An 80-year-old female presented to our office with complaints of left hip pain with discharge for the past 6 months. The patient had a left anterior total Hip replacement done by an outside physician. The patient was unable to bear weight on the right side and was using crutches as a walking aid. She was emotionally distressed and was accompanied by her son.
The patient was a retired school teacher with a medical history of osteoarthritis, coronary stents, dyslipidemia, and hypertension. The patient stated she underwent total anterior hip replacement 7 months ago. She had worsening pain in the left hip after the procedure with a subsequent discharge and swelling anteriorly. She was unable to bear weight on the left side but denied any history of falls.
On her office visit, she described the pain as moderate in intensity (5/10) and a dull ache in character. Her physical examination revealed redness, warmth and necrotic tissues around the proximal part of the incision anteriorly on the left side. The necrotic tissues extended 1 cm away from the incision on both sides superiorly. The drainage was scant serous in nature.
There was tenderness on superficial and deep palpation of the Scarpa’s triangle. The range of motion about the hip was limited due to pain. Internal and external rotation of the Hip was especially painful. Further, examination revealed no deficit of the distal neurovasculature structures. The examination of the bilateral knee and ankle was normal.
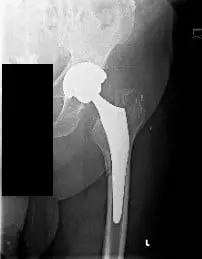
Preoperative X-ray of the Left Hip AP view showing a periprosthetic femoral fracture (minimally displaced along the medial aspect of the proximal femoral shaft) with subsidence of the stem.
Risks, benefits, and alternatives were discussed extensively with the patient and her son. She was made aware of the high risk associated with the surgery due to her co-morbidities. Alternatives such as nonoperative management, staged revision surgery and single-stage revision surgery was discussed with the patient at length. She was deemed as a suitable candidate for a staged revision. She agreed with the plan and decided to go ahead with the surgery.
Surgery
Removal of the implant, irrigation, and debridement, fixation of the periprosthetic fracture with cerclage cables and placement of antibiotic spacer.
IMPLANTS USED: Biomet cable system x3 with a hip cement mold 56 mm head with hip stem 15 mm, stage 1 prosthesis.
PROCEDURE: The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist. The patient was then definitively positioned with the left hip up and the left hip was then draped and prepped in the usual sterile manner. Care was taken to ensure that the anterior incision was in the field for debridement.
The posterior approach was used for arthrotomy. Skin and subcutaneous tissues were incised. Posterior soft tissue structures were then taken down and tagged for future repair. The hip was then dislocated. The femoral component was then removed.
Attention was then turned to the acetabulum. The explant was used and the cup was then removed. Thorough debridement was done on both sides, acetabular and femoral side. Acetabular membrane, femoral membrane. and periprosthetic tissue was then sent for culture and sensitivity and for pathology. The cup was then reamed to the fresh bone.
Attention was then turned towards the femur. The femoral fracture was then fixed with three cables and the cables were then tightened. Attention was then turned towards the intramedullary canal. The femur was then sequentially reamed and broached and the final broach was left into position.
The head and the tendon were then placed over the trunnion and trial reduction was carried out. The length was found to be correct. The hip was stable in all physiological range of motion. The hip was then dislocated. Thorough lavage was given again.
The final tightening of the cables was then performed. The final cement antibiotic spacer was then placed into position and the hip was then reduced. The cables were finally tightened again and they were crimped. The ends of the cables were then cut. Thorough lavage was given again and injection was given. Fascia was closed. Subcutaneous tissue was then closed.
Attention was then turned towards the anterior wound and thorough debridement was performed. The anterior wound was then irrigated and the closure was then performed with #2 nylon. The posterior soft skin was closed with staples. Sterile dressing was applied over the wound and the patient was then transferred to the postoperative care unit in stable condition.
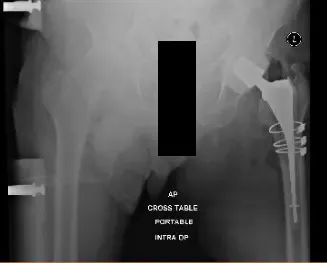
Postoperative X-ray showing AP view of pelvis with both hips, Left Hip has cerclage wires and antibiotic spacer in situ.
The Patient was prescribed i.v antibiotics in the form of vancomycin and meropenem. She was also started on Eliquis 2.5 mg BID for deep vein thrombosis (DVT) prophylaxis. On her subsequent, the posterior surgical wound was clean, dry and intact. The anterior wound was healthy without any discharge. There was no neurovascular deficit and the patient was compliant with hip precautions and using abduction pillow.
Aspiration: The patient was following up with his physical and occupational therapy with excellent pain control. On her subsequent visits both the anterior and posterior surgical wound healed well and had no signs of discharge or inflammation.
Aspiration of the left hip joint was performed to rule out infection with cell count and differential. The results demonstrated no growth. The patient was planned for antibiotic spacer removal and revision hip replacement after 11 weeks of the first surgery.
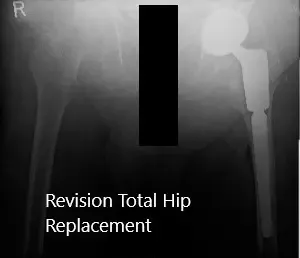
Postoperative X-ray of the pelvis with both hips shows total hip replacement of the left hip with no acute fractures.
The patient had an excellent recovery postoperatively. The pain was well managed with medications and she was started on Eliquis 2.5 mg BID for DVT prophylaxis. On subsequent visits, her wound was dry, clean and intact. The staples were removed and the patient went through a period of physical therapy. She was bearing weight on the left hip as tolerated and was compliant with hip precautions.
After 3 months the patient had successfully concluded her physical therapy and was now able to walk free of pain. She was able to play with her grandkids and was able to climb stairs and go on extended walks. She was extremely happy with her outcome.


