A 45-year-old male presented to us with complaints of left knee pain. The patient stated he had a snowmobile accident when was 15 years old when the blade of the snowmobile smacked into his knee. He had previously through years seen a number of physicians for his left knee pain.
The patient previously had treatment in the form of multiple nerve blocks and blood patching. He underwent meniscus surgery 10 years ago. He stated to not have improved after the surgery. The patient again had surgery involving meniscus suturing at another hospital but with no relief. He also states to have had multiple knee viscous injections, taping and genicular nerve blocks.
He had tried a myriad of conservative treatment options in the form of physical therapy, bracing and pain medications but with only temporary relief. The patient worked as a school teacher and was in a great deal of stress secondary to knee pain. He was no longer able to play with kids at school and participate in school events due to pain.
Recently, he stated that he found it difficult to walk for long and climb stairs. He experienced great pain while riding a bicycle and going hiking. He accompanied his wife on his office visit with us and the couple was emotionally tormented due to his lifestyle limiting knee pain. The patient was a nonsmoker with no pertinent family history or drug allergies.
His physical examination revealed tenderness of the medial joint line with mild swelling. The knee revealed no instability on anterior, posterior, valgus and varus stress tests. Imaging revealed post-traumatic arthritis of the left knee. He was given a cortisone knee injection with excellent control of pain. Subsequently, the patient was followed up in 3 months.
Subsequent follow-up visits, the patient still complained of left knee pain with restriction in his daily activities. Various surgical and nonsurgical treatment options were discussed with him at depth. The patient was found to be a suitable candidate for custom total knee replacement. Risks and benefits were discussed with him at length including durability of the implants and revision surgery. The patient agreed to the procedure.
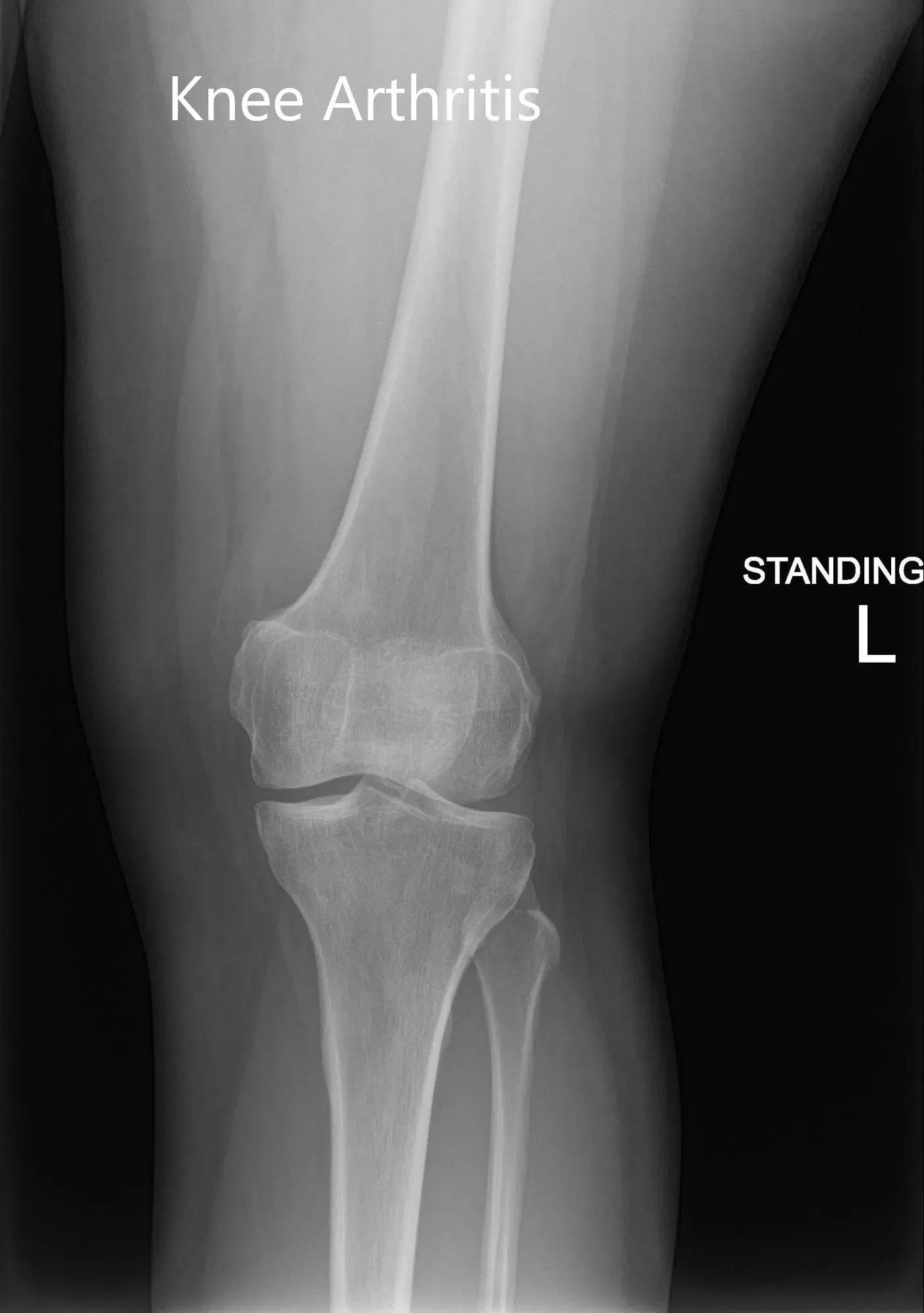
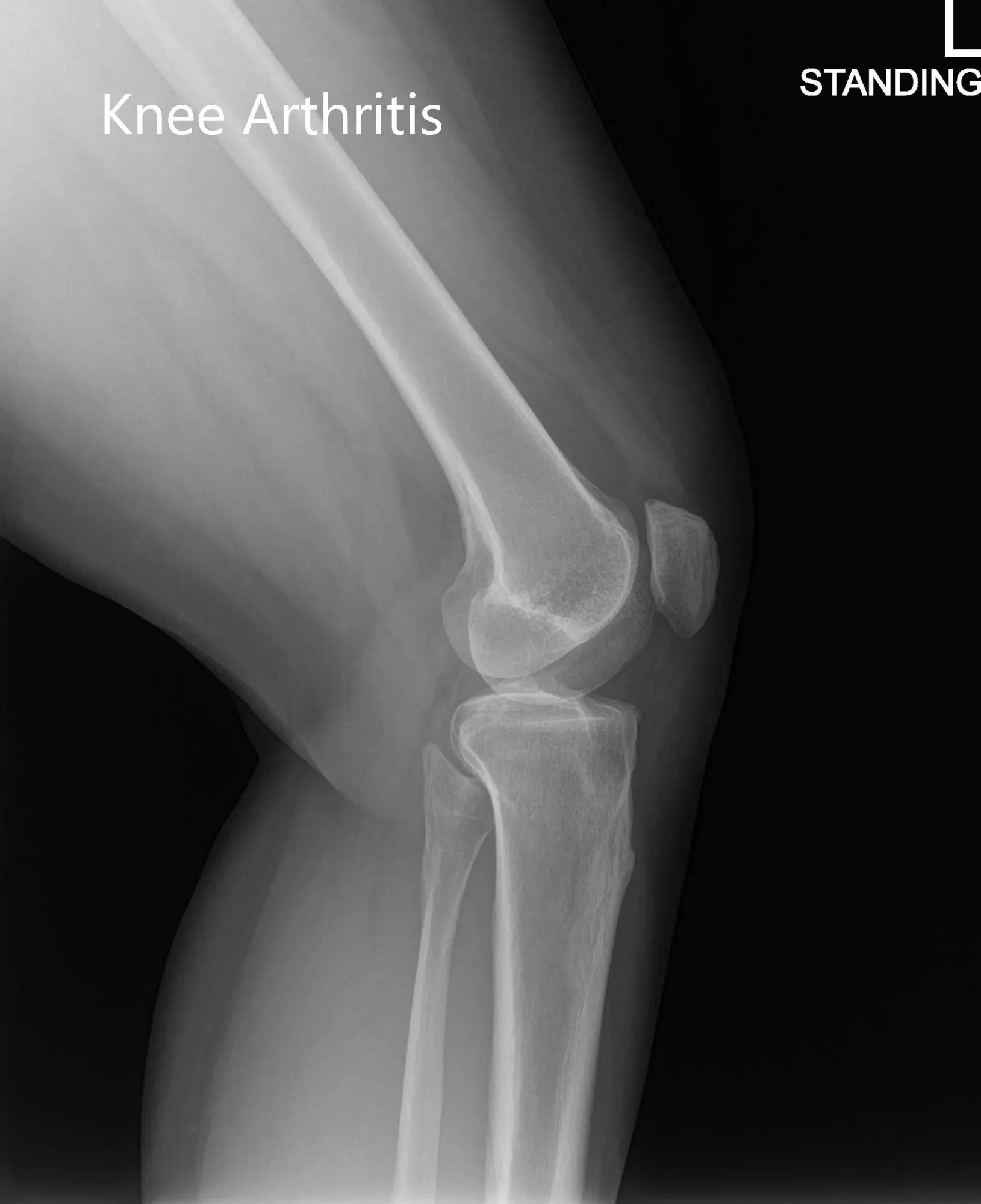
Preoperative X-ray of the left knee showing AP and lateral images
A preoperative CT scan of the patient’s left knee was obtained to assess his biomechanics and anatomy. The data was then used to obtain 3D images of the patient’s knee helping in constructing patients’ specific unique implants and instruments. Custom knee replacement offers a bone preserving surgery. Unique implants specific for the patient ensure restoration of the natural articulating surface and geometry of the knee.
We were provided with preoperative surgery plans outlining the bone resection and the distal femoral implant offset values. The plan helps the surgeon in a better understanding of the patient’s anatomy before the procedure. The 3 D printed implant jigs ensure bone resection outlined in the plan.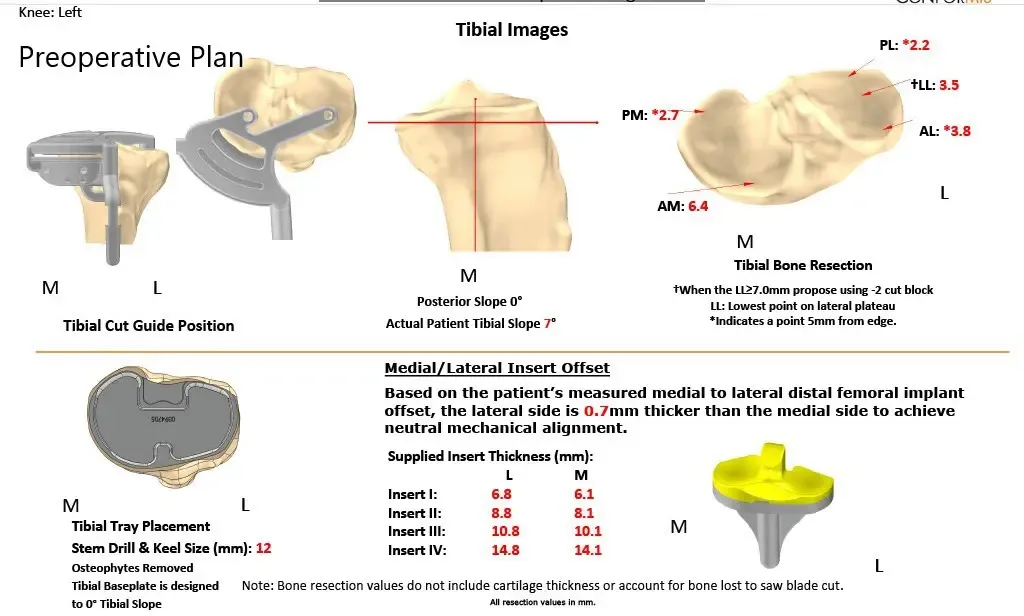
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement for post-traumatic arthritis in a 45-year-old male.
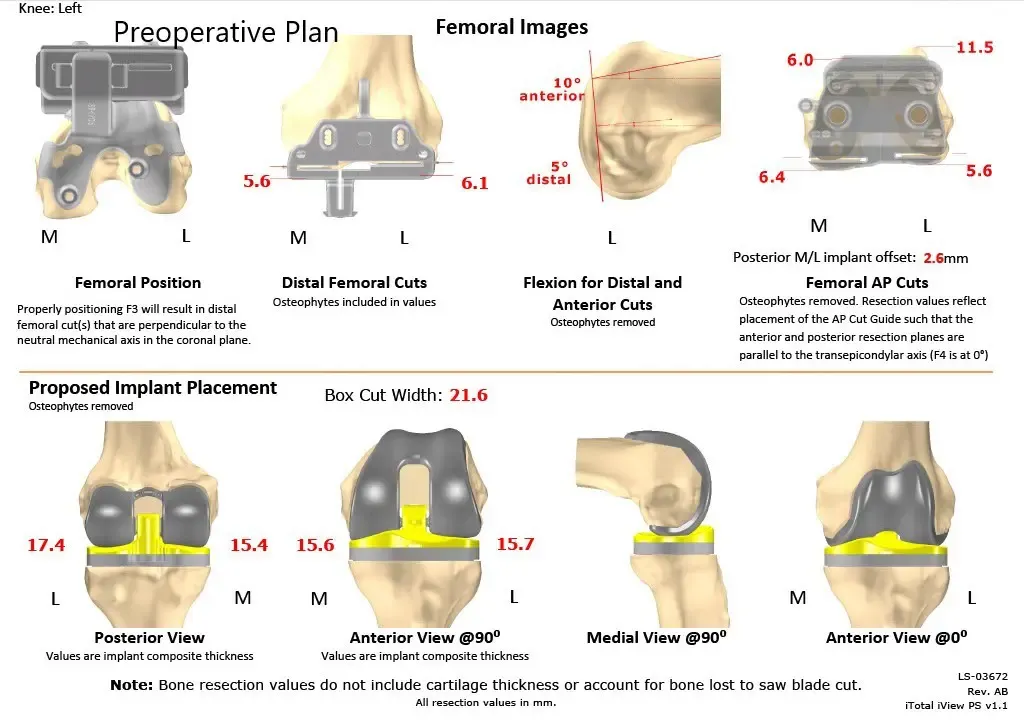
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement for post-traumatic arthritis in a 45-year-old male (scan 2)
Operative report:
Implant – Left total knee arthroplasty using custom femur, custom tibia, patella, and 6-mm polyethylene.
The patient was brought to the operating room and anesthesia was obtained by the anesthesiology. The patient was then definitely positioned and the left knee was then draped and prepped in the usual sterile manner. A straight incision was used for the arthrotomy.
Skin and subcutaneous tissues were then incised. Medial parapatellar arthrotomy was performed. The tibial resection was then made with the tibial resection guide. The resection was then checked with the alignment guide onto the correct tibia, then prepared. Custom disposable cutting blocks (jigs)
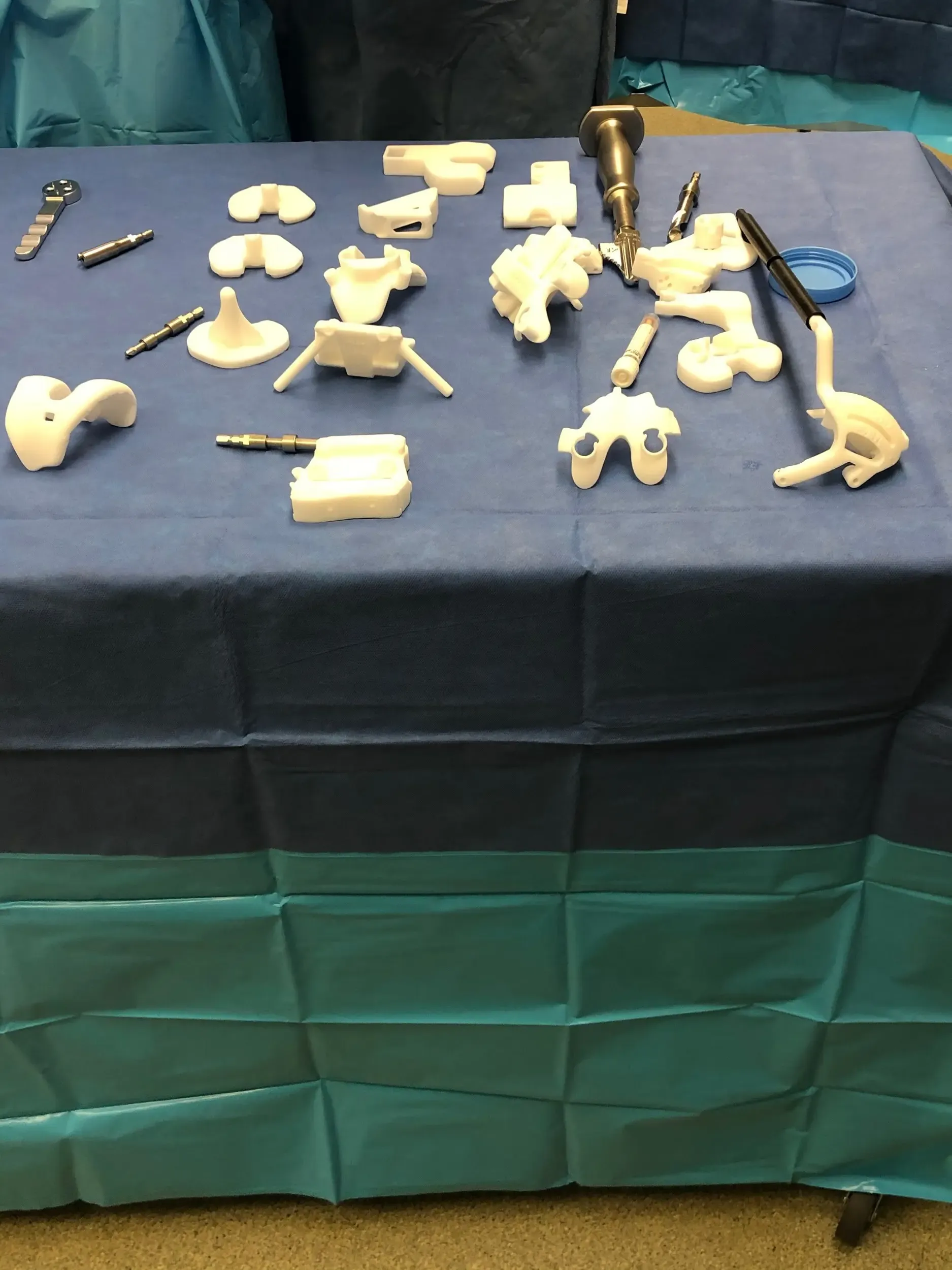
Attention was then turned towards the femur. The distal cutting guide was used. The alignment was checked. The anterior, posterior and chamfer cuts were made using the respective guide.
A notch cut was then performed laminar spreaders were used medially and laterally, and the remainder of the meniscus and the cruciates were then debrided. The gap was found to be perfectly balanced. The patella was then resected. Drill holes were made in the patella.
Trial patella was then placed into position followed by the trial femur and trial tibia. The poly was then placed into position. The knee was ranged to a full range of motion. Patellar tracking was found to be excellent. The trial components were then removed. The lavage was given, the injection was given.
The femur was cemented into position. Excess cement was removed. Tibia was cemented into position. Excess cement was removed. Poly was placed into position, and the knee was then reduced and held in position with a bump under the right ankle. The patella was then cemented into position and was held in position with a patellar guide. Excess cement was then removed.
After the cement hardened, the tourniquet was let down. Hemostasis was achieved. The patellar clamp was removed. Evicel was used. Medial parapatellar arthrotomy was then closed, and the wound was then closed in layers. A sterile dressing was applied over the wound, and the patient was then transferred to the postoperative unit in stable condition.
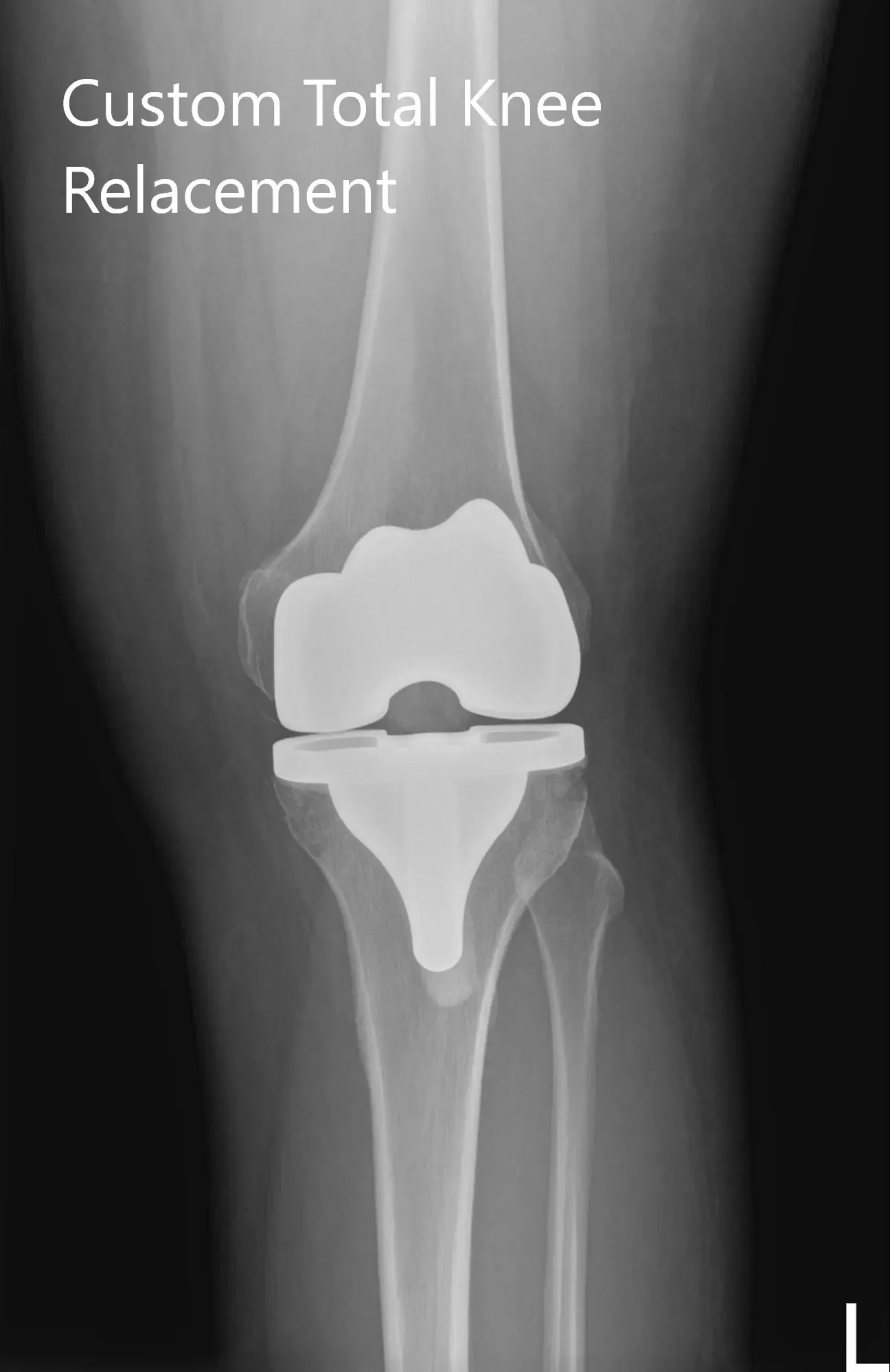
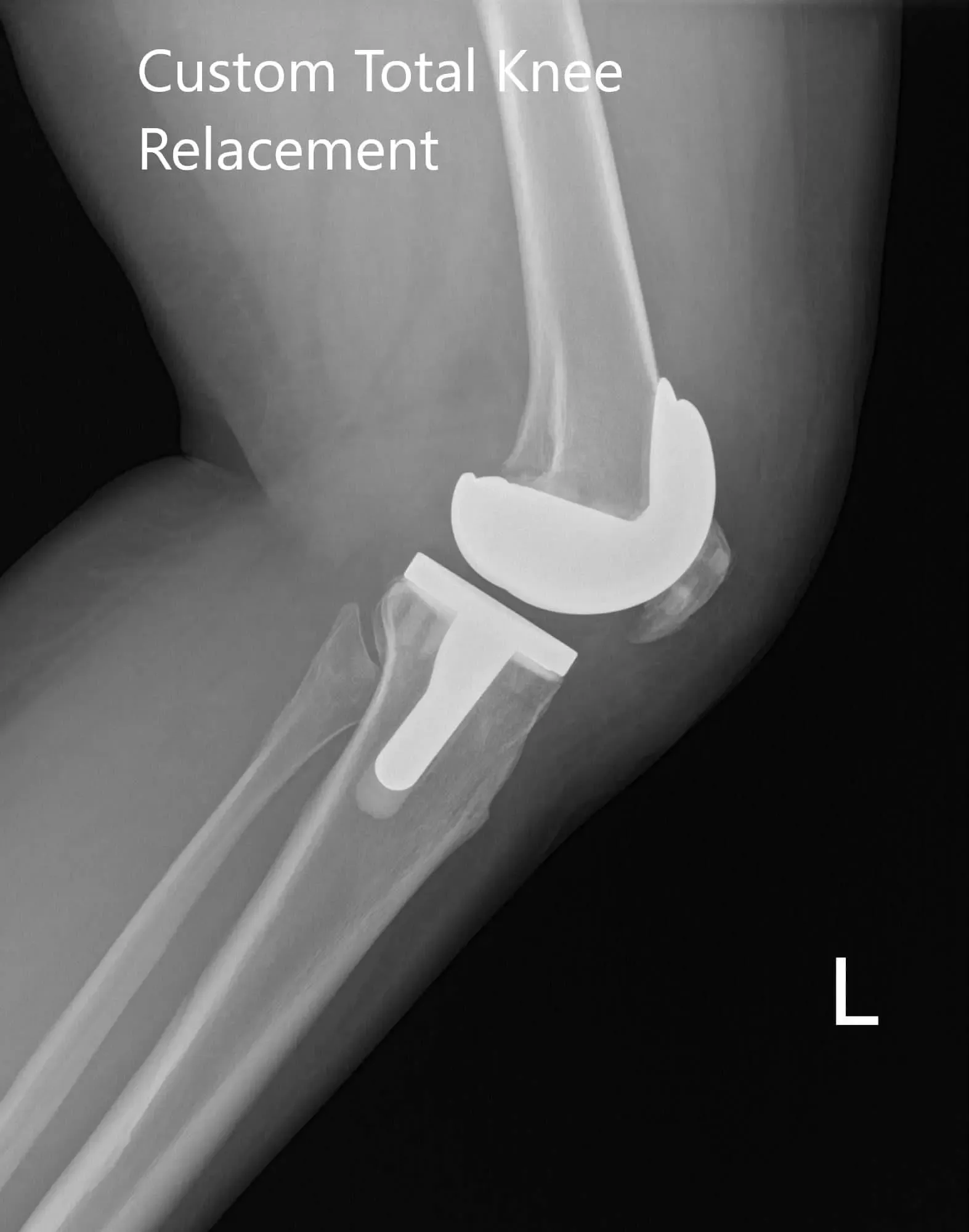
Postoperative X-ray of the left knee showing AP and lateral images
The patient was ambulatory the same day of the surgery. He reported well control of pain with medications and had a good range of motion about the left knee. The patient’s wound was clean, dry and intact. He had excellent compliance with physical therapy and home exercise program. He reported no pain (0/10) and an excellent range of motion after 3 months.
The patient had successfully concluded his physical therapy and joined back as a school teacher. He loves the freedom of movement playing around kids. He was able to get back to moderate hiking and riding his bicycle without pain. The couple was happy stating the results had exceeded their expectations. He follows up as needed.


