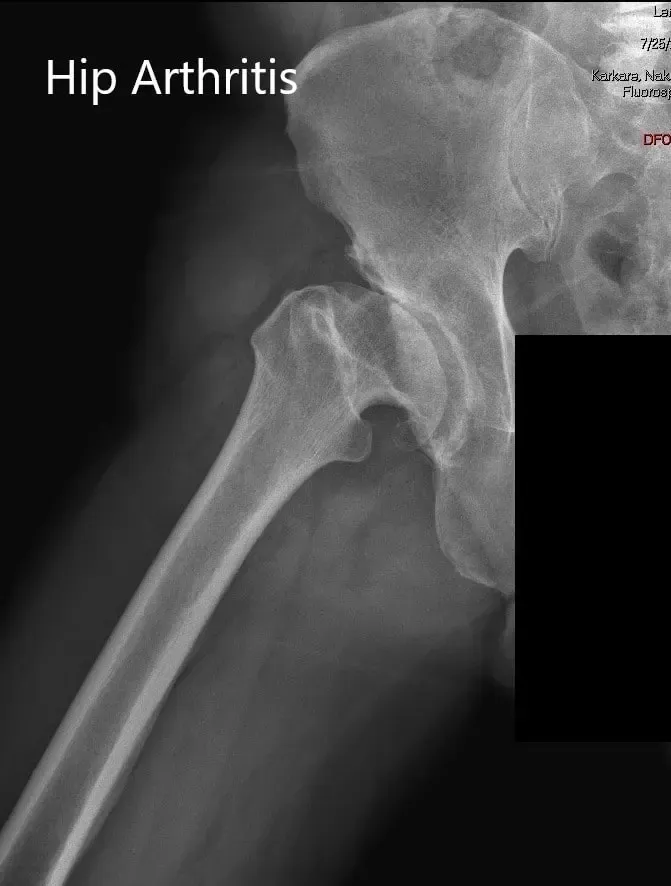
AP and lateral views of the right hip joint
Imaging revealed markedly deformed right femoral head and impacted the femoral neck. There were severe degenerative changes of the right hip.
Considering the DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent,imaging and physical examination, the patient was advised surgical management for the squeal of coxa plana. He was advised about total hip replacement. Risks, benefits, and alternatives were discussed with him at length. He agreed to go ahead with the procedure.
IMPLANTS USED: Restoration modular stem 195-mm with a 15-mm diameter with a constrained liner with a 22.2-mm femoral head with proximal body 19-mm plus 0.
Signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as with the family prior to the procedure. The patient understands the significantly increased risk of orthopedic complications because of the complexity of the primary hip replacement that he is undergoing.
The patient was brought to the operating room and was definitively positioned with the right hip up and the right hip was then draped and prepped in the usual sterile manner. A curved incision centered over the greater trochanter was used for the arthrotomy. Skin and subcutaneous tissues were incised.
Fascia was then divided. The posterior soft tissue structures were then taken down and tagged for future repair. The incision was extended distally for the release of the gluteus tendon. The hip was significantly tight and significant tendon releases had to be done for exposure of the acetabulum and for anterior translation of the femur.
The hip was then dislocated. Lesser trochanter to the center measurement was taken and was compared to the preoperative planning. The head was then resected. Attention was then turned towards the acetabulum. A significant superior dissection was needed for exposure of the acetabulum.
The reflected head of the rectus femoris was incised for anterior translation of the femur. The acetabulum was exposed. Remainder of the labrum was then debrided. The acetabulum was sequentially reamed. The final shell was then placed into position in the correct abduction and anteversion. A liner was then placed onto the shell. Attention was then turned towards the femur.
The femoral resection was performed before for exposure of the acetabulum and the femur was reamed for placement of the restoration modular stem. The distal stem was then placed into position after reaming. The proximal reaming was then performed and the proximal body was then placed into position. The head was placed over the body. Lesser trochanter to center distance was then taken.
An attempt was made to lessen the hip by doing adequate releases. The hip was then attempted to be reduced. When trialing, it was found that the hip was dislocating posteriorly. This was accounted for despite the releases and that the releases would be closed at the end of the procedure.
The hip was dislocated. The anteversion of the proximal body was increased and the reduction was attempted again. The hip was still unstable. It was decided to do a constrained liner. The hip was dislocated. Attention was then turned towards the cup, then the liner was removed.
The constrained liner was then placed into position. The head for the constrained liner was then placed over the stem. The stem was then articulated with the constrained liner. The hip was then trialed again and the hip was stable.
Thorough lavage was given. Posterior soft tissue structures were then tacked with the greater trochanter through transosseous tunnels. The release was closed. The fascia was closed with Ethibond and #1 Vicryl. Cutaneous tissues were closed with O Vicryl.
Subcuticular tissues were closed with 2-0 Vicryl. The skin was closed with staples. Sterile dressing was applied over the wound. The patient was then transferred to the postoperative care unit in stable condition.
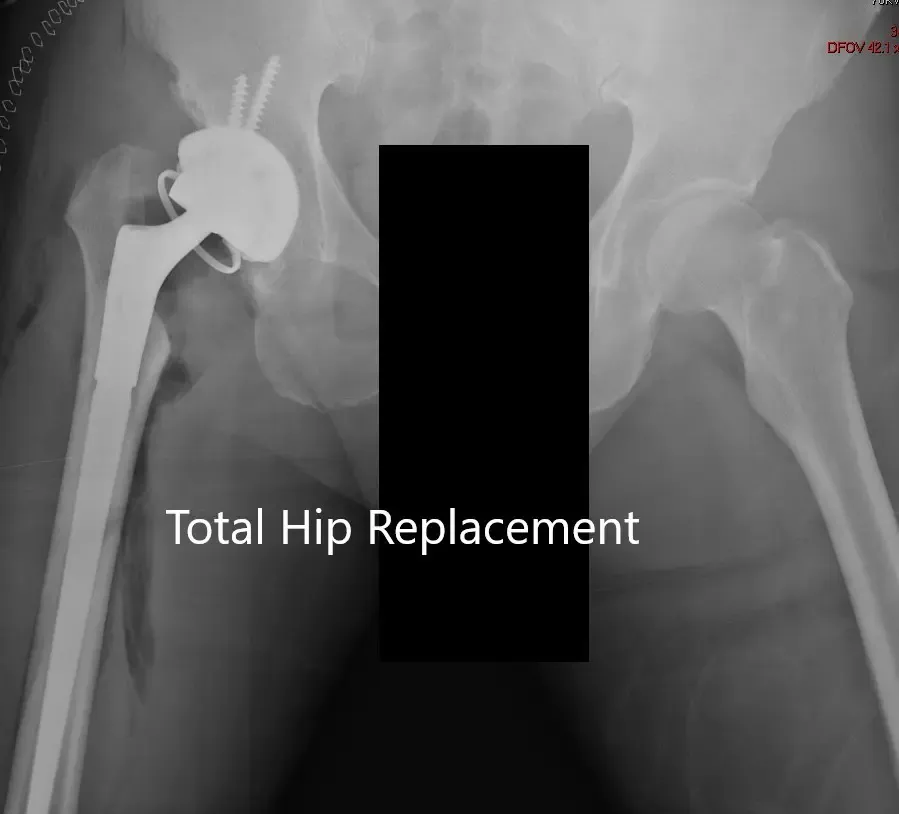
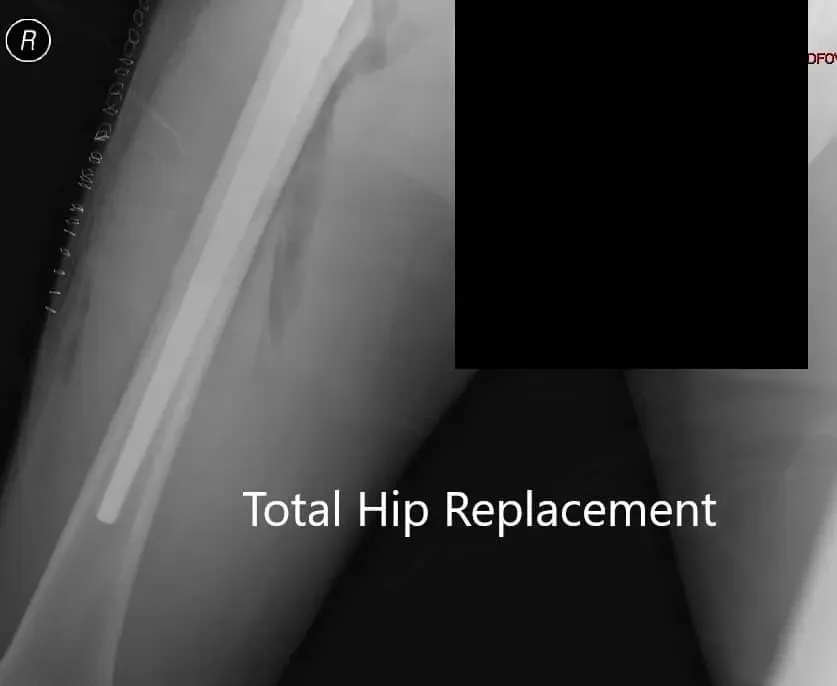
Postoperative X-ray showing AP view of the pelvis.
The recovery of the patient was unremarkable. He was started on aspirin 325mg BID for deep vein thrombosis prophylaxis. The pain was managed with medications. Hip precautions were explained to the patient. Weight-bearing was allowed as tolerated. Postoperatively there was no neurological deficit in bilateral lower extremities.
He was advised physical therapy focusing on gait training, fall prevention, muscle strengthening, range of motion and home safety. The sutures were removed uneventfully.
The three months post-surgery follow up demonstrated good pain control. The aspirin was discontinued and the patient was advised to wean off the hip precautions gradually. He follows up regularly.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


