A 40-year-old male patient presented to our office with complaints of worsening left hip pain. The pain began insidiously 4 years ago and gradually progressed. The pain was associated with a limp and stiffness of the left hip. The patient was currently walking using a cane as an assistive device.
The patient was a former alcoholic and was admitted to a rehabilitation facility three times. He was a heavy drinker consuming more or equal to a quarter of a bottle of whiskey every day for the past 20 years. He previously had a history of gastric bleeding and hospitalization for deranged electrolytes.
He had successfully quit alcohol after his last visit to the rehabilitation center. He was currently living with his mother. He was working as a software developer and he was unable to travel to his work secondary to hip pain and stiffness.
The pain was located in the left groin which would radiate down his left knee on the inner side. The pain was described as a dull ache in character. The intensity was reported as moderate to severe (8/10).
He was unable to do his daily activities. His walking tolerance was reduced to less than two blocks secondary to pain. He found it difficult to stand for prolonged periods of time. The pain was worse on bending, getting up from a chair, squatting, sitting cross-legged. Recently he found it difficult to even tie his shoelaces.
The limp occurred in association with the pain. He felt he lurched towards the left side. The limp exaggerated on the increased intensity of pain. He had been using a cane for the past year now.
He denied any history of falls or trauma. He had no history of any surgeries around the hip or any history of blood disorders. He previously consulted another physician who prescribed him bisphosphonates and analgesics. He was currently taking omeprazole, alendronate, and liver supplements.
On physical examination, his gait was observed to be antalgic with a reduced stance phase and a lurch on the left side. Both the shoulders, iliac spines, patella, and malleolus were at the same level. There was no exaggeration of the lumbar lordosis. There was an absence of any functional or structural scoliosis.
There was no scar, sinus or any redness on the left hip. Tenderness was present on the left anterior hip joint line. There was no fullness in the Scarpa’s triangle. On digital palpation, both the greater trochanters were at the same level. There was no broadening or thickening of the greater trochanter.
The range of motion of the left hip was reduced in internal rotation and abduction. There were no fixed deformities but the motion was reduced secondary to pain. The flexion was present from 0 degrees to 130 degrees, extension from 0 to 5 degrees, abduction from 0 degrees to 40 degrees, abduction from 0 to 10 degrees. The rotational movements were markedly painful.
The examination of the contralateral hip was normal. The examination of the lower back, the bilateral knees and ankles were normal. There was no evidence of distal neurological deficit. The bilateral lower extremity pulses were palpable and comparable.
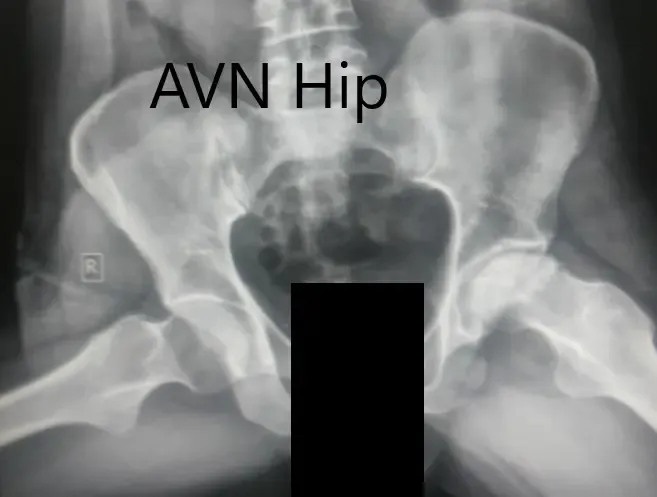
An imaging study in the form of an X-ray was obtained showed marked joint space obliteration. The normal spherical contour of the head of the femur was lost. There were marked degenerative changes suggesting arthritis. Avascular necrosis of the left hip joint was suspected with a positive history of alcohol abuse.

An MRI was obtained for diagnostic confirmation and staging of the disease. The left femoral head was collapsed with irregular contour and showed areas of altered signal intensity with a line of demarcation. Hypointense areas both on T1WI & T2WI seen in head suggestive of sclerosis. Surrounding marrow edema was seen
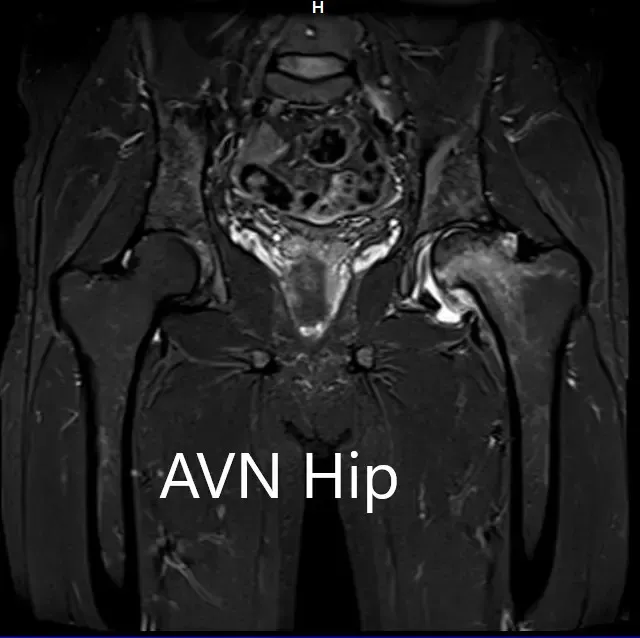
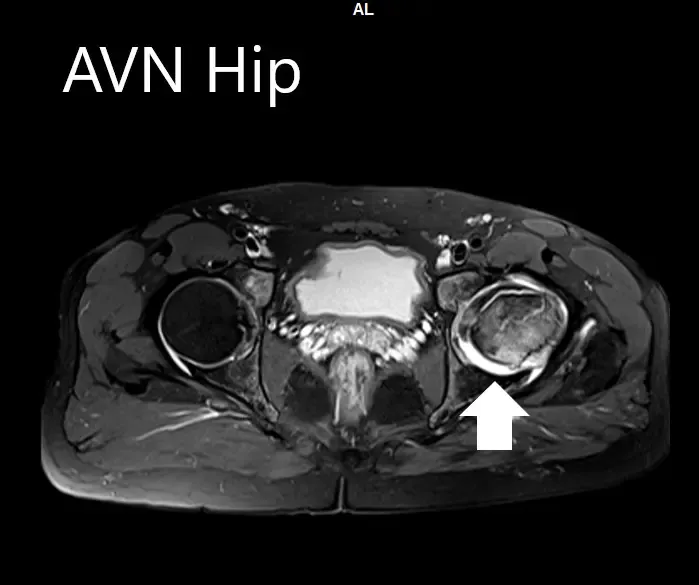
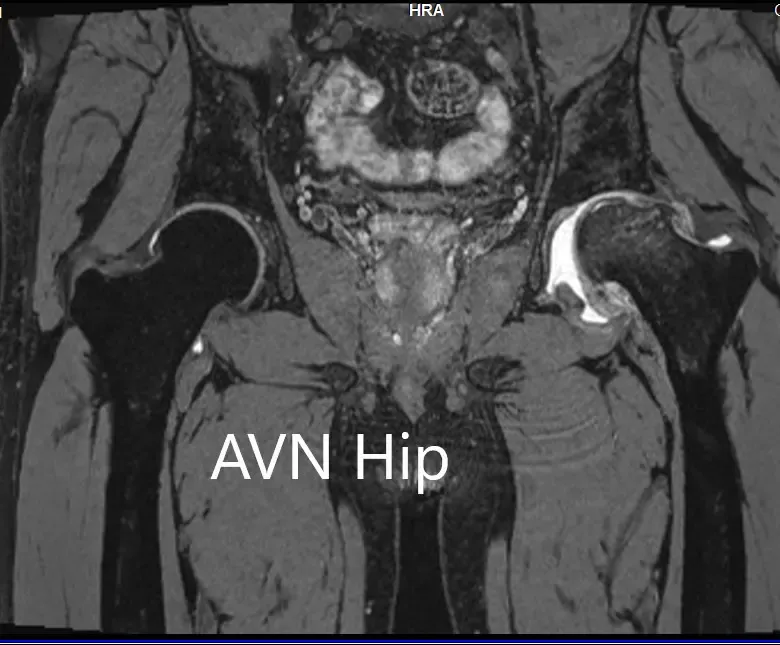
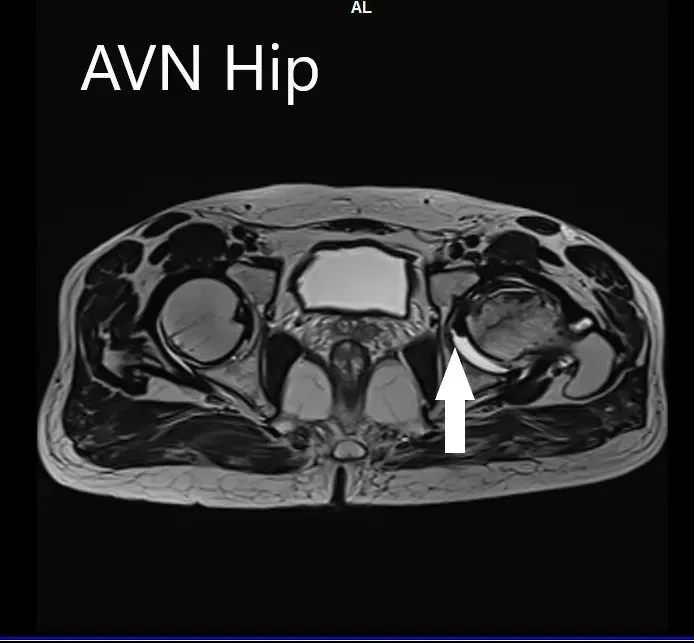
The left hip had advanced avascular necrosis with a collapse. The right hip was uninvolved presently. He was educated about the worsening collapse of the hip joint leading to his symptoms. Although the patient was young, he was advised a total hip replacement surgery in view of the collapse of the head of the femur with arthritis.
The risks, benefits, and alternatives were discussed at length with the patient. He was made aware of possible revision in the future. He agreed to go ahead with the surgery. A left total hip replacement was performed. He had an expedited recovery post-op.
The patient was ambulatory with support the next day. He was compliant with his hip precautions and physical therapy. The pain was managed with pain medications. The patient returned 8 weeks post-op and reported zero pain. He was able to walk without support and demonstrated an excellent range of motion of the left hip. He follows up regularly for surveillance of avascular necrosis in the right hip.


