Knee discomfort is a common issue that can range from mild to severe. When knee pain becomes intense or persistent, it may significantly affect daily activities. Seeking medical advice is important to manage pain and prevent further complications. One potential cause of knee pain is kneecap maltracking, where the patella (kneecap) moves out of its normal alignment. This condition can cause pain, stiffness, and difficulty moving the knee.
How Common It Is and Who Gets It? (Epidemiology)
Kneecap maltracking is often seen in active individuals, particularly those who engage in sports. It may occur at any age but is more commonly seen in young adults who participate in activities that put stress on the knee joint. Individuals with anatomical or structural issues are also at higher risk, as are those who experience trauma to the knee.
Why It Happens – Causes (Etiology and Pathophysiology)
Kneecap maltracking is caused by several factors that affect the proper alignment of the patella within the groove of the femur (thigh bone). These factors include muscle weakness, anatomical abnormalities (e.g., patella alta or dysplastic patella), and injuries. When the patella doesn’t track correctly during movement, it leads to stress on the joint, eventually causing pain and damage to the cartilage.
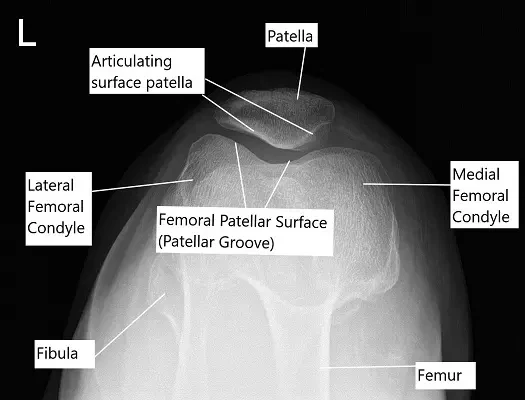
Skyline X-ray view of the patella.
How the Body Part Normally Works? (Relevant Anatomy)
The knee joint is the largest in the body and consists of the tibiofemoral and patellofemoral joints. The patellofemoral joint allows the patella to move smoothly within a groove on the femur, which is critical for proper knee movement. When maltracking occurs, the patella does not glide properly, which can lead to increased stress on the knee joint.
What You Might Feel – Symptoms (Clinical Presentation)
Common symptoms of kneecap maltracking include anterior knee pain, especially at the front of the knee. People with this condition may also experience the sensation of the knee “giving away” during activities like walking or running. Some individuals may feel a grinding or popping sensation. In more severe cases, the patella may dislocate, causing acute pain and swelling.
How Doctors Find the Problem? (Diagnosis and Imaging)
Diagnosing kneecap maltracking typically involves a thorough physical examination, where the doctor assesses the movement of the patella. Key diagnostic tests may include the Q angle, which measures the alignment of the patella in relation to the femur. Imaging tests such as X-rays, MRI, or CT scans may be used to evaluate joint structure and identify underlying causes of maltracking.
Classification
Kneecap maltracking can be classified by the severity of the symptoms and the underlying causes. It may be categorized as mild, moderate, or severe, depending on how much the patella deviates from its normal path. In severe cases, there may be significant cartilage damage or recurrent dislocations.
Other Problems That Can Feel Similar (Differential Diagnosis)
Other conditions that may present with knee pain and symptoms similar to kneecap maltracking include patellar tendinitis, chondromalacia patella, and osteoarthritis. A healthcare provider must differentiate these conditions to ensure appropriate treatment.
Treatment Options
Non-Surgical Care
Non-surgical treatments for kneecap maltracking often involve a combination of anti-inflammatory medications, rest, and physical therapy. Therapy may focus on strengthening the quadriceps muscles, particularly the vastus medialis obliquus (VMO), to help correct muscle imbalances. This approach is generally recommended for less severe cases.
Surgical Care
In more severe cases, surgical intervention may be necessary. Common procedures include lateral release, where the tight ligament on the outer knee is cut, and medial patellofemoral ligament (MPFL) repair, which stabilizes the inner side of the patella. Bony procedures like osteotomy or trochleoplasty may be performed when there is significant misalignment of the patella or femur..
Soft tissue Surgeries
Soft tissue procedures are used to repair or tighten loose and stretched soft tissues or release of the tight ligaments that contribute to patellar instability. They are best indicated in isolation in the setting of recurrent instability with minimal underlying bony malalignment.
Lateral Release
A commonly used procedure is lateral release which is a knee arthroscopic surgery. Surgery is performed through small incisions and the tight ligament on the outer knee cap is released so as to allow the knee cap to settle towards the inside of the trochlea.
Medial PatelloFemoral Ligament (MPFL) Repair
Reconstruction of the Medial Patellofemoral Ligament (a ligament stabilising the inner side of patella preventing outward dislocation) is a procedure usually done for recurrent lateral patellar instability. The ligament provides vital inner side support to the patella. The ligament is tightened to provide stability to the knee cap.
Bony Procedures
When the underlying cause is bony malalignment, procedures such as:
- Osteotomy : Tibial tubercle (part of tibia providing attachment to patellar tendon) transfer osteotomy can be performed. It involves cutting of the bone and changing the insertion of the patellar tendon, the procedure ultimately affect the position of patella engaging in the trochlea during range of motion. It also prevents the damaged articular cartilage from coming in contact therefore reducing pain and increasing stability.
- Trochleoplasty : Lastly a procedure known as trochleoplasty may be indicated in the patient with significant trochlear dysplasia/malformation causing PFM. This procedure involves altering the shape of the trochlea so that the patella engages in the trochlea effectively during the range of motion.
If you have any above said symptoms or may think you’re suffering from patellar maltracking disorder, consider visiting an orthopaedic surgeon with expertise in knee arthroscopy.
Recovery and What to Expect After Treatment
Recovery after treatment for kneecap maltracking typically involves rest, physical therapy, and gradual reintroduction of activities. After surgery, patients may use a brace or crutches to protect the knee while healing. The recovery process varies depending on the type of treatment and the severity of the condition.
Rest and Protection: After a diagnosis of kneecap maltracking, your healthcare provider may recommend resting the affected knee and avoiding activities that aggravate pain. This might mean taking a break from high-impact exercises like running or jumping to give your knee time to heal. Using supportive braces or taping techniques can also help protect the knee joint during this initial phase of recovery.
Physical Therapy: Physical therapy plays a crucial role in rehabilitating a knee affected by maltracking. A skilled physical therapist will design a personalized exercise program to strengthen the muscles around the knee, particularly the quadriceps and hamstrings. These exercises help correct muscle imbalances and improve the alignment of the patella within its groove. Additionally, the therapist may incorporate stretching exercises to improve flexibility and range of motion in the knee joint.
Modalities for Pain Relief: To manage pain and inflammation associated with kneecap maltracking, your healthcare provider may recommend modalities such as ice therapy, heat therapy, or transcutaneous electrical nerve stimulation (TENS). These modalities can help alleviate discomfort and promote healing in the affected area.
Activity Modification: During the recovery period, it’s essential to modify activities that put excessive stress on the knee joint. Your healthcare provider may advise you to avoid activities like squatting, kneeling, or prolonged sitting with the knees bent. Instead, focus on low-impact exercises like swimming or cycling that provide cardiovascular benefits without straining the knees.
Gradual Return to Activity: As your knee begins to heal and strengthen, your healthcare provider will guide you through a gradual return to your normal activities. This may involve starting with gentle exercises and gradually increasing intensity and duration as tolerated. It’s essential to listen to your body and avoid pushing through pain during this phase of recovery.
Long-Term Management: Once you’ve completed the initial phase of recovery, it’s crucial to maintain a proactive approach to knee health. This includes continuing with prescribed exercises to keep the muscles around the knee strong and flexible. It’s also essential to maintain a healthy weight and avoid activities that put excessive strain on the knee joint to prevent recurrence of maltracking.
Follow-up Care: Regular follow-up appointments with your healthcare provider are essential to monitor your progress and address any lingering concerns. Your provider may recommend periodic check-ups to assess your knee function and make adjustments to your treatment plan as needed.
Possible Risks or Side Effects (Complications)
Potential complications from kneecap maltracking treatment include infection, blood clots, or failure of the surgery to fully correct the misalignment. There is also a risk of recurring instability or continued pain, particularly if the underlying cause of the maltracking is not adequately addressed.
Long-Term Outlook (Prognosis)
With proper treatment, most individuals with kneecap maltracking can achieve significant improvement in pain and knee function. Non-surgical treatments may require ongoing management, including physical therapy and activity modification. Surgery can provide long-term relief, though there is a possibility of recurrence if the condition is not managed properly.
For insurance and cost information, see our Insurance Information page.
Frequently Asked Questions (FAQ)
Q. What causes kneecap maltracking?
A. Kneecap maltracking is often caused by muscle weakness, anatomical abnormalities, trauma, or overuse.
Q. Can physical therapy help with kneecap maltracking?
A. Yes, physical therapy focusing on strengthening the muscles around the knee can be highly beneficial.
Q. What is the best treatment for kneecap maltracking?
A. Treatment depends on the severity. Non-surgical options, such as physical therapy, are effective for mild cases, while surgery may be necessary for severe cases.
Q. How long does recovery take after surgery?
A. Recovery time varies but generally takes several weeks to months, depending on the type of surgery performed.
Q. Can kneecap maltracking lead to arthritis?
A. Yes, if untreated, kneecap maltracking can lead to damage to the cartilage and the development of osteoarthritis.
Summary and Takeaway
Kneecap maltracking is a condition that causes pain, instability, and difficulty moving the knee. It can be caused by muscle imbalances, anatomical issues, or injuries. Non-surgical treatments like physical therapy can help, but surgery may be needed for severe cases. With the right treatment, most individuals can manage the condition effectively and return to normal activities.
Clinical Insight & Recent Findings
A recent study explored the long-term outcomes of patellar maltracking treatment and found that patients who underwent lateral release and physical therapy had significant improvements in knee stability and a reduction in pain levels.
The study highlighted the effectiveness of combining surgical intervention with a focused rehabilitation program, especially in younger patients and athletes. This approach not only alleviated symptoms but also reduced the risk of further complications, such as osteoarthritis, by promoting proper knee alignment and strengthening surrounding muscles.
These findings support the value of a multi-faceted treatment approach for managing patellar maltracking. (“Study of Patellar Maltracking Treatment Outcomes – see PubMed”)
Who Performs This Treatment? (Specialists and Team Involved)
Orthopedic surgeons, particularly those specializing in knee surgery, are typically involved in the treatment of kneecap maltracking. A team may also include physical therapists to assist with rehabilitation and recovery.
When to See a Specialist?
You should see a specialist if you experience persistent knee pain, instability, or episodes of dislocation that do not improve with rest or physical therapy.
When to Go to the Emergency Room?
Seek emergency care if you experience severe pain, swelling, or if the kneecap dislocates and cannot be relocated. Immediate medical attention is necessary to prevent further damage to the joint.
What Recovery Really Looks Like?
Recovery from kneecap maltracking involves a combination of rest, rehabilitation, and gradual return to normal activities. It may take several weeks or months to fully recover, and some individuals may require ongoing physical therapy to maintain knee function.
What Happens If You Ignore It?
Ignoring kneecap maltracking can lead to worsening pain, cartilage damage, and osteoarthritis. It may also result in recurrent instability or the need for more invasive treatments later on.
How to Prevent It?
Preventing kneecap maltracking involves maintaining strong and flexible muscles around the knee, using proper techniques during physical activities, and addressing any anatomical issues early with the help of a healthcare provider.
Nutrition and Bone or Joint Health
Eating a diet rich in calcium and vitamin D is essential for maintaining healthy bones and joints. Proper nutrition can help support joint health and reduce the risk of conditions like osteoarthritis.
Activity and Lifestyle Modifications
Low-impact activities like swimming or cycling are ideal for individuals with kneecap maltracking, as they provide cardiovascular benefits without putting undue stress on the knee joint. Avoiding high-impact sports and activities that exacerbate symptoms can also help prevent further damage.


