A 71-year-old female presented to our office with complaints of pain in her left shoulder and left hip. The patient stated that at the beginning of March 2017 she fell off the steps at the Post Office Cafe hitting her face on a car and landing on her left side. She was referred here by her PCP.
The pain was described as a dull ache located in the left groin anteriorly. The patient reported the intensity as moderate to severe (7/10). The pain increased in intensity insidiously since the onset. Activities such as walking, going up and down the stairs, bending, getting up from chair exacerbated the pain. She also complained of increasing stiffness especially after sitting for a long time.
The patient initially sought treatment from another physician for a year. She tried conservative management in the form of medications, physical therapy, heat pads, and laser therapy. She had an ultrasound-guided hip cortisone injections but with minimal relief.
She was a retired medical transcriber and currently living with her son and his family. She expressed dismay at the inability to go upstairs at her home and walk down the block. She stated difficulty in tying her shoelaces and getting up from bed after a long time. She described the pain as constant but not disturbing her sleep.
She was a nonsmoker and nondrinker. She was allergic to penicillin. Her past medical history was positive for diabetes mellitus, hyperlipidemia, coronary artery disease (CAD) and varicose veins. In the past, she had a left shoulder arthroscopic surgery and endovenous laser ablation therapy. She had a cardiac catheterization done last year which suggested non-obstructive CAD.
On physical examination, she walked with an antalgic gait. The stance phase of the gait was reduced on the left side. Bilateral shoulder, anterior and posterior iliac spines, patella and medial malleolus were at the same level. There as no exaggerated lumbar lordosis. There was no structural or functional scoliosis.
There was no evidence of any leg length discrepancy. Tenderness was positive on the left anterior hip joint line. There was no fullness or swelling in the Scarpa’s triangle. The skin overlying the left hip and buttock was normal. There was no tenderness on bilateral trochanter. There was no abnormal thickening/broadening of the trochanter.
The range of motion was restricted especially in the abduction and internal rotation. There was no fixed adduction or flexion deformity. There were no enlarged inguinal lymph nodes. The examination of the right hip, bilateral knee and ankles were normal. There was no distal neurological deficit. Bilateral lower extremity pulses were palpable and good volume.
Imaging revealed severe osteoarthritis of the left hip. Considering, patients’ medical conditions and lifestyle limiting hip pain, she was advised left total hip replacement. Risks, benefits, and alternatives were discussed at length. She agreed to go ahead with the procedure.
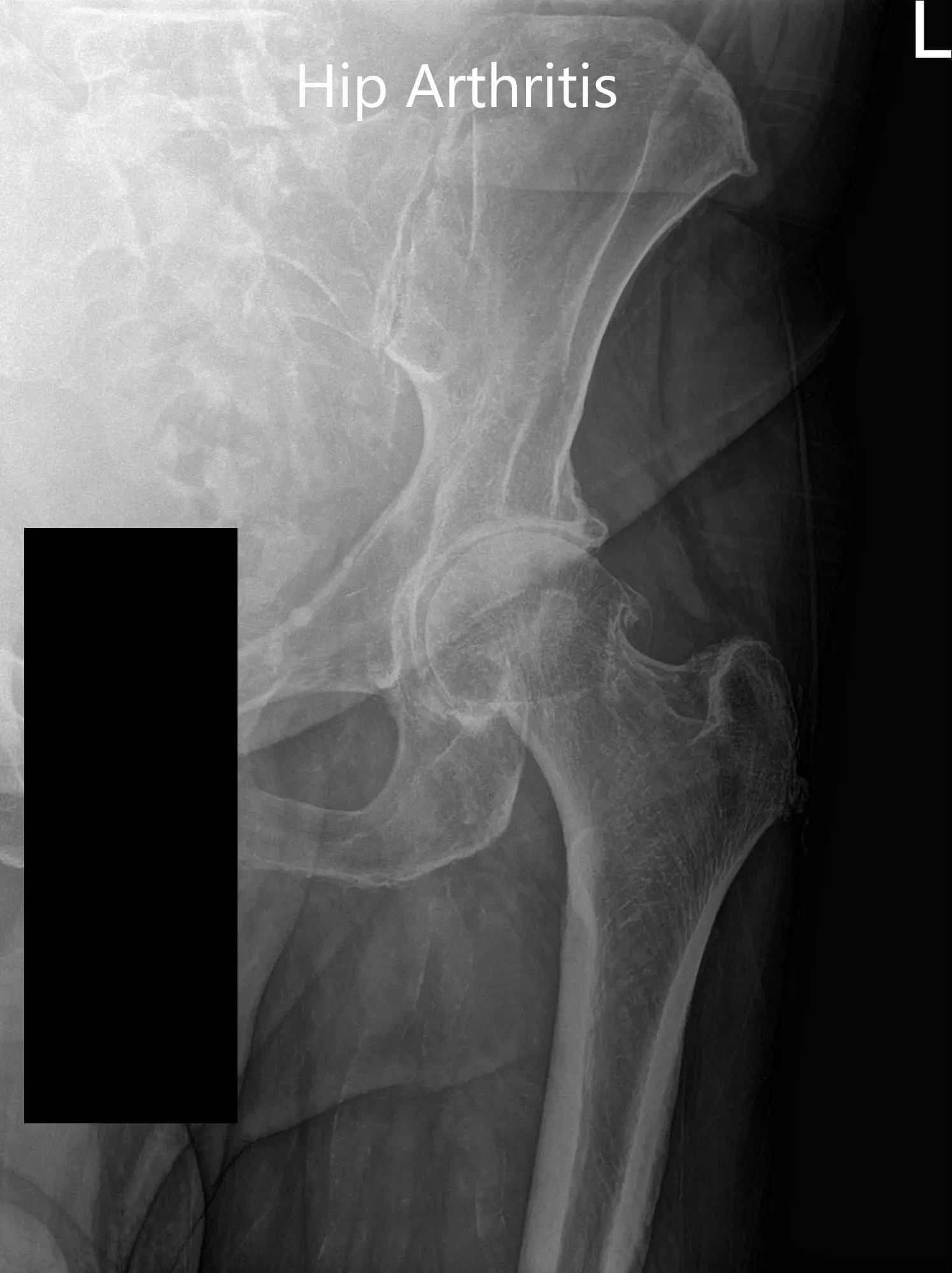
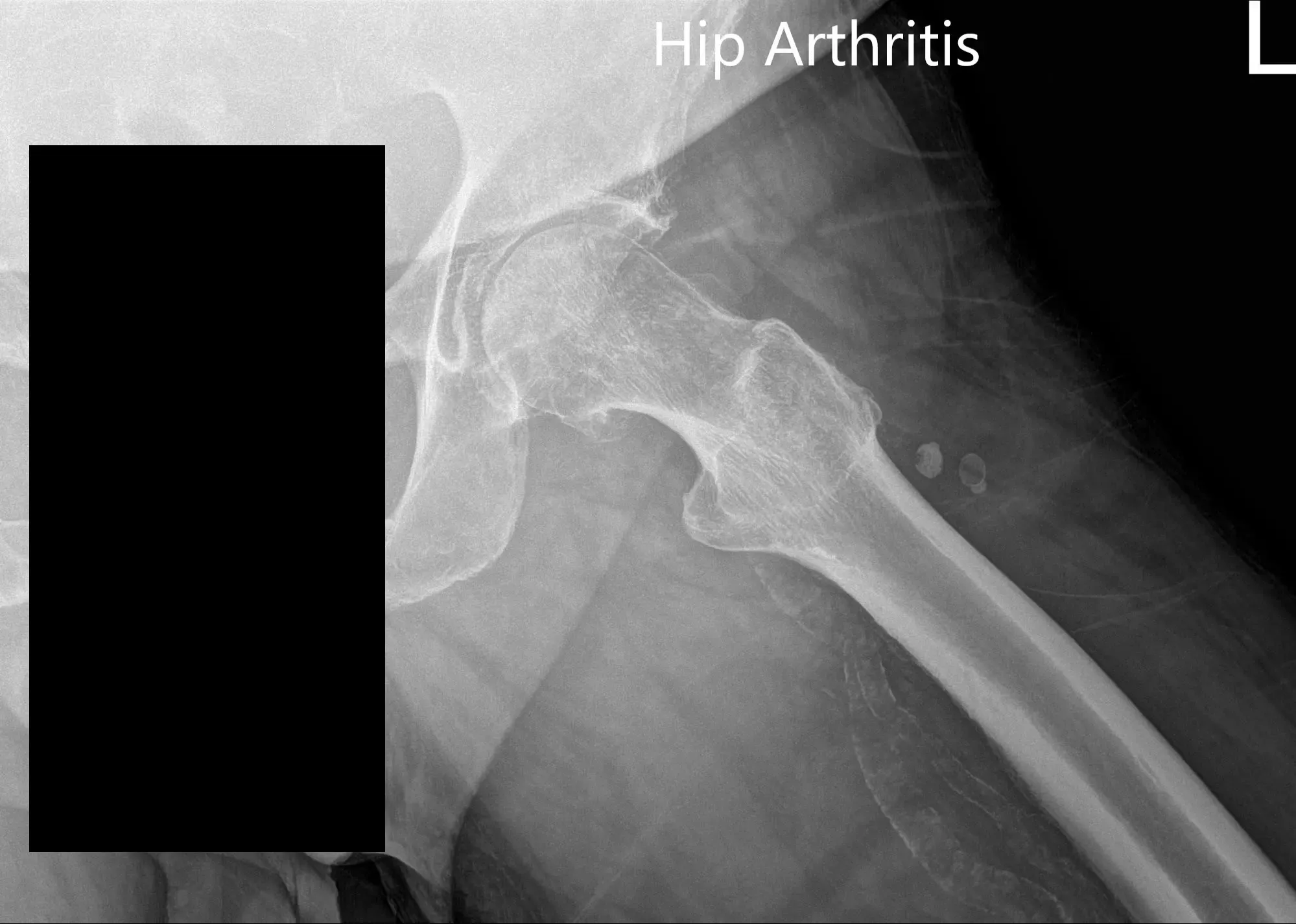
Preoperative X-ray of the left hip showing AP and frog-legged lateral view
OPERATION: Left total hip arthroplasty, robot-assisted.
IMPLANTS USED: Ceramic femoral head 36-mm plus 5 with 127-degree neck stem system size 5 with a 54-mm acetabular shell cluster hole with polyethylene insert with a 25-mm screw.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as with his relative,
prior to the procedure. They understand she is at increased risk of medical and surgical complications prior to the surgery.
The patient was brought to the operating room. Anesthesia was obtained by the anesthesiologist. The patient was then definitively positioned with the left hip up and the left hip was then draped and prepped in the usual sterile manner. A curved incision centered over the greater trochanter was used for the arthrotomy. Skin and subcutaneous tissues were incised.
The fascia was then divided. The posterior soft tissue structures were then taken down and tacked for future repair. A probe was placed over the greater trochanter and the limb length was measured prior to the dislocation. Before making the incision for the hip replacement, three external fixator pins were placed over the iliac crest and the array was then connected with the robot.
The limb length was measured preoperatively and the hip was then dislocated. The lesser trochanter to the center measurement was taken and was compared to the preoperative templating. The neck resection was made at the correct level. The head was then removed.
Attention was then turned towards the cup. The remainder of the labrum was then debrided. The acetabulum was analyzed and the marker was placed over the superior aspect of the acetabulum and the array was then connected to the robot. Bone morphing was performed.
The robotic arm was used to ream the bone and for placing of the cup. The cup was also assessed manually for the correct abduction and anteversion after placement. The screw was used for additional fixation. Thorough lavage was given. Poly was placed over the cup.
Attention was then turned towards the femur. The femur was then sequentially broached. The final broach was left into position. The trochanter and the head were placed over the broach. Lesser trochanter to the center measurement was taken and was found to be correct. The hip was then relocated and was trialed through a full physiologic range of motion and hip was stable in all physiological range of motion.
The hip was then dislocated. Trial components were then removed. Final components were then placed into position and the limb assessment was performed again on the robot and was found to be correct. The trochanteric landmark and the acetabular landmark were then removed. Thorough lavage was given again.
Posterior soft tissue structures were then tacked to the greater trochanter through transosseous tunnels. The fascia was closed with Vicryl and Ethibond. Cutaneous tissues were closed with Vicryl. Subcuticular tissues we re closed with 2-0 Vicryl. The skin was closed using staples.
The external fixator pins were then removed and the pin site was then closed with 2-0 Vicryl and staples. Sterile dressing was applied over both wounds. The patient was then transferred to the postoperative care unit in stable condition.
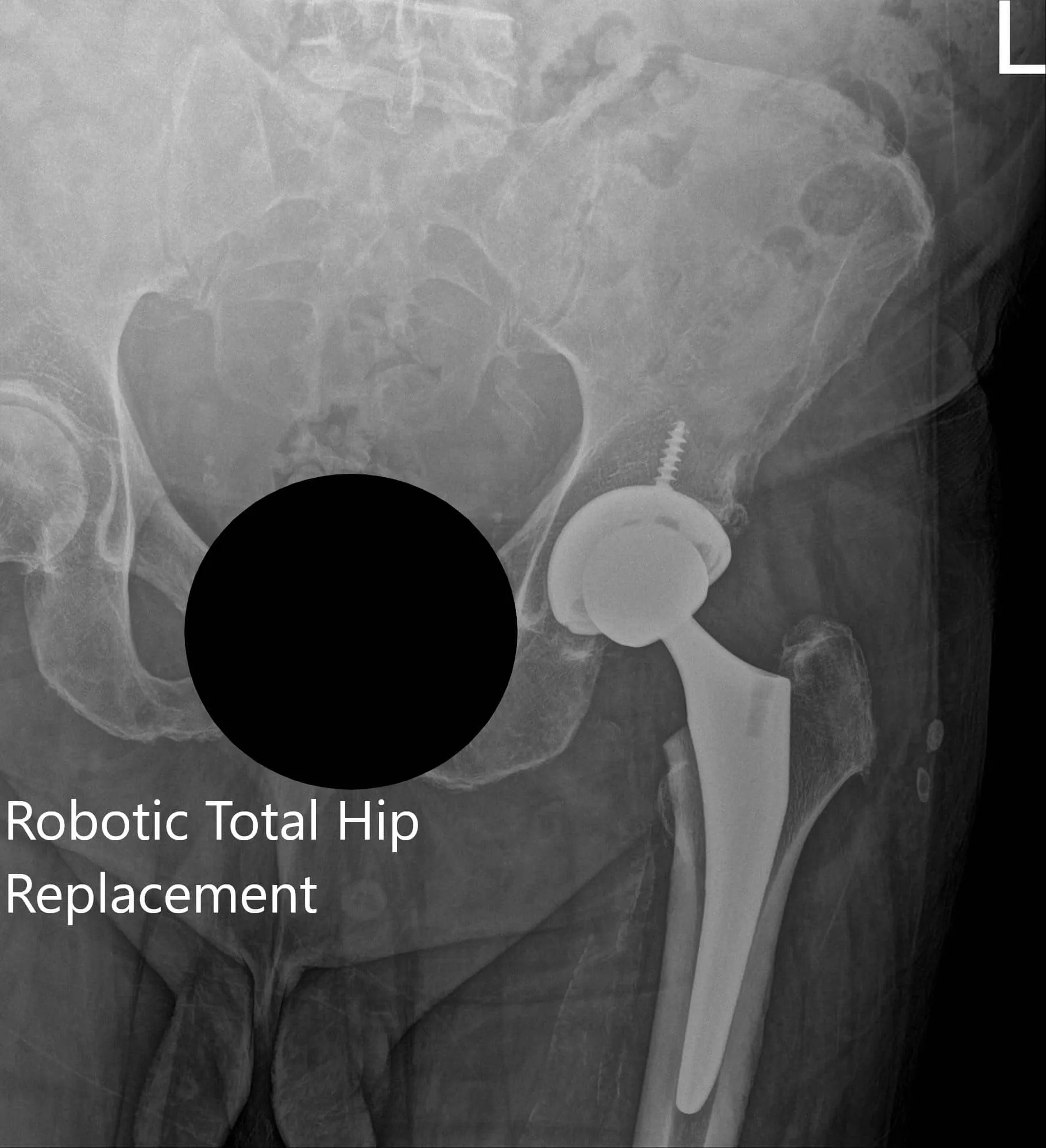
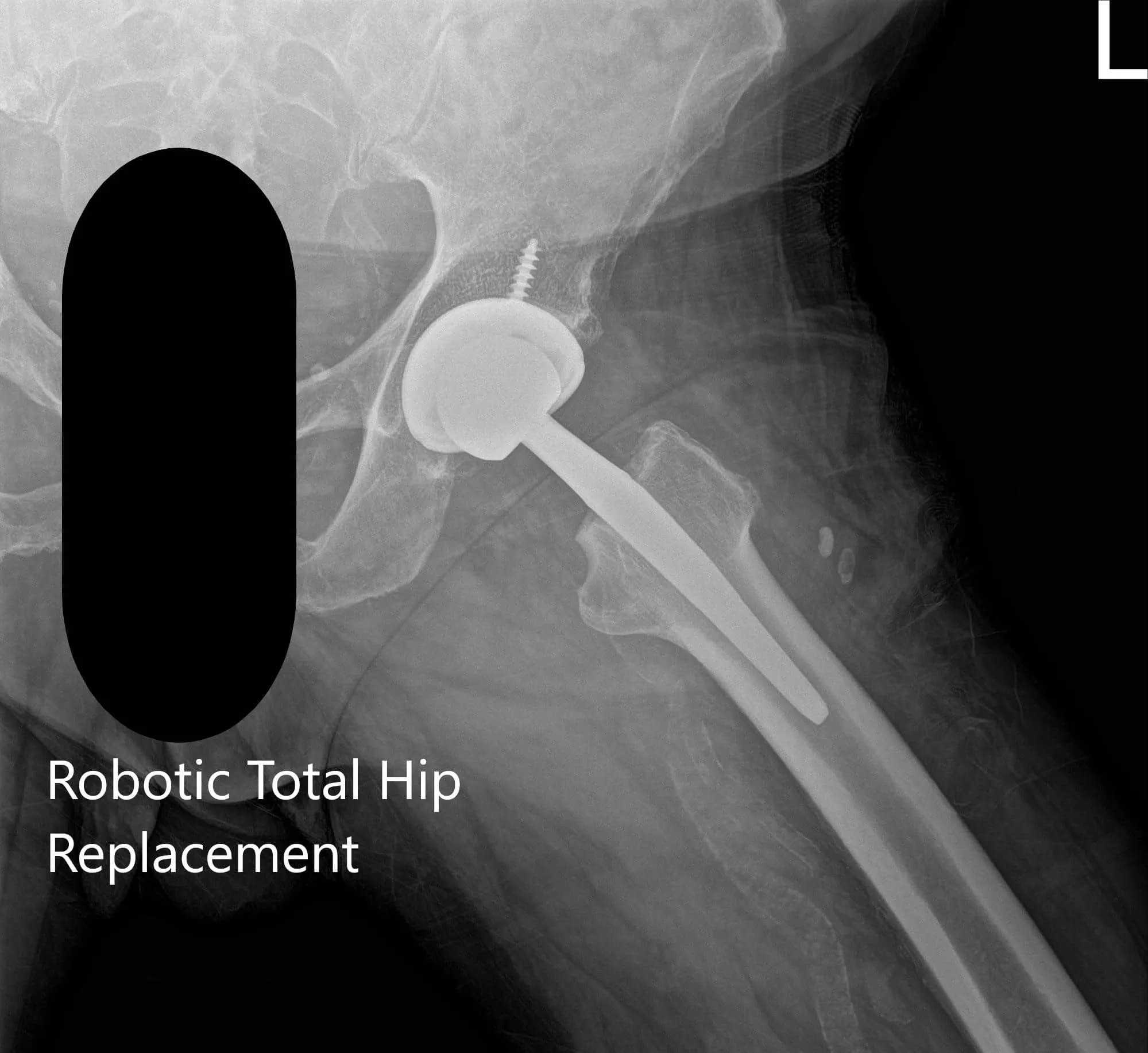
Postoperative X-ray of the left hip showing AP and frog-legged lateral view
Post-op her vitals remained stable. Abduction pillow was used and she was educated about hip precautions in detail. Aspirin 325mg was started to prevent deep vein thrombosis. The pain was controlled well with medications. She was allowed weight bearing as tolerated with support.
Physical therapy was started to strengthen the muscles and increased flexibility. Gait training and fall prevention education was given to the patient. She had an excellent recovery and reported zero pain in three months follow up. She was able to walk and perform her daily activities without any discomfort. She was satisfied with the outcome of the procedure.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


