A 66 year old male presents with chronic left knee pain which began in approximately 2013. Patient had a prior left knee arthroscopy procedure performed in 1983, which provided relief for about 20 years.
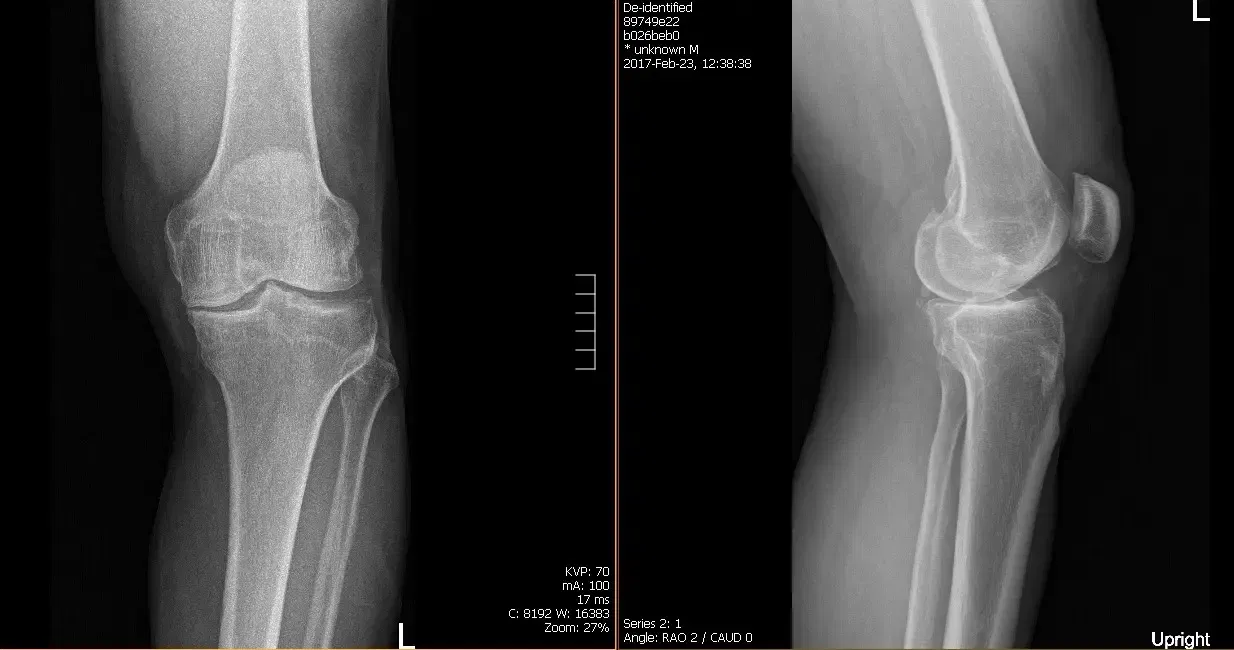
Patients’ pain started again about 1 year ago causing him to undergo non surgical options including physical therapy sessions and a sequence of cortisone injections which provided temporary relief.
Patient originally wanted to delay undergoing a TKA but the pain was significantly increased. The knee pain began to affect his ability to complete tasks at work and home, the patient stated complete discomfort at night when sleeping/resting, descending/ascending the stairs in the home and trouble getting in and out of bed. He was having increased difficulty lifting his own leg.
Patients had no other medical conditions noted and was overall an healthy individual. Patient was overall emotional and and cried during the initial evaluation and subsequent office visits prior to surgical intervention. Despite the patients anxiety and emotions, he remained very motivated.
He was a bank manager and his job required an extended amount of time sitting, standing, and walking. He was motivated to return to work. Currently he was working on an HEP provided by his physical therapist. He was able to describe his HEP in detail and performed exercises correctly showing compliance.
His HEP consisted of quadricep isometric, hamstring, and gluteal exercises, a seated knee flexion stretch and a supine knee hang. Patient was instructed to continue his HEP in addition to the new HEP program that would be given to him in outpatient PT. Presurgical films revealed there are moderate osteoarthritic degenerative changes.
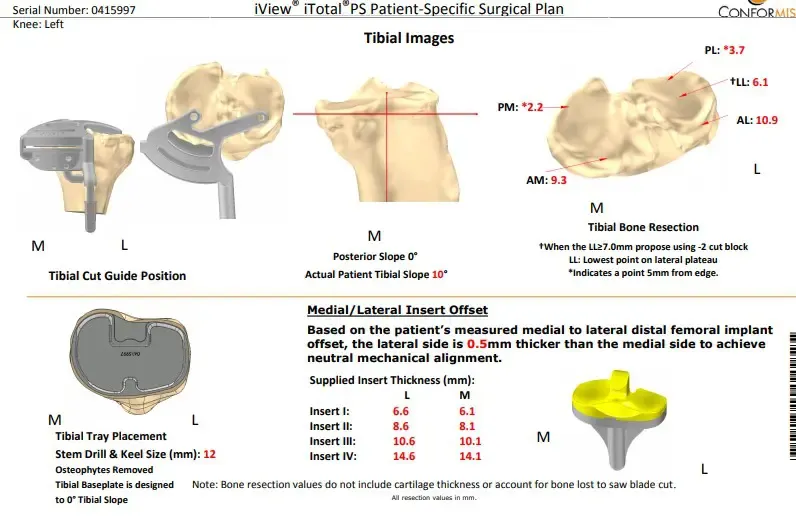
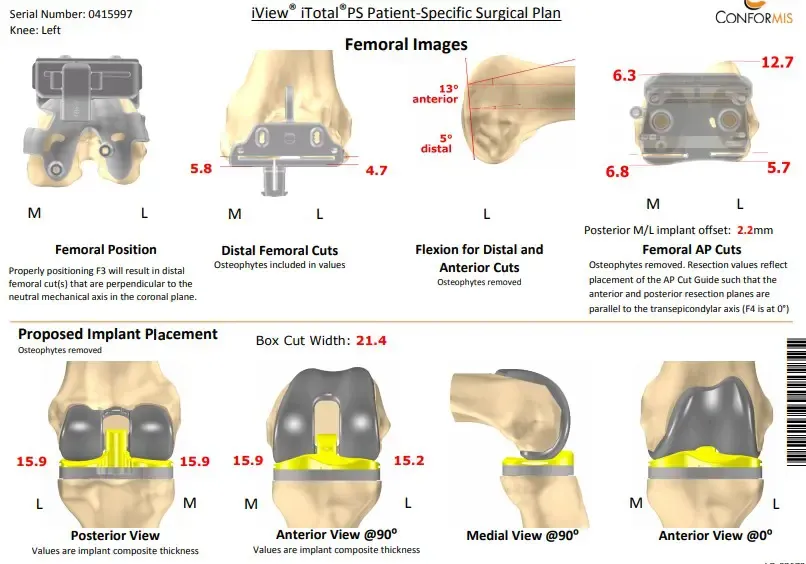
Patient underwent a Left Total Knee Arthroplasty using custom implant, During the procedure his surgeon noted advanced osteoarthritis was already present. A medial parapatellar approach was used, the tibial resection guide was then placed into position after exposure of the tibia, and the tibial resection was made and checked.
Attention was then turned towards the femur, distal cut was performed using a jig. The anterior-posterior chamfer cuts were then made using respective cutting guides. The notch cut was performed. Laminar spreaders were used medially and laterally, and the remainder of the meniscus and the cruciate were then divided.
Tibia was prepared along with a gap balancing turned to patella, allowing resection of the patella, trial patella was placed into position. Trial femur was placed into position followed by trial tibia and poly. The knee was trialled through a full ROM.
Patellar stability was excellent. The full range of knee was obtained thereafter. Trial components removed. Femur was cemented into position, excess cement was then removed. Poly placed into position. The knee was then reduced and held in full extension with a bump under the ankle.
Patella cemented into position. Excess cement was removed and held with patellar clamp. The clamp was then removed after cement hardened. Thorough lavage and injection was given. Medial parapatellar arthrotomy was closed, and the remainder of the wound was closed in layers.
Sterile dressing was then applied over the wound. The tourniquet was let down, and the patient was transferred to post operative care unit in stable condition, Patient was discharged from the post operative care unit after 28 hours. Patient had no complications with anesthesia/recovery.
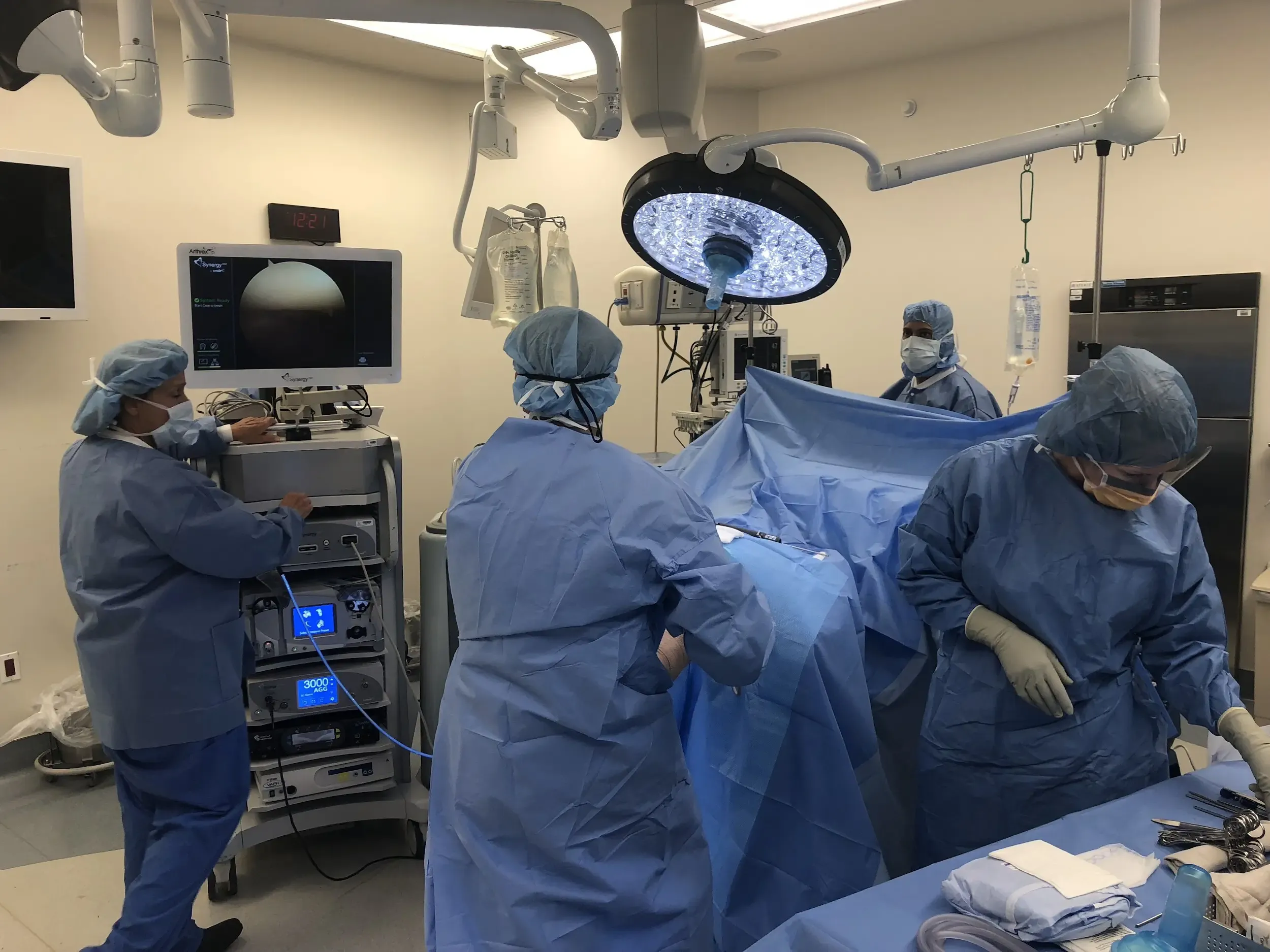
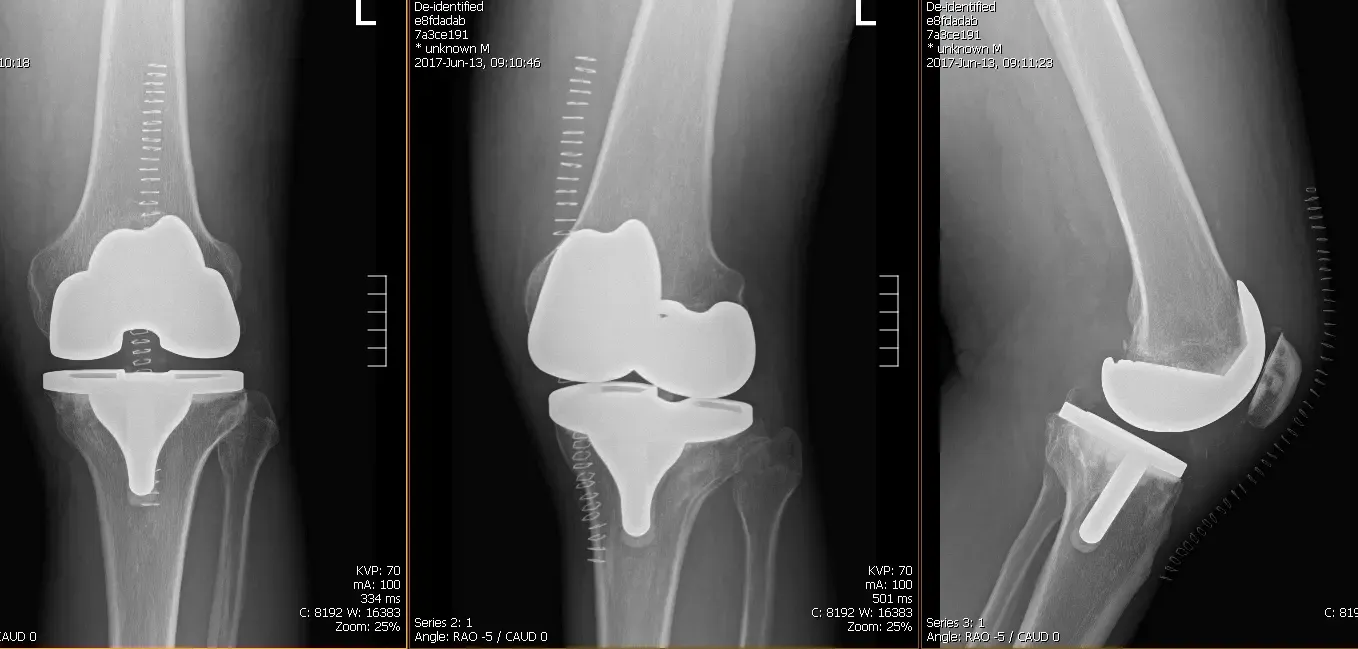
Postoperative films revealed Distal femur, patella, proximal tibia and proximal fibula demonstrate intact cortical margins with no acute fracture. His wound was inspected, clear no signs of infection.Staples removed.
Patients prognosis was good due to patients’ successful and uncomplicated surgery, he was compliant with the postop HEP program along with the standard outpatient physical therapy services.
Patient is weight bearing as tolerated with great flexion, extension, ROM. There was mild knee stiffness associated with arthroscopy but pain was scaled at a 3/10 at the 6 week follow up evaluation.
At the 3 month evaluation patient presented with full ROM, full weight bearing and a pain level scaled at 0/10. Patients physical therapy services were concluded with excellent results. Patients stated his quality of life was significantly improved, and can now move far better than he could even after his original procedure.
Patients home and work duties are completed with ease. Lower extremity use is excellent and requires no assistive devices, can get in and out of bed with no assist and ascend and descend on stairs with 0 pain. Patient was not expecting to be able to return to activities of daily living with optimal success, he stated we have exceeded his expectations of Left Total Knee Arthroscopy surgery.


