Flatback Syndrome
If spine pain worsens, interferes with daily activities, or is accompanied by swelling and redness, it’s crucial to consult a healthcare professional. At Complete Orthopedics, our expert team specializes in addressing spine issues through customized treatment plans and surgical options. We prioritize understanding your symptoms, identifying the underlying causes, and recommending the most suitable treatments or surgeries.
Our clinics are conveniently located throughout New York City and Long Island, and we collaborate with six leading hospitals to ensure you receive the highest quality care for spine issues. Schedule an appointment with one of our orthopedic surgeons online or by phone. Learn about the causes and treatments for spine pain and determine when surgery might be necessary.
Overview
The straightening of the normal lumbar lordosis is known as a flatback syndrome. The condition may affect patients who had prior spine surgeries or suffer from degenerative spine conditions. Flatback syndrome results in back pain, difficulty walking and standing straight. The management of flatback syndrome involves the use of conservative measures and in some patients, surgical correction may be needed.
The human spine consists of 24 vertebrae stacked upon each other to form the vertebral column. The vertebral column provides a safe conduit for the spinal cord and the numerous spinal nerves branching from the spinal cord. Each vertebra joins the adjoining vertebrae through facet joints and the intervertebral discs.
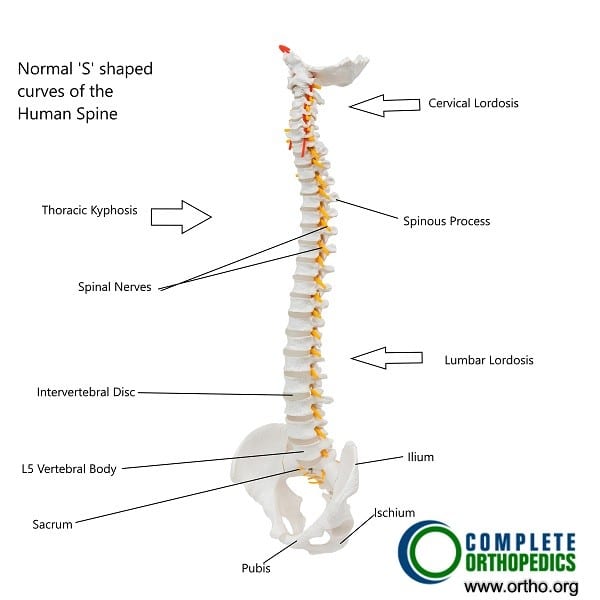
Natural curves in the human spine.
The natural vertebral column is curved in an ‘S’ shape. The neck spine is curved inwards, the thoracic spine is curved backward and the lumbar spine is curved inwards. The natural curves in the spine function to keep the center of gravity of the spine in line with the pelvis and the legs. The natural alignment thus functions to maintain the balance of the body in activities such as standing, walking, etc.
In flatback syndrome, the natural inward curve of the spine is lost and the lumbar spine is straight. The resulting alignment shifts the balance of the spine forward and causes the symptoms associated with the flatback syndrome.
Symptoms of Flatback Syndrome
The symptoms of flatback syndrome can vary in severity but generally include:
Difficulty Standing Upright: One of the hallmark symptoms of flatback syndrome is the inability to stand up straight without discomfort. Individuals often feel like they are leaning forward.
Lower Back Pain: Chronic pain in the lower back is common due to the abnormal posture and strain on the muscles and ligaments.
Fatigue: Because the spine is not properly aligned, the muscles have to work harder to maintain balance, leading to fatigue, especially after standing or walking for extended periods.
Pain in the Legs: Some people with flatback syndrome experience pain that radiates down into the legs. This is often due to nerve compression or irritation.
Restricted Mobility: The loss of the natural curve can limit the spine’s flexibility, making it difficult to perform everyday activities.
Patients with flatback syndrome find it difficult to stand straight as the center of gravity shifts forward. The patients report a feeling of falling forward on walking or standing. Initially to compensate for the altered balance of the spine the patients may often bend their hips and their knees to stand straight. The back muscles contract to pull the spine back to stand straight.
Bending of the knees and hips along with constantly contracted back muscles, results in severe pain in the back and the legs. The patients may feel tired and fatigued and stoop while walking especially at the end of the day. They may use an assistive device in the form of a cane or a walker to support the body falling forward on walking.
Causes
Often patients who receive surgical treatment for scoliosis with a fusion of multiple segments end up with a flatback syndrome due to loss of natural curve. Patients having a prior surgical history of fusion of the lumbar spine or laminectomy of the lumbar spine may also develop the flat back syndrome.
Besides the history of prior surgery, the flatback syndrome may be present in certain patients due to a developmental deformity or they may be born with the condition (congenital). Patients suffering from ankylosing spondylitis in the advanced stage of disease may develop the flatback syndrome. The lumbar spine in ankylosing spondylitis becomes fused due to the ossification of ligaments and the formation of bridging syndesmophytes.
With advancing age, there may be a loss of disc height secondary to the decreased water content of the intervertebral disc and lead to degenerative changes in the vertebra. This results in loss of the natural lordotic curve of the lumbar spine that may cause the flatback syndrome. In patients with metabolic bone disease such as osteoporosis, there may be compression fractures of the vertebrae that may disturb the natural alignment of the spine and cause flatback syndrome.
Diagnosis
The diagnosis of flatback syndrome is made by the orthopedic spine surgeon after a thorough evaluation of the patient. The evaluation consists of extraction of the history of symptoms and any prior surgical procedures. The physician conducts a thorough examination of the spine to look for the alignment and the gait of the patient. The physician also checks for the integrity of the neurological system.
The physician may request a full-length X-ray to check for the alignment of the spine. CT scan may be done for further evaluation of the bony spine and an MRI may be done to look for the soft tissue structures of the spine.
Treatment
The flatback syndrome is initially managed using conservative treatment options. The conservative treatment options include physical therapy to strengthen and improve the flexibility of the back and the abdominal muscles. Gait training is done to help form a correct posture during walking.
Nonsteroidal anti-inflammatory medications and other pain medications such as Tylenol may be used to relieve the pain associated with the flatback syndrome. Heat and cold therapy may be used to reduce pain and inflammation of the lumbar spine. Epidural and nerve block injections may be used to provide pain relief and symptoms of radiculopathy.
Surgical Treatments:
- Spinal Fusion Revision: If flatback syndrome is the result of a previous spinal fusion surgery, a revision surgery might be necessary to restore the normal curvature of the spine.
- Osteotomy: This is a surgical procedure where a section of bone is removed to correct the alignment of the spine.
- Decompression Surgery: If there is nerve compression contributing to pain, decompression surgery can relieve the pressure on the nerves.
Surgery is reserved for patients who have failed to benefit from conservative measures. The surgical treatment of flatback syndrome involves correction of the lumbar curve to align the spine. A spinal osteotomy and pedicle subtraction surgery involve cutting a wedge-shaped part of the lumbar spine to make a natural curve. The surgery usually involves the fusion of the involved vertebrae using a cage and a bone graft. The fused segment is stabilized using a screw and a rod construct on either side of the midline.
The patients treated with surgical correction techniques experience significant relief of symptoms and are quickly able to get back to their daily routines. As with any surgery, there may be risks and complications associated with corrective surgery such as bleeding, infection, blood clot formation, failure of fusion, damage to nerves/dural sac, etc. The operating spine surgeon will discuss all the potential benefits and risks before doing the surgery.
Living with Flatback Syndrome
Living with flatback syndrome can be challenging, but there are ways to manage the condition and improve your quality of life. Here are some tips:
Stay Active: Regular exercise, especially activities that strengthen the core and improve flexibility, can help manage symptoms.
Maintain a Healthy Weight: Excess weight can put additional strain on the spine, so maintaining a healthy weight is important.
Use Proper Posture: Being mindful of your posture while sitting, standing, and lifting can help prevent further strain on the spine.
Follow Your Treatment Plan: Adhering to the treatment plan prescribed by your healthcare provider, including physical therapy and medication, is crucial for managing symptoms.
Seek Support: Joining a support group or seeking counseling can help you cope with the emotional aspects of living with a chronic condition.
Conclusion
Flatback syndrome is a condition that affects the natural curvature of the spine, leading to a forward-leaning posture and various symptoms like back pain and difficulty standing upright. It can result from degenerative disc disease, previous spinal surgeries, certain spinal conditions, or poor posture. Diagnosis typically involves a combination of medical history, physical examination, and imaging tests. Treatment options range from non-surgical methods like physical therapy and pain management to surgical interventions to correct the spine’s alignment. Living with flatback syndrome requires a combination of medical management, lifestyle adjustments, and support to improve quality of life.
Do you have more questions?
What is flatback syndrome?
Flatback syndrome is a condition where the natural inward curve of the lower spine (lordosis) is lost, resulting in a spine that appears flat and causing a forward-leaning posture.
What are the symptoms of flatback syndrome?
Symptoms include difficulty standing upright, lower back pain, fatigue, pain in the legs, and restricted mobility.
What causes flatback syndrome?
It can be caused by degenerative disc disease, previous spinal surgeries (especially spinal fusions), conditions like Scheuermann’s kyphosis or ankylosing spondylitis, and poor posture over time.
When is surgery necessary for flatback syndrome?
Surgery may be necessary if non-surgical treatments fail to relieve symptoms, if there is significant spinal deformity, or if there is nerve compression causing severe pain or functional impairment.
What are the non-surgical treatment options for flatback syndrome?
Non-surgical treatments include physical therapy, pain management with medications, and sometimes wearing a brace to support the spine.
What surgical options are available for flatback syndrome?
Surgical options include spinal fusion revision, osteotomy (removal of a bone section to correct alignment), and decompression surgery to relieve nerve pressure.
Can flatback syndrome be prevented?
While not all cases can be prevented, maintaining good posture, staying active, managing weight, and avoiding unnecessary spinal surgeries can reduce the risk.
Can flatback syndrome worsen over time?
Yes, without appropriate treatment and management, the condition can worsen, leading to increased pain and disability.
Is flatback syndrome common?
It is relatively uncommon, often seen as a complication of previous spinal surgeries or specific spinal conditions.
How effective is physical therapy for flatback syndrome?
Physical therapy can be very effective in strengthening the muscles that support the spine, improving posture, and reducing pain.
Are there any risks associated with surgery for flatback syndrome?
As with any surgery, risks include infection, bleeding, nerve damage, and complications related to anesthesia. There is also a risk of the surgery not fully correcting the deformity or relieving symptoms.
What types of exercises are recommended for flatback syndrome?
Core strengthening exercises, stretching, and activities that promote good posture are recommended.
How long is the recovery period after surgery for flatback syndrome?
Recovery can take several months. The initial hospital stay might be a few days to a week, followed by a period of rehabilitation and gradual return to normal activities.
What is the prognosis for someone with flatback syndrome?
With appropriate treatment, many people can manage their symptoms effectively and maintain a good quality of life. Surgical correction can significantly improve posture and reduce pain.
Can flatback syndrome lead to other health problems?
If left untreated, it can lead to chronic pain, reduced mobility, and an increased risk of falls and other injuries due to the altered posture.
Can flatback syndrome recur after treatment?
Recurrence is possible, especially if the underlying causes are not fully addressed or if there is degeneration in other parts of the spine.
Can children develop flatback syndrome?
It is more common in adults, especially those with a history of spinal surgery or specific spinal conditions. However, children with conditions like Scheuermann’s kyphosis could potentially develop it.
Is flatback syndrome the same as scoliosis?
No, scoliosis involves a sideways curvature of the spine, whereas flatback syndrome involves a loss of the normal inward curvature of the lower spine.
How does flatback syndrome affect daily activities?
It can make standing and walking for long periods difficult, cause chronic pain, and lead to fatigue, impacting overall mobility and quality of life.
What lifestyle changes can help manage flatback syndrome?
Maintaining a healthy weight, staying active with appropriate exercises, using proper posture, and following a treatment plan can help manage symptoms.
Are there any supportive devices that can help with flatback syndrome?
Braces can sometimes be used to support the spine and improve posture. Additionally, ergonomic furniture and supportive shoes can help reduce strain.
How does flatback syndrome affect sleep?
Chronic pain and discomfort can interfere with sleep. Finding a comfortable sleeping position and using supportive mattresses and pillows can help improve sleep quality.
What role do diet and nutrition play in managing flatback syndrome?
A balanced diet that supports overall health, including bone and muscle health, can be beneficial. Maintaining a healthy weight is particularly important to reduce strain on the spine.
Can alternative therapies help with flatback syndrome?
Some individuals find relief through alternative therapies like chiropractic care, acupuncture, or massage, but these should be used in conjunction with conventional treatments and under the guidance of a healthcare professional.

Dr. Suhirad Khokhar
My name is Dr. Suhirad Khokhar, and am an orthopaedic surgeon. I completed my MBBS (Bachelor of Medicine & Bachelor of Surgery) at Govt. Medical College, Patiala, India.
I specialize in musculoskeletal disorders and their management, and have personally approved of and written this content.
My profile page has all of my educational information, work experience, and all the pages on this site that I've contributed to.
