Anterior lumbar interbody fusion (ALIF) is a specialized surgical technique used to treat various lumbar spine conditions, including herniated discs, degenerative disc disease, and spinal deformities. This procedure involves removing the damaged intervertebral disc from the front of the spine, replacing it with a bone graft and a cage to promote fusion. ALIF is typically performed when conservative treatments, such as physical therapy and medications, have failed to alleviate symptoms. The procedure may be performed alone or combined with posterior surgery to enhance stability.
How Common It Is and Who Gets It? (Epidemiology)
Lumbar spine issues are prevalent, especially among adults aged 30 and older. Conditions like herniated discs and degenerative disc disease often result in pain and impaired function, affecting mobility and quality of life. ALIF surgery is generally recommended for patients with severe symptoms that do not improve with conservative treatments. These conditions are common in both men and women, though the risk increases with age, particularly in individuals over 50.
Instruments Used in ALIF
The success of ALIF depends significantly on the precise use of surgical instruments. These include forceps for disc removal, bone graft cages (metal or PEEK – a type of plastic), and stabilization tools such as screws, plates, and rods. A quick implant inserter with a depth gauge and release mechanism is often utilized to ensure the accurate placement of the implants.
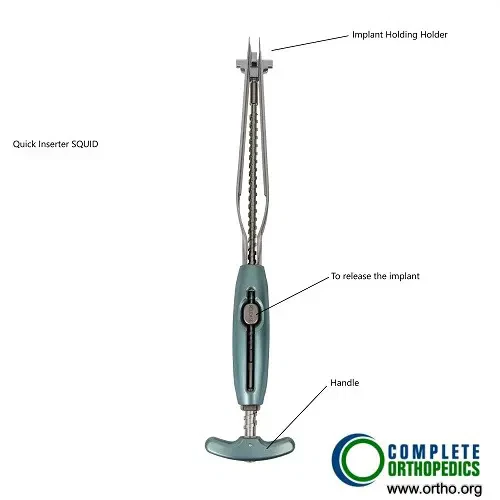
A quick implant inserter for ALIF with depth gauge and release mechanism

Instruments used in ALIF
Why It Happens – Causes (Etiology and Pathophysiology)
ALIF is typically used to address conditions such as:
- Herniated intervertebral discs: When the disc’s inner core pushes through a tear in the outer layer, it may compress surrounding nerves, causing pain and numbness.
- Degenerative disc disease: Aging leads to the breakdown of discs, reducing their ability to cushion the spine.
- Spondylolisthesis: A condition where one vertebra slips over another, causing instability and nerve compression.
- Spinal deformities: Curvatures or misalignments that lead to nerve pressure and pain.
How the Body Part Normally Works? (Relevant Anatomy)
The lumbar spine consists of five vertebrae (L1-L5) that provide stability and support to the upper body. Between each vertebra is an intervertebral disc, which acts as a shock absorber, allowing for movement and flexibility. When these discs degenerate or become damaged, it can lead to nerve compression, causing pain, numbness, and weakness.
What You Might Feel – Symptoms (Clinical Presentation)
Common symptoms of lumbar spine issues that may require ALIF include:
- Severe lower back pain, especially when standing or walking.
- Radicular pain (sciatica) that radiates down the legs.
- Numbness, tingling, or weakness in the legs.
- Loss of mobility and difficulty bending or twisting.
- Severe pain that worsens with movement and improves with rest.
How Doctors Find the Problem? (Diagnosis and Imaging)
Diagnosis begins with a physical examination to assess muscle strength, reflexes, and pain levels. Imaging tests, such as MRI or CT scans, are used to visualize the spine, assess disc degeneration or herniation, and evaluate nerve compression. X-rays may also be used to evaluate spinal alignment and identify potential deformities.
Classification
Spinal conditions that may be treated with ALIF can be classified based on their severity:
- Mild: Minor disc degeneration or bulging without significant nerve compression.
- Moderate: Disc herniation with nerve compression causing pain or weakness.
- Severe: Advanced degeneration, spondylolisthesis, or deformities leading to significant nerve damage and functional impairment.
Other Problems That Can Feel Similar (Differential Diagnosis)
Other conditions that may cause similar symptoms include:
- Muscular strain or ligament injury.
- Kidney stones or infections.
- Sciatica from piriformis syndrome.
- Hip joint issues like arthritis or labral tears.
Treatment Options
Non-Surgical Care: Conservative treatments, including physical therapy, medications (e.g., NSAIDs), epidural steroid injections, and lifestyle changes, are typically the first line of treatment.
Surgical Care: ALIF is considered when conservative treatments fail to relieve symptoms. Other options may include posterior lumbar fusion or minimally invasive spine surgeries.
The ALIF Procedure
Patients undergoing ALIF are given general anesthesia, rendering them unconscious and unable to feel pain. The patient is positioned on a specially designed operating table with their back down.
- Incision and Exposure:
- An oblique incision is made on the left side of the abdomen.
- Abdominal muscles are split and retracted, revealing the peritoneum, a protective covering of the abdominal organs.
- The surgeon carefully retracts the peritoneum to one side, avoiding the sympathetic nerve plexus and major blood vessels, with assistance from a vascular surgeon.
- Disc Removal and Grafting:
- Special forceps are used to remove the intervertebral disc material and any structures compressing the neural elements.
- The adjacent vertebrae are distracted (gently separated) to insert a cage filled with bone graft material. The bone graft can be autologous (from the patient’s pelvic bone) or obtained from a bone bank.
- Stabilization:
- The construct is stabilized using screws and plates from the front or screws and rods from the back.
- If needed, a posterior surgery may also be performed for additional stability and decompression.
- Closure:
- The incisions are closed in layers, and a bandage is applied.
Advantages of the Anterior Approach
The anterior approach in ALIF has several benefits over the posterior approach:
- Muscle Preservation: The back muscles are not cut or separated, which is common in posterior approaches. This preservation leads to reduced postoperative pain and better muscle function.
- Avoiding Dural Manipulation: The anterior approach does not involve disturbing the dural sac (the protective covering of the spinal cord), reducing the risk of dural scarring and related complications.
- Larger Implants and Better Compression: Surgeons can place larger cages and compress the bone graft more effectively, enhancing the fusion process.
- Better Access to Pathologies: Conditions located at the front of the spine are more accessible and manageable through the anterior approach.
- Ideal for Revision Surgeries: Patients who have undergone previous posterior surgeries are often good candidates for the anterior approach, providing an alternative route for additional procedures.
Recovery and What to Expect After Treatment
Patients who undergo ALIF surgery can expect:
- Immediate Postoperative Care: Most patients are able to walk the same day or within a few hours of surgery.
- Early Recovery: Patients typically remain in the hospital for 1-3 days, with some returning to normal activities within a few weeks.
- Long-Term Recovery: Full recovery and return to regular activities may take 3-6 months, depending on the complexity of the surgery and the patient’s overall health.
Possible Risks or Side Effects (Complications)
As with any surgery, ALIF carries some risks, including:
- Infection at the surgical site.
- Nerve damage, which may lead to weakness or numbness.
- Vascular injury, particularly due to the proximity of major blood vessels.
- Organ damage to the peritoneum and abdominal organs.
- Failure of fusion where the vertebrae do not fuse as expected.
- Retrograde ejaculation (in men) due to nerve damage.
Long-Term Outlook (Prognosis)
The prognosis for patients undergoing ALIF is generally positive. Most patients experience significant pain relief, improved function, and better quality of life. However, long-term follow-up is necessary to monitor the success of the fusion and ensure proper healing.
Out-of-Pocket Cost
Medicare
CPT Code 22558 – Anterior Lumbar Interbody Fusion Surgery (ALIF): $368.50
Under Medicare, 80% of the approved amount for this procedure is covered once the annual deductible has been met. The remaining 20% is typically the patient’s responsibility. Supplemental insurance plans—such as Medigap, AARP, or Blue Cross Blue Shield—generally cover this 20%, leaving most patients with little to no out-of-pocket expenses for Medicare-approved ALIF procedures. These supplemental plans work directly with Medicare to ensure full coverage for the surgery.
If you have secondary insurance—such as Employer-Based coverage, TRICARE, or Veterans Health Administration (VHA)—it serves as a secondary payer once Medicare has processed the claim. After your deductible is satisfied, these secondary plans may cover the remaining balance, including coinsurance or any uncovered charges. Most secondary insurance plans have a modest deductible, typically between $100 and $300, depending on the specific policy and network status.
Workers’ Compensation
If your spinal condition requiring ALIF surgery is work-related, Workers’ Compensation will fully cover all treatment-related costs, including surgery, hospitalization, and rehabilitation. You will have no out-of-pocket expenses under an accepted Workers’ Compensation claim.
No-Fault Insurance
If your spinal condition or injury is the result of a motor vehicle accident, No-Fault Insurance will cover the full cost of your surgery, including anterior lumbar interbody fusion. The only potential out-of-pocket expense may be a small deductible depending on your individual policy terms.
Example
John, a 64-year-old patient with degenerative disc disease and spinal instability, underwent anterior lumbar interbody fusion (CPT 22558) to stabilize his spine and relieve pain. His estimated Medicare out-of-pocket cost was $368.50. Since John had supplemental insurance through Blue Cross Blue Shield, the 20% that Medicare did not cover was fully paid, leaving him with no out-of-pocket expenses for the surgery.
Frequently Asked Questions (FAQ)
Q. How long does recovery from ALIF surgery take?
A. Recovery from ALIF surgery varies, but most patients experience significant pain relief within a few weeks. Full recovery and return to normal activities may take 3-6 months.
Q. Are there any risks associated with ALIF surgery?
A. Risks include infection, nerve damage, vascular injury, and organ damage. The risk of complications is relatively low, and the procedure is considered safe when performed by a skilled surgeon.
Q. Will I need additional surgery after ALIF?
A. In some cases, additional surgeries such as posterior fusion may be needed, but most patients achieve long-term relief with ALIF alone.
Summary and Takeaway
Anterior lumbar interbody fusion (ALIF) is a safe and effective surgical option for treating lumbar spine conditions like herniated discs, degenerative disc disease, and spinal deformities. By accessing the spine from the front, ALIF minimizes muscle disruption, reduces pain, and promotes faster recovery. As with any surgical procedure, a thorough consultation with a qualified spine surgeon is necessary to determine the best treatment approach for your specific condition.
Clinical Insight & Recent Findings
A recent study conducted a systematic review and meta-analysis to evaluate the safety and analgesic efficacy of preoperative regional anesthetic blocks, such as the transversus abdominis plane (TAP) block, in patients undergoing anterior lumbar interbody fusion (ALIF).
The study found that preoperative regional blocks significantly reduced opioid requirements at 48 and 72 hours post-surgery. However, the reduction in pain scores at 24 hours did not reach statistical significance.
Despite these findings, the study suggests that TAP and rectus sheath blocks are reasonably safe and can effectively reduce opioid consumption, offering potential benefits in postoperative pain management, especially given the risks associated with opioid use in this patient population. (“Study of regional anesthetic blocks in ALIF surgery – see PubMed“)
Who Performs This Treatment? (Specialists and Team Involved)
ALIF is typically performed by orthopedic spine surgeons or neurosurgeons with specialized training in complex spinal procedures.
When to See a Specialist?
If you experience persistent or worsening back pain, leg weakness, or numbness, consult a spine specialist to evaluate whether ALIF or another treatment is appropriate.
When to Go to the Emergency Room?
Seek emergency care if you experience sudden and severe pain, loss of bladder or bowel control, or new weakness or paralysis in the legs.
What Recovery Really Looks Like?
Recovery from ALIF is generally quicker than traditional open spine surgeries. Patients can typically return to daily activities within a few weeks, with full recovery taking a few months.
What Happens If You Ignore It?
Untreated lumbar spine conditions can lead to worsening pain, decreased mobility, and permanent nerve damage. Early intervention can prevent further complications and improve long-term outcomes.
How to Prevent It?
Maintaining a healthy weight, staying active, and practicing proper posture can help prevent lumbar spine issues. Regular exercise, especially core strengthening, is essential for spinal health.
Nutrition and Bone or Joint Health
A diet rich in calcium and vitamin D supports bone health. Weight-bearing exercises help maintain strong bones and prevent degeneration.
Activity and Lifestyle Modifications
Post-surgery, patients should avoid heavy lifting and twisting movements. Continuing physical therapy is essential for a full recovery and to prevent future issues.
Do you have more questions?
What conditions are typically treated with ALIF?
ALIF is commonly used to treat conditions such as degenerative disc disease, herniated discs, traumatic anterior extradural compression, deformities, and tumors in the lumbar spine. It may also be used for lumbar disc replacement and revision surgeries.
Why is the anterior approach preferred over the posterior approach in some cases?
The anterior approach avoids cutting or separating the back muscles, leading to reduced postoperative pain and faster recovery. It also allows the surgeon to place larger cages and better address pathologies located at the front of the spine.
What are the main risks associated with ALIF?
Risks include damage to major blood vessels, potential injury to abdominal organs, retrograde ejaculation in male patients, infection, nonunion of the fusion, and implant-related issues. However, these complications are relatively rare.
How long is the recovery period after ALIF?
Patients are encouraged to walk on the first day after surgery and can usually resume daily activities within a few weeks. Full recovery, including bone fusion, can take several months, depending on individual factors and adherence to postoperative guidelines.
What types of implants are used in ALIF?
Implants typically include metal or PEEK (polyether ether ketone) cages filled with bone graft material. Screws and plates or rods are used to stabilize the construct until fusion occurs.
Is general anesthesia always required for ALIF?
Yes, ALIF is performed under general anesthesia to ensure the patient is unconscious and does not feel pain during the procedure.
Where is the bone graft material obtained from?
Bone graft material can be harvested from the patient’s pelvic bone (autograft) or obtained from a bone bank (allograft).
What postoperative care is necessary following ALIF?
Postoperative care includes early mobilization, avoiding heavy lifting and bending, and following a rehabilitation program as prescribed by the surgeon. Pain management and wound care are also important aspects of recovery.
Can ALIF be performed on patients with previous spine surgeries?
Yes, ALIF can be an excellent option for patients who have had previous posterior spine surgeries, as it provides an alternative route for accessing and treating the spine.
What is the success rate of ALIF?
The success rate of ALIF is high, with most patients experiencing significant pain relief and improved spinal stability. Long-term studies indicate sustained benefits and low complication rates.
How does ALIF compare to other spinal fusion techniques?
ALIF offers advantages such as muscle preservation, better implant placement, and more direct access to certain spinal pathologies. Compared to posterior approaches, it often results in less postoperative pain and faster recovery.
What symptoms indicate the need for ALIF?
Symptoms that may indicate the need for ALIF include chronic lower back pain, leg pain, numbness or weakness due to nerve compression, and spinal instability.
What are the alternatives to ALIF?
Alternatives include posterior lumbar interbody fusion (PLIF), transforaminal lumbar interbody fusion (TLIF), and less invasive techniques such as minimally invasive spinal fusion, depending on the specific condition and patient needs.
How does the surgeon decide between using an anterior or posterior approach?
The decision is based on the specific spinal pathology, the location and extent of disc degeneration or compression, the patient’s anatomy, and previous surgical history. A thorough evaluation and imaging studies guide this decision.
Can ALIF address multiple levels of the spine at once?
Yes, ALIF can be used to address multiple levels of the lumbar spine in a single surgery, although this depends on the patient’s specific condition and overall health.
What is the typical duration of an ALIF surgery?
The duration of ALIF surgery varies but typically ranges from 2 to 4 hours, depending on the complexity of the case and whether additional procedures (such as posterior stabilization) are performed.
What are the signs of a successful fusion after ALIF?
Signs of successful fusion include the absence of pain or significant reduction in pain, stability in the treated spinal segment, and evidence of bone growth and fusion on follow-up imaging studies.
How soon can patients return to work after ALIF?
The timeline for returning to work varies based on the individual’s job demands and recovery progress. Light-duty work may be possible within a few weeks, while more physically demanding jobs may require several months before a full return.
What are the long-term outcomes of ALIF?
Long-term outcomes are generally positive, with many patients experiencing sustained pain relief, improved function, and enhanced quality of life. Regular follow-up with the surgeon ensures monitoring of fusion progress and early identification of any issues.
Is there a risk of needing additional surgeries after ALIF?
While ALIF aims to provide a lasting solution, some patients may require additional surgeries if new spinal issues arise or if the initial fusion does not achieve the desired stability.
Can ALIF be combined with other treatments for better results?
Yes, ALIF can be combined with posterior fusion techniques or other spinal treatments, such as decompression surgery, to address complex cases and enhance overall outcomes.
How do patients manage pain after ALIF?
Pain management may involve medications, physical therapy, and other modalities such as heat/cold therapy. The surgeon will provide a comprehensive pain management plan tailored to the patient’s recovery process.
What kind of rehabilitation is involved after ALIF?
Rehabilitation typically includes physical therapy focused on strengthening the core muscles, improving flexibility, and gradually increasing activity levels. A personalized rehab plan is created based on the patient’s progress and specific needs.


