A retired businessman presented as a new patient complaining of bilateral knee pain. The pain was worse in the right knee. He stated that he first noticed the pain a couple of years back located medially on both knees. The pain was worse on going up and down the stairs and including activities such as walking or twisting. The pain was moderate to severe in intensity (7/10) and sharp to dull aching in character.
The patient loved to travel and worked as a volunteer at a rescue dog center. However, recently he has limited his volunteer work and was not able to travel in the past 1 year secondary to knee pain. He stated he had become inactive and constantly worried about being bedridden with the current state of knee pain. He expressed difficulty in sitting for extended periods of time.
He had reportedly tried a myriad of treatment options such as heat pads and cortisone injections but feels the relief doesn’t last. He regularly goes to physical therapy and does a home exercise program but with no relief. He is a former smoker with a medical history of diabetes mellitus and hypertension, both well controlled with medications. He is currently taking Vasotec, Toprol xl and metformin.
The patient stated a desire to get back to his daily routine and hobbies free from knee pain. He was accompanied by his wife who was equally distressed with his arthritis.
His physical examination revealed tenderness in bilateral medial joint line and medial patellar facet which was especially worse on the right side. There was mild joint effusion (R>L). There was no evidence of any signs of acute inflammation or infection.
The range of motion on both the knees was full of copious crepitus. He walked with an antalgic gait with a reduced stance phase on the right side. There was mild genu varus deformity. There was a small reduction of abduction and internal rotation on the right hip compared to the left. Mild right trochanteric tenderness was present.
Imaging revealed severed tricompartmental osteoarthritis of the bilateral knee (right greater than left) with osteophytes and medial joint space reduction.
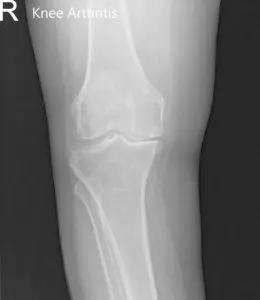
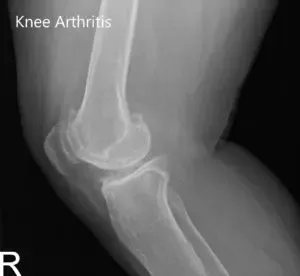
Preoperative X-ray of the right knee showing AP and lateral views
Considering his lifestyle limiting knee pain, various management options in the form of nonoperative and operative were discussed with him at length. He was found to be a candidate for custom knee replacement. Risks, benefits and potential complications due to his age and comorbidities of diabetes and hypertension were discussed with him. The patient decided to go ahead with custom total knee replacement of the right knee.
Several weeks before a CT scan of the patient’s right knee with the hip and ankle was obtained. The data generated was used to create a preoperative plan outlining the femoral offsets and bone cuts. Custom implants were then constructed with custom implants unique for the patient. The customization ensured that biomechanics were restored accurately. This would result in a more natural feeling knee.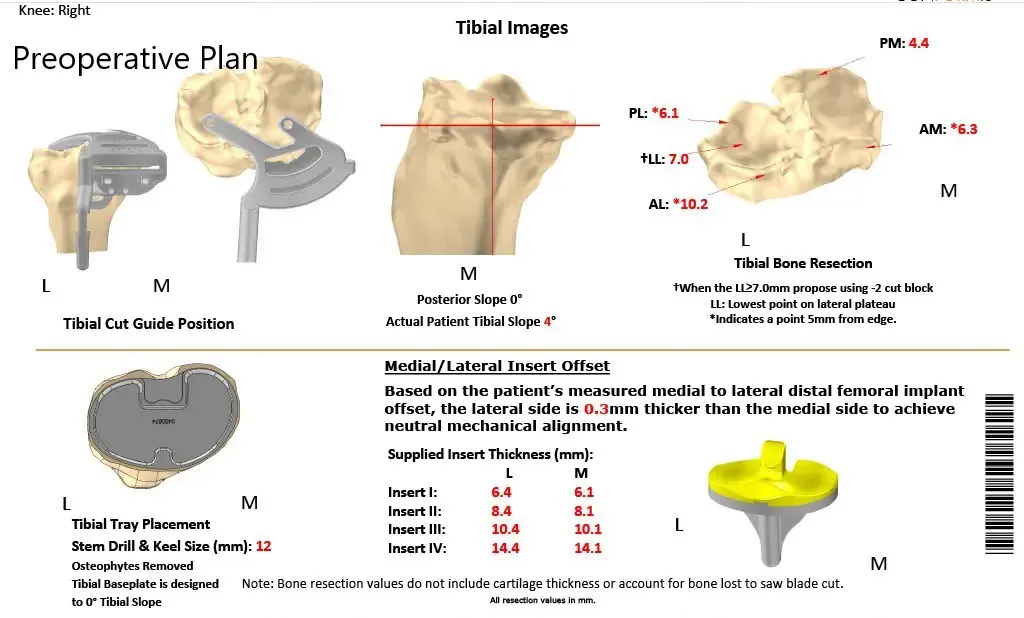
Complete Orthopedics patient-specific surgical plan for a customized right knee replacement in a 71-year-old patient.
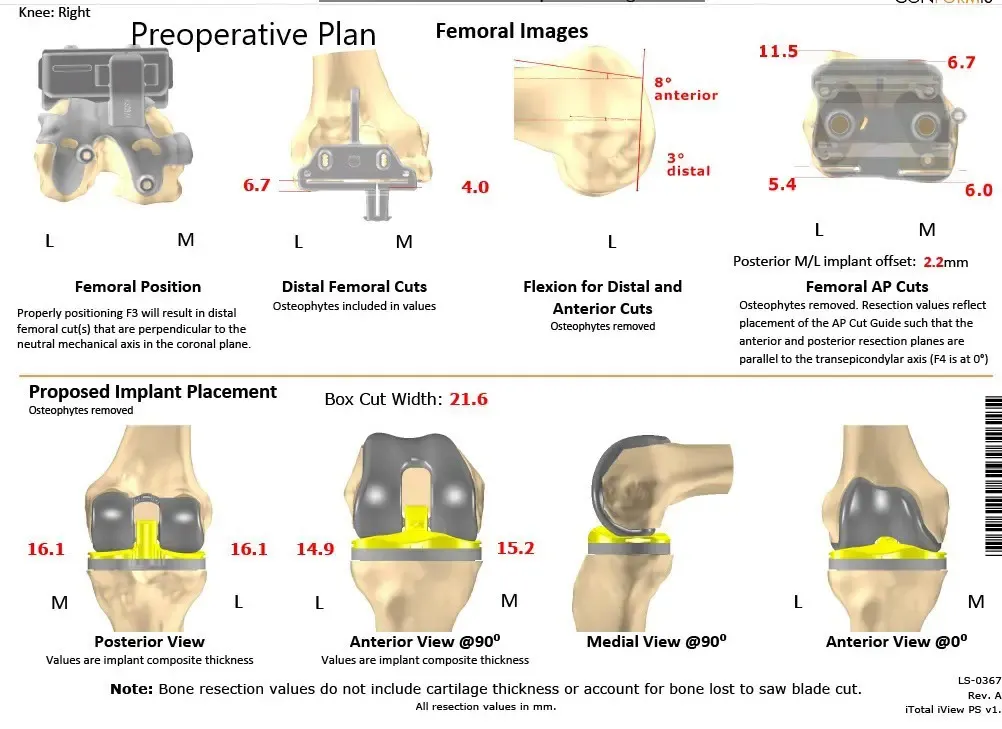
Complete Orthopedics patient-specific surgical plan for a customized right knee replacement in a 71-year-old patient (scan 2)
The patient underwent a right custom total knee replacement.
Implants used: Custom femoral implant with a custom tibial tray with a 6 mm polyethylene insert and 32 mm patella.
Description of procedure: The patient was brought to, the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure.
Anesthesia was obtained by the anesthesiologist. The patient was then definitively positioned and the tourniquet was used to exsanguinate the extremities. A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were incised.
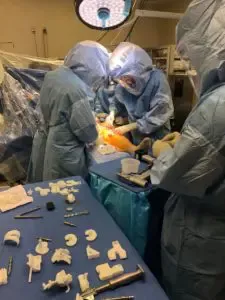
Medial parapatellar arthrotomy was then performed. The tibial cutting guide was used to make the tibial cut and the tibia was then prepared.
Attention was then turned on towards the femur. The femoral cutting guides were used for preparing the femur and then medially and laterally, laminar spreaders were then used and the remainder of the cruciates and the meniscus were then debrided. Gap balancing was performed and found to be perfect.
The patella was resected. Drill holes were made in the patella. The trial patella was placed into position followed by a trial of the femur, trial tibia, and the polyethylene was then placed over the tibia.
The knee was reduced and trialed through a full physiological range of motion and excellent stability and excellent patella tracking was then observed. The trial components were then removed. The injection was given. A thorough lavage was given. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed.
Poly was then placed over the tibia and the knee was reduced and held in full extension with a bump under the ankle. Patella was then cemented into position and held with a patellar clamp. Medial patellar arthrotomy was closed with Vicryl and Stratafix.
The wound was closed in layers. Sterile dressing was then applied over the wound. The tourniquet was then let down, and the patient was transferred to the postoperative care unit in stable condition.
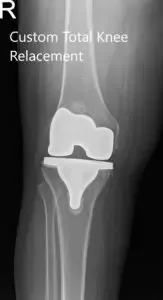
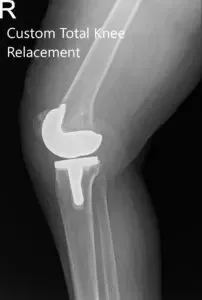
Postoperative X-ray of the right knee showing AP and Oblique views.
He had an excellent recovery from their total knee replacement in the postoperative period. He was able to walk with support the same day of the surgery. The pain was managed with oral medications and was started on aspirin for DVT prophylaxis. On his subsequent visit, the staples were removed and the range of motion was found to be full. He was stressed on the importance of strict control of blood sugar levels and compliance with physical therapy.
Subsequently, the patient followed three months later stating complete relief of pain in the right knee and decreased pain on the left side. He was planning to travel to Phoenix on his grandson’s graduation and was happy with the prospect of doing it without pain. He regularly follows up and will plan for the left knee replacement in the future if required.


