A 65-year-old female presented to our office with complaints of bilateral hip pain for the past 5 years. The patient was working as a utility worker at a nursing home. She stated she had been working at the nursing home for the past 35 years. She also complained of bilateral knee pain and right elbow pain.
The patient reported as a utility worker her work involved lifting, loading of food carts, bending, pushing, pulling and returning the food trucks to the kitchen. Additionally, she was mopping, sweeping the food truck room, preparing and delivering food trays as needed. She had to lift kitchen garbage and empty it into the dumpster.
She stated during her time at work she was standing for prolonged periods of time. She had to go up and down the stairs frequently. She had been working 5 days a week for about 8 hours every day. She felt her hip pain as a result of her chronic repetitive work over the years.
She denied any trauma to the hip and had tried physical therapy with pain medications. She felt the relief from conservative management options didn’t last for long. Recently, the pain and stiffness had been worsening. She found it increasingly difficult to walk, get up sitting position, squat and bend.
She was a nonsmoker and nondrinker. Her medical history included hypertension and dyslipidemia, both well controlled with hydrochlorothiazide and atorvastatin. She denied any long term steroid abuse. She was ambulatory with the help of a cane. She denied any known drug allergies.
The patient felt frustrated by the disability brought on by pain and stiffness in the hips. She located the pain in the bilateral groin area (right greater than left). The pain was moderate in intensity and dull aching in character. She denied any radiating pain from the lower back.
She reported the inability to perform daily activities such as climbing up and down the stairs, putting on socks, and walking. On her physical examination, there was no leg length discrepancy or exaggeration of lumbar lordosis. There was no evidence of functional or structural scoliosis.
The skin overlying the bilateral hips was normal. There were no scar, sinuses or any swelling in the bilateral groin. There was no lymphadenopathy and her gait was steady. Bilateral knees had signs of mild arthritis with normal bilateral ankles. There was no distal neurological deficit.
There were no fixed deformities but the reduction of internal rotation of the bilateral hips. Abduction was painful and the power of bilateral hip abductors was 4+ with normal bulk of muscles. Light touch checked in all sensory dermatomes was normal. Bilateral lower extremity pulses were good volume and palpable.
There was bilateral anterior Hip joint line tenderness. The bilateral digital Bryant triangle was comparable suggesting no suprapelvic shortening or lengthening. Imaging studies revealed severe bilateral hip arthritis.
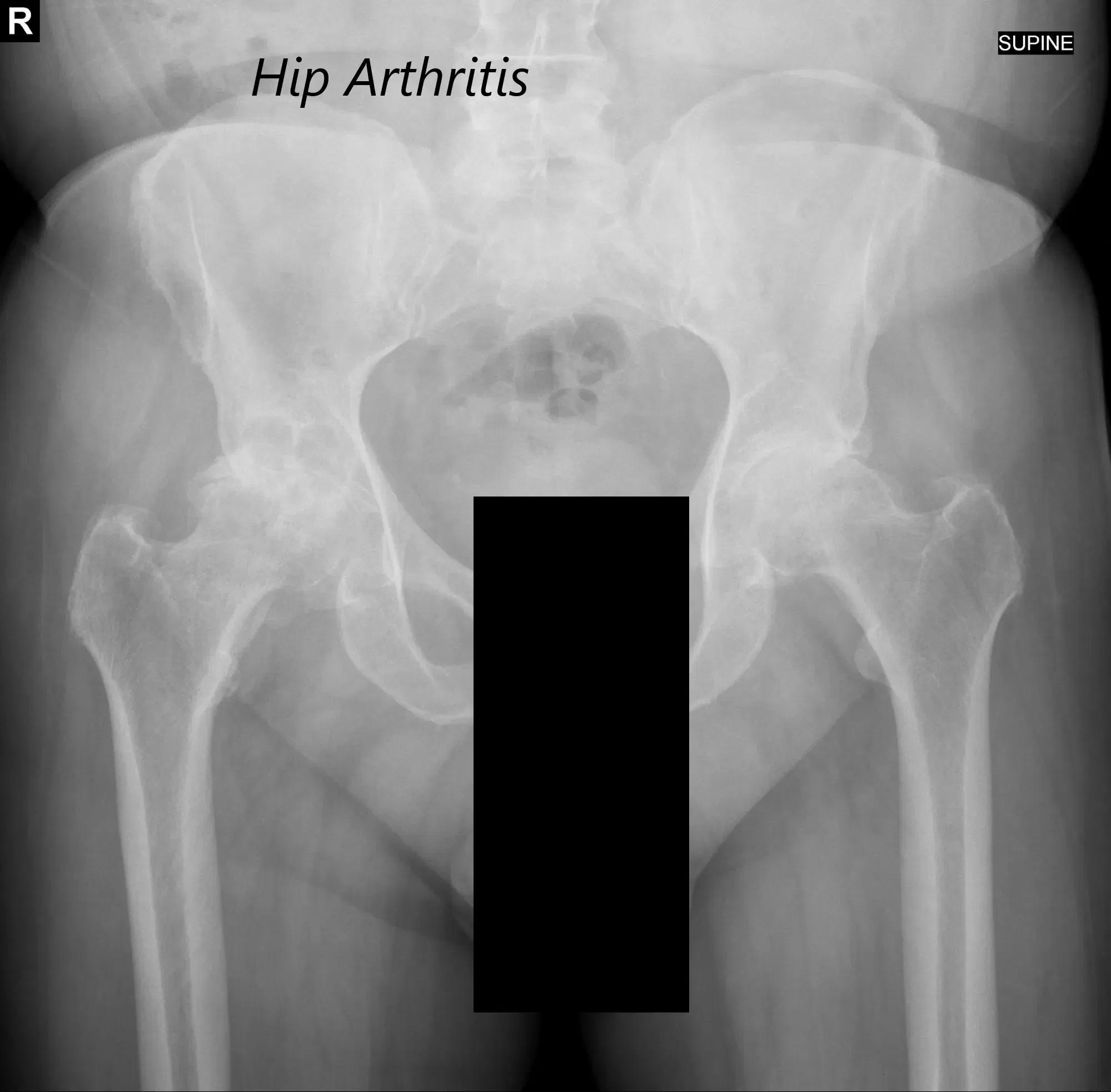
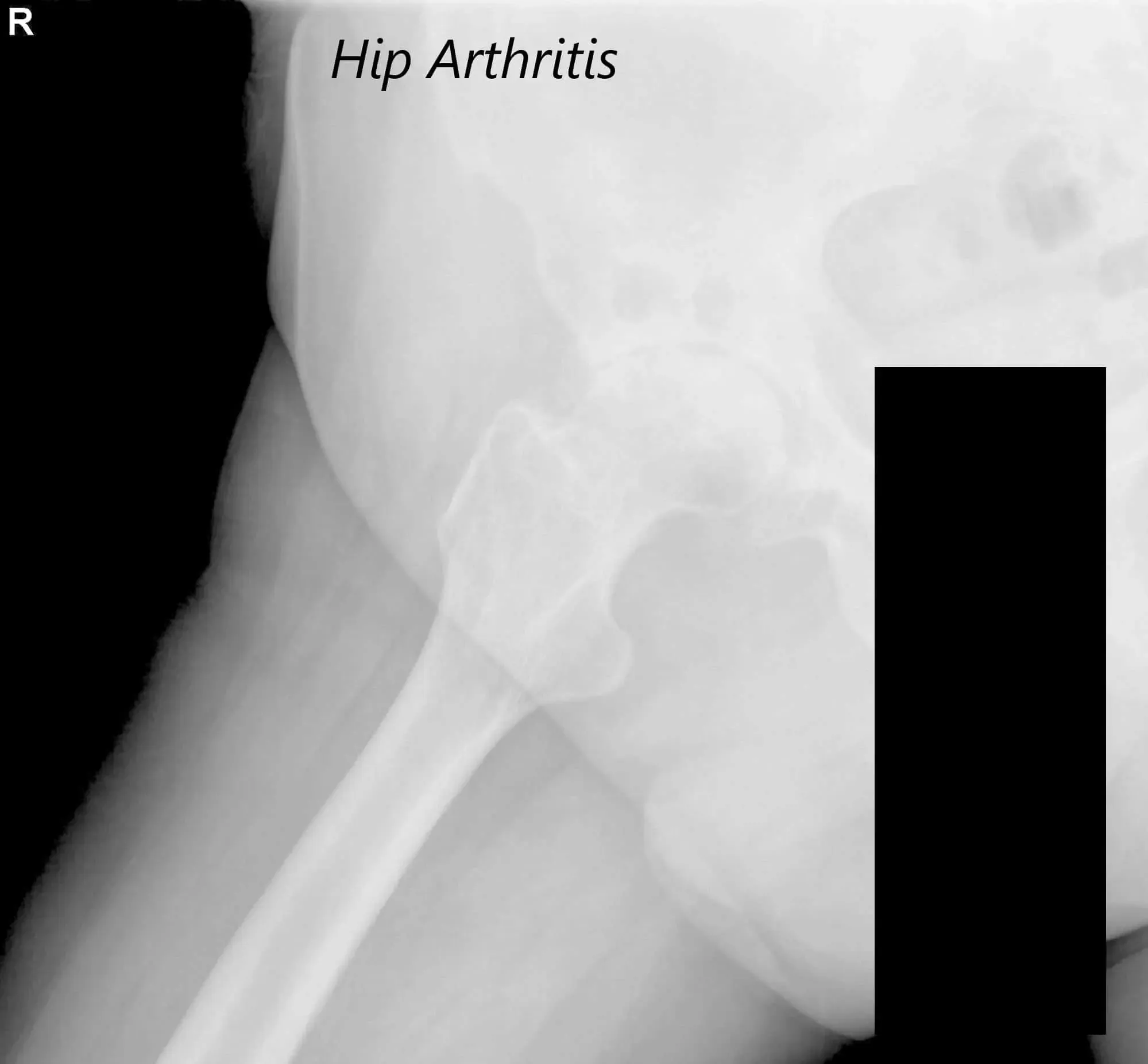
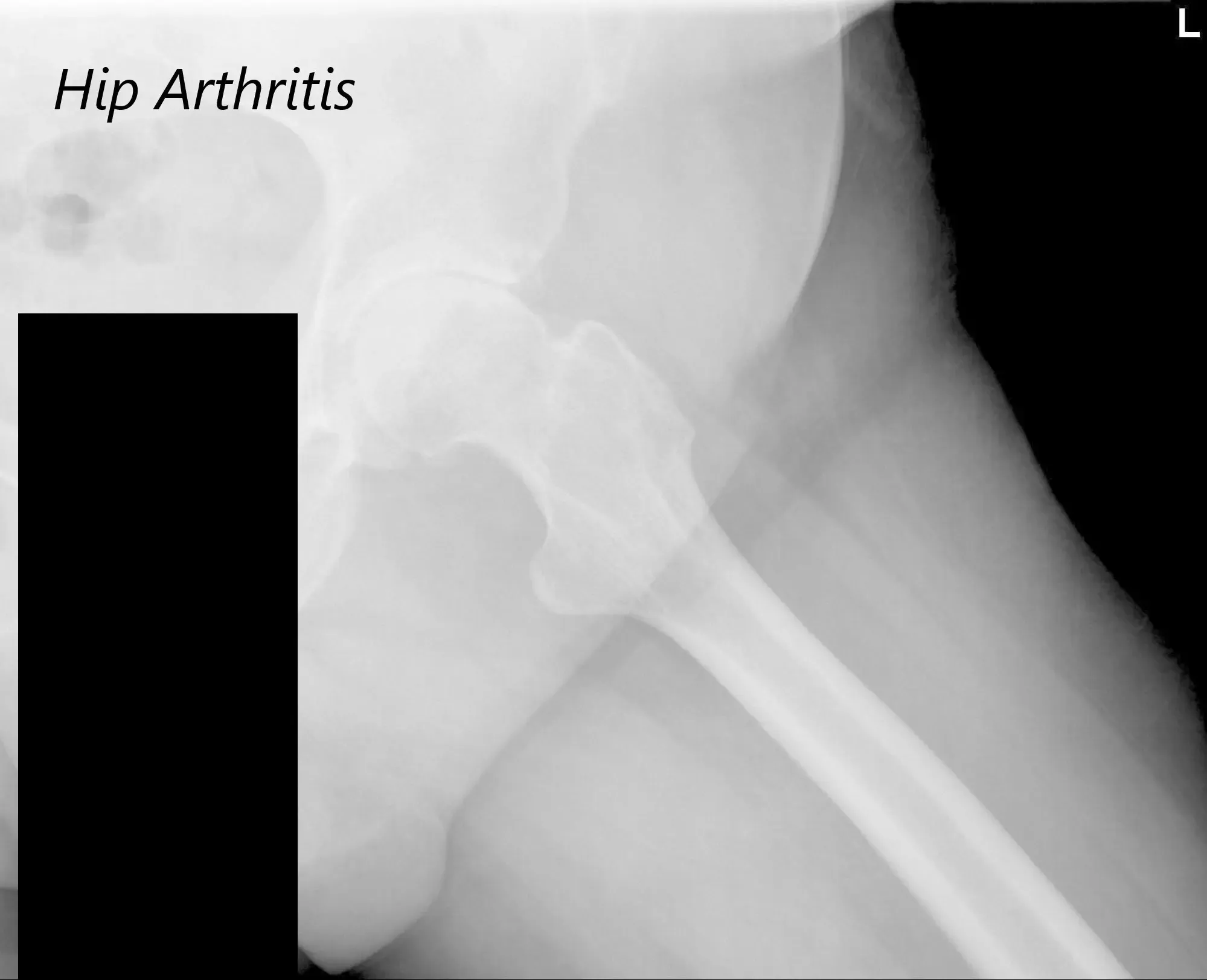
AP view of the Pelvis X ray showing both hip joints with frog leg lateral views of the right and left hip joints suggesting severe bilateral osteoarthritis of the hip joints.
After careful consideration of her comorbidities and needs, she was deemed as a candidate for bilateral total hip replacement surgery. She was advised about the increased risk of bilateral surgery. Other risks, benefits, complications, and alternatives were all discussed at length with the patient and her family. She agreed to go ahead with bilateral total hip replacement.
OPERATION: Bilateral total hip arthroplasty.
IMPLANTS USED: Ceramic femoral head 36 mm + 5 bilaterally with a 50-mm Tritanium hemispherical cluster hole shell with a screw (6.5 mm x 25 mm) with 127-degree size 3 femur with an 0-degree 36 mm polyethylene.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient and her husband understand the increased risk of bilateral total hip arthroplasty.
Because the right hip had more pain, it was decided to do the right total hip arthroplasty initially. The patient was then placed in a lateral decubitus position and the right hip was then draped and prepped in the usual sterile manner.
A curved incision centered over the greater trochanter was used for the arthrotomy. Skin and subcutaneous tissues were incised. The fascia was then divided.
The hip was then placed in internal rotation, the posterior soft tissue structures were then taken down, and tagged for future repair. The neck resection was then performed. The head was then removed. The acetabulum was exposed. The remainder of the labrum was then divided.
Acetabulum sequentially reamed and the final shell was then placed into position in the correct abduction and anteversion. The screw was then placed for additional fixation. The poly was then placed over the cup.
Attention was then turned towards the femur. The femur was then sequentially broached. The final broach was left into position, and the trunnion and the head were then placed over the broach. The lesser trochanter center distance was found to be correct.
The hip was then relocated and was trialed through the physiological range of motion. The hip was found stable in all physiological range of motion.
The hip was then dislocated. The trial components were then removed. The final components were then placed into position. The injection was then given, thorough lavage was given. Evicel was placed and excellent hemostasis was achieved.
The fascia and the gluteus muscle were then closed. Fascia lata was then closed. Subcutaneous tissues were closed. Subcuticular tissues were closed. The skin was then closed using staples. A sterile dressing was then applied over the wound.
The patient was stable and therefore it was decided to proceed with the left total hip arthroplasty. The left total hip arthroplasty was done in a similar manner.
After the procedure, x-rays were obtained and were then saved to the PACS system. The alignment and stability on the x-ray was found to be acceptable. The patient was transferred to the postoperative care unit in stable condition.
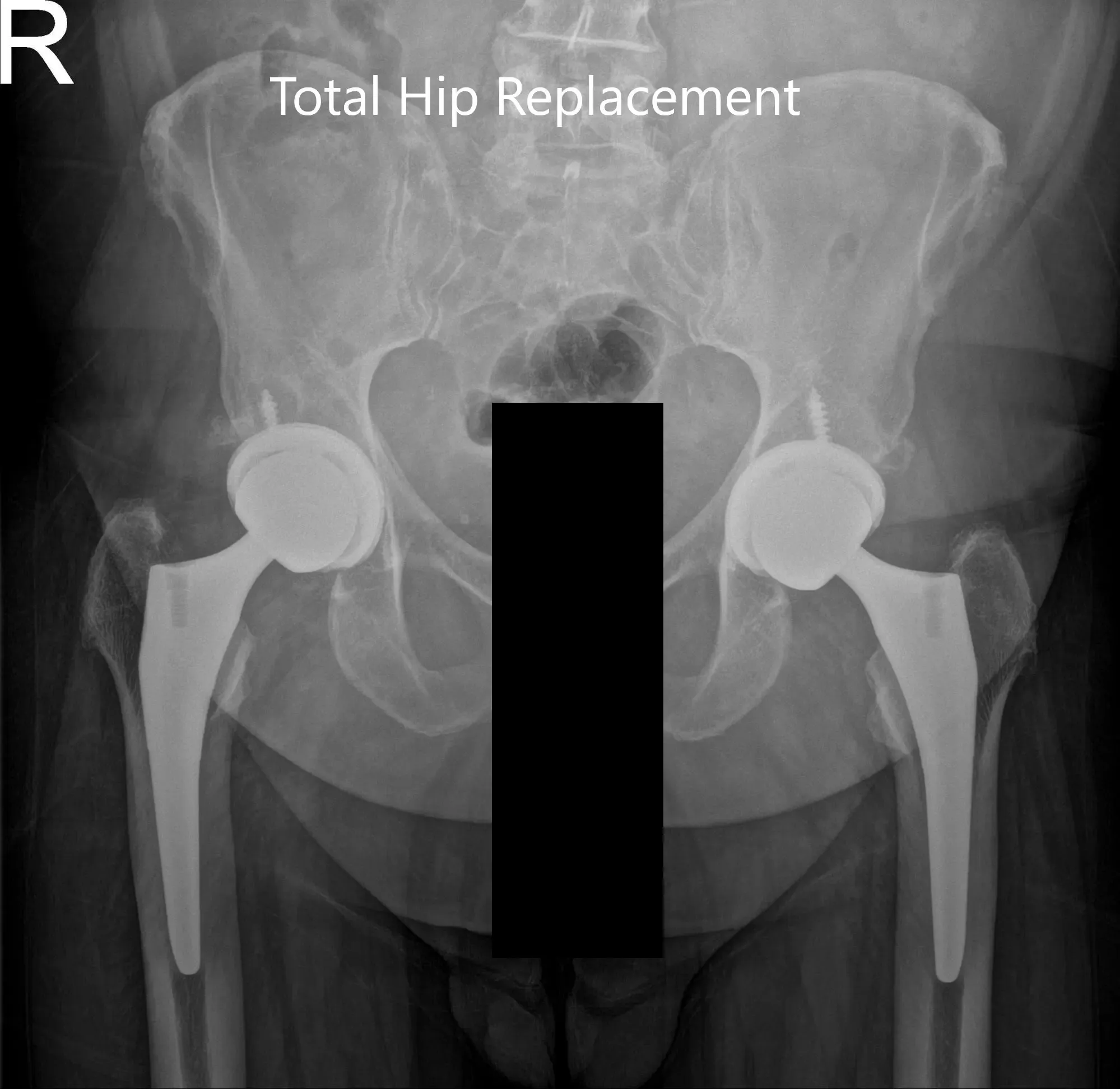
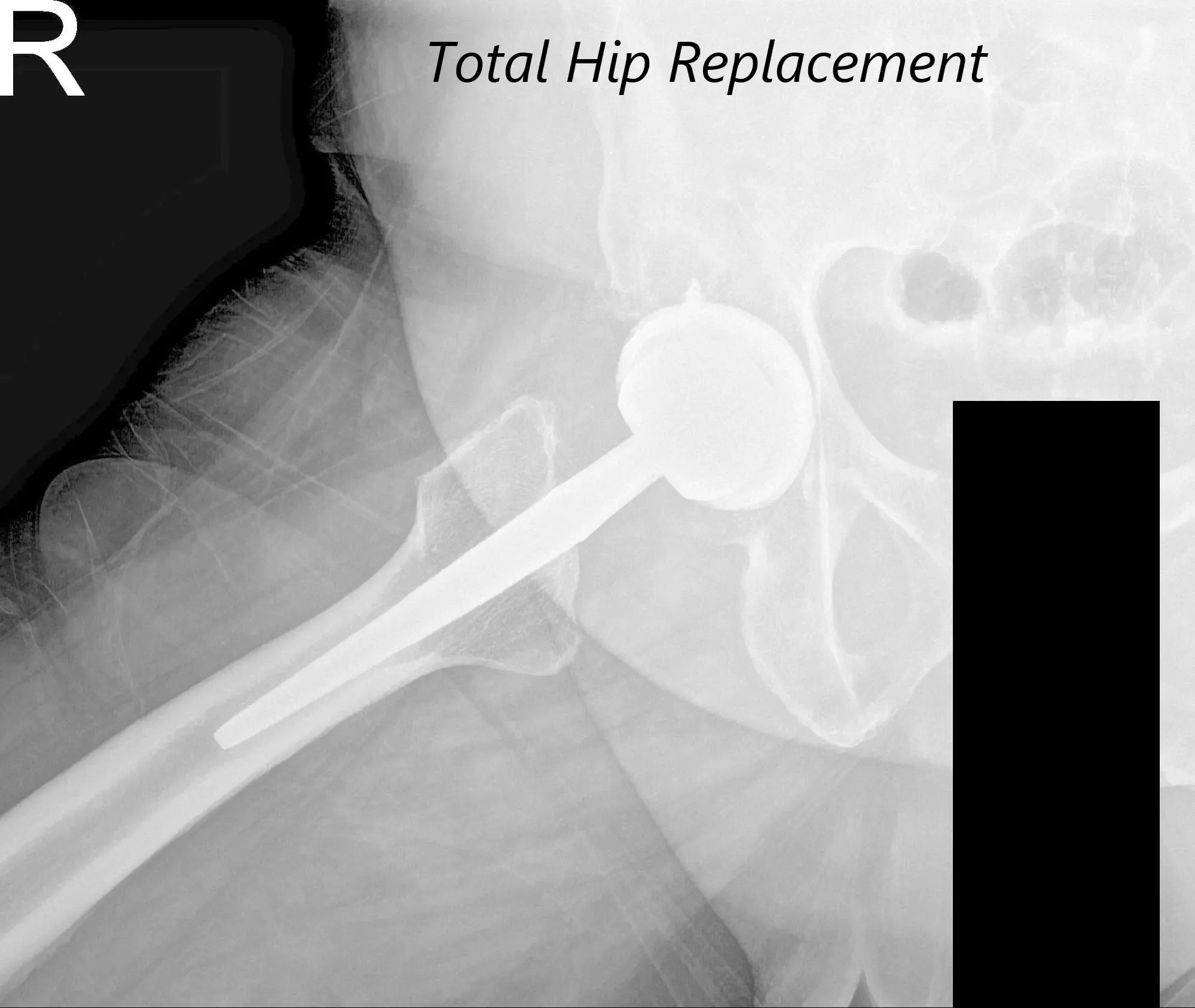
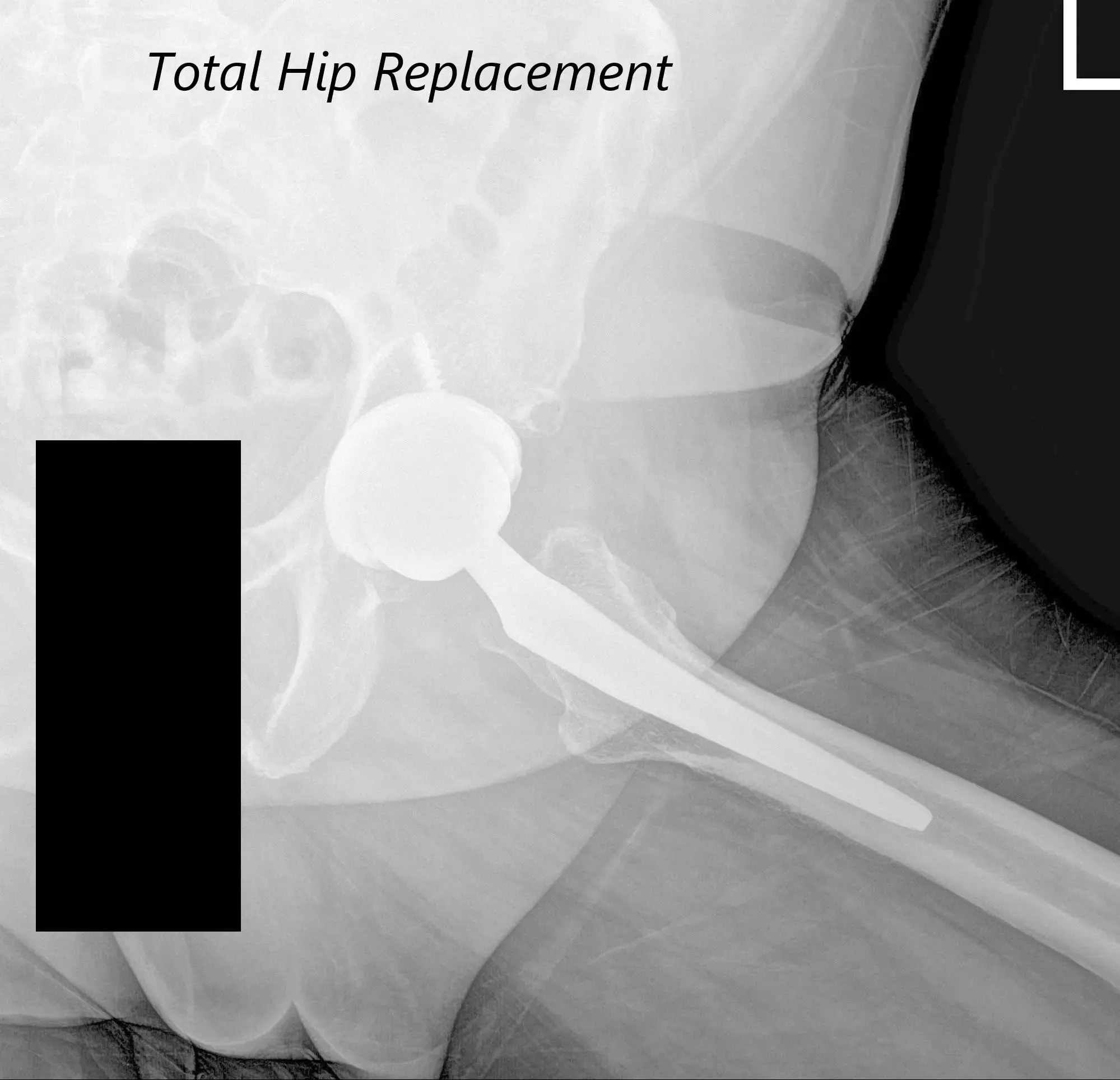
Postoperative AP view of the Pelvis X-ray showing both hip joints with frog-leg lateral views of the right and left hip joints.
The patient was started on aspirin 325mg BID for deep vein thrombosis prophylaxis. The pain was managed with medications (oxycodone + acetaminophen). Postoperative her vitals were stable and she had no episodes of fever. Sterile dressings were changed and the wound was clean, dry and intact.
A home exercise program along with gait training and fall prevention training was started. Chest breathing exercises and physical therapy were continued. Three months post-op she demonstrated excellent recovery and was ambulatory without any aid.
She reported pain free range of motion of both hips. The patient stated the results exceeded all her expectations. She follows up as needed.


