A 55-year-old female was seen with complaints of right knee pain. She stated she had a total of 3 surgeries performed on the right knee in the last 25 years. The first surgery that was done was the removal of cartilage and it was performed in 1990. The second surgery was a total reconstruction from a torn ACL (anterior cruciate ligament) that was performed in 1991 by another physician. The last surgery was another total ACL reconstruction and it was performed in 1992.
She was experiencing pain and constant locking in the right knee. She was considering surgery. Her initial injury was a sports injury 25 years ago. Since her last surgery in 1992, she experienced constant pain in her right knee. The pain was sharp in character and moderate in intensity (5/10).
She had previously also tried knee injections and physical therapy with no relief. She was a full-time worker as a manager at a departmental store currently not working. Activities such as twisting, turning, bending, kneeling and going up and down the stairs exacerbated her pain.
She was found it increasingly difficult to drive for a long time. Recently, she reported her sleep was disturbed because of knee pain. She was an occasional smoker and social drinker. She was allergic to beta-blockers. Her medical history included high blood pressure and asthma. She was currently using an inhalation pump and amlodipine 10 mg.
On her physical examination, her gait was steady. There was mild swelling of the right knee as evident with a positive patellar tap. The skin overlying the right knee was normal. There was positive tenderness on the medial and lateral joint line. Tenderness was also positive on patellar facets. There was ample crepitus on range of motion.
The range of motion was terminally restricted due to pain (5 degrees to 90 degrees). There was no valgus or varus instability of the right knee. Lachman and anterior drawer tests were negative. There was mild genu varus deformity of both the knee.
The examination of the left knee revealed mild arthritic changes. The examination of both hips and ankles was normal. There was no distal neurological deficit. The lower extremity pulses were palpable and comparable.
Imaging studies revealed arthritis of bilateral knees with severe tricompartmental arthritis of the right knee. In view of lifestyle limiting knee pain and exhaustion of conservative management, she was advised right knee custom replacement. Risks, benefits, alternatives were discussed with the patient at length. She agreed with the plan.
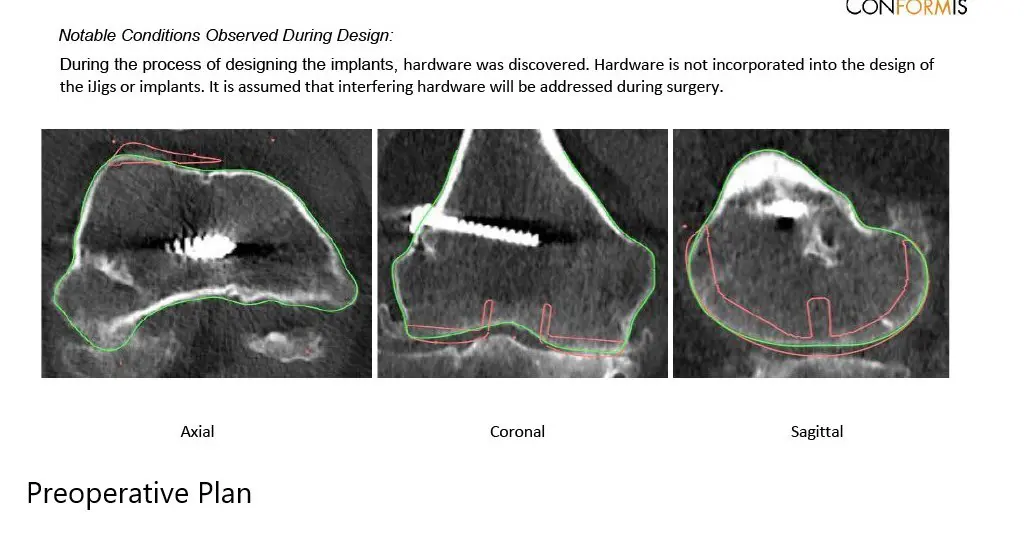
A preoperative CT scan obtained a few weeks prior to the procedure. The data was used to assess the patient’s unique anatomy and biomechanics. Customized unique patient-specific implants were made. Disposable bone cutting guides were 3D constructed to match the patient’s anatomy. A preoperative plan was formulated to guide the surgery.
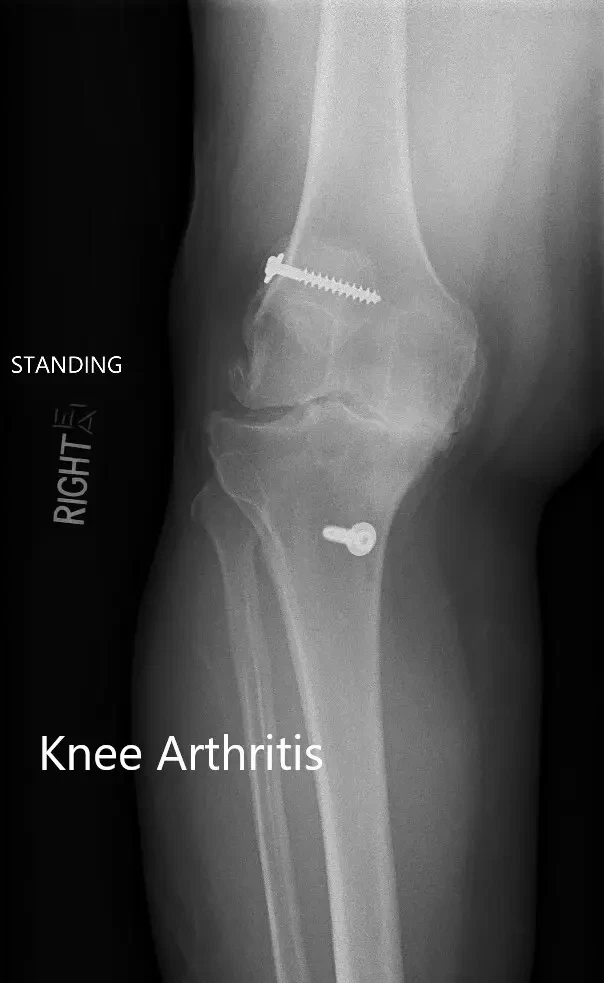
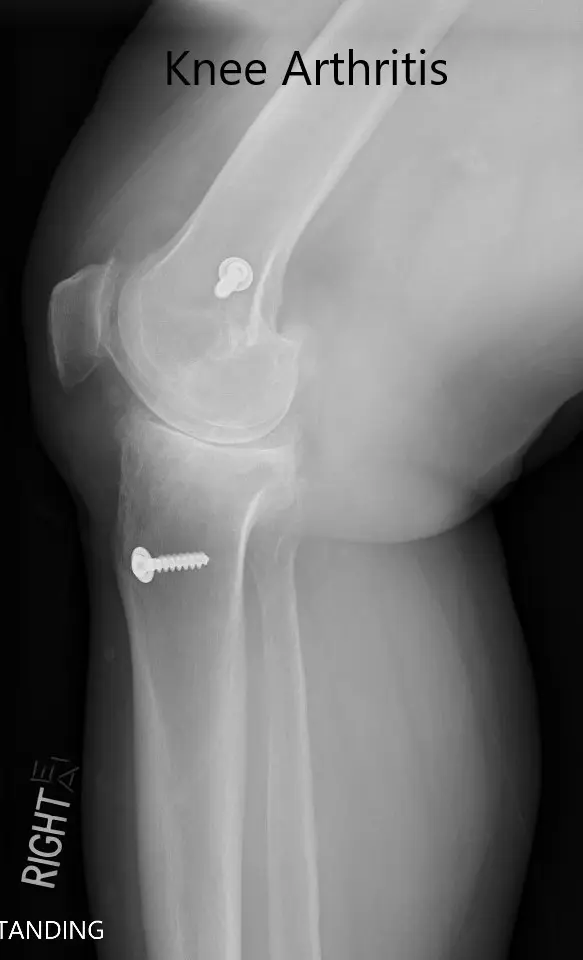
Preoperative X-ray showing the AP and lateral views of the right knee with retained screws consistent with ACL reconstruction.
Preoperative X-ray showing the AP and lateral views of the right knee with retained screws consistent with ACL reconstruction (image 3)
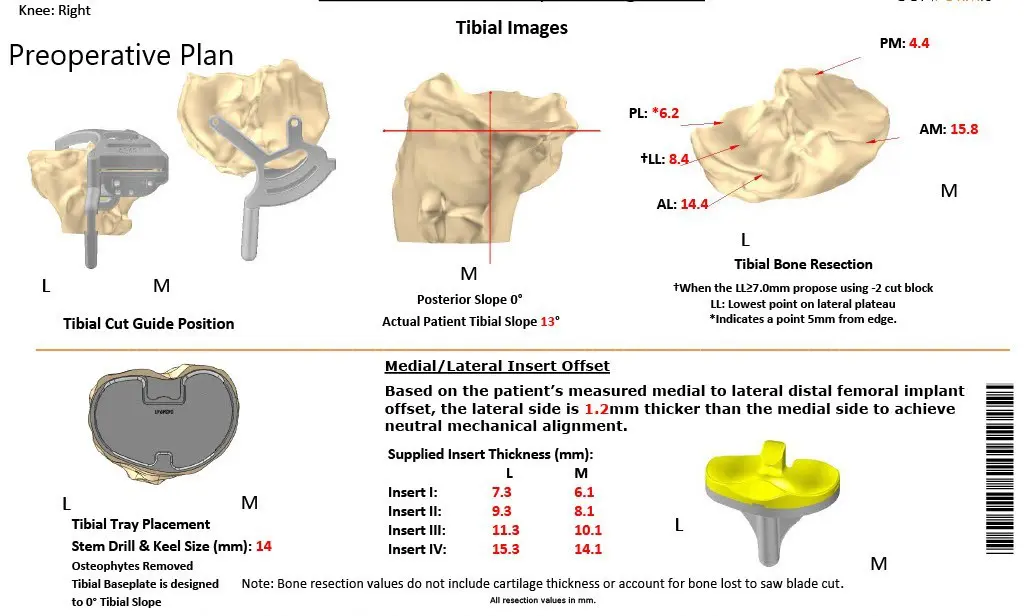
Complete Orthopedics patient-specific surgical plan for a custom right total knee replacement in a 55-year-old female with Prior ACL Reconstruction.
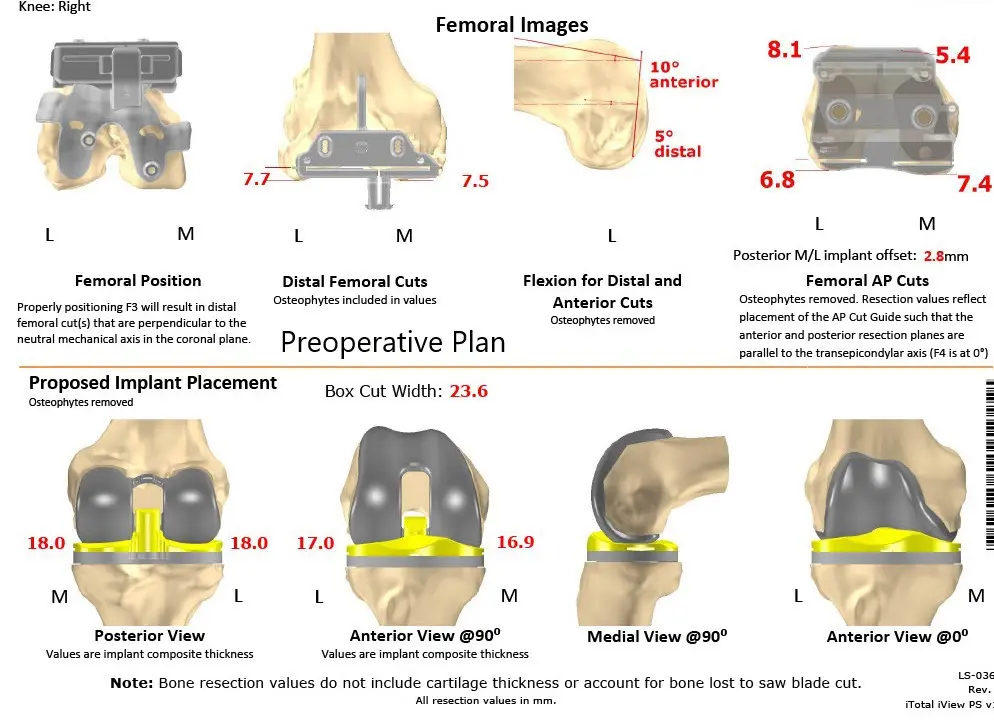
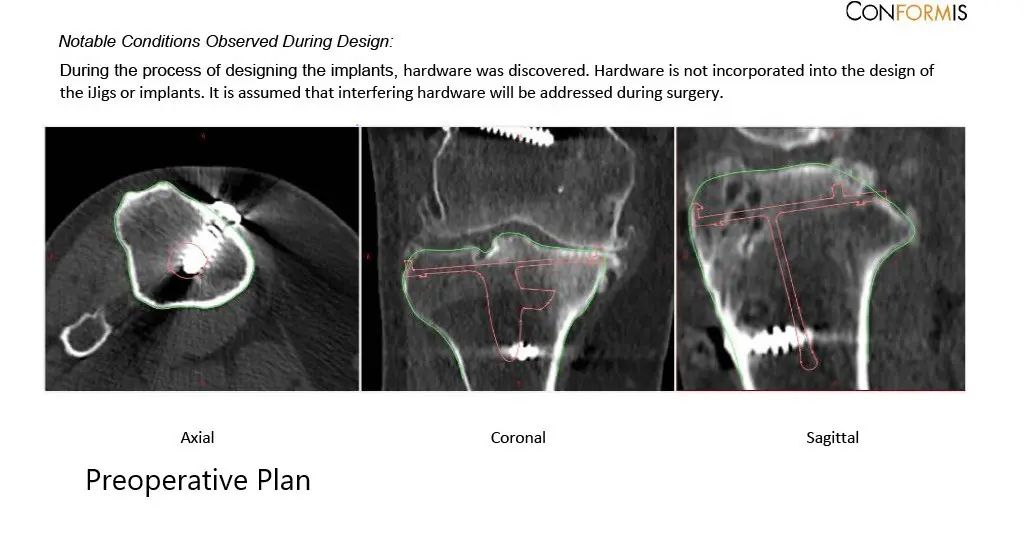
Complete Orthopedics patient specific surgical plan for a custom right total knee replacement in a 55-year-old female with prior ACL Reconstruction (scan 2)
Preoperative X-ray showing the AP and lateral views of the right knee with retained screws consistent with ACL reconstruction (image 3)
OPERATION: Right total knee arthroplasty.
IMPLANTS USED: 35-mm patella with 10 mm posterior stabilized polyethylene insert with a custom tibial tray with a custom femoral implant, posterior stabilized.

DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient understands the increased risk of medical and surgical complications.
Anesthesia was obtained by the anesthesiologist, and the patient was then definitively positioned. The right knee was then draped and prepped in the usual sterile manner after placing a cuff over his thigh. The limb was exsanguinated. A straight incision was made over the anterior aspect of the knee.
The skin and subcutaneous tissues were incised. Medial parapatellar arthrotomy was then performed. The knee was then exposed. The tibial surface was then prepared using the custom jig. Tibial dissection was performed and alignment was checked with the alignment guide. The tibial preparation was then performed.
Attention was then turned towards the femoral side. The distal cuts were made using the custom guides. The anterior, posterior, and chamfer cuts were made using custom guides. A notch cut was performed using the custom guide. Lamina spreaders were used medially and laterally, and the remainder of the meniscus and the cruciates were then debrided.
Posterior osteophytes were then removed. Gap balancing was performed and was found to be correct. The patellar resection was then performed until holes were made in the patella. The patellar osteophytes were then removed.
Trial patella was then placed into position. The trial femur was then placed into position. The trial tibia was then placed into position. The trial poly was then placed into position, and the knee was ranged to a full range of motion.
The knee was stable throughout the range of motion, and the patellar tracking was excellent. Trial components were then removed. Thorough lavage was given. Additional drill hates were made in the raw part of the tibia and the femur for cemented into position. Thorough lavage was given.
The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. Poly was then placed into position, and the knee was then reduced and held in full extension with a bump under the ankle. Patella was then cemented into position. Excess cement was removed.
After the cement hardened, thorough lavage was given. After removing the trial components, the injection was given to the knee joint. After the cement hardened, thorough lavage was given. The patellar clamp was removed.
Medial parapatellar arthrotomy was closed using #1 Vicryl and Stratafix. Cutaneous tissues were closed using Vicryl and subcuticular tissues were closed with 2-0 Vicryl. The skin was closed using staples. Sterile dressing was applied over the wound. The patient was then transferred to the postoperative care unit in stable condition.
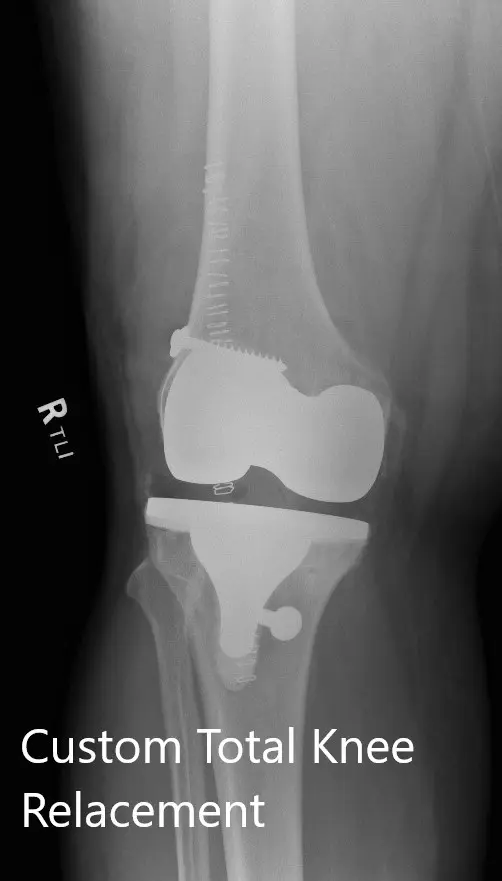
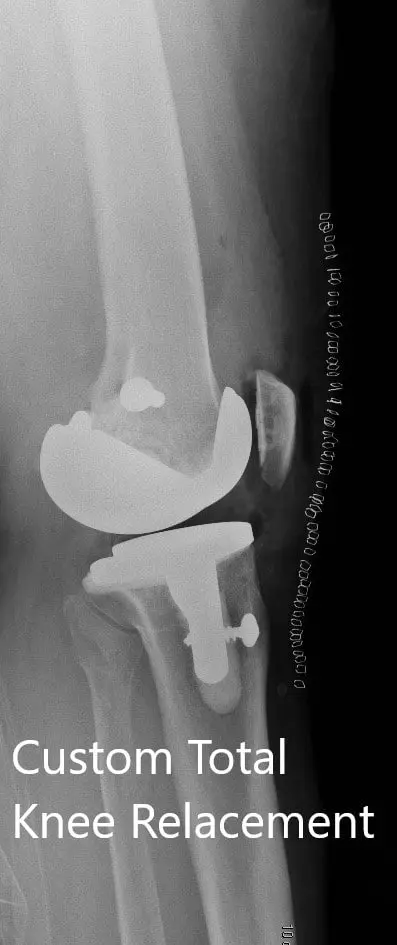
Postoperative images showing AP and lateral views of the right knee
Post-op weight-bearing was allowed the same day and the patient was able to walk 100 feet in the ward. The pain was managed well with oxycodone + acetaminophen. Aspirin was started for deep vein thrombosis prophylaxis. The patient was compliant with physical therapy and home exercise program.
The sutures were removed uneventfully. The patient was followed after three months and demonstrated a full range of motion. She was happily back to her work and enjoyed her baseline activities as she did before knee pain. She reported decreased pain in the left knee secondary to offloading of the weight. She follows up as needed.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


