At Complete Orthopedics, our spine specialists focus on helping patients with back pain through careful diagnosis, personalized treatment plans, and, when necessary, advanced surgical options. We take time to understand your symptoms and identify their cause so we can recommend the most effective path toward recovery.
Our clinics are conveniently located throughout New York City and Long Island and are affiliated with six leading hospitals, providing patients with access to modern facilities and experienced orthopedic surgeons. Appointments can easily be scheduled online or by phone.
How Common It Is and Who Gets It? (Epidemiology)
Back muscle spasms are one of the most common causes of back pain. They can affect people of any age, from young athletes to older adults. Those who perform repetitive bending, lifting, or twisting motions—such as workers, athletes, or people with physically demanding jobs—are more likely to experience spasms. Sedentary lifestyles and poor posture can also increase the risk.
Why It Happens – Causes (Etiology and Pathophysiology)
Back muscle spasms occur when one or more muscles in the back tighten suddenly and involuntarily. This tightening often happens as the body’s way of protecting itself from injury. Common causes include:
- Lifting something too heavy or lifting with poor form
- Twisting the spine suddenly or awkwardly
- Sitting or sleeping in poor posture for long periods
- Overexertion during exercise
- Weak or unconditioned back and abdominal muscles
Sometimes, muscle spasms are a sign of a deeper spine problem such as a herniated disc (when the cushion between the vertebrae bulges out), spinal arthritis, or spinal stenosis (narrowing of the spine). Less commonly, conditions like osteoporosis, infection, or inflammation can cause muscle spasms due to irritation of nearby nerves.
How the Body Part Normally Works? (Relevant Anatomy)
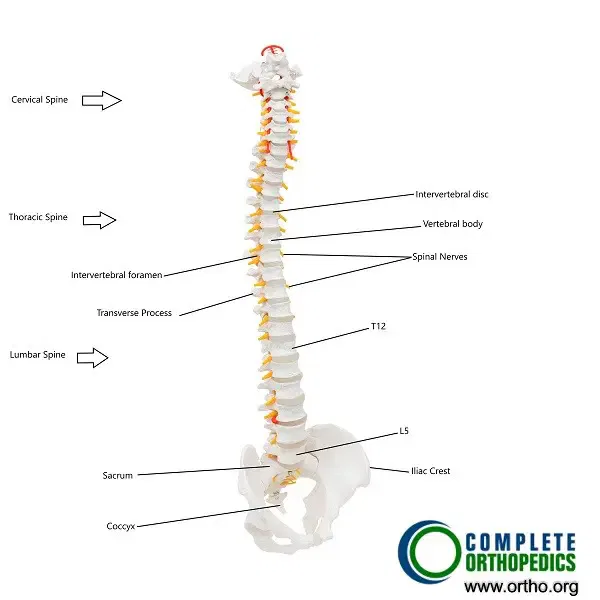
The spine is supported by several layers of muscles that work together to stabilize and move the back.
- The erector spinae muscles help maintain posture and allow bending and twisting.
- The latissimus dorsi and trapezius muscles help move the shoulders and upper back.
- Smaller muscles deep in the spine provide fine control and stability.
When these muscles are strained, overused, or fatigued, they can tighten suddenly to prevent further movement—resulting in a spasm.
What You Might Feel – Symptoms (Clinical Presentation)
Symptoms of back muscle spasms can range from mild discomfort to severe pain. Common signs include:
- Sudden, sharp, or cramping pain in the back
- Tightness or stiffness, especially after lifting or bending
- Difficulty standing upright or moving normally
- Muscle tenderness or soreness when touched
If the spasm is linked to a spinal issue, pain may radiate to the legs and be accompanied by tingling or numbness. In rare cases, such as when the spinal nerves are compressed, patients may experience weakness or loss of bladder or bowel control—these are medical emergencies requiring immediate care.
How Doctors Find the Problem? (Diagnosis and Imaging)
Diagnosis begins with a discussion about your symptoms, recent activities, and any history of back injuries. A physical exam helps the doctor identify which muscles are affected and whether there are signs of nerve involvement.
Most cases don’t require advanced imaging. However, if symptoms persist beyond a few weeks or are accompanied by numbness or weakness, doctors may recommend:
- X-rays to check bone alignment and rule out fractures
- MRI to examine discs, nerves, and soft tissues
- CT scans in more complex cases
These tests help determine whether muscle spasms are caused by a deeper spine problem.
Classification
Back muscle spasms are generally classified by their duration and underlying cause:
- Acute spasms: Last from a few hours to several days, often caused by minor strain or overuse.
- Chronic spasms: Last for weeks or recur frequently, often related to posture problems or spine disease.
Other Problems That Can Feel Similar (Differential Diagnosis)
Conditions that can resemble muscle spasms include:
- Sciatica (nerve pain from a herniated disc)
- Kidney stones or infections causing flank pain
- Gallbladder problems causing upper back discomfort
- Spinal arthritis or degenerative disc disease
- Fibromyalgia or muscle inflammation
A detailed history and physical exam help doctors rule out these causes.
Treatment Options
Non-Surgical Care
Most patients recover with conservative treatment. Typical measures include:
- Rest and activity modification: Avoid activities that trigger pain but remain lightly active. Prolonged bed rest is discouraged.
- Cold therapy: Apply ice packs for 10–20 minutes several times a day during the first 48 hours to reduce pain and swelling.
- Heat therapy: After a couple of days, switch to warm compresses or heating pads to relax tight muscles and improve blood flow.
- Pain relief medications: Over-the-counter options like acetaminophen or ibuprofen help manage discomfort and reduce inflammation.
- Muscle relaxants: Sometimes prescribed for severe spasms that don’t respond to simple measures.
- Physical therapy: Once pain subsides, stretching and strengthening exercises help restore movement and prevent recurrence.
Surgical Care
Surgery is rarely needed for back spasms unless they are caused by a structural spine problem such as a herniated disc, spinal stenosis, or instability. In those cases, procedures such as discectomy (removing part of a damaged disc) or laminectomy (relieving pressure on spinal nerves) may be considered after thorough evaluation.
Recovery and What to Expect After Treatment
Most people begin to feel better within two to three weeks with rest and simple home treatments. Gentle stretching and gradual return to normal activity are encouraged once pain decreases.
For chronic or recurring spasms, long-term relief often depends on improving posture, maintaining core strength, and avoiding repetitive strain. A physical therapist can guide proper techniques for movement and lifting.
Possible Risks or Side Effects (Complications)
If left untreated, repeated muscle spasms can lead to:
- Chronic back pain
- Limited mobility
- Muscle weakness or imbalance
- Poor posture or spinal strain
In rare cases involving nerve compression, delaying treatment can lead to lasting numbness or weakness.
Long-Term Outlook (Prognosis)
Most patients recover fully from back muscle spasms. Recurrence is possible, but regular exercise, good posture, and healthy habits greatly reduce the risk. Only a small percentage of patients require further intervention for underlying spine conditions.
For insurance and cost information, see our Insurance Information page.
Frequently Asked Questions (FAQ)
Q. Are back spasms dangerous?
A. Most are not dangerous and improve with rest and home care, but sudden severe spasms with leg weakness or numbness need immediate attention.
Q. Can stress cause back spasms?
A. Yes. Emotional stress can lead to muscle tension and increase the likelihood of spasms.
Q. Should I use heat or ice?
A. Use ice in the first 48 hours after injury, then switch to heat to relax the muscles.
Q. Can exercise help prevent spasms?
A. Yes. Regular stretching and strengthening exercises for your back and abdomen help prevent recurrence.
Summary and Takeaway
Back muscle spasms are common and often result from muscle strain, poor posture, or overuse. They typically improve within a few weeks with rest, gentle activity, and simple home treatments. However, persistent or severe pain—especially when accompanied by leg weakness or loss of bladder control—requires immediate medical attention.
With the right treatment and preventive care, most people can fully recover and return to normal activities without lasting problems.
Clinical Insight & Recent Findings
A recent study introduced the “ischemic model of chronic muscle spasm,” offering new insight into how persistent back muscle spasms may lead to chronic pain. The research demonstrated that prolonged muscle contraction reduces local blood flow, causing ischemia and energy depletion within muscle fibers. This cycle triggers spontaneous electrical activity, maintaining spasm and pain.
The study also described the “Coletti Method of EMG ChemoDenervation” (CMECD®), which targets these electrically overactive muscles using medications to suppress abnormal signals, restore blood flow, and reverse the ischemic injury. Findings showed significant long-term relief in most patients, with over 70% reporting substantial improvement without opioid use.
These results emphasize early diagnosis, targeted therapy, and non-opioid interventions for managing chronic back muscle spasms. (Study of the ischemic model of chronic muscle spasm – See PubMed.)
Who Performs This Treatment? (Specialists and Team Involved)
Treatment for back muscle spasms is typically provided by orthopedic surgeons, physical therapists, or rehabilitation specialists. In complex cases involving nerve compression, a spine surgeon may be consulted to evaluate for possible surgical treatment.
When to See a Specialist?
You should see a specialist if:
- Pain lasts more than two weeks despite home care
- Spasms are frequent or worsening
- You experience numbness, tingling, or weakness in your legs
- Pain interferes with work or daily activities
When to Go to the Emergency Room?
Seek emergency care if you experience:
- Sudden loss of bladder or bowel control
- Severe pain after a fall or injury
- Fever, unexplained weight loss, or night pain
- Numbness or weakness in the legs
What Recovery Really Looks Like?
Most patients recover quickly with proper rest and care. Initially, some soreness may persist, but improvement is steady with light movement, stretching, and posture correction. Ongoing exercise and strengthening help prevent future episodes.
What Happens If You Ignore It?
Ignoring repeated muscle spasms may lead to chronic pain, poor posture, and spine stiffness. Without addressing the cause, spasms can become more frequent and limit daily function.
How to Prevent It?
To prevent back spasms:
- Stretch regularly, especially before exercise or physical work
- Maintain strong core and back muscles
- Use proper posture while sitting, standing, and lifting
- Avoid sudden twisting or jerking motions
- Stay active and maintain a healthy weight
Nutrition and Bone or Joint Health
A healthy diet rich in calcium, vitamin D, and protein supports strong bones and muscles. Staying hydrated and avoiding smoking also help maintain tissue and joint health.
Activity and Lifestyle Modifications
After recovery, patients should resume physical activity gradually. Low-impact exercises like walking, swimming, and yoga help maintain flexibility and strength. Consistent exercise, good posture, and attention to ergonomics at work and home can greatly reduce the chance of recurrence.
Do you have more questions?
How long do back muscle spasms typically last?
The duration of back muscle spasms can vary. They can last from a few seconds to several minutes. In some cases, if not properly treated, they can persist for days or even weeks.
Can back muscle spasms be a sign of a more serious condition?
Yes, back muscle spasms can sometimes indicate a more serious underlying condition, such as a herniated disc, spinal stenosis, or arthritis. It’s important to seek medical evaluation if spasms are severe, recurrent, or accompanied by other symptoms like numbness or weakness.
What are the most effective home remedies for back muscle spasms?
Effective home remedies include applying heat or cold packs, taking over-the-counter pain relievers, staying hydrated, performing gentle stretches, and resting the affected muscles.
When should I see a doctor for back muscle spasms?
You should see a doctor if your back muscle spasms are severe, recurrent, or accompanied by other symptoms like numbness, tingling, or weakness. Additionally, seek medical attention if the spasms do not improve with home remedies within a few days.
Can dehydration really cause back muscle spasms?
Yes, dehydration can lead to an imbalance in electrolytes, which are essential for normal muscle function. This imbalance can cause muscles to contract uncontrollably, leading to spasms.
Are there specific exercises that can help reduce the risk of back muscle spasms?
Yes, exercises that strengthen the core and back muscles, improve flexibility, and promote good posture can help reduce the risk of back muscle spasms. Examples include yoga, Pilates, and specific back-strengthening exercises.
Can stress and anxiety directly cause back muscle spasms?
Yes, stress and anxiety can cause muscle tension and lead to spasms. The body’s stress response releases hormones that can increase muscle tightness and trigger spasms.
What role does nutrition play in preventing back muscle spasms?
Proper nutrition helps maintain a balance of electrolytes and essential minerals like potassium, calcium, and magnesium, which are crucial for muscle function. A balanced diet can help prevent muscle spasms.
Are there any long-term effects of untreated back muscle spasms?
Untreated back muscle spasms can lead to chronic pain, reduced mobility, and muscle weakness. They can also cause compensation in other muscles, potentially leading to additional problems.
Can poor posture cause back muscle spasms even if I'm not lifting heavy objects?
Yes, poor posture can strain the muscles and ligaments in the back, leading to spasms, even without lifting heavy objects. Maintaining good posture is important to prevent muscle strain.
Is it safe to exercise while experiencing a back muscle spasm?
It’s generally recommended to rest the affected muscles and avoid strenuous activities during a spasm. Gentle stretches and low-impact activities may be safe, but it’s best to consult a healthcare professional.
How can I differentiate between a muscle spasm and a more serious back injury?
Muscle spasms often involve sudden tightness and pain but usually improve with rest and home treatments. More serious injuries may involve severe pain, numbness, tingling, or weakness in the legs. If in doubt, seek medical evaluation.
Can sleeping positions affect the likelihood of back muscle spasms?
Yes, sleeping positions that do not support the natural curve of the spine can strain back muscles and lead to spasms. Using a supportive mattress and pillow can help maintain proper alignment.
Are there any specific medications that are particularly effective for back muscle spasms?
Over-the-counter pain relievers like ibuprofen or acetaminophen can be effective. Muscle relaxants may be prescribed for more severe spasms. Always consult a doctor before taking any medication.
How does physical therapy help with back muscle spasms?
Physical therapy helps by improving muscle strength, flexibility, and posture. Therapists can teach specific exercises and stretches that reduce spasms and prevent future occurrences.
Can certain activities or sports increase the risk of back muscle spasms?
Yes, activities and sports that involve repetitive movements, heavy lifting, or sudden twists and turns can increase the risk of back muscle spasms. Proper warm-up and technique are important.
Is it possible for back muscle spasms to cause referred pain in other parts of the body?
Yes, back muscle spasms can sometimes cause referred pain, meaning the pain is felt in another area of the body, such as the hips, legs, or shoulders.
Can massage therapy help with back muscle spasms?
Yes, massage therapy can help relax tight muscles, improve circulation, and reduce pain associated with back muscle spasms.
How does maintaining a healthy weight contribute to preventing back muscle spasms?
Maintaining a healthy weight reduces the strain on your back muscles and spine, lowering the risk of muscle spasms and other back problems.
Are there any specific stretching routines recommended for preventing back muscle spasms?
Yes, routines that include stretches for the hamstrings, hip flexors, and lower back can help prevent spasms. Examples include the child’s pose, knee-to-chest stretch, and the cat-cow stretch.
Can back muscle spasms occur without any physical activity?
Yes, back muscle spasms can occur without physical activity due to factors like poor posture, dehydration, or underlying medical conditions.
How does cold therapy help with back muscle spasms?
Cold therapy helps by numbing the sharp pain, reducing inflammation, and slowing down nerve impulses, which can reduce muscle contractions and spasms.
What is the role of heat therapy in treating back muscle spasms?
Heat therapy helps relax tight muscles, increase blood flow to the affected area, and promote healing by bringing more oxygen and nutrients to the muscles.
Can back muscle spasms be a symptom of fibromyalgia?
Yes, back muscle spasms can be a symptom of fibromyalgia, a condition characterized by widespread muscle pain and tenderness. If you suspect fibromyalgia, consult a healthcare professional for a proper diagnosis.


