A 74-year-old female presented to our office with complaints of bilateral groin pain for the past four years. She denied any preceding trauma or fall and didn’t remember the specific onset of pain. The pain progressed gradually with an insidious onset.
The pain was described as a sharp to dull pain in both the groins (left >right). There was radiation to the medial knee and buttocks posteriorly. The intensity of the pain was moderate, which would be severe on activity.
She described exacerbation of pain with activities such as prolonged walking, going up and down the stairs, bending, squatting and getting up from a chair.
She stated her mother also suffered from bilateral knee and hip arthritis and so did her sister. She was a nonsmoker and social drinker. There was no history of any inflammatory dis jointease or multiple joint pains.
The patients previously tried conservative management in the form of hip cortisone injections, heat pads and physical therapy without significant relief. Her walking tolerance was limited to a block secondary to pain. She used a cane as an assistive device for walking.
She was a retired professor and before the onset of pain maintained an active lifestyle. She loved traveling outdoors and photographing the streets, a hobby she was no longer able to pursue. She was dismayed at her decreased mobility.
She denied any known drug allergies. Her past medical history was positive for migraines, gastroesophageal reflux disease, dyslipidemia, and hypertension. Her current medications included Topiramate, Simvastatin, Pantoprazole, and Vasotec. All her medical conditions were well controlled with medications.
On physical examination, she walked with an antalgic gait. Both the shoulders, iliac spines, patella, and medial malleolus were at the same level. There was no exaggeration of lumbar lordosis. There was no atrophy of the buttocks and thigh muscles.
On the supine examination, both the anterior superior iliac spines were at the same level. There was no fullness in the Scarpa’s triangle. Tenderness was present on the bilateral anterior joint line. There were no enlarged inguinal lymph nodes. There was no thickening or broadening of the trochanter.
The range of motion of both the hips was restricted in the abduction and internal rotation due to pain. There was no fixed coronal, sagittal or axial plane deformity. Bilateral trochanters were at the same level and there was no leg length discrepancy.
The examination of the bilateral knees and ankles was normal. There as no distal neurological deficit and bilateral extremity pulses were palpable and comparable. The power and sensory examination of both lower extremities were unremarkable.
Imaging studies revealed severe bilateral osteoarthritis of the hips with subchondral cysts, sclerosis, and osteophytes. Considering the lifestyle limiting hip pain, she was advised bilateral total hip replacement. She agreed to go ahead with the procedure.
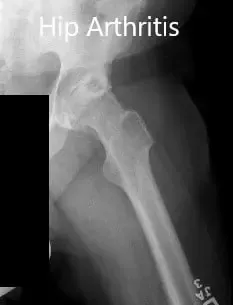
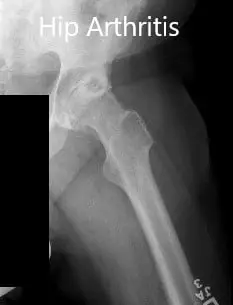
Preoperative X-ray showing the frog-leg lateral views of the right and the left hip joint.
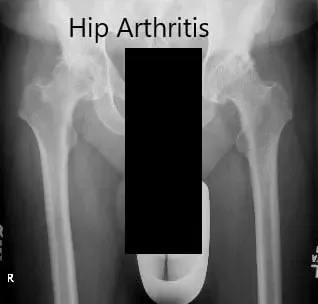
Preoperative X-ray showing the AP view of the pelvis with both the hips.
OPERATION: Bilateral total hip arthroplasty.
IMPLANTS USED: Bilateral 54-mm acetabular shell with a 6.5-mm screw, 25 mm with, 0-degree polyethylene 36-mm with 127 degrees size 5 stem with femoral head, 36 mm plus 0.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room. After obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as the family prior to the procedure. The left hip was more painful, and it was decided to do the left hip first.
The patient was brought to the operating room and anesthesia was obtained by the Anesthesiology. The patient was definitely positioned with the left hip up, and the left hip was then draped and prepped in the usual sterile manner. A curved incision centered over the greater trochanter was used for the arthrotomy. Skin and subcutaneous tissues were incised.
The fascia was then divided. The posterior soft tissue structures were then taken down and tacked for future repair. The hip was dislocated. The lesser trochanter center distance was measured, as compared to the preoperative planning and additionally, the center of the head and the tip of the trochanter was used with preoperative findings.
A neck resection was then made. The head was then removed. Attention was then turned towards the acetabulum. The remainder of the labrum was then removed. The acetabulum was then sequentially reamed, and the final shell was then positioned in the correct abduction and eversion.
The screw was used for additional fixation. A poly was then used over the shell, and attention then turned towards the femur. The remainder of the tissue under the greater trochanter was removed. The femur was then sequentially broached.
The final broach was left into position. The trunnion and the head were then placed over the broach. Lesser trochanter distance again was measured. The distance above the tip of the greater trochanter was then measured and was found to be accurate.
The hip was then reduced and trialed through the physiological range of motion, and the hip was found to be stable in all physiological range of motion.
The hip was then dislocated. The trial components were then removed. The final components were then placed into position. The hip was then relocated. A thorough lavage was given. The injection was given for postoperative pain control.
The drill holes were made in the greater trochanter, and the posterior soft tissue structures were then tacked to the greater trochanter through transosseous tunnels.
The fascia was closed, subcutaneous tissues were closed, subcuticular tissues were closed, and the skin was then closed using staples. A sterile dressing was applied over the wound.
The patient was then turned to the other side, and the right hip was then draped and prepped in the usual sterile manner. The right hip replacement was done in a similar fashion. The patient was then transferred to the postoperative care unit in stable condition.
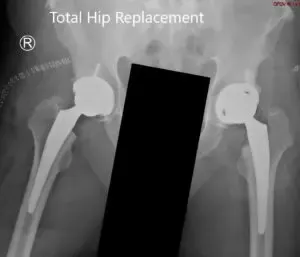
Postoperative X-ray showing the AP view of the pelvis with both hips.
Post-op, the pain was managed well with medications and she was advised hip precautions. Aspirin 325mg BID was started for deep vein thrombosis prophylaxis. Gait training and fall prevention education was given to the patient.
Physical therapy to strengthen the muscles and increase flexibility was started. The sutures were removed uneventfully. Two months post-op she was able to walk without support and reported zero pain.
The hip precautions were weaned off gradually. She was back to her regime and enjoyed walking without any discomfort or limitation. She follows as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


