A 50-year-old male patient who started experiencing excruciating pain down his left leg with weakness in that leg and numbness in his peroneal region. His sensory deficit included his lateral thigh and entire foot as well. He obtained an MRI that showed a disk fragment compressing on the L5 and S1 nerve roots with severe lumbar stenosis in the lateral recess and encroachment on the left side at L5 and S1.
Grade I anterolisthesis of L2 on L3. Straightening of the lumbar lordosis. Degenerative changes are identified diffusely within the lumbar spine. At L5-S1, there is a left-sided disc herniation/protrusion causing mild narrowing of the thecal sac and narrowing of the left lateral recess. This encroaches upon the left S1 nerve root within the left lateral recess.
The hernia also extends into the proximal left neural foramen causing mild narrowing. The mild right neural foraminal narrowing is also visualized. Mild to moderate narrowing of the thecal sac is identified at L2-3.
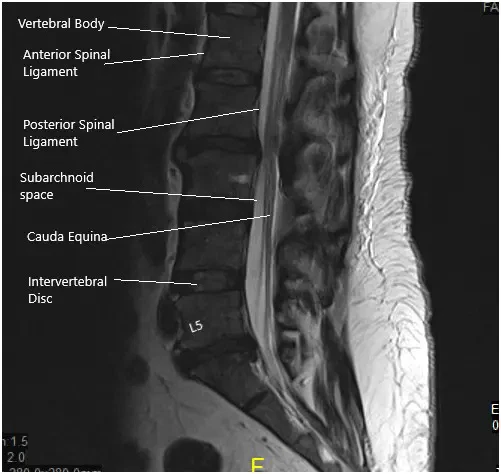
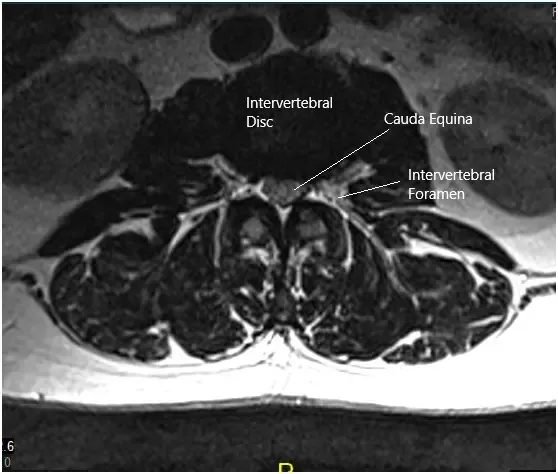
MRI of the lumbosacral spine in sagittal and axial views.
Given his signs and symptoms with neurological compromise as well as imaging findings, we considered this an emergency and offered the patient immediate surgery and he gave informed consent, understanding all the risks, benefits, and alternatives to spine surgery.
PREOPERATIVE DIAGNOSES:
- Left leg monoparesis.
- Severe lumbar stenosis with an acute herniated disk at L5-S1 and cauda equina syndrome.
POSTOPERATIVE DIAGNOSES:
- Left leg mono-paresis.
- Severe lumbar stenosis with an acute herniated disk at L5-S1 and cauda equina syndrome.
OPERATION:
- L5/S1 foraminotomy.
- L5/S1 discectomy.
- L5 and S1 neuroplasties.
- Application of epidural steroid paste.
- Use of intraoperative neuromonitoring.
- Use of intraoperative fluoroscopy.
- Use of intraoperative surgical microscope.
ANESTHESIA: General endotracheal anesthesia.
ESTIMATED BLOOD LOSS: Minimal.
PROCEDURE IN DETAIL: The patient was identified in the preoperative holding area and then brought back to the operating room where she was induced under general anesthesia and then intubated without incident. Neuromonitoring electrodes were attached and tested.
The patient was turned prone on to a Wilson frame attached to a Jackson table. All of her pressure points were padded and secured and, using palpable bony landmarks, we marked an incision over the L5-S1 interspace using an indelible marker. We then prepped and draped the patient in the usual sterile fashion and a call to order was completed.
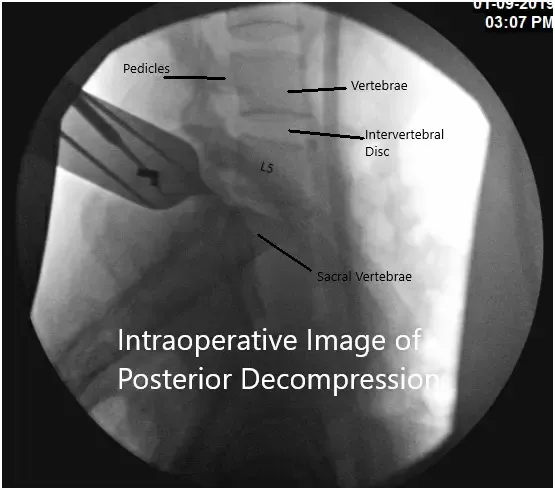
Intraoperative fluoroscopic image.
Preoperative antibiotics were dosed and fluoroscopy was used to localize our incision using a spinal needle inserted at the L5-S1 disk interspace. A #10 blade was used to incise the skin in the midline over the L5-S1 interspace down to the level of the subcutaneous fat.
Thereafter, Bovie cautery was used to continue the dissection along the left laminae of L5 and S1 exposing the interspace. We used a Taylor retractor to hold the muscle and skin edges apart. Using fluoroscopy once again, we confirmed our level of operation. A high-speed electric drill was used to create a foraminotomy at L5 and S1 in order to expose the epidural space.
The ligamentum flavum was removed using curettes and Kerrison punches. At this point, we brought in the surgical microscope and under intense illumination and magnification, we explored the S1 nerve root after identifying it clearly.
There was a significant amount of hypertrophied ligamentum flavum and the nerve root was under significant pressure. There was EMG activity as we tried to manipulate the nerve root and we noted that there was an anatomic anomaly of this nerve root. There was a duplicated S1 nerve root and a conjoined L5-S1 nerve root as well. This was an extremely rare finding, but this also explained the hypersensitivity of these nerve roots as well.
We continued our exploration very carefully removing additional bone into the lamina of L5. Because of the duplicated nerve root, we were not able to safely reach the disk in the axilla; however, we were able to go over the shoulder of the S1 nerve root as well as into the axilla of the L5 nerve root.
We completed wide foraminotomies at L5 and S1 and freed these nerve roots circumferentially of all compressive elements from the thecal sac and out of their respective neural foramen. Using a love nerve root retractor, we came over the shoulder of S1 and into the axilla of L5 and exposed the herniated disk.
This was entered with a #11 blade and removed with a pituitary rongeur. This material was then sent for pathology. We continued our exploration thoroughly using the Woodson dental instrument and removed additional herniated and extruded disk material. We controlled all bleeding using bipolar cautery in a meticulous fashion and applied an epidural steroid paste to the L5 and S1 nerve roots.
Once we’re satisfied with the decompression, we closed the incision in layers using 0-Vicryl sutures into the muscle and fascia, 2-0 Vicryl sutures in an inverted interrupted fashion in the subcutaneous space and we applied vancomycin powder on to the muscle beds. The skin was closed using a subcuticular Monocryl stitch and the incision was dressed with Steri-Strips and an island dressing.
All neuromonitoring signals returned to their baseline and remained stable throughout the case.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


