If your spine pain becomes severe enough to hinder daily activities or is accompanied by swelling, tenderness, or redness, it is important to seek medical attention.
At Complete Orthopedics, our expert spine specialists are adept at managing spine pain using both surgical and non-surgical techniques. We analyze symptoms, determine the cause, and propose suitable treatments, including surgery if required.
We provide services to New York City and Long Island, partnering with six hospitals to deliver cutting-edge spine surgery and comprehensive orthopedic care. You can schedule consultations with our orthopedic surgeons either online or by phone.
Learn about the common causes of spine pain and the various treatment options, including situations where surgery might be the best choice.
Overview
Interspinous process spacer decompression surgery is a minimally invasive spine surgery used to treat conditions such as spinal canal stenosis. The surgery involves placing a metallic/plastic spacer in between the spinous process of the adjacent vertebrae. The surgery benefits the patients via decompressing the spinal nerve roots and the thecal sac.
Anatomy of Spine
The spinal cord runs in the vertebral canal and gives numerous branches (spinal nerves) as it travels down the canal. The vertebral canal is formed by the vertebrae stacked upon each other. The lamina creates the vertebral canal’s roof, and the vertebral body forms the floor.
The spinous process is a bony projection at the back of the vertebrae. The projections may be felt under the skin as you run your hand in the lower back’s midline. The spinous processes provide stability and help in the backward movement of the spine.
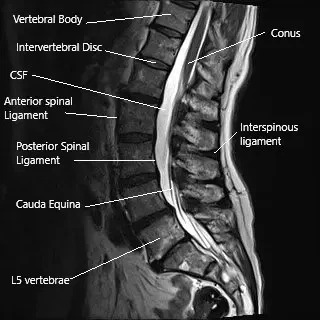
MRI of the lumbar spine showing the interspinous ligament and the spinous process.
Spinal Stenosis
In spinal canal stenosis, the space available for the neural tissues in the vertebral column decreases. Usually, an age-related degenerative process triggers the changes leading to stenosis. The intervertebral disks lose their fluidity with age causing decreased disk height which may result in degeneration of the facet joints that support the adjacent vertebrae.
The facet joint and disk degeneration may cause the formation of bone spurs and thickening of the ligamentum flavum as the body tries to re-align the vertebrae. The bone spurs and thickening of ligaments may narrow the vertebral canal and the neural foramen leading to compression.
The compression of the spinal nerve roots and the dural sac may cause symptoms of radiculopathy and neurogenic claudication. The patients may experience shooting pain down the buttocks, thighs, leg, or feet depending upon the nerve compressed. The pain may accompany numbness and tingling sensation along the region of the involved nerve. In severe cases, there may be a weakness of the muscles of the lower extremities or loss of bowel and bladder control.
Neurogenic Claudication
Symptoms of neurogenic claudication include pain in the buttocks, thighs, groin, or legs on walking. The symptoms get worse on walking downhill and relieved by bending forward. The symptoms occur due to the narrowing of the vertebral canal and the neural foramen on the backward movement of the spine.
As the spine bends backward, the ligamentum flavum buckles to compress the dural sac, and the capsule of the facet joints press on the neural foramen. The resulting compression of the dural sac and spinal nerves may cause symptoms due to decreased blood supply to the involved nerves.
Management
The initial treatment of spinal stenosis is conservative that may involve the use of physical therapy, pain medications, alternative medicine, and epidural/nerve block injections in the spine. The patients who have not benefited from conservative treatments for six months may be candidates for decompression surgery.
Laminectomy
Lumbar decompression surgeries usually involve removing bony or soft tissue structures to widen the vertebral or the neural foramen. Laminectomy, laminotomy, or laminoplasty are the surgeries usually performed to decompress the involved segment. The surgery may be accompanied by lumbar fusion surgery to provide rigid stabilization to the spine.
Interspinous Process Spacer
Interspinous process spacer surgery decompresses the involved segment with dynamic stabilization. The surgery is usually performed with a minimally invasive technique that involves tiny incisions at the back.
A local or general anesthesia may be given to the patient to numb the involved area. Under fluoroscopic guidance, the surgeon introduces small tubes to reach the interspinous area and gradually introduces increasing diameters of tubes to separate the tissues. The spacer is then introduced through the tubes and turned to its proper position. The incision is then closed in layers, and the skin incision is closed with one or two sutures.
Benefits of Interspinous Process Spacer
Interspinous process spacer limits the backward bending of the spine. The symptoms of canal stenosis and neurogenic claudication are position-dependent. The backward motion of the spine exacerbated the symptoms. The spacers prevent the backward movement and thus result in relief of symptoms.
The rigid fixation offered by fusion surgeries often results in limitation of motion of the spine. The interspinous process spacers do dynamic stabilization by allowing limited forward bending, side bending, and twisting movement.
The surgery also allows the patients to go home the same day of the surgery. The majority of the interspinous process spacers may be inserted in an outpatient setting. There is little postoperative pain as the incisions used are very small. The back muscles are also separated and not cut as compared to the traditional fusion surgeries.
The distraction of the spinous processes leads to the opening of the neural foramen, thus alleviating canal stenosis symptoms. The decompression achieved is dynamic as opposed to lumbar fusion surgery.
Potential complications
Being a minimally invasive surgery, the risks of complications is minimal, but there may be potential complications associated with interspinous process spacers. The spacer may dislodge and move out of its place. The interspinous process spacer may break or fracture the spinous process. There may be inadequate relief of symptoms, or additional surgery may be needed.
Contraindications
The interspinous process spacers are not indicated in patients with motor and sensory weakness associated with nerve compression. The patients with bowel and bladder incontinence who may have cauda equina syndrome are not candidates for spacers as they may require immediate open decompression. Also, patients with spine infection and osteoporosis are not candidates for interspinous process spacer.
Do you have more questions?
What exactly is an interspinous process spacer?
An interspinous process spacer is a small device made of metal or plastic that is inserted between the spinous processes of the vertebrae to keep them apart and relieve pressure on the spinal cord and nerves.
Is the procedure painful?
The procedure is minimally invasive and typically performed under local or general anesthesia, so patients should not feel pain during the surgery. Postoperative pain is usually minimal due to the small incisions used.
How does the spacer relieve spinal stenosis symptoms?
The spacer limits the backward bending of the spine, which exacerbates spinal stenosis symptoms. By maintaining space between the vertebrae, it reduces pressure on the spinal cord and nerves, alleviating pain and discomfort.
What is the recovery time after the surgery?
Most patients can go home the same day of the surgery. Recovery time is generally shorter compared to traditional fusion surgeries, with many patients returning to normal activities within a few weeks.
Are there any risks associated with the surgery?
As with any surgery, there are risks, including infection, bleeding, and potential complications related to the spacer, such as dislodgement or breakage. However, the overall risk is lower compared to more invasive procedures.
Can the spacer move or dislodge after surgery?
While it is rare, there is a possibility that the spacer can move or dislodge. Proper surgical technique and postoperative care can minimize this risk.
Are there any risks associated with the surgery?
As with any surgery, there are risks, including infection, bleeding, and potential complications related to the spacer, such as dislodgement or breakage. However, the overall risk is lower compared to more invasive procedures.
What are the main benefits of choosing this surgery over traditional fusion surgery?
The main benefits include shorter recovery time, minimal postoperative pain, preservation of spinal mobility, and a lower risk of complications.
Who is a good candidate for this surgery?
Good candidates are patients with lumbar spinal stenosis who have not found relief from conservative treatments. Candidates should not have significant motor or sensory weakness, bowel or bladder incontinence, spine infections, or severe osteoporosis.
Are there any conditions that would prevent a patient from having this surgery?
Yes, patients with motor and sensory weakness due to nerve compression, bowel or bladder incontinence, spine infections, or osteoporosis are generally not candidates for this surgery.
How long does the surgery take?
The procedure typically takes about 1-2 hours, depending on the specific circumstances and the surgeon’s experience.
Will I need to wear a brace after surgery?
Most patients do not need to wear a brace after surgery. However, some surgeons may recommend a brace for additional support during the initial recovery period.
What kind of anesthesia is used for this procedure?
The procedure can be performed under local or general anesthesia, depending on the patient’s health, preferences, and the surgeon’s recommendation.
How soon can I return to work after the surgery?
Many patients can return to light work within a few days to a week. Those with more physically demanding jobs may need a longer recovery period.
What activities should I avoid after surgery?
Patients should avoid heavy lifting, strenuous activities, and excessive bending or twisting during the initial recovery period. Your surgeon will provide specific guidelines based on your condition.
Will I need physical therapy after surgery?
Physical therapy may be recommended to help strengthen the back muscles and improve flexibility. The need for physical therapy varies from patient to patient.
Can the spacer be removed if it doesn’t work?
Yes, if the spacer does not provide the desired relief or causes complications, it can be removed, and alternative treatments can be considered.
Is this procedure covered by insurance?
Coverage varies by insurance provider and policy. It is important to check with your insurance company to determine if the procedure is covered.
What should I expect during the postoperative period?
You can expect some discomfort and mild pain, which can be managed with medications. Follow-up appointments with your surgeon will monitor your progress and ensure proper healing.
How does this surgery compare to other minimally invasive procedures?
This surgery offers dynamic stabilization and preservation of spinal motion, which is an advantage over some other minimally invasive procedures that may result in more rigid fixation.
Can the spacer treat other conditions besides spinal stenosis?
The primary indication for interspinous process spacers is lumbar spinal stenosis. It is not typically used for other spinal conditions.
Will I need any special imaging tests before the surgery?
Yes, imaging tests such as MRI or CT scans are essential to evaluate the spine’s condition and plan the surgery accurately.
Can this surgery be performed on multiple levels of the spine?
Yes, the surgery can be performed on multiple levels if necessary, but this depends on the specific condition and extent of stenosis.
What are the long-term outcomes of the surgery?
Long-term outcomes are generally positive, with many patients experiencing sustained symptom relief. Regular follow-up is important to monitor for any potential issues.
What should I do if my symptoms return after surgery?
If symptoms return, it is important to consult your surgeon. Additional treatments or interventions may be necessary depending on the cause of the recurrent symptoms.


