A 67-year-old female presented to our office with complaints of bilateral knee pain which was greater on the left side. The patient worked as a security guard and stated she had a slip and fall while walking on wet cement four years back, injuring her both knees, shoulders and lower back. She was treated at a hospital and was released subsequently. She stated while her other injuries resolved, the left knee pain worsened over time.
She consulted an orthopedic surgeon for her left knee pain and was subjected to arthroscopic debridement of the joint and knee injections. Initially, she stated to have experienced relief but the pain returned. She also stated to have tried physical therapy, heat pads, pain medications, and braces but with only momentary relief.
The patient stated that since the last year her left knee pain has restricted her daily activities such as walking, climbing stairs, kneeling and getting up from the chair. She was unable to walk her dog, a routine she enjoyed earlier. She was visibly under immense emotional distress due to pain and had recently learned about knee replacement surgery from one of her colleagues.
On her office visits she stated to be a former smoker having quit 20 years ago and with a past medical history of hyperlipidemia and hypertension, both well controlled with medications. Her physical examination revealed mild swelling in the left knee. On palpation, there was medial joint line and medial patellar facet tenderness.
The patient had a previous trial of conservative management but had lifestyle limiting left knee pain. She was found to be a candidate for a left total knee replacement after discussing all management options in detail. She was well motivated and looked forward to her surgery. The patient was given an option of custom knee replacement and she agreed with the plan.
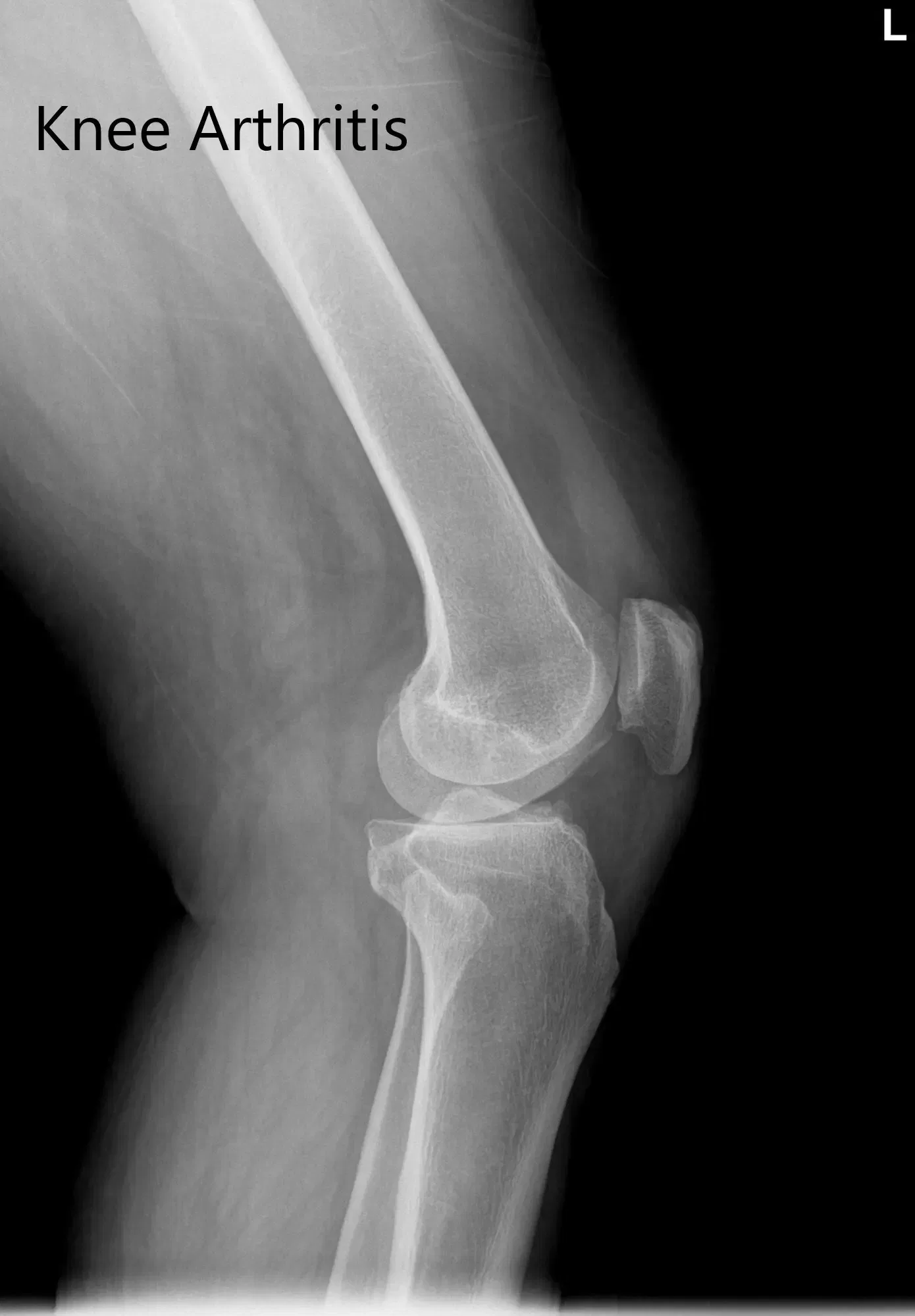

Pre-operative X-ray of the left knee showing AP and lateral views
Imaging studies demonstrated medial joint space narrowing with degenerative changes. A CT scan of the patient’s left knee with hip and ankle was obtained a few weeks before the surgery demonstrating tricompartmental osteoarthritis. The data from the CT scan were used to create a 3D model of the patient’s anatomy. The data was then used to create custom implants and custom instruments.
Custom implants and instruments offer surgeons to have perfect alignment and recreation of the joint line before the disease process with bone preservation. A custom patient-specific plan was provided detailing the sizing and cuts of the procedure for accurate alignment. Disposable 3 D printed jigs were to be used designed uniquely for the patient to create bone resection. The details were outlined in a preoperative plan.

Complete Orthopedics patient-specific surgical plan for a left custom knee replacement in a 67-year-old female.

Complete Orthopedics patient-specific surgical plan for a left custom knee replacement in a 67-year-old female (scan 2)
Operative Notes:
The patient underwent a left total knee arthroplasty using the customized femoral component with a customized tibial component with a 32 mm patella with an 8 mm polyethylene insert.
Prior to the procedure, the patient was brought to the operating room and anesthesia was obtained by the anesthesiologist. The left knee was then definitely positioned and was draped in the usual sterile manner. A straight incision was used for the arthrotomy after exsanguinating the limb and elevating the tourniquet.
Skin and subcutaneous tissue were incised. A medial parapatellar arthrotomy was performed. The femoral cutting guide was then placed into position and the femur cuts were made.
The tibial cutting guide was then placed in position, tibial cuts were then made. Laminar spreaders were used medially and then laterally and the remainder of the menisci and the cruciate were then debrided. The knee was balanced. The trial components were then placed into position.
The knee was then trialed through the physiological range of motion and patellar tracking was found to be perfect. The range of motion of the knee was felt the knee was very well balanced.
The trial components were then removed and the femoral component was cemented into position. Excess cement was removed. The tibial component was cemented into position, excess cement I removed.
The poly was placed into position and the knee was reduced and was held in full extension with a bump underneath the knee joint.
The patella was then cemented into position and was held within a patellar clamp. Once the cement hardened excess cement was then removed. The knee was injected with Marcaine.
After the cement hardened, the clamp was removed. Medial parapatellar arthrotomy was closed. Cutaneous tissues were closed, subcutaneous tissues were closed, the skin was closed using staples.
Sterile dressings were then applied over the wound and the patient was transferred to the postoperative care unit in stable condition.
The patient was able to walk with support the same day and her pain was well controlled. She was started on Aspirin 325mg BID for deep vein thrombosis (DVT) prophylaxis. On her subsequent visits, the wound was found to be clean, dry and intact. Skin staples were removed subsequently and she elicited an excellent range of motion of the left knee.
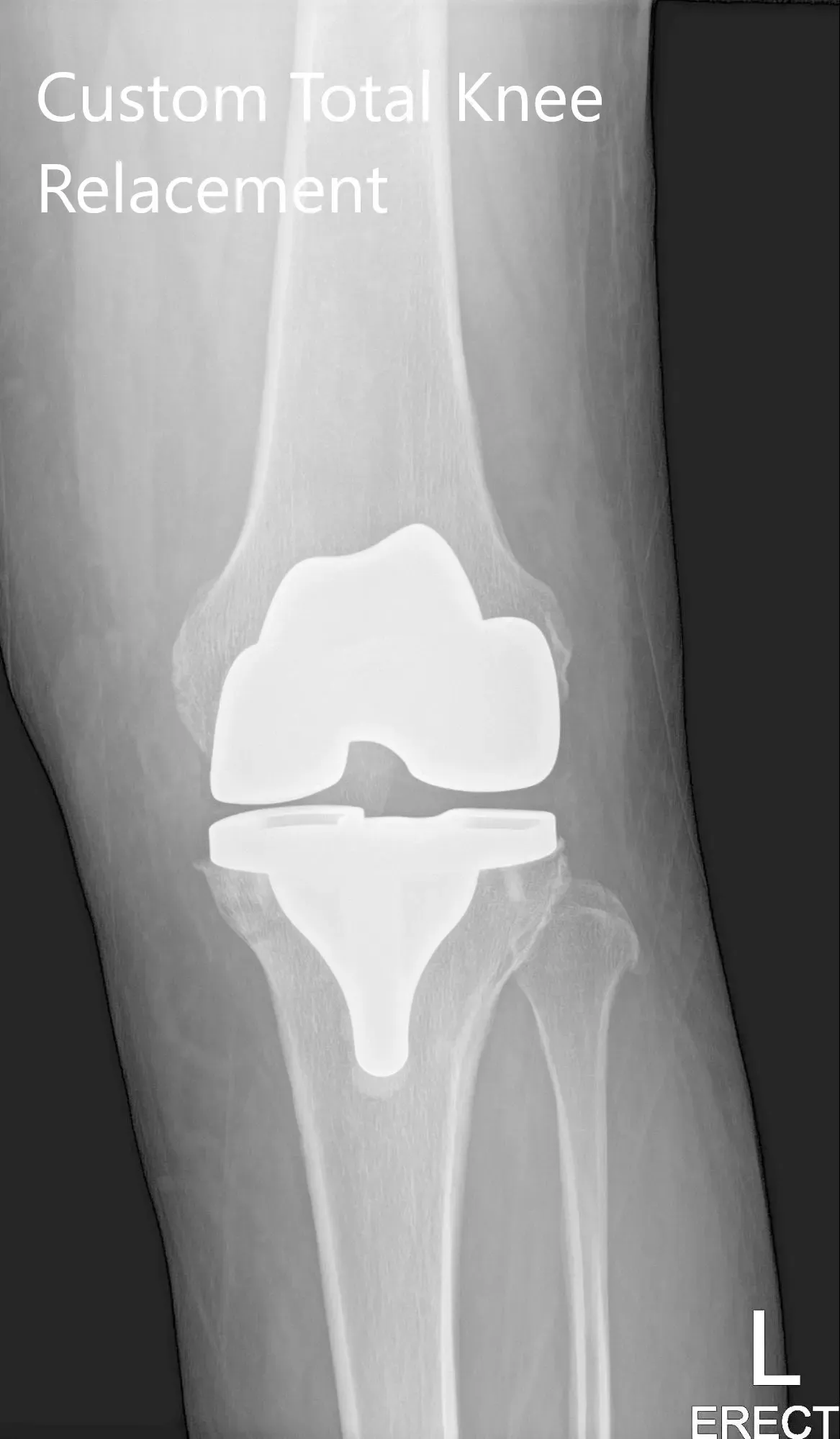
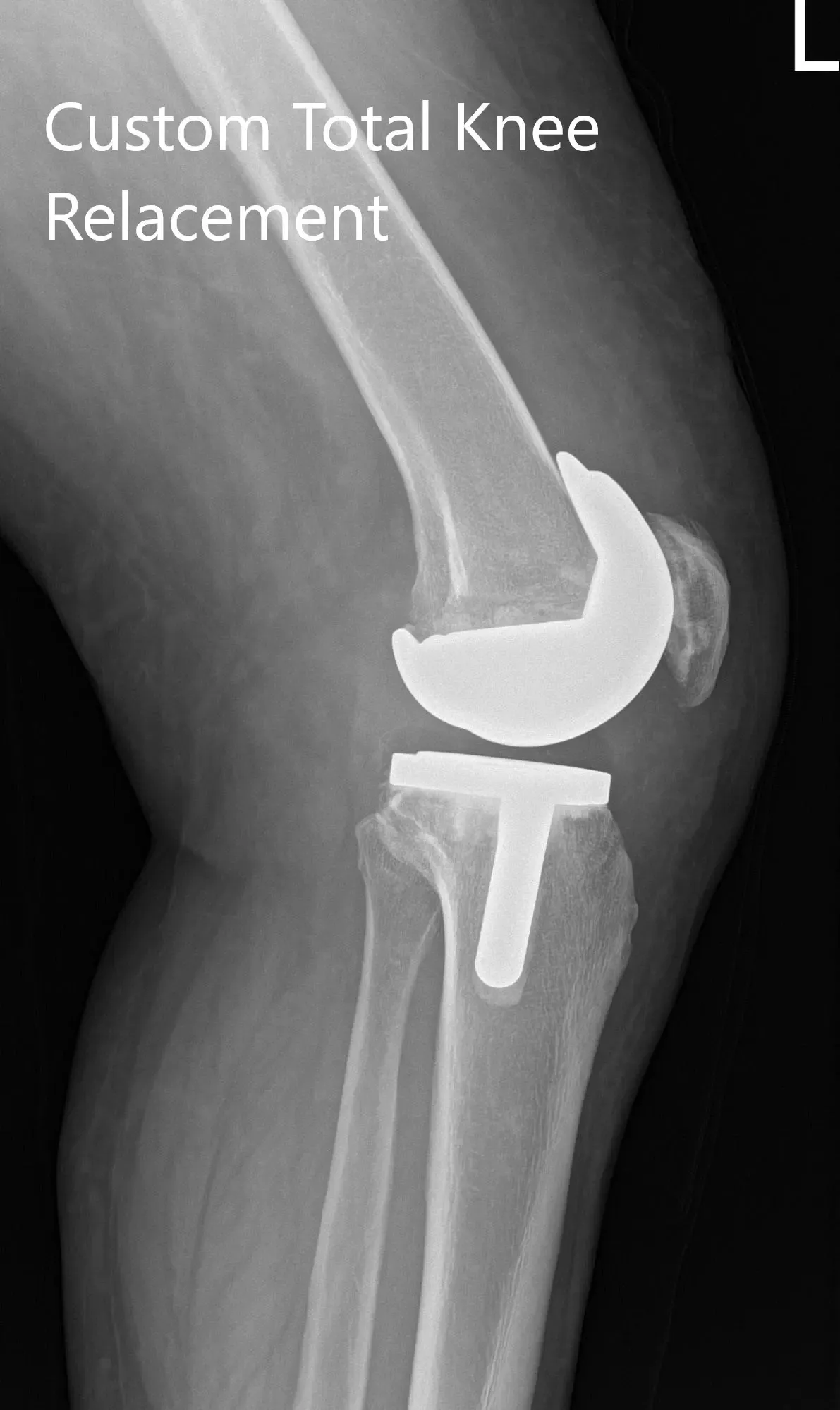
Post Operative X-ray images showing AP and lateral view of the left knee.
The patient had excellent compliance with physical therapy and range of motion exercises. She reported no discomfort in her daily activities and was happy she was able to walk her dog. She had joined a new job as a social worker and was happily able to carry her activities without pain and discomfort. She reported decreased pain in her right knee due to equal load sharing on both knees. She regularly follows up as needed.


