Overview
Anterior hip replacement is a hip replacement surgery performed through an anterior surgical approach. Traditionally, hip replacements have been performed through posterior or lateral approaches. Both of these surgical approaches involve dissection of muscles or tendons that are involved in a normal gait cycle – the process of walking. The anterior surgical approach is unique in that it involves minimal disruption to the muscles and tendons surrounding the hip joint, and as such, allows for quicker recovery from the hip replacement procedure.
Patient Selection
Patients who suffer from moderate-severe hip arthritis are considered candidates for hip replacement surgery. Good candidates for anterior hip replacement surgery specifically will include patients with low-normal BMI or patients who do not have a large abdominal pannus that will create a skin crease around the area of the incision for an anterior hip replacement – this causes a bacterial reservoir to form over the area of the incision and increases the risk of superficial wound infection and possibly deeper joint infection. Patient anatomy can also influence the surgeon’s decision as to whether they feel that the patient is a candidate for anterior hip replacement surgery, if a patient has a naturally broad pelvis for example, gaining access to the femoral canal may prove challenging and would preclude these patients from being candidates for anterior hip replacement surgery.
Procedure
Anterior hip replacement surgery requires general anesthetic – once this has been administered, a surgical approach using the anterior skin directly overlying the hip is used. The surgeon then parts the muscles in this area without cutting them and exposes the hip capsule. This will then be opened and the arthritic femoral head will be removed. The acetabulum will be prepared for its replacement component by grinding away the arthritic bone with a special tool, and once it is placed in position, it may be held in place with one or more bone screws.
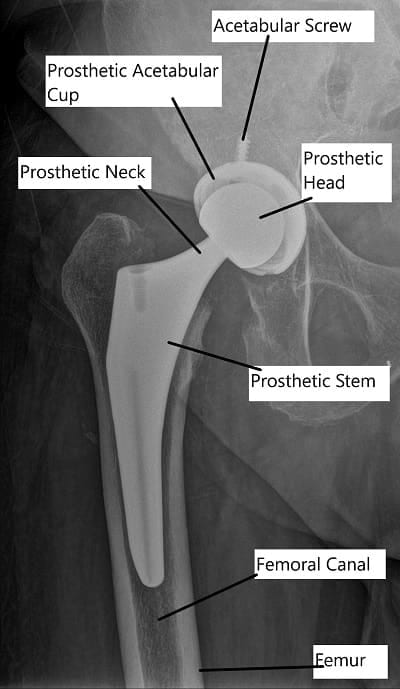
X-ray showing Total Hip Replacement in AP view
Once this is completed, some further surgical dissection is necessary to expose the proximal femur and this includes releasing some of the capsule and tendons from the posterior part of the cut end of the femur.
Once retractors are placed and visualization of the proximal femur is adequate, other special tools can be used to determine the correct size of replacement component for each patient. X-rays are used to help determine the appropriate position and size of the implant intraoperatively. It is also used to help the surgeon determine that the length of the leg is equal to the other side once the right size component has been selected.
Once the surgeon is satisfied, he will place the final components and reduce the hip one final time and then surgically close the hip capsule.
The patient is able to bear weight on the operative leg immediately following the surgery (although adequate pain relief will be necessary for them to achieve this). For some patients, discharge from hospital later the same day is possible, others may require a single night stay in the hospital to recover and are usually home the following day.
Success Rate
Anterior hip replacement surgery is an area of major interest in current research institutions. The current best evidence indicates that, at 3-months post-surgery, the outcomes between anterior hip replacement and all other hip replacement techniques are equivalent with no obviously superior technique. However, in the first 6 weeks to 3 months, it is felt that the anterior hip replacement technique offers a quicker earlier recovery as compared to alternative techniques. As such, it is felt to be a superior technique in terms of early postoperative recovery, especially in younger patients who have greater physiological reserves to be able to cope with the stresses of surgery.
Ultimately, the difference in success rates long term is not known, as we do not have sufficient research data to inform us of this, but medium term the results indicate equivalent outcomes when compared to alternative surgical approaches.
How Medicare Covers Direct Anterior Total Hip Arthroplasty (THA)
If you have Medicare, your healthcare provider may bill for CPT Code 27130 — this refers to a total hip replacement, also called total hip arthroplasty (THA). In the direct anterior approach, the surgeon accesses the hip joint from the front of the hip. This allows muscles to be spread aside instead of cut, which can lead to less pain, shorter hospital stays, and faster recovery, while still replacing the damaged joint with implants.
“What Will It Cost You?”
If you don’t have secondary insurance, here’s what you can expect:
Estimated Out-of-Pocket Cost for Direct Anterior THA (27130): $303.45
“For example, hypothetical patient, Diego, needed a hip replacement after years of painful arthritis. His surgery included 1 procedure: direct anterior total hip arthroplasty (27130). Thanks to Medicare, his total out-of-pocket cost was about $303.45. His secondary insurance then covered it completely!”
Summary
Anterior hip replacement surgery is fast becoming a widely used and highly successful technique for performing hip replacement surgeries. The benefits of using this technique include enhanced early recovery, shorter stays in hospital and even shorter times for returning to work and recreational activities.
If you think, you may be a candidate for an anterior hip replacement, please arrange to see one of our specialist orthopedic surgeons who will be happy to see you in consultation and review your surgical options with you.
Do you have more questions?
What are the main differences between anterior hip replacement and traditional posterior or lateral approaches?
The main difference lies in the surgical approach used to access the hip joint. Anterior hip replacement involves accessing the hip joint from the front, minimizing disruption to muscles and tendons. Traditional approaches, such as posterior or lateral, require dissection of these structures, potentially leading to longer recovery times.
How do I know if I’m a suitable candidate for anterior hip replacement surgery?
Suitable candidates typically have moderate to severe hip arthritis. Factors such as BMI and pelvic anatomy may influence candidacy. An evaluation by an orthopedic surgeon can determine eligibility based on individual circumstances.
Are there any specific risks or complications associated with anterior hip replacement compared to other techniques?
While anterior hip replacement offers advantages in terms of early recovery, there are potential risks such as nerve injury, fracture, and implant malposition. These risks are typically discussed during preoperative consultations.
How long does the procedure typically take, and what is the expected recovery time?
The duration of surgery varies but generally takes a couple of hours. Recovery time varies among patients but may involve immediate weight-bearing and discharge within a day or two. Full recovery can take several weeks to months.
What type of anesthesia is used for anterior hip replacement surgery?
General anesthesia is commonly used for anterior hip replacement, although regional anesthesia techniques may also be employed depending on the patient’s preferences and medical history.
Can you explain the process of muscle sparing in anterior hip replacement and how it contributes to quicker recovery?
Muscle sparing involves minimal disruption to muscles and tendons during surgery. This preservation of soft tissues allows for quicker recovery and reduced postoperative pain compared to traditional approaches.
Are there any specific preoperative preparations or precautions I should take before undergoing anterior hip replacement surgery?
Preoperative preparations may include medical evaluations, cessation of certain medications, and lifestyle modifications. Your surgeon will provide detailed instructions tailored to your individual needs.
What postoperative pain management options are available, and how effective are they?
Postoperative pain management may involve a combination of medications, regional anesthesia techniques, and physical therapy modalities. These approaches aim to minimize discomfort and facilitate recovery.
Will I need physical therapy after anterior hip replacement surgery, and if so, what does it entail?
Yes, physical therapy is typically recommended to improve strength, range of motion, and functional mobility. A physical therapist will create a personalized rehabilitation program focusing on these goals.
How soon after surgery can I expect to resume normal daily activities, such as walking and driving?
The timeline for resuming activities varies among patients but may begin shortly after surgery with guidance from your healthcare team. Driving restrictions may apply initially, depending on individual recovery progress.
Are there any restrictions on movement or weight-bearing following anterior hip replacement surgery?
Initially, precautions may be advised to protect the surgical site, such as avoiding excessive bending or twisting at the hip joint and adhering to weight-bearing instructions. Your surgeon will provide specific guidelines tailored to your surgery.
What are the potential benefits of anterior hip replacement surgery compared to other approaches in the long term?
Long-term benefits of anterior hip replacement include reduced risk of dislocation, faster recovery, and potentially improved functional outcomes. However, research on long-term outcomes is ongoing.
How frequently will I need follow-up appointments after surgery, and what will these involve?
Follow-up appointments are typically scheduled in the weeks and months following surgery to monitor healing, assess range of motion, and address any concerns. Your surgeon will determine the frequency based on your progress.
What measures are taken during surgery to minimize the risk of infection?
Sterile techniques, antibiotic prophylaxis, and meticulous wound care are employed to minimize the risk of infection during surgery. Additionally, surgical facilities adhere to strict protocols to maintain a sterile environment.
Are there any factors that could increase the likelihood of needing revision surgery in the future after anterior hip replacement?
Factors such as implant wear, instability, and osteolysis (bone loss) may increase the likelihood of needing revision surgery in the future. Regular follow-up appointments and adherence to postoperative instructions can help monitor and manage these risks.
Can you explain the role of X-rays during the procedure and in postoperative assessment?
X-rays are used intraoperatively to assess implant positioning and ensure accurate placement. Postoperatively, X-rays are utilized to evaluate implant stability, detect any abnormalities, and monitor healing progress.
How do you determine the appropriate size and positioning of the implant during surgery?
Surgical techniques, preoperative imaging, and intraoperative assessments are used to select the appropriate implant size and position based on the patient’s anatomy and specific surgical requirements.
What criteria do you use to assess the success of anterior hip replacement surgery?
Success is typically evaluated based on pain relief, functional improvement, implant stability, and patient satisfaction. Long-term outcomes, including implant survival rates, are also considered indicators of success.
Are there any lifestyle modifications or precautions I should take after surgery to prolong the longevity of the hip replacement?
Maintaining a healthy weight, engaging in regular low-impact exercise, and avoiding high-impact activities can help prolong the longevity of the hip replacement. Your surgeon may provide additional recommendations based on your individual circumstances.
What ongoing support or resources are available to patients undergoing anterior hip replacement surgery, both during recovery and in the long term?
Patients have access to various resources, including physical therapy services, educational materials, and support groups, to assist them during recovery and beyond. Your healthcare team can provide guidance on accessing these resources.


