A 63-year-old patient presented with complaints of right knee pain. He was involved in a worker’s compensation accident seven years ago. He was employed by the Town Police as a police officer. On the date of the accident, he was doing a training drill with another police officer. Unfortunately, his foot got stuck in between his feet causing his body to twist and his right knee to dislocate.
He had a knee cap dislocation. The patella was relocated on the way to the hospital. He had an Anterior Cruciate Ligament (ACL) repair in two years after by an outside physician. He started experiencing worsening pain and he was advised Partial knee replacement.
He underwent a partial right knee replacement in 3 years after by another physician. He never got a full extension and was never pain-free. He had an exacerbation a year ago while getting up from a chair at work. He heard a pop in her knee and went to a hospital where he was evaluated and x-rays were performed.
He presented to us with the CD of the images. He described the pain as a sharp pain located anteriorly. The pain was especially worse on negotiating stairs. He stated she was only able to negotiate stairs one step at a time and with the help of a banister. The intensity of the pain was described as severe.
He had a previous medical history for gallbladder removal and denied any allergies. He did take a powder called Cholestyramine daily for hyperlipidemia. He was currently not working and used a cane as an assistive device.
On physical examination, there was pain throughout the arc of motion. The range of motion was decreased secondary to pain. The right knee range of motion was 10 degrees to 90 degrees. There was patellofemoral tenderness and medial joint line tenderness. Further, examination revealed mild swelling of the knee joint.
There was no laxity or instability in the sagittal and axial planes. The varus and valgus stress tests were done at 0 degrees, 30 degrees and 60 degrees were negative. The patellar tendon and the quadriceps tendon were intact with no evidence of disruption. The skin overlying the right knee was normal with a well-healed incision. There was no rise in local temperature.
The examination of the left knee, bilateral hips and ankles were normal. There was no distal neurological deficit. The power and tone of both lower extremities were normal. The lower extremity deep tendon reflexes were intact and comparable. The bilateral lower extremity pulses were palpable and comparable.
He was advised a right knee aspiration for gram staining, culture and sensitivity and biochemistry. He was also advised basic blood investigations in the form of Hb, TLC, DLC, ESR, CRP quantitative and qualitative. He agreed for the investigations.
The results of his investigations were within normal limits. There was no evidence of infection of the right knee. Imaging revealed failure of the partial knee replacement. He was advised a revision total knee replacement in view of advanced osteoarthritis. He agreed with the plan.
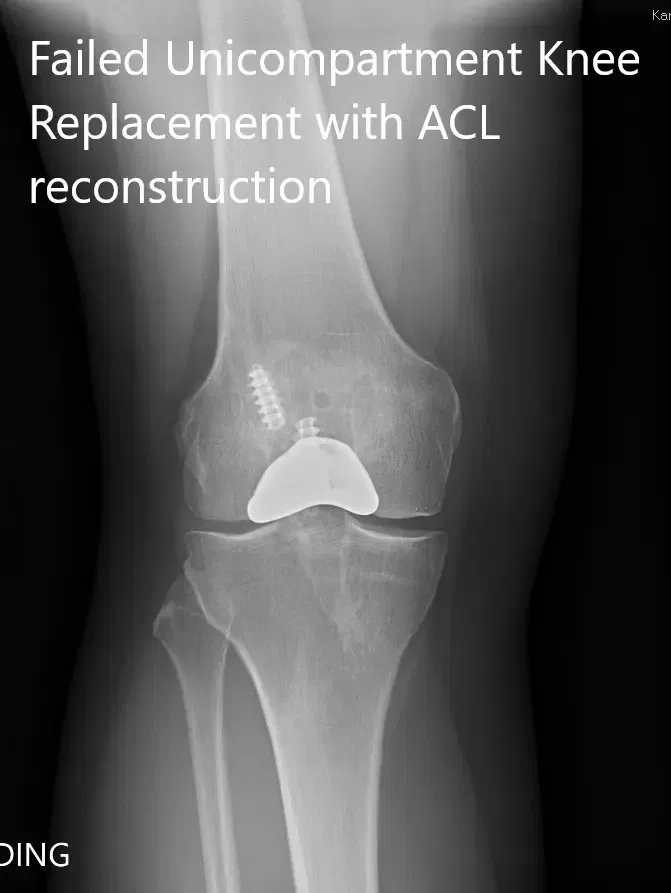
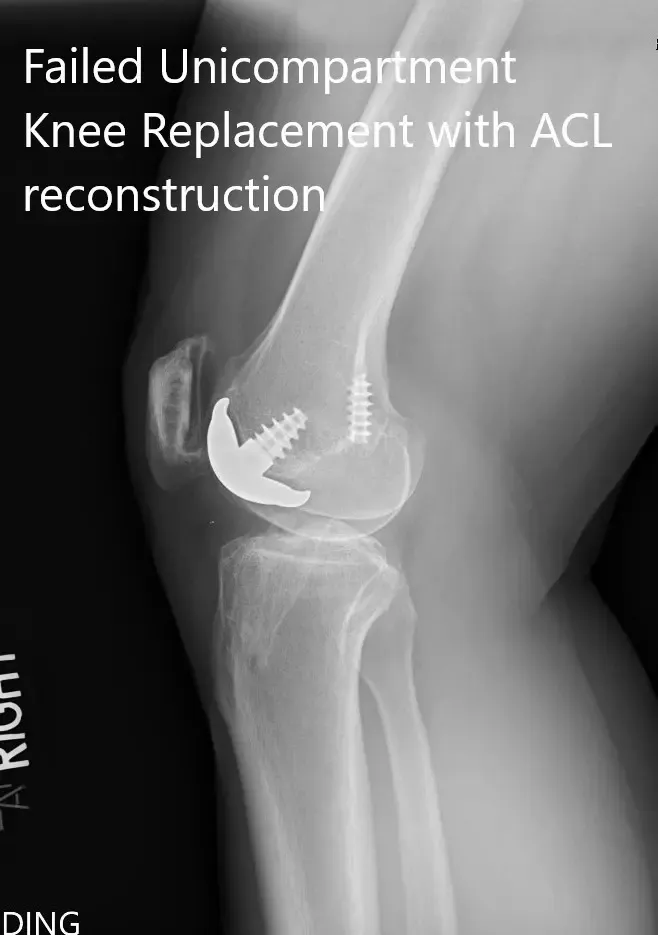
Preoperative x-ray showing the anteroposterior and lateral views of the right knee
PREOPERATIVE DIAGNOSIS(ES): Failed Right knee unicondylar knee replacement.
OPERATION: Revision right total knee arthroplasty.
IMPLANTS USED: PS tibial bearing E1 antioxidant 10 mm polyethylene with Vanguard femur60 mm with tibial component 67 mm.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient, as well as the family, understands that he is at increased risk of surgical complications because of the nature of the revision.
The patient was definitively positioned and the earlier incision was marked after the patient was anesthetized. The right lower extremity was draped and prepped in the usual sterile manner. The earlier incision was used for the arthrotomy and was extended proximally and distally for dissection purposes and for identifying the anatomical planes.
Skins and subcutaneous tissues were incised. Medial parapatellar arthrotomy was then performed. The femur was then exposed. The patellofemoral replacement was found to be loose and was removed. The screw was well fixed in the bone and using osteotomes and screwdriver, the screw of the patellofemoral replacement was then removed.
The distal cutting guide was then placed into position. The distal cut was then performed. The femur was then sized. Anterior and posterior chamfer cuts were then performed. The screw from the initial surgery was then visualized and it was anticipated that it will interfere with insertion of the final prosthesis and screw was also removed using implant removal instruments.
Attention was then turned towards the tibia. The tibial resection was then performed. The tibial cut was then removed. The overall limb alignment was checked using an alignment guide. The tibia was then prepared. The knee was then kept in extension and in the collapsed state. The patella was reverted and the patellar stability was found to be good.
The tissue around the patella that could help interfere with the range of motion was resected. The patella on the lateral to the patellar prosthesis was resected using a saw to improve the patellar tracking. The patella did not need to be revised.
Attention was then turned towards the femur. The notch cut was then performed. The femur was placed into position. The tibia was placed into position. The poly was placed into position. The knee was reduced. The knee was trialed through a full range of motion and there was a full extension possible, the full flexion was possible intraoperatively. The patellar tracking was excellent
The injection was given into the knee joint for postoperative pain control. The bone was prepared. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. The poly was then placed into position.
The knee was then reduced and held in full extension with the bump under the ankle. After the cement hardened, the bump was removed and the knee was again trialed through a full range of motion. Medial parapatellar arthrotomy was closed with Vicryl and Stratafix.
Cutaneous tissues were then closed with O Vicryl. Subcutaneous tissues were closed with 2-0 Vicryl. The skin was closed using staples. Sterile dressing was then applied over the wound and the patient was then transferred to the postoperative care unit in a stable condition.
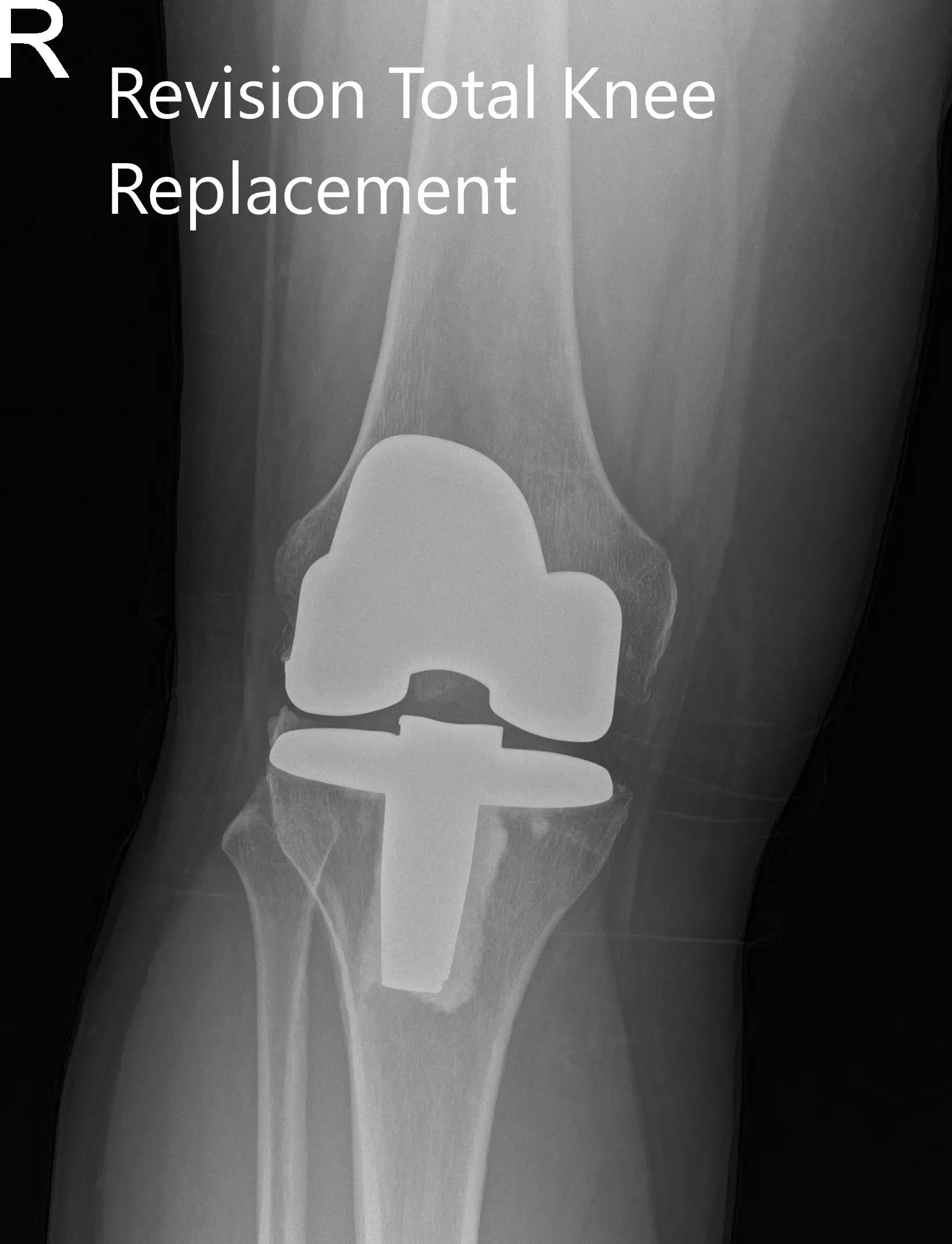
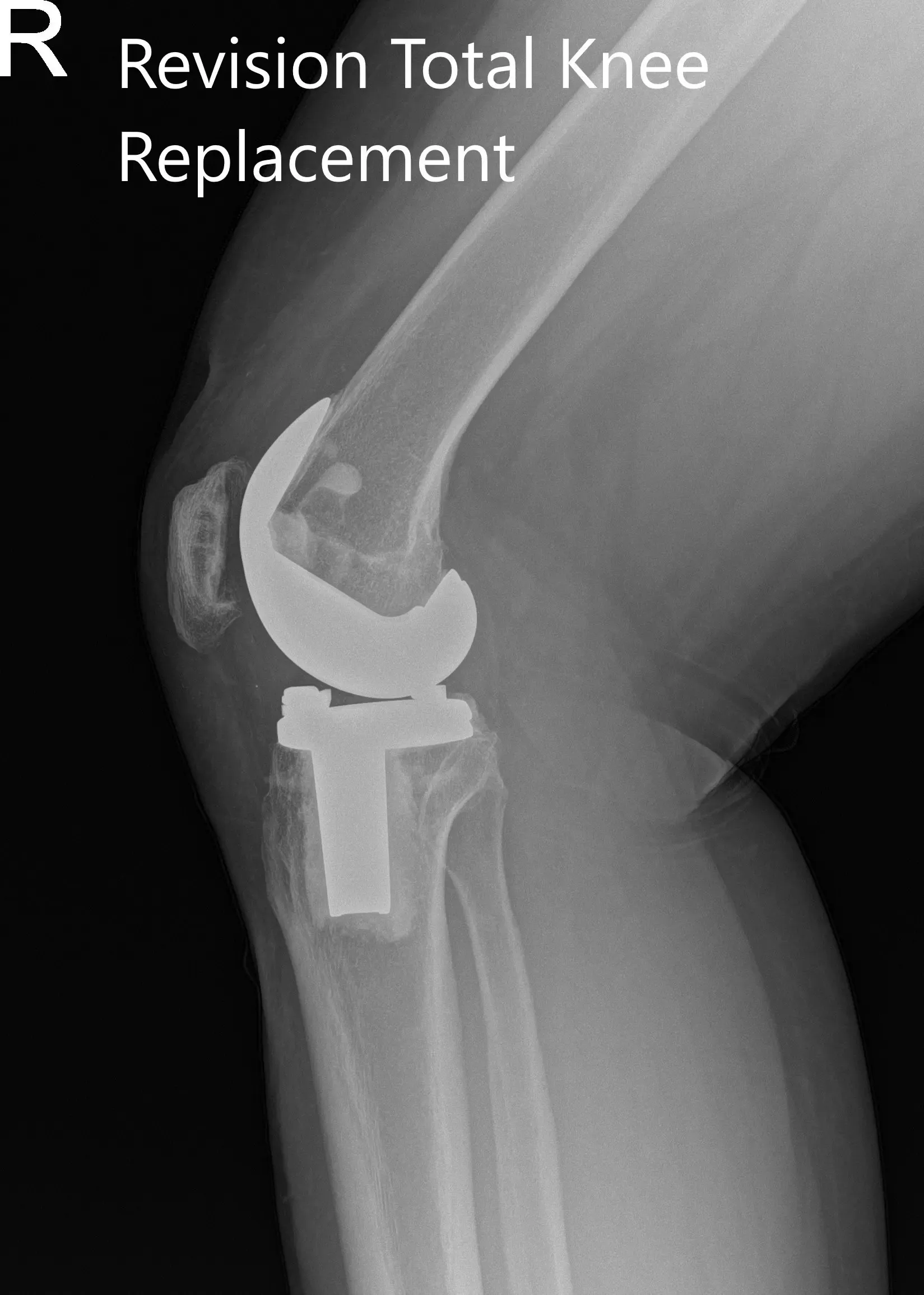
Postoperative x-ray showing the anteroposterior and lateral views of the right knee.
Post op his recovery was excellent. The pain was managed well with medications and he was ambulatory the same day of the surgery. He was given aspirin for deep vein thrombosis prophylaxis. He was advised physical therapy and home exercise program.
The sutures were removed uneventfully. The patient demonstrated a full range of motion with no pain at three months. The patient was able to walk without support and do her daily activities with ease. She was extremely happy with the outcome of the procedure.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


