The patient is a 67-year-old female with complaints of shooting right leg pain. The pain is described as sharp and severe in character. The pain radiates down from the right buttock to the back of the thigh and leg. The patient reports the pain is associated with numbness and tingling.
Activities such as bending forward, coughing, sneezing, lifting, pushing, sitting make the symptoms worse. The patient previously has tried physical therapy and medications but without any significant relief from symptoms. She is currently on Tylenol and Naproxen for pain.
The patient works as a cab driver and is currently not working secondary to pain. Her past medical history is significant for hypertension, and diabetes mellitus. The patient’s past surgical history is significant for hysterectomy. She denies any known drug allergies and any illicit substance abuse.
The patient is in significant pain and reports an inability to perform day-to-day activities. Physical examination revealed paraspinal tenderness at L4-L5 and a positive right straight leg test at 50 degrees. Power and sensory examination of both the lower extremities was normal. The deep tendon reflexes were symmetrical and equal bilaterally. She does not complain of any weakness or bowel or bladder involvement.
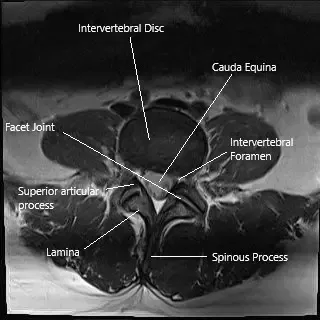
MRI of the lumbar spine in axial section.
MRI examination of the lumbar spine revealed a right S1 nerve compression with multilevel disc degenerative disease. Due to the failure of conservative management, the patient was advised a selective nerve root block. The risks, benefits, and potential complications were all discussed with the patient at length. The patient verbalized agreement and signed the informed consent.
PREOPERATIVE DIAGNOSIS: Right S1 radiculopathy.
POSTOPERATIVE DIAGNOSIS: Right S1 radiculopathy.
OPERATION: Selective nerve root block, right S1.
PROCEDURE: The patient was taken to the endoscopy suite. She was put in prone position. The time-out was called. The right side of the back was prepped and draped aseptically in the usual fashion. Fluoro was brought in. Local was given. A #22 gauge 5-inch needle was introduced and inserted till the right S1 foramen. Finding it in a satisfactory position in AP and lateral view, 0.5 ml of Omnipaque was introduced.
The needle was repositioned but the nervogram could not be produced. On repeat aspiration, blood could be aspirated, so the needle was removed and discarded. A new needle was taken and inserted again. At this time, finding it in a satisfactory position, Omnipaque was again reintroduced and a good nervogram was achieved of the right S1.
The patient was also complaining of pain radiating down the back of this thigh and leg. Then, 1 cc of 40 mg of Kenalog mixed with 1 cc of Sensorcaine was injected into the right S1 foramen. The needle was removed and the Band-Aid was applied. Postop examination revealed good pain relief with no neurological deficit. The patient was instructed to move his leg as well as ambulate and see if the pain can be reproduced. The patient was discharged to home with pain medication.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


