A 78-year-old male presented to our office with complaints of bilateral knee pain. He states the knee pain has worsened over the past 6 months affecting his daily activities. He found difficulty in driving a car or doing his laundry. The patient stated he was emotionally disturbed due to interference in his daily routine.
He was a retired office manager living with his wife. He was currently not working and enjoyed driving to his friend’s house and walk to the local market with his wife. He first noticed the pain while getting up from a chair a few years back. He was not able to recall the exact onset but stated the pain increased over time.
The pain was described as a dull ache located along the inner side of both knees. The intensity was reported to be 6/10 which was exacerbated by walking, going up and down the stairs, bending, turning and getting up from a chair.
He previously had cortisone knee injections and tried physical therapy along with gel injections. The relief was stated to be moderate and only lasted for a few days. The patient was unable to take any NSAIDs due to gastric ulcers.
He was allergic to Avelox and his medical history included hypertension and gastric ulcers. Currently, he was on omeprazole 40mg and amlodipine 10 mg. He was a nonsmoker and nondrinker. He previously had an inguinal hernia repair done 5 years ago.
His physical examination revealed a steady coordinated gait. There was no genu varum or genu valgum deformity. The skin overlying both the knee joints was normal. There was mild knee swelling in both knees (right greater than left).
There was a presence of bilateral medial and lateral joint line tenderness. Bilateral bulk and tone of muscles were normal. The patient had tenderness in bilateral patellar facets. Anterior and posterior drawer, valgus and varus stress tests were negative for any instability.
The range of motion of the right knee was 5-90 degrees and the left knee was 0-90 degrees. The examination of bilateral hips revealed hip bursitis and examination of bilateral ankles was normal. The distal neurological examination was normal. Bilateral lower extremity pulses were palpable and good volume.
Imaging studies revealed bilateral Osteoarthritis of all three compartments. In view of lifestyle limiting knee pain, he was advised bilateral knee total knee replacement. He was found a suitable candidate for customized replacement. After gaining the information about all risks, benefits, and alternatives, the patient agreed to undergo customized bilateral knee replacement.
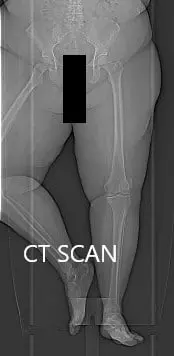
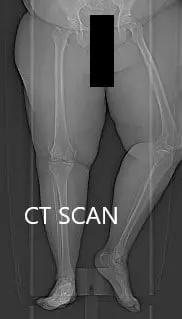
Topographic CT images of the weight-bearing Right and Left knee respectively.
A few weeks prior, a CT scan of the bilateral lower extremities was performed to obtain detailed data on the patient’s unique anatomy and biomechanics of the knees. A preoperative plan was formed to guide the surgeon in bone cuts and offsets. Disposable instruments were custom made for the patient. Unique customized implants were made to match the patients cut surface of the knee.
IMPLANTS USED: Customized knee replacement systems left and right. Bilateral polyethylene size 8 mm and patella size 32 mm x 6 mm.
The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as with the family members prior to the procedure. The right knee was more painful than the left knee and it was therefore decided to do the right knee first.
DESCRIPTION OF PROCEDURE: The patient brought to the operating room and anesthesia was obtained by the anesthesiologist. Both her lower extremities had been draped and prepped in a typical sterile manner. The right lower extremity was exsanguinated and the tourniquet was elevated.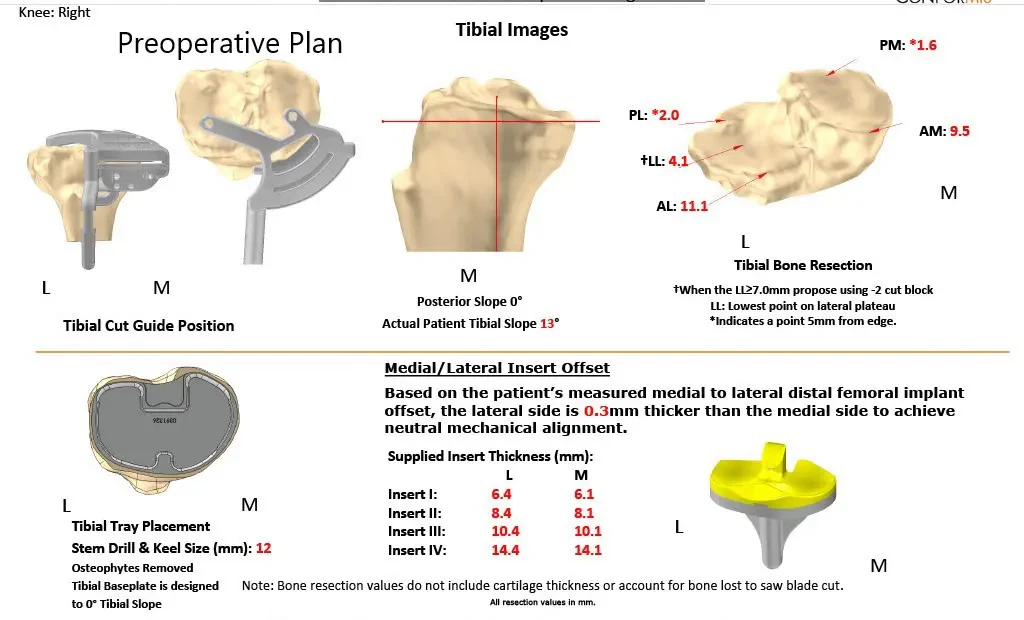
Complete Orthopedics patient-specific surgical plan for a customized bilateral knee replacement in a 78-year-old male.
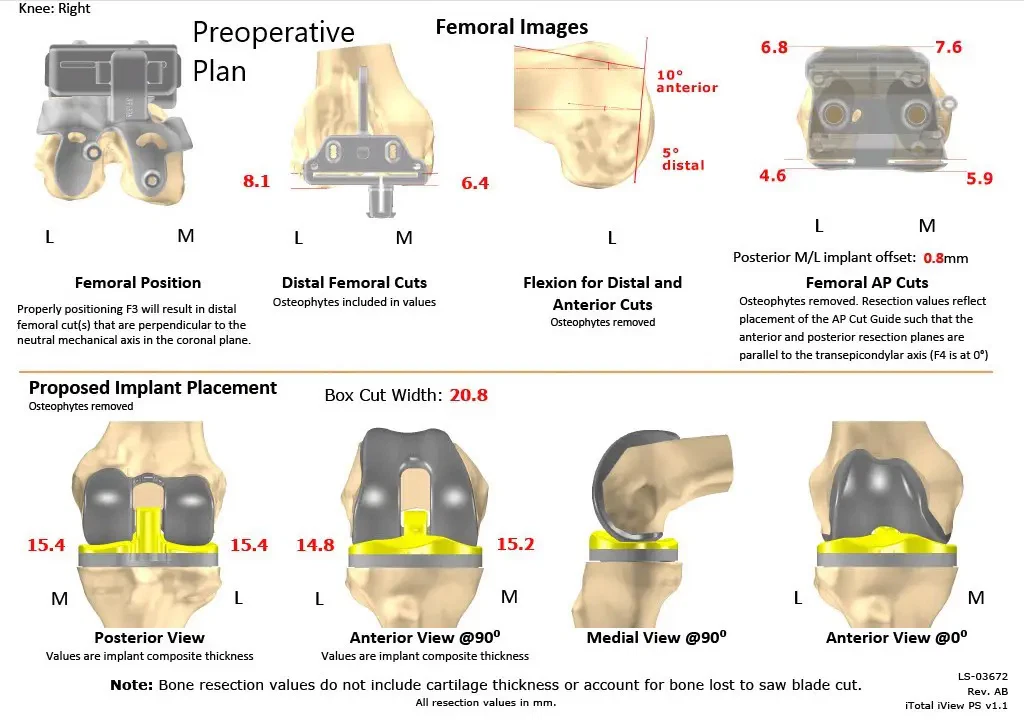
Complete Orthopedics patient-specific surgical plan for a customized bilateral knee replacement in a 78-year-old male (scan 2)
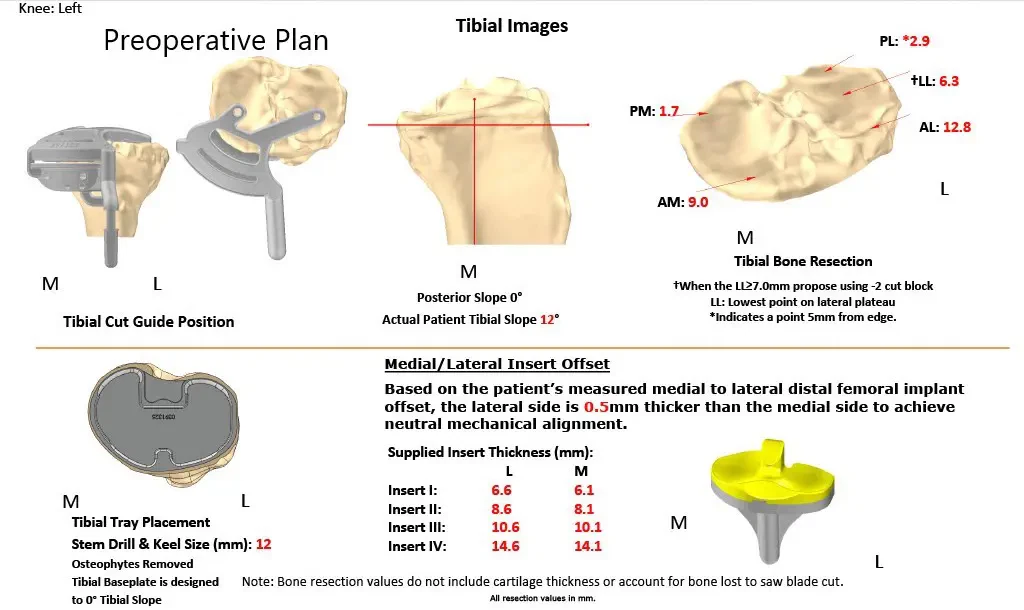
Complete Orthopedics patient-specific surgical plan for a customized bilateral knee replacement in a 78-year-old male (scan 3)
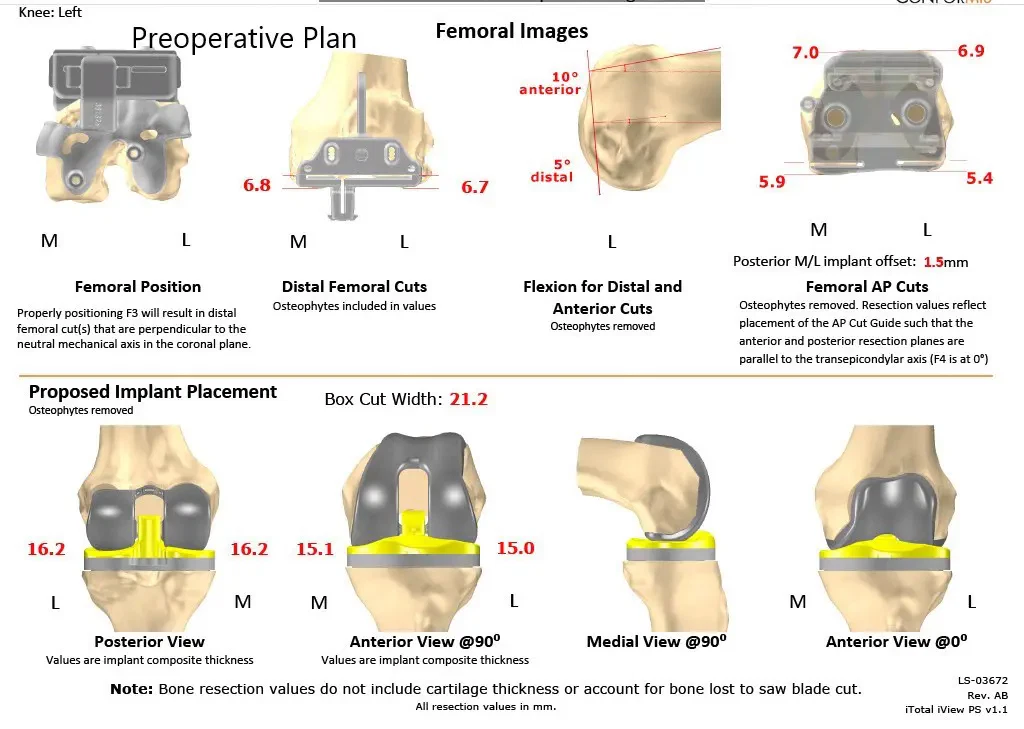
Complete Orthopedics patient-specific surgical plan for a customized bilateral knee replacement in a 78-year-old male (scan 4)
Skin and subcutaneous tissues were then incised. Medial parapatellar arthrotomy was then performed. The femur was then exposed. The cutting guides were then placed into position and the distal and the chamfer cut, as well as the notch cuts, were then performed. Attention was then turned to the tibia and the tibial dissection was then performed.
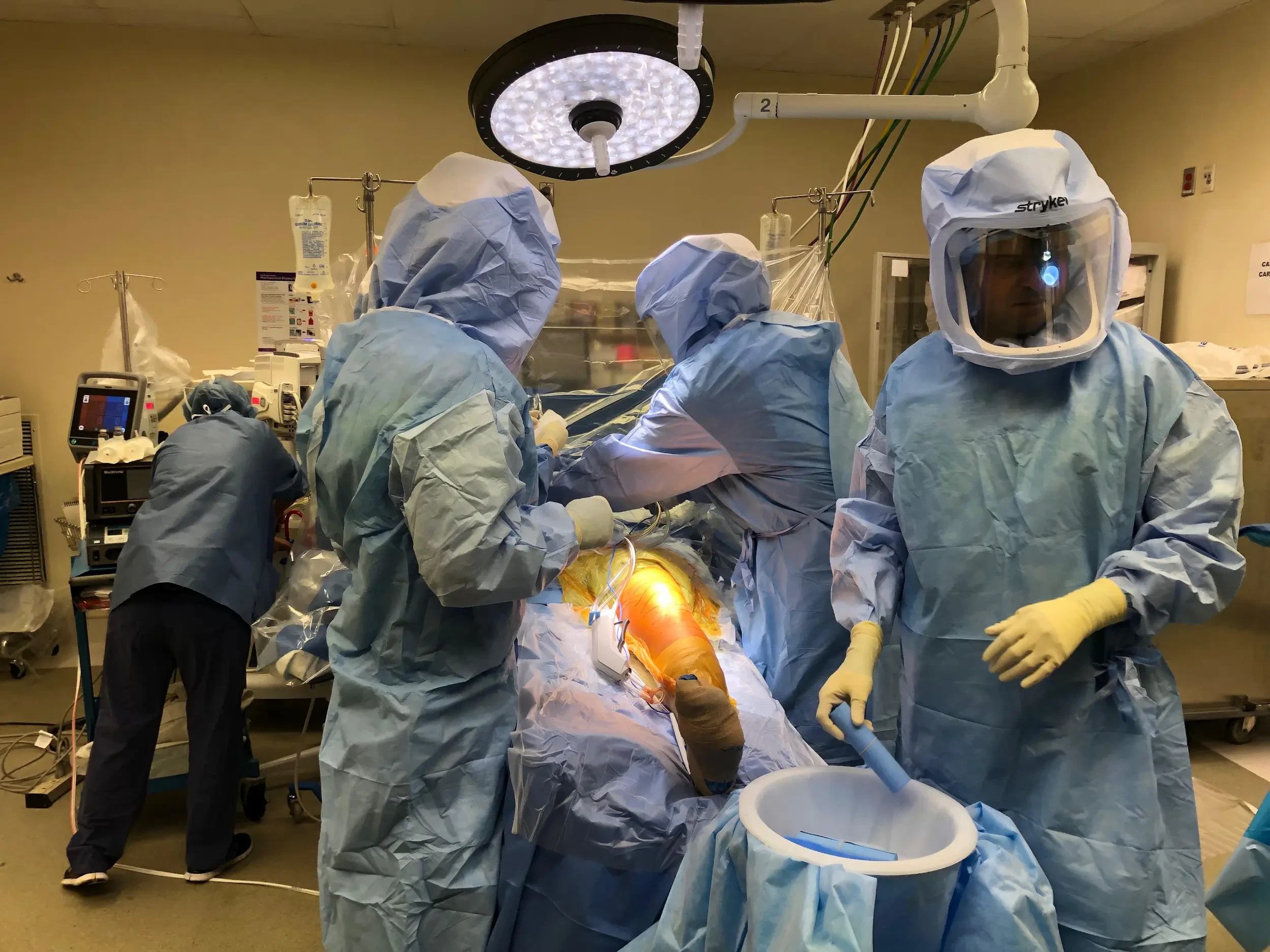
The dissections were then checked with alignment guides. There was significant patellar deformity and the patella was then resected and drill holes were then made in the patella. The trial patella was then placed into position. Lamina spreaders were used medially and laterally and then the posterior osteophytes were then removed.
The remainder of the meniscus and the cruciate were then removed. Gap balancing was performed and was found to be correct.
The trial femur was then placed into position followed by the trial tibia and the trial poly was then placed into position. The knee was then ranged through a full range of motion. Patellar tracking was excellent. The stability was excellent.
All trial components were then removed. Thorough lavage was given. The injection was given. After the bone guide, the femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed.
The poly was then placed into position. The knee was then reduced and held in full extension with a bump under the ankle. The patella was then cemented into position and excess cement was removed after the cement hardened. The medial parapatellar arthrotomy was then closed and the closure was done in layers. The skin was closed with staples. Tourniquet was let down and then attention was turned towards the left knee joint.
The left knee was replaced in a similar manner using customized implants. After the procedure, the patient was then transferred to the postoperative care unit in stable condition.
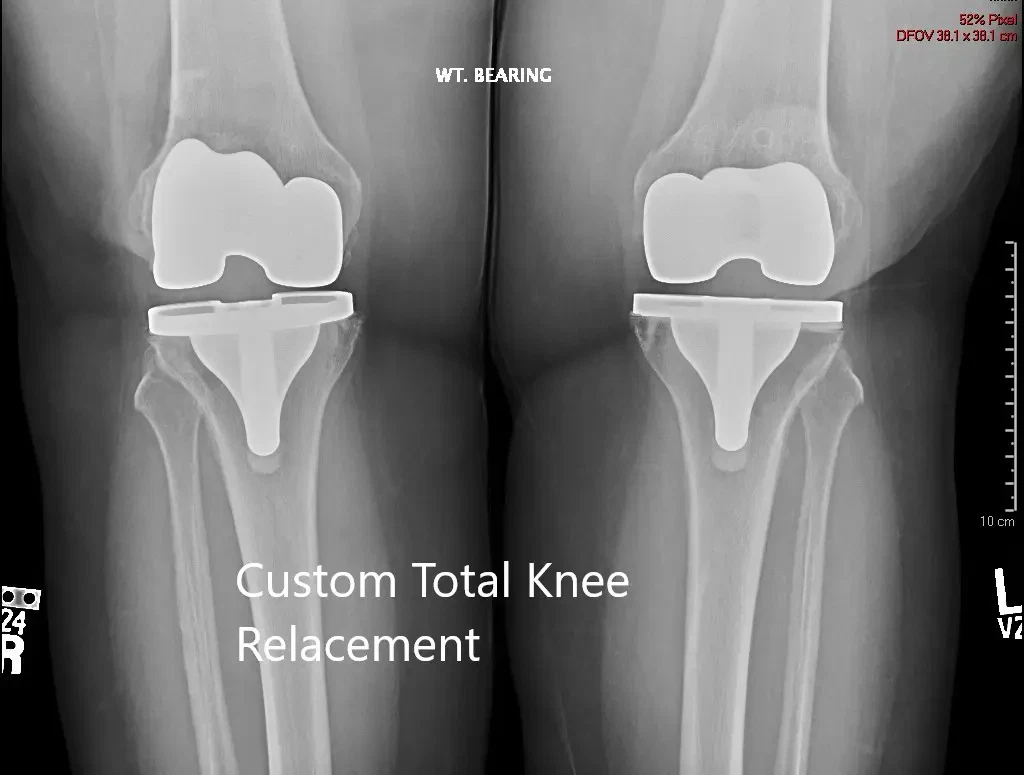
Postoperative X-ray showing the AP view of both knees
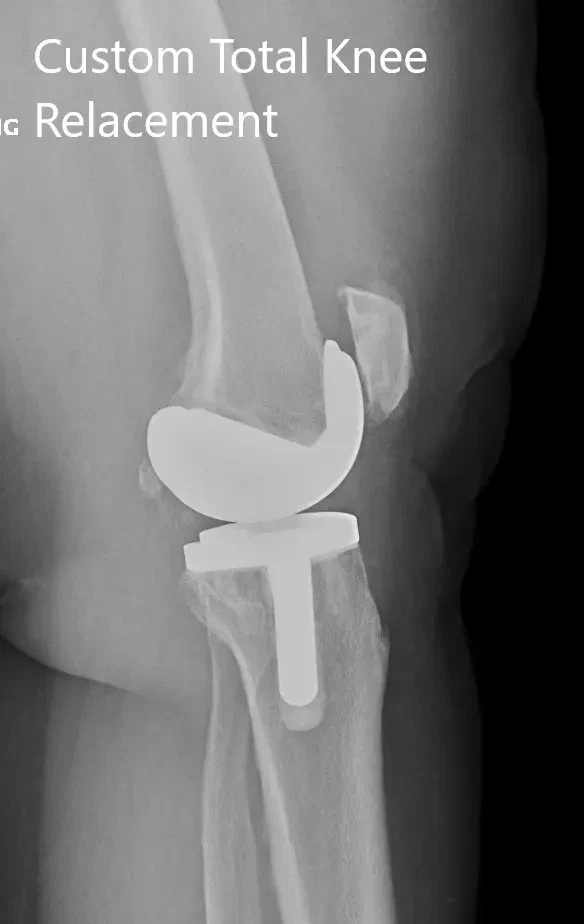
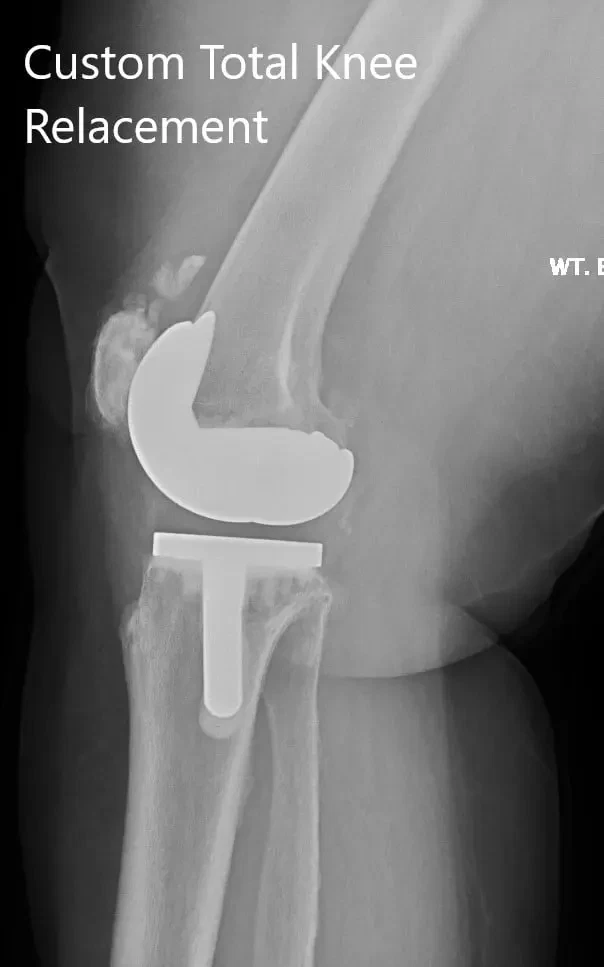
Postoperative X-ray showing the lateral views of both knees.
The patient had an excellent recovery post-op and weight-bearing was allowed the same day of surgery with support. The patient was started on deep vein thrombosis prophylaxis and pain medications. He was advised to undergo physical therapy for early rehabilitation.
The surgical wound was clean, dry and intact. The sutures were removed uneventfully. He was able to drive his car, move about the house, climb stairs and bend without pain. He demonstrated a full range of motion of both knees. The patient was extremely happy with the outcome and stated he was emotionally relieved from a stressful life full of pain and apprehension.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


