A retired bank manager presented to our office with complaints of bilateral knee pain. She first noticed the pain a few years back but was unable to localize the exact time of onset. She stated the pain was insidious in onset and progressed gradually with some good days and some bad days.
The pain was located diffusely within both the knees and was a dull aching in character. The pain was especially worse on prolonged walking, standing and activities which involved sitting, squatting, turning, twisting and climbing stairs. She was unable to do daily activities such as cooking, doing laundry or going up the stairs.
She previously had a meniscal surgery on her right knee with only relief for a couple of months. She also received hyaluronic gel injections in both knees but with minimal relief. She tried physical therapy and hot-cold treatment, with no relief.
She was currently living with her family and was distressed with the worsening knee pain. She was unable to socialize with her family and relatives. She was a nonsmoker and a nondrinker. Her past medical history was positive for diabetes mellitus, hypertension, and asthma. All her medical conditions were well controlled with medications.
On physical examination, there was genu varum deformity in both knees. Her gait was steady and well-coordinated using cane as an assistive device. The skin overlying both the knees was normal. There was no evidence of any swelling in both knees.
On palpation, tenderness was present on bilateral joint lines and patellar facets. The range of motion of both knees was painful with restricted end movements. There was crepitus in both the knees joints on motion. The range of motion of the right knee was from 5 degrees to 110 degrees and that of the left was 0 degrees to 110 degrees.
The examination of the bilateral hip and ankle was normal. There was no evidence of distal neurological deficit. Bilateral lower extremity pulses were palpable and comparable. The lower extremity deep tendon reflexes were illustrated and comparable bilaterally.
Her imaging studies of both the knee revealed severe tricompartmental osteoarthritis. Considering her lifestyle limiting knee pain, she was advised bilateral custom total knee replacement. Risks, benefits, and alternatives were discussed with the patient at length. She agreed to go ahead with a bilateral custom knee replacement.
A few weeks prior to the procedure, a CT scan of both knees, ankles, and hips was obtained. The data was utilized to form 3D images of the patient’s knees. Unique customized patient-specific implants were constructed along with disposable bone cutting jigs. A unique preoperative plan was formed suggesting bone cuts and femoral offsets.
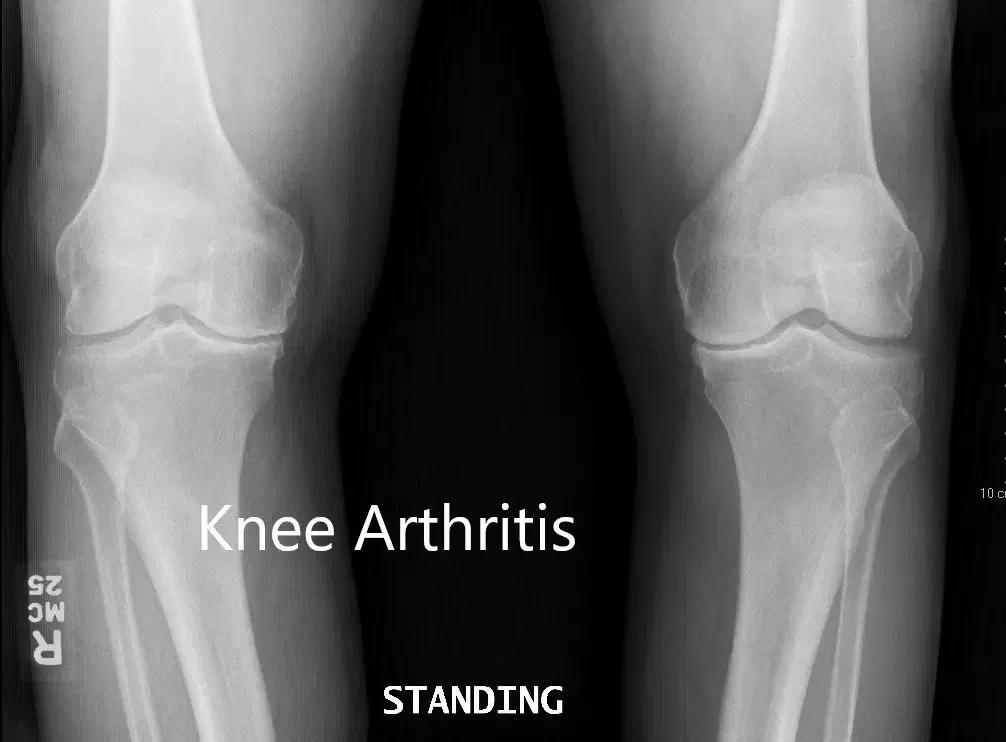
Preoperative X-ray showing the AP view of both knees.
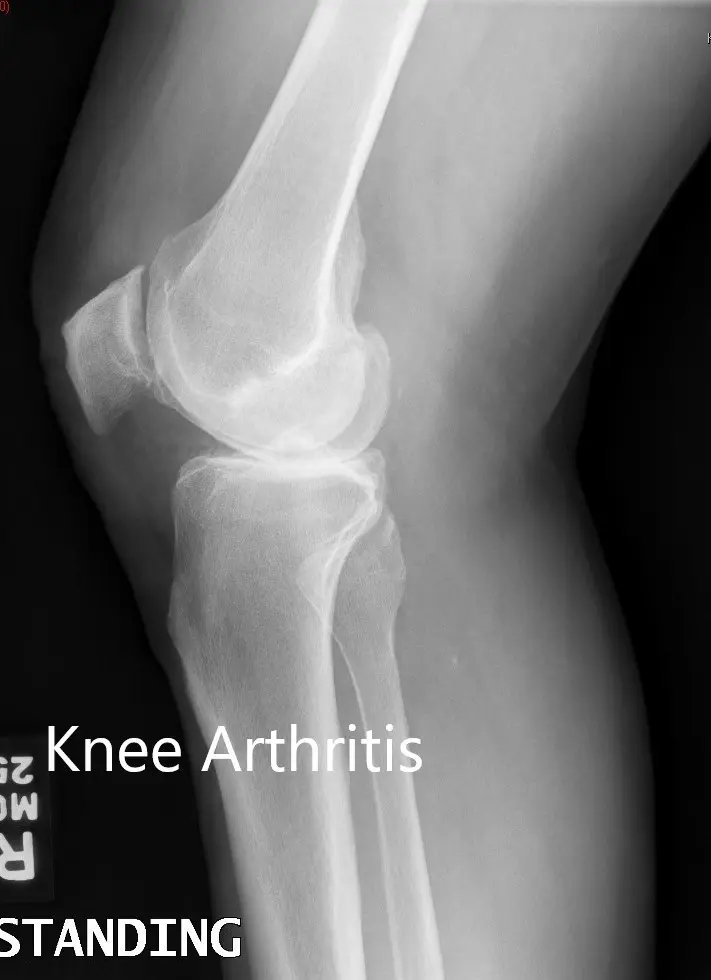
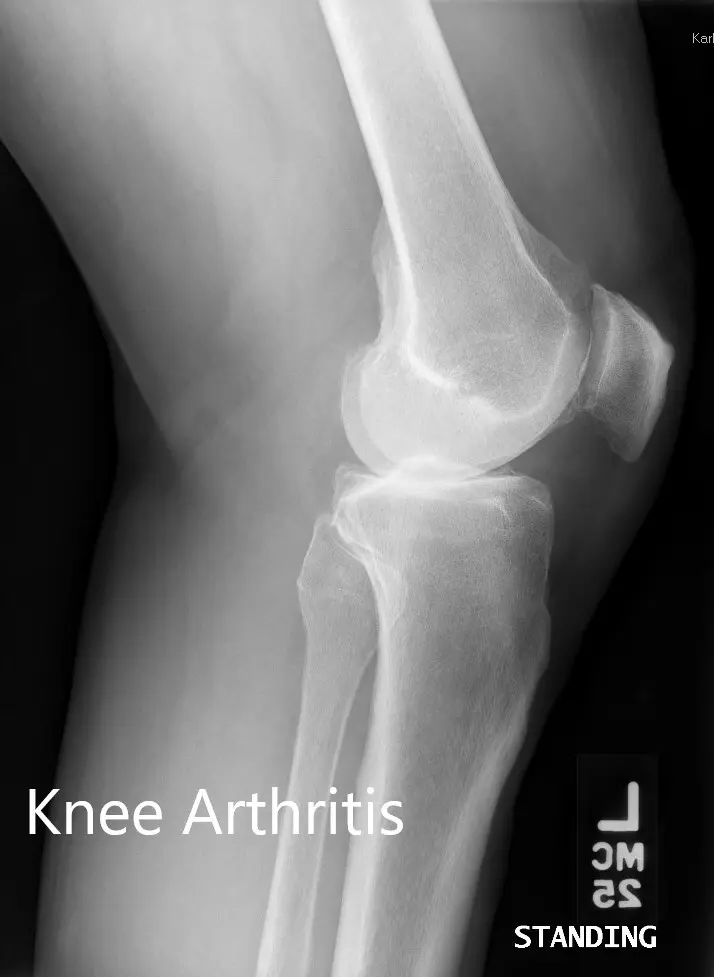
Preoperative X-ray showing the lateral views of the right and the left knee respectively.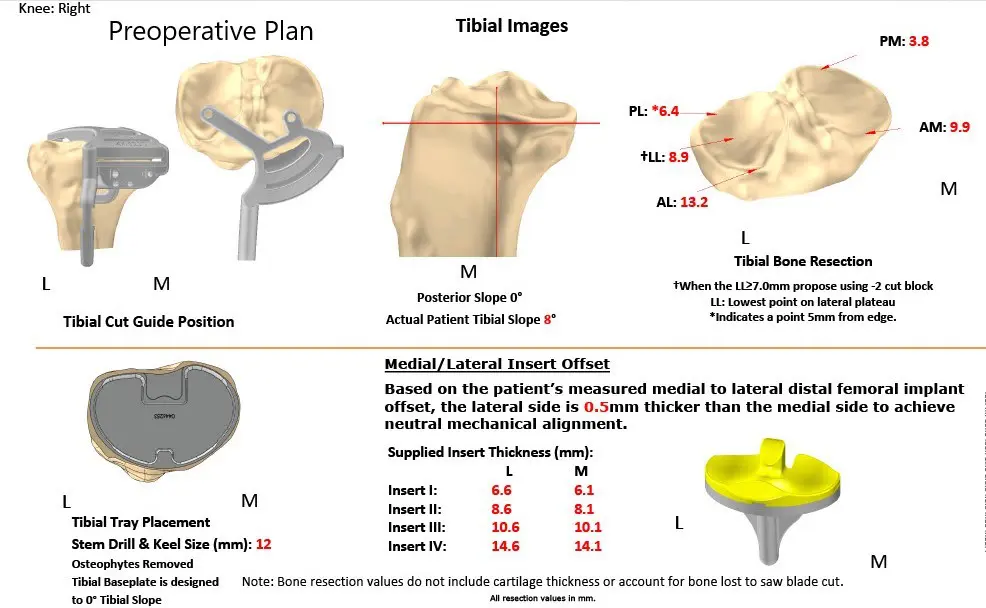
Complete Orthopedics patient-specific surgical plan for a bilateral customized total knee replacement in a 72-year-old patient with arthritis.
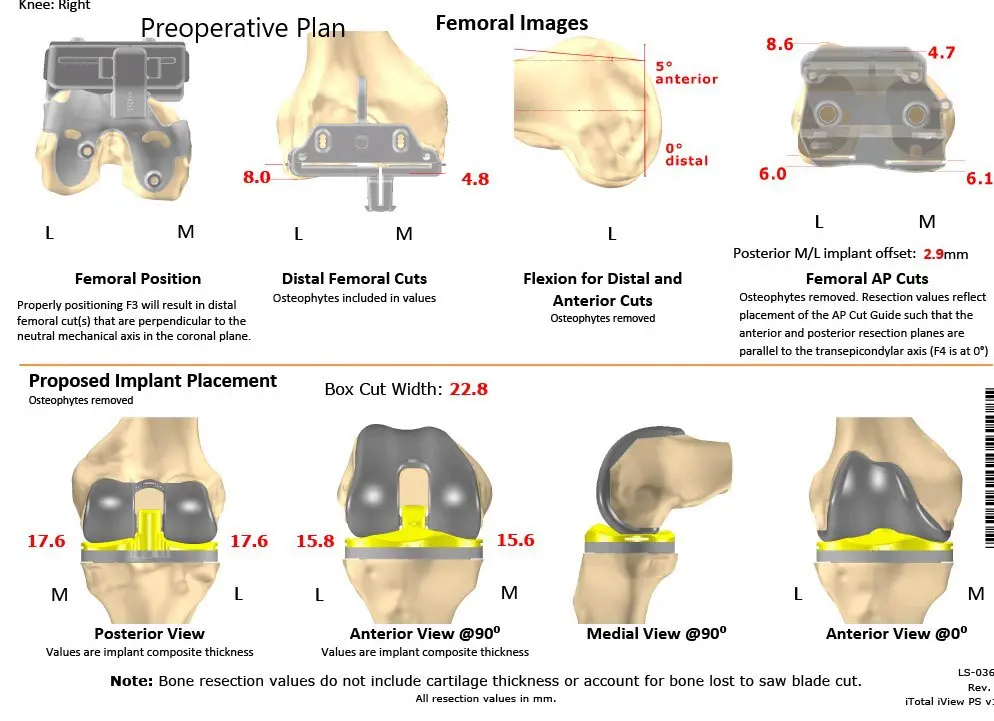
Complete Orthopedics patient-specific surgical plan for a bilateral customized total knee replacement in a 72-year-old patient with arthritis (scan 2)
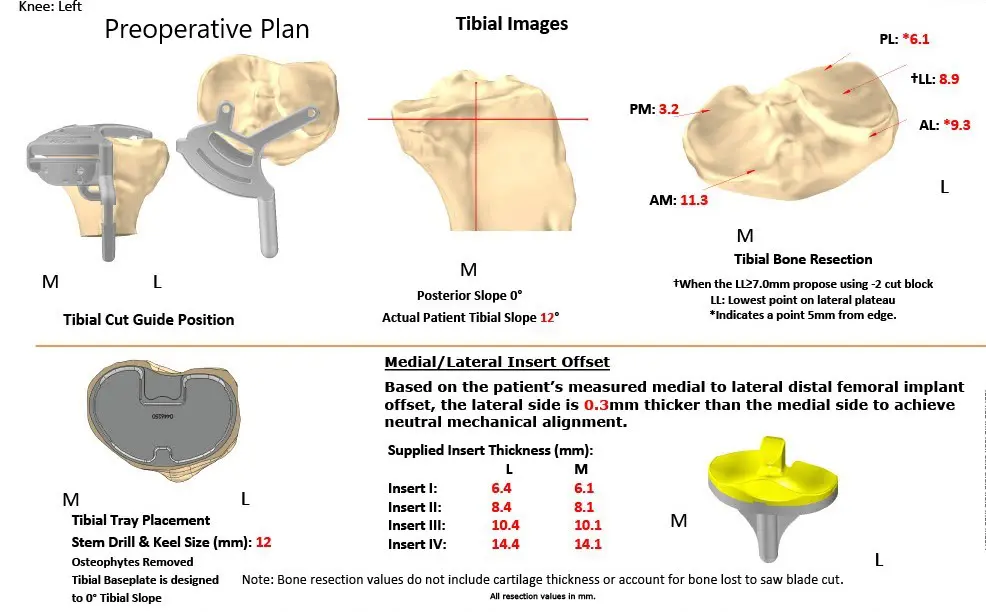
Complete Orthopedics patient-specific surgical plan for a bilateral customized total knee replacement in a 72-year-old patient with arthritis (scan 3)
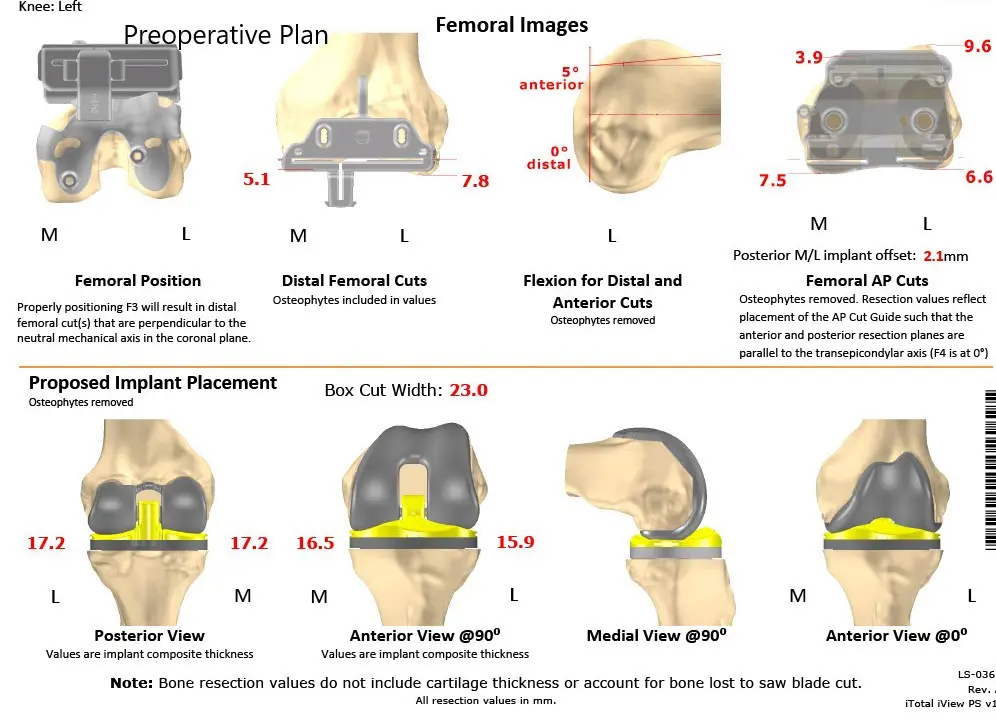
Complete Orthopedics patient-specific surgical plan for a bilateral customized total knee replacement in a 72-year-old patient with arthritis (scan 4)
PROCEDURE: Bilateral total knee arthroplasty.
IMPLANTS USED: Custom femoral implant with a tibial tray with 6-mm polyethylene inserts on the right side with 29-mm patellar component. Custom femoral implant with a custom tibial tray with 6-mm polyethylene inserts on the left side with the 32-mm patellar implant.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. Risks, benefits. and alternatives were extensively discussed with the patient as well as the family prior to the procedure.
They understand the increased risk of bilateral total knee arthroplasty. Then, it was decided to do the right knee first.
After obtaining anesthesia. both knees were then draped and prepped in the usual sterile manner. The knee was exsanguinated. A straight incision was performed. Medial parapatellar arthrotomy was performed on the right side.
The tibia was exposed. The tibial cutting guide was used. and the tibial resection was performed. The tibia was reamed and broached.
Attention was then turned towards the femur. Distal chamfer cutting guides were used, and the notch cutting guide was used for making the cuts. Medially and laterally laminar spreaders were used to remove the remainder of the meniscus and the cruciates.
Posterior osteophytes were then removed. The knee was then balanced, and the balance was found to be correct. The trial tibia was placed into position followed by the trial femur and the poly.
The patellar resection was then performed. Ori ti holes were made in the patella. The trial patella was placed into position.
The knee was then trialed through a full physiological range of motion. Full-extension was achieved. Full flexion was achieved. Patellar tracking was excellent. The trial components were then removed. A thorough lavage was given. The femur was cemented into position. Excess cement was removed.
The tibia was cemented into position. Excess cement was removed. Poly was then placed into position, and the knee was then held in full extension with a bump under the ankle. The patella was then cemented into position. Excess cement was removed and was held with a clamp until the cement hardened.
After the cement hardened, the patellar clamp was removed. The tourniquet was let down. Thorough hemostasis was achieved. The injection was given for pain control. Medial parapatellar arthrotomy was closed, followed by O Vicryl, 2-0 Vicryl, and then, the skin was closed with sutures.
Attention was then turned towards the left side. A straight incision was performed. After exsanguinating the extremity, medial parapatellar arthrotomy was performed. The tibia was then exposed, and the tibial cut was made with the tibial cutting guide. Tibia was then broached and reamed. Attention was then turned towards the femur.
The femur was then resected using distal chamfer cutting guides as well as the notch cutting guide. Medial and lateral laminar spreaders were used for resection of the meniscus and the cruciates. Posterior osteophytes were then removed. The gap balancing was performed and found to be correct.
The trial femur was placed followed by the trial tibia. Poly was placed into position. The extension was full, and full flexion was obtained. Patellar resection was then performed. Drill holes were made in the patella. Patellar tracking was found to be perfect.
Trial components were then removed. Thorough lavage was given. The injection was given. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. Poly was then placed into position. The knee was then reduced and held in full extension with a bump under the ankle.
Tourniquet was let down. Thorough hemostasis was achieved. Medial parapatellar arthrotomy was closed followed by subcutaneous tissue, subcuticular tissue. The skin was closed using Prineo. A sterile dressing was then applied over both wounds. The patient was then transferred to the postoperative care unit in stable condition.
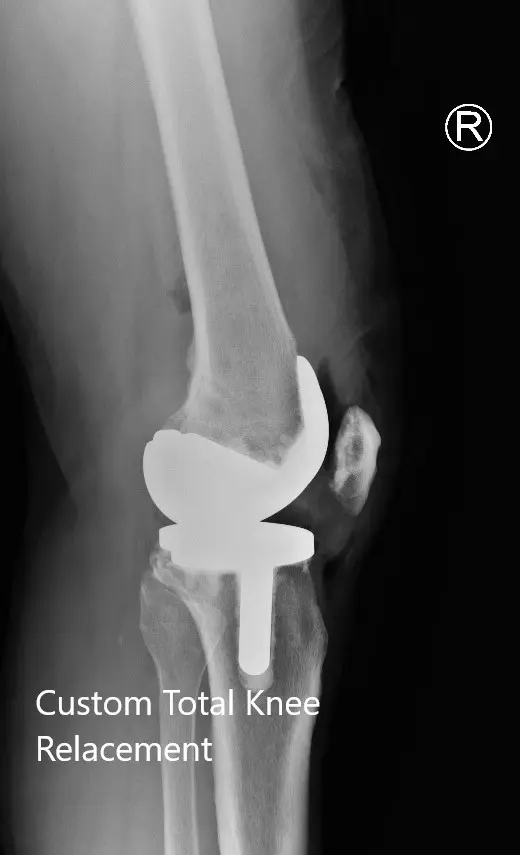
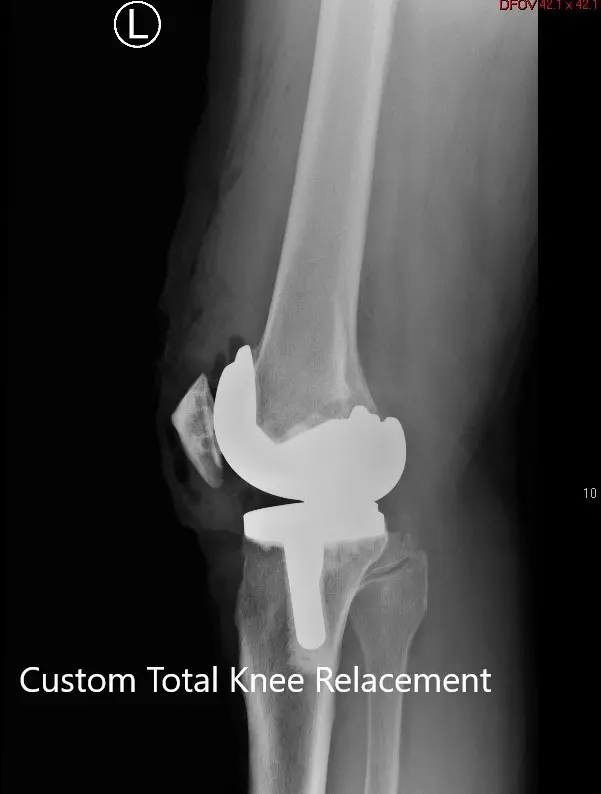
Postoperative X-ray showing the lateral views of both knees.
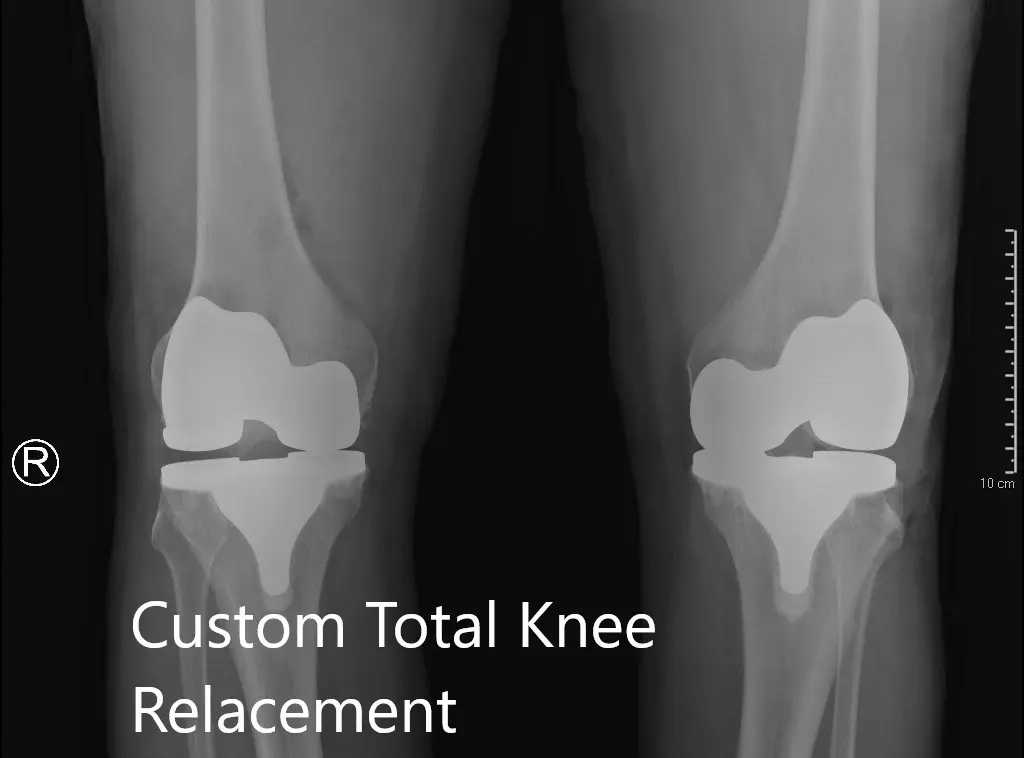
Postoperative X-ray showing the AP view of both knees.
Post-op she had an excellent recovery, she was walking the day of surgery with support. Her pain was managed with medications and she was able to go home the next day of the procedure. The patient was started on aspirin and TED stockings to prevent deep vein thrombosis. Physical therapy was started to increased flexibility.
Sutures were removed uneventfully. On her eight weeks follow up, she reported zero pain with a full range of motion in both knees. She was happily back to her baseline. She was able to drive a car, navigate stairs and do her daily activities without any discomfort. She was extremely happy with the outcome.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


