A 71-year-old retired practice manager presented to our office with complaints of bilateral knee pain which was worse on the left side. The pain was described as severe in severity. The patient describes the pain as sharp, stabbing, and aching. The pain was constant and disturbed his sleep.
The pain was not associated with numbness, tingling and radiating pain. The problem was getting worse since it started. Walking, standing, lifting, exercising, twisting, lying in bed, bending, squatting, kneeling, using stairs and sitting made the symptoms worse. Pain medications made the symptoms better.
The patient first noticed the pain a couple of years back without any precipitating event. She denied any trauma to the knees. The pain gradually worsened over time. For the past few months, he was unable to even stand or walk to the store without discomfort.
He found it increasingly difficult driving or getting up from a toilet chair. He was currently living with his wife. He denied the use of any recreational drugs or smoking. He was calm, conscious, cooperative and well oriented to time, place and person. He denied any drug allergies. His past medical history was positive for asthma, benign prostate hypertrophy, and hypertension, all well controlled with medications.
The patient reported cortisone knee injections and physical therapy for knee pain. With conservative methods, the relief only lasted for a few days. The patient was distressed with constant knee pain.
On his examination, his gait was antalgic with a reduced stance phase on the left side. He used a cane as a walking aid. There was a presence of mild swelling in the left knee with normal overlying skin. There were no scars, sinuses or erythema of the skin.
Tenderness was present along the medial and lateral joint line. Patellar facet tenderness was also present. The anterior drawer, posterior drawer, Lachman, valgus and varus stress test was negative for instability. The range of motion was painful terminally (5 to 90 degrees). There was no genu varum or genu valgus deformity.
Imaging revealed severe tricompartmental osteoarthritis of the left knee with obliteration of the medial joint space and copious osteophyte.
In view of lifestyle limiting osteoarthritis of the left knee, he was advised to undergo custom left knee total replacement. Risks, benefits, and alternatives were discussed with the patient at length. He agreed to the procedure.
As a part of the preparation, a preoperative CT scan of the patient’s left knee along with ankle and hip was taken. The patient’s unique anatomy was utilized to build customized implants. Accurate bone cuts and offsets were determined from the CT scan data. Disposable bone jigs were made to match the patient’s unique anatomy. A preoperative plan was formed.
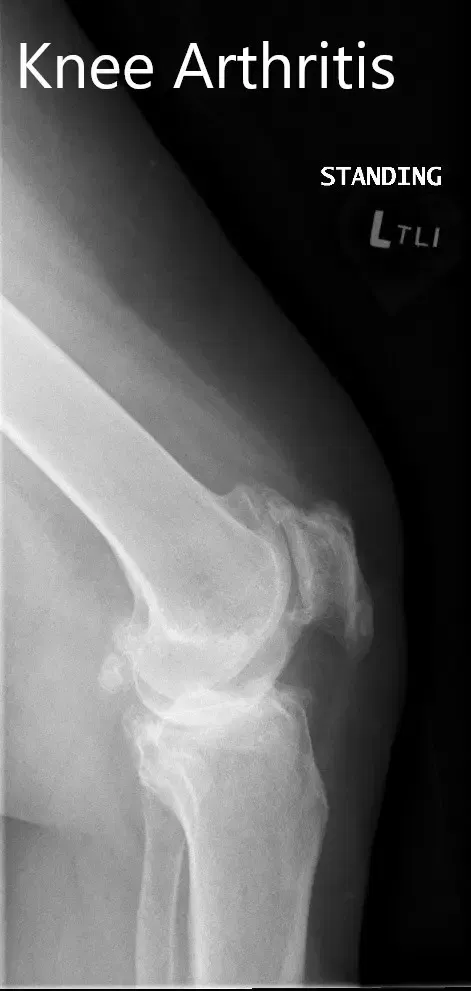
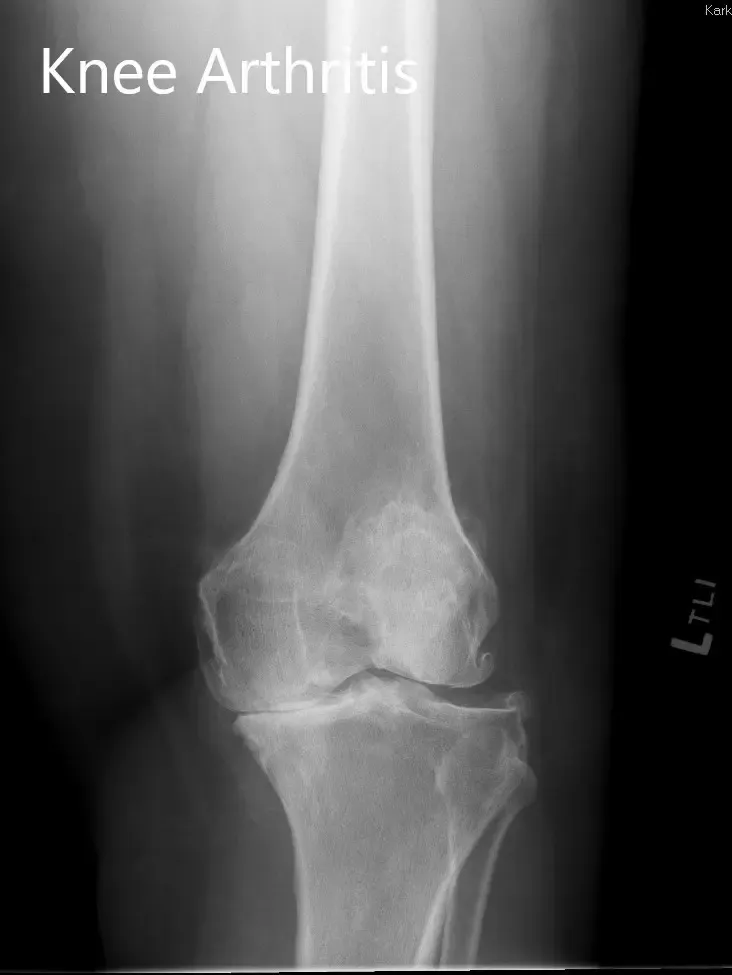
Preoperative X-ray showing the lateral and the AP views
OPERATION: Left total knee arthroplasty.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were discussed with the patient prior to the procedure.
The left lower extremity was then draped and prepped in the usual sterile manner. A tourniquet was used and the lower extremity was then exsanguinated.
A straight incision was used for the arthrotomy. Skin and subcutaneous tissue were incised and medial parapatellar arthrotomy was then performed. The tibia was then exposed. The tibial resection was then made using the guides and tibial preparation as then performed.
The alignment was found to be correct. The femur was then prepared. The distal cuts, the chamfer cuts, and the notch cut were used using customized guides. The medial and lateral meniscus was then removed using lamina spreaders and the posterior osteophytes were then removed using curved osteotomes and a curette. Gap balancing was performed and found to be correct.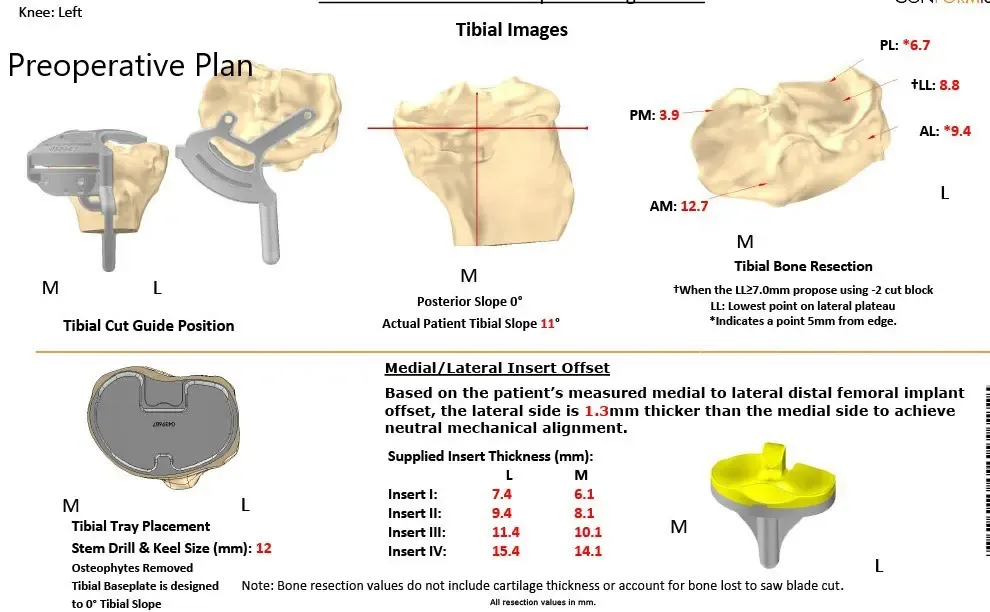
Complete Orthopedics patient specific surgical plan for a custom left knee replacement in a 71-year-old-male.
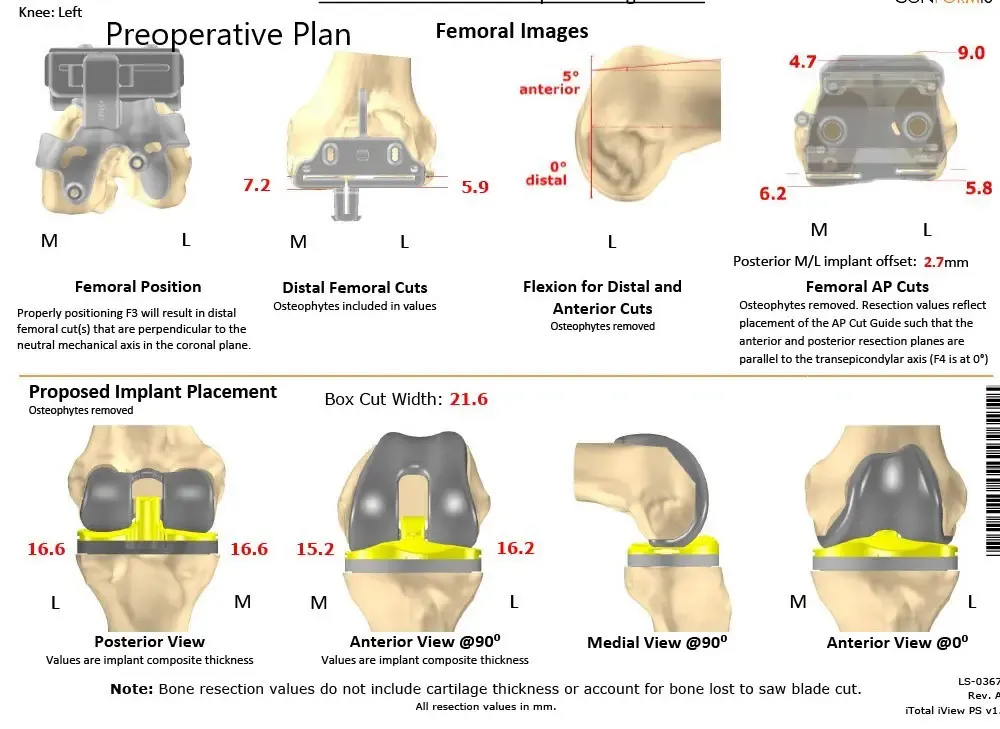
Complete Orthopedics patient specific surgical plan for a custom left knee replacement in a 71-year-old-male (scan-2)
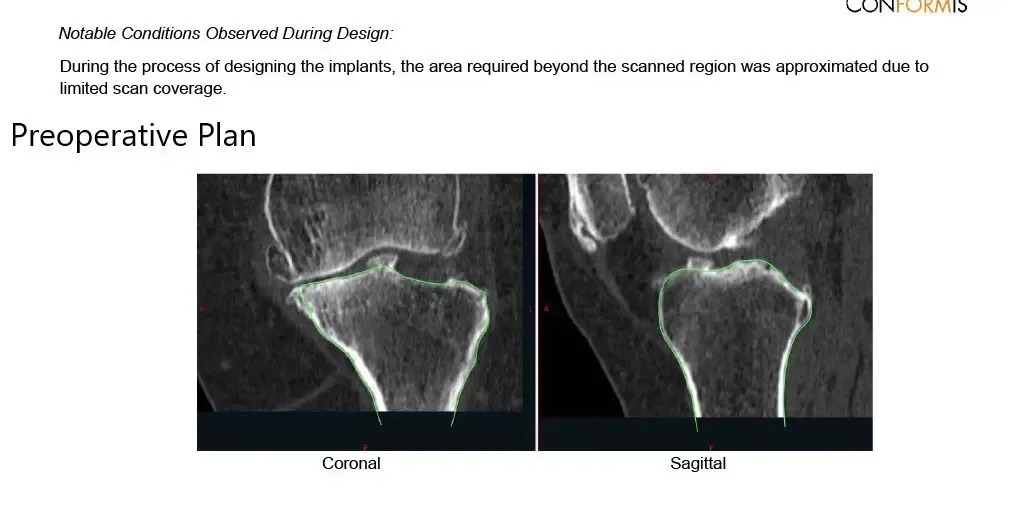
Complete Orthopedics patient-specific surgical plan for a custom left knee replacement in a 71-year-old male (scan 3)
The patellar resection was then made and drill holes were then made in the patella. The trial patella was then placed into position. The trial femur was placed into position followed by the trial tibia. The poly was placed into position. The knee was reduced. The knee was then trialed through a full physiological range of motion.
Full-extension was obtained. Full flexion was obtained. Patellar tracking was excellent. The trial components were then removed. A thorough lavage was performed. An injection was given.
The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was then removed.
Poly was then placed into position. The knee was then reduced and held in full extension with a bump under the ankle. The patella was then cemented into position and excess cement was removed. Medial parapatellar arthrotomy was then closed with Vicryl and barbed suture.
Cutaneous tissues were closed with 2-0 Vicryl, the skin was closed using subcuticular sutures, a dressing was applied and the patient w s then transferred to the postoperative care unit in stable condition.
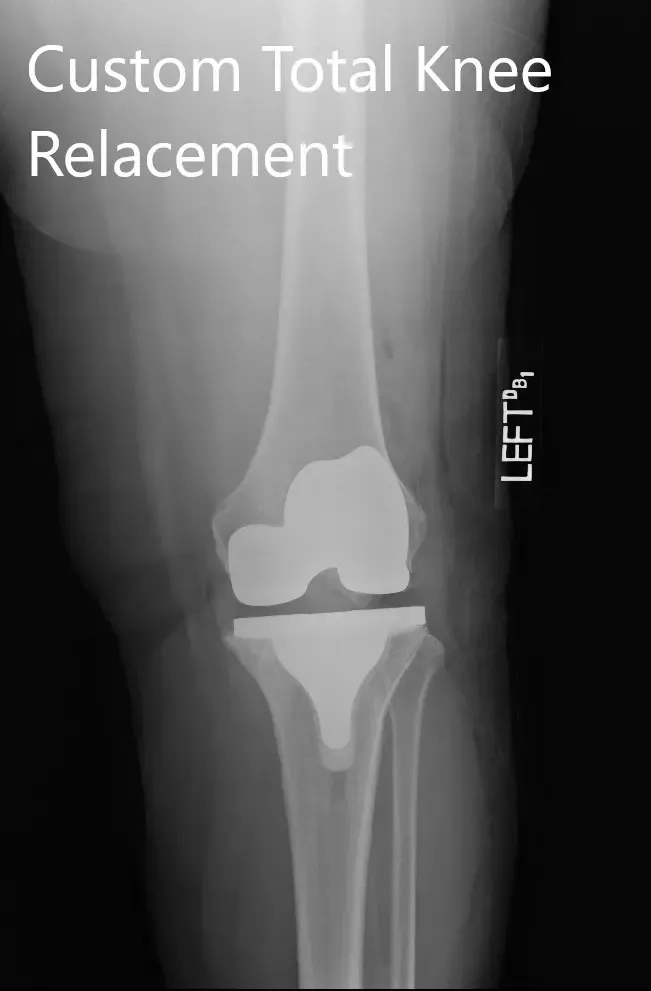
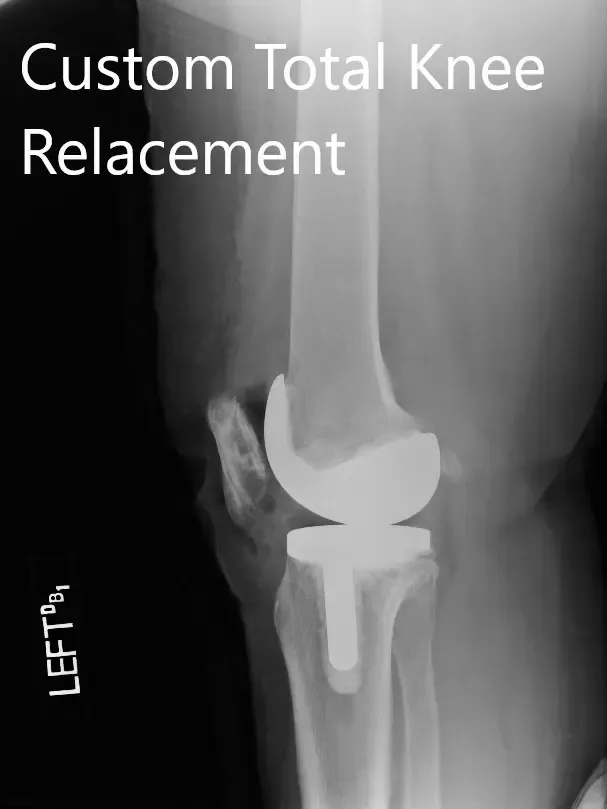
Postoperative X-ray images showing the AP and lateral views of the left knee
Post-op weight-bearing was started on the same day of the surgery. He was able to walk for 50 feet. The pain was well controlled with medications. Aspirin 325mg BID was started for DVT prophylaxis.
The patient demonstrated a full range of motion of the left knee. Physical therapy focusing on muscle strengthening and flexibility was continued. After 2 months, the patient was happily driving his car, performing his daily activities and brought a picture of him playing golf. He follows up as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


