This Patient presented to our outpatient clinic with signs and symptoms of lumbar stenosis and spondylotic radiculopathy as well as epidural lipomatosis. They failed extensively with non surgical treatments, which were unsuccessful in alleviating their symptoms. Imaging demonstrated the above mentioned issue.
Surgery was recommended to decompress their lumbosacral spine. The risks, benefits, alternatives and potential complications of the surgery were explained to them. All questions were answered until no further issues were raised and they provided written informed consent which was placed in the chart.

The patient was brought to the operating room. Their identity was verified. General anesthesia was induced, and they were intubated by the Anesthesia Service. Respiratory and cardiac monitoring leads were placed. They received preoperative prophylactic IV antibiotics.
They were positioned prone on a Wilson frame. All pressure points were carefully padded. Lumbar area was prepped with electric hair clipper, cleaned with chlorhexidine, and sterilized with DuraPrep solution.
Spinal needle and fluoroscopy were used to localize the L5-S1 level. A midline incision was demarcated. Skin was sterilized with DuraPrep. Sterile drapes were placed in usual manner. 1% lidocaine with epinephrine was infused.
Skin was opened with #10 blade scalpel. Hemostasis was obtained with bipolar. Bovie monopolar and Cobb elevators were used to carry the incision down, incising the fascia and performing subperiosteal dissection exposing the L4, L5 and S1. Self-retaining retractors were placed. A Woodson elevator was placed under the L4 lamina. C-arm unit, which was draped sterilely, was brought into the field and used to confirm the level.
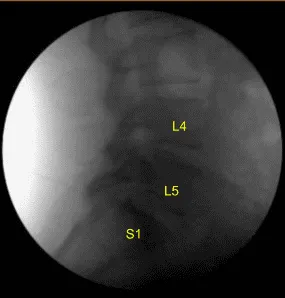
L4, L5 and S1 spinous processes were resected with Horsley rib cutters and Leksell rongeurs. Bone bleeding was controlled with bone wax. Electric high-speed drill with sterile irrigation was used to perform L4, L5 and S1 laminectomy. This was continued with Kerrison rongeurs, carefully protecting the dura. No cerebrospinal fluid or durotomy was identified.
Hypertrophied ligamentum flavum was resected at L4 and L5. Significant epidural lipomatosis similar to preoperative imaging was identified at L5-S1. Lateral recess at L4, L5 and S1 was decompressed with Kerrison rongeurs. Decompression was confirmed with nerve hooks and Woodson elevators. Bilateral L4, L5 and S1 nerve roots were completely neurolyzed with Metzenbaum-Penfield technique and confirmed with nerve hooks.
Epidural fat was gently resected with bayonets, Woodson elevator and coagulated with bipolar electrocautery. The laminectomy was continued in a caudal direction including full S1 laminectomy until the sacral nerves were completely decompressed in the midline and confirmed with the Woodson elevator. Hemostasis was confirmed.
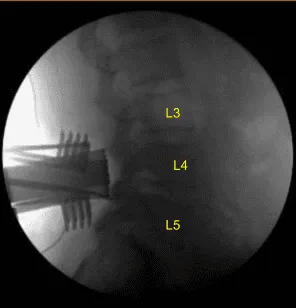
The wound was irrigated copiously. A medium size Hemovac drain was tunneled in a subfascial manner and secured to the skin with 3-0 nylon suture. The fascia was closed in a watertight manner with interrupted 0 Vicryl sutures. Exparel long-acting local anesthetic was infused into soft tissues.
The subdermal layer was closed with interrupted 2-0 Vicryl sutures. The skin was reapproximated with running 4-0 subcuticular stitch, then cleaned, dried sterilely, and dressed with Dermabond glue. Hemovac canister was applied to suction.
The patient was then turned supine on the cart, extubated uneventfully and transported to the recovery room in stable condition. At the end of the case, all sponge counts, needle counts, and instrument counts were correct. The patient tolerated the procedure well.
The patient followed up two weeks after the surgery and then continued to follow up in a periodical manner. In their last office visit the patient showed signs of improvement with spondylotic radiculopathy. They also stated they had begun to perform their usual activities at home.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


