The patient is a 49 yr old female, with complaints lower back pain and right leg pain. The patient remembers injury to her lower back a year ago while she was picking up her mother who fell. She states she heard a pop on the right side of the back, went to the hospital had an MRI which shows a herniated disc/bulging disc.
The pain is extremely severe in intensity. The patient describes the pain as sharp, aching, and burning in the lower back. The pain is constant and disturbs her sleep. The pain is associated with swelling, numbness (in the right foot dorsally and on the sole), radiating pain down the leg (along the back and side of the thigh and leg).
The patient takes over the counter pain medications and the pain has improved since it started. Activities such as walking, standing, and using the stairs made the symptoms worse. The patient has been limping and walks with the body tilted to the left. She got a Medrol dose pack which helped for a few days.
The patient is right-handed. She is a police officer and has returned back to work. She had earlier tried conservative management in the form of physical therapy, heat, and cold therapy. Her past medical history is positive for Hypothyroidism and Hypertension, both conditions under good control with medications. She is a nonsmoker and teetotaller and denies any known drug allergies.
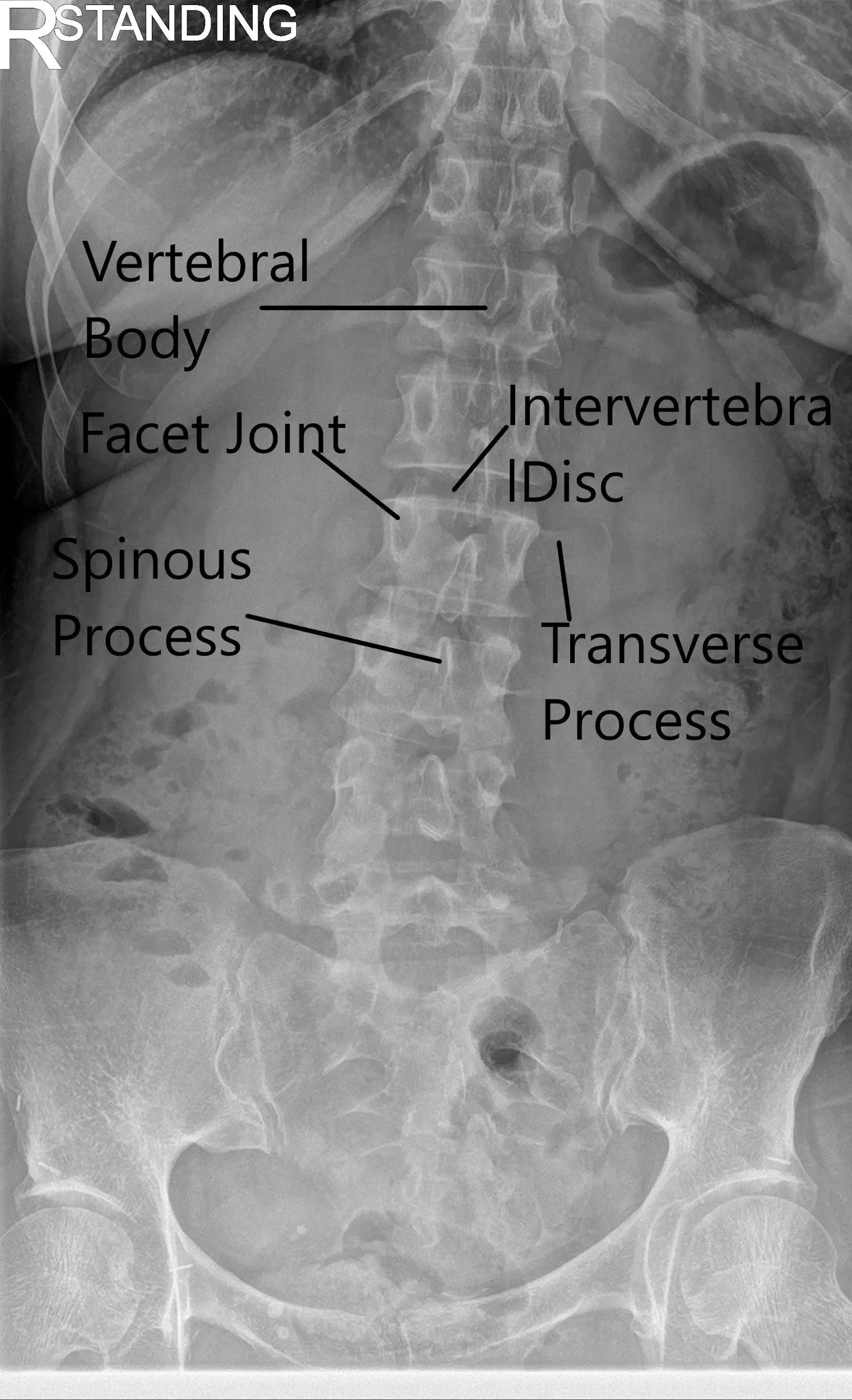
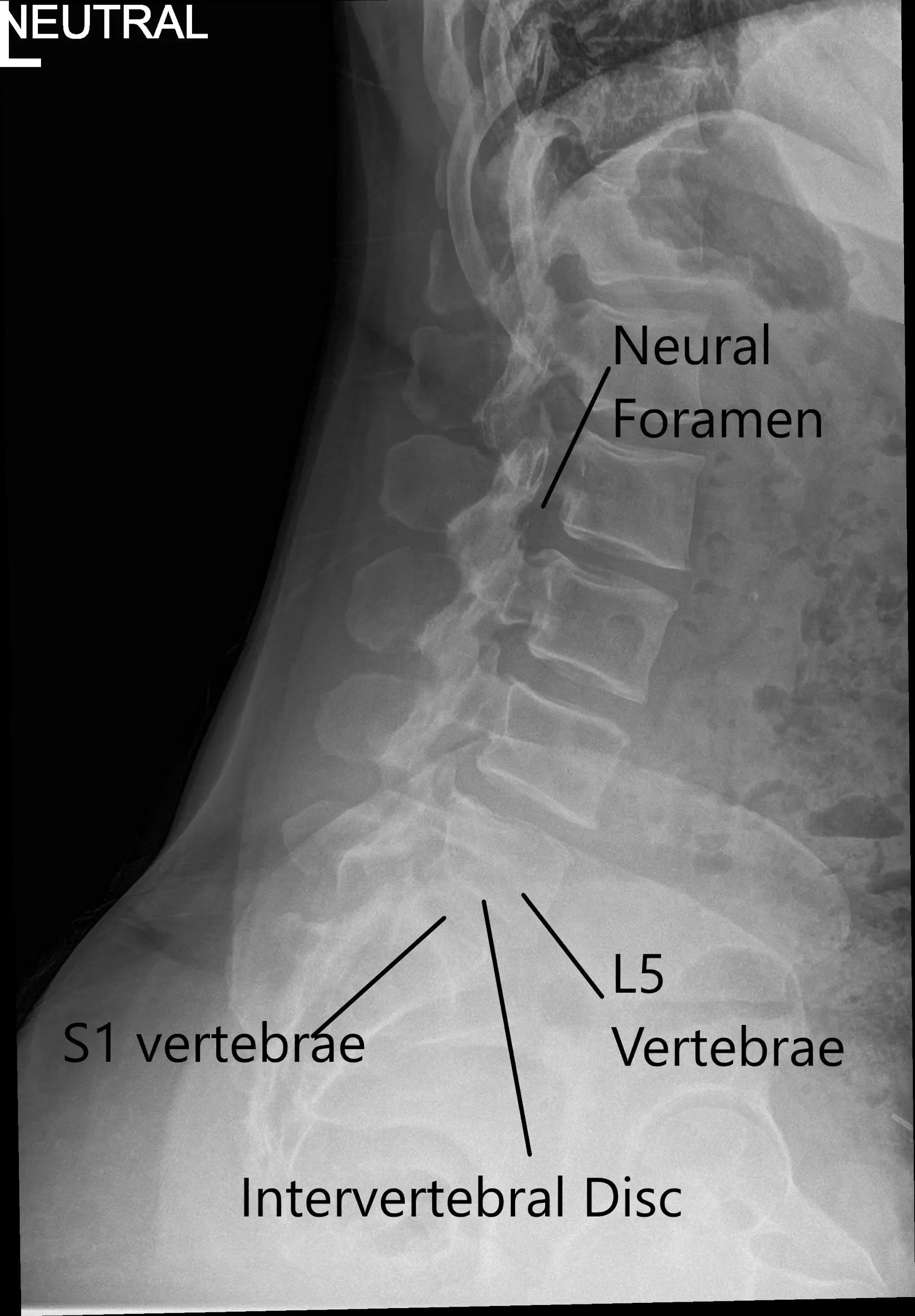
X-ray of the LS spine in AP and Lateral views showing degenerative changes.
The patient was calm, conscious, cooperative, and well oriented to time, place, and person. Upon examination of the lumbar spine, the patient was tender to palpation over the right paraspinal musculature. The patient stands with a list to the left and forward bending. There is no tenderness over the spinous processes and there is no crepitus with ranging.
The range of motion of the lumbar spine was limited secondary due to discomfort. The straight leg raise test was positive on the right side. Extension of the spine was painful and causes radiculopathy.
There was no tenderness on palpation over the trochanteric bursa and hip. There was no soft tissue swelling and ecchymosis. The patient has a full range of motion of the hips. The hips are stable on the examination. Both the lower extremities have 5/5 strength and are neurovascularly intact distally. There are no erythema, warmth, or skin lesions present.
The patient was advised of a transforaminal lumbar epidural injection. Risks, benefits, and alternatives were discussed with the patient at length, The patient agreed with the plan.
PREOPERATIVE DIAGNOSIS: Radiculopathy of right L5/S1.
OPERATION: Transforaminal epidural steroid injection right L5 and right S1.
DESCRIPTION OF THE PROCEDURE: The patient was seen in the preoperative area, where we discussed the risks and benefits and complications including no or incomplete or sort lasting benefit, injury to adjacent nerve or vessel, bleeding, injection, worsening of pain. The patient agreed and signed informed consent. The patient was taken to the operating room where she was placed prone on a well-padded operating table. Sedation was given to alleviate her pain. A time-out was called and the correct patient, correct side, and correct procedure were identified.
After aseptic prep and drape under C-arm, the needle was introduced to reach the level of the L5-S1 foramen. It was checked under C-arm and found to be in the satisfactory position in AP and lateral view; 0.5 cc of iodine dye was introduced and found to form a good nervogram; 40 mg of Kenalog mixed with 1 cc of 0.5% Marcaine was introduced into the L5 nerve root sheath on the right side.
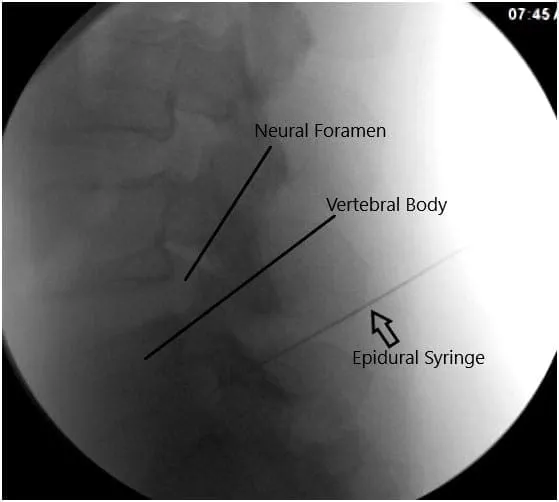
Intraoperative Fluoroscopy Images.
The patient was on light sedation and was asked about the pain relief. She states there was around 40% pain relief. So, we decided to continue with the injection onto the right S1.
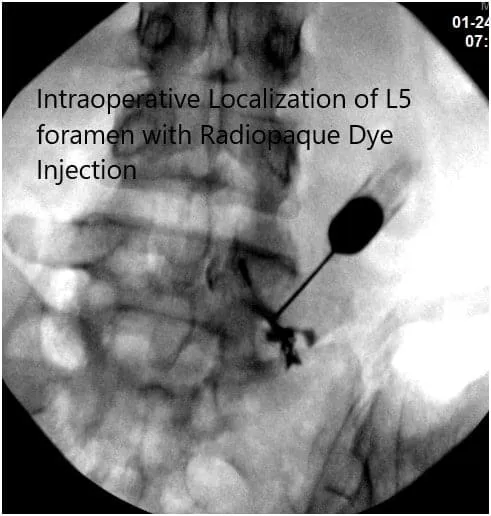
Intraoperative Fluoroscopy Images.
The needle was again re-directed towards the right S1 foramen. It was checked under C-arm and found to be in a satisfactory position. 0.5 cc of Iodine dye was introduced and found to make a good nervogram; 40 mg of Kenalog mixed with 1 cc of 0.5% Marcaine was injected into the right S1 nerve root sheath. The needle was removed. The patient was asked about pain relief and she had near 100% pain relief.
The patient was laid supine into a bed and moved to the postoperative care unit in a stable condition.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


