A 72-year-old female presented to our office with complaints of worsening right knee pain. She first noticed the pain while climbing stairs about three years ago. She denied any associated or preceding injury to the knee. The pain had worsened to the point she was unable to walk for more than half a block.
She stated that the pain was located on the inner side of the right knee. She described crunching/cracking/grinding sensation on moving the right knee. The pain was described as a dull to sharp ache. The intensity was variable and was severe on certain activities.
She stated the pain was exacerbated with activities such as prolonged standing, walking, bending, kneeling, squatting, twisting and turning. She used a cane as an assistive device and climbed stairs using the banter one step at a time.
She as a retired nurse who was active previously in organizing volunteer activities at a hospital. Since the severity of pain increased, she described her lifestyle as moribund. She felt distressed not being able to be active as earlier.
She previously tried conservative management in the form of physical therapy and heat pads. She also received visco-supplement injections from her physical therapist but with no relief.
She was a former smoker and consumed moderate alcohol socially. She denied any drug allergies and her past medical history was positive for hypertension, asthma, and dyslipidemia. Her medical conditions were well controlled with medications. She had a carpal tunnel release done a few years back.
On physical examination, she walked with an antalgic gait with a reduced stance phase on the right side. There was mild swelling of the right knee. Tenderness was present on the medial joint line. Tenderness was also present on the patellar facets.
The patellar tendon and quadriceps tendon was intact and non-tender. There was no evidence of any instability in the coronal, sagittal and axial planes. The range of motion was painful with copious crepitus.
The examination of the left knee, bilateral hips and ankles were normal. There was no distal neurological deficit. The bilateral lower extremity pulses were palpable and comparable. The bulk and tone of the bilateral lower extremities were normal.
Imaging studies revealed severe tricompartmental osteoarthritis of the right knee. Considering the lifestyle limiting knee pain, the patient was advised right total knee replacement. All the risks, benefits and alternatives were discussed in detail with the patient. The patient agreed to go ahead with the procedure.
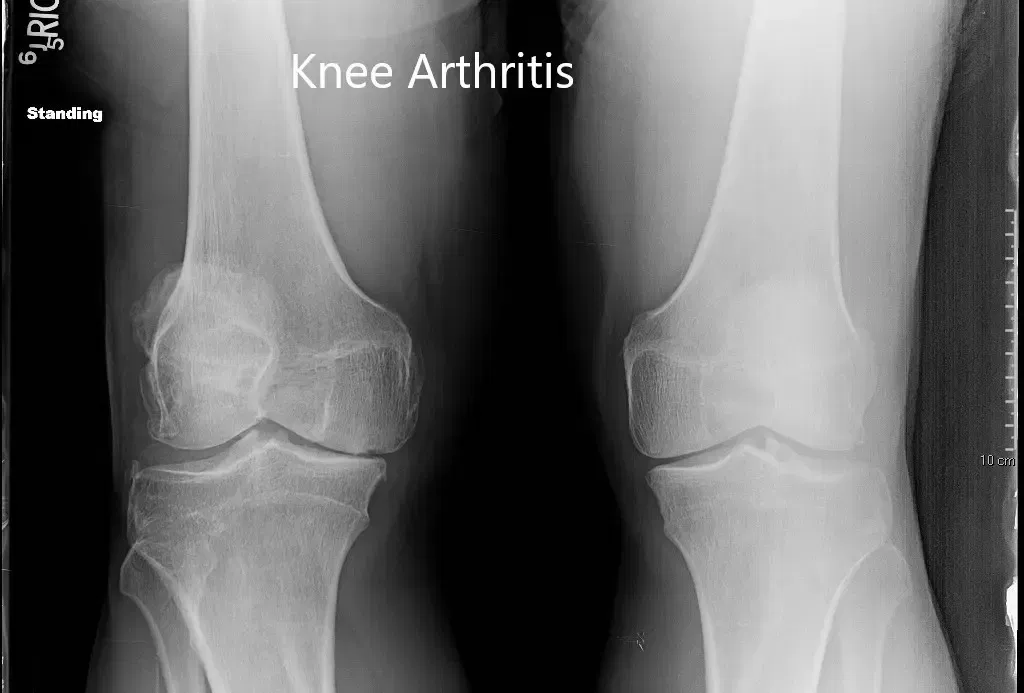
Preoperative X-ray of both the knees in anteroposterior view.
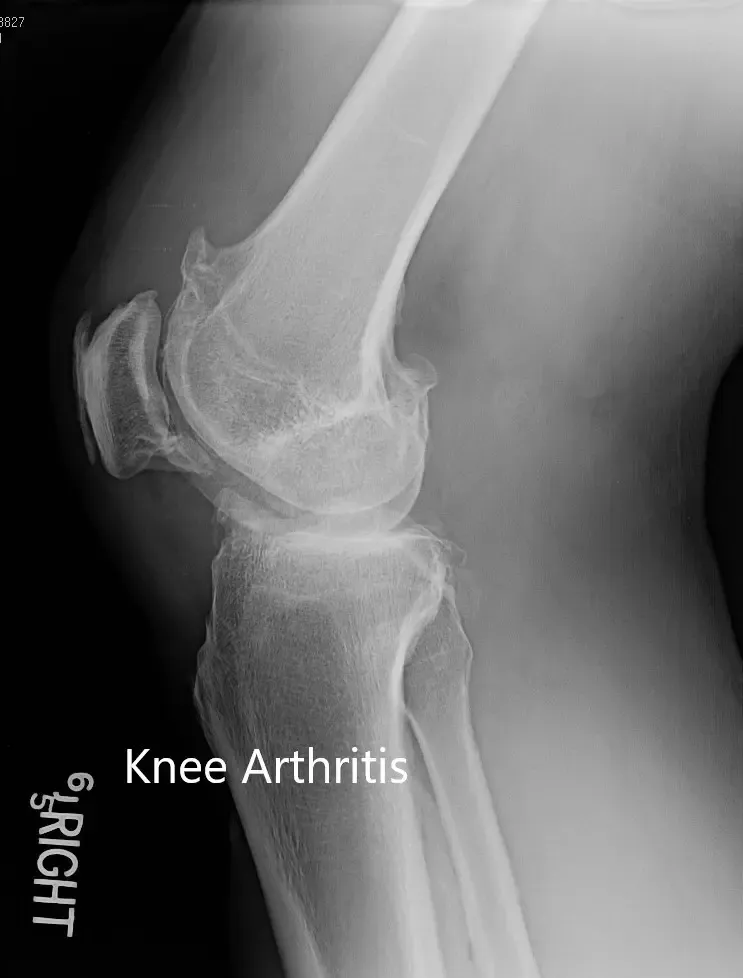
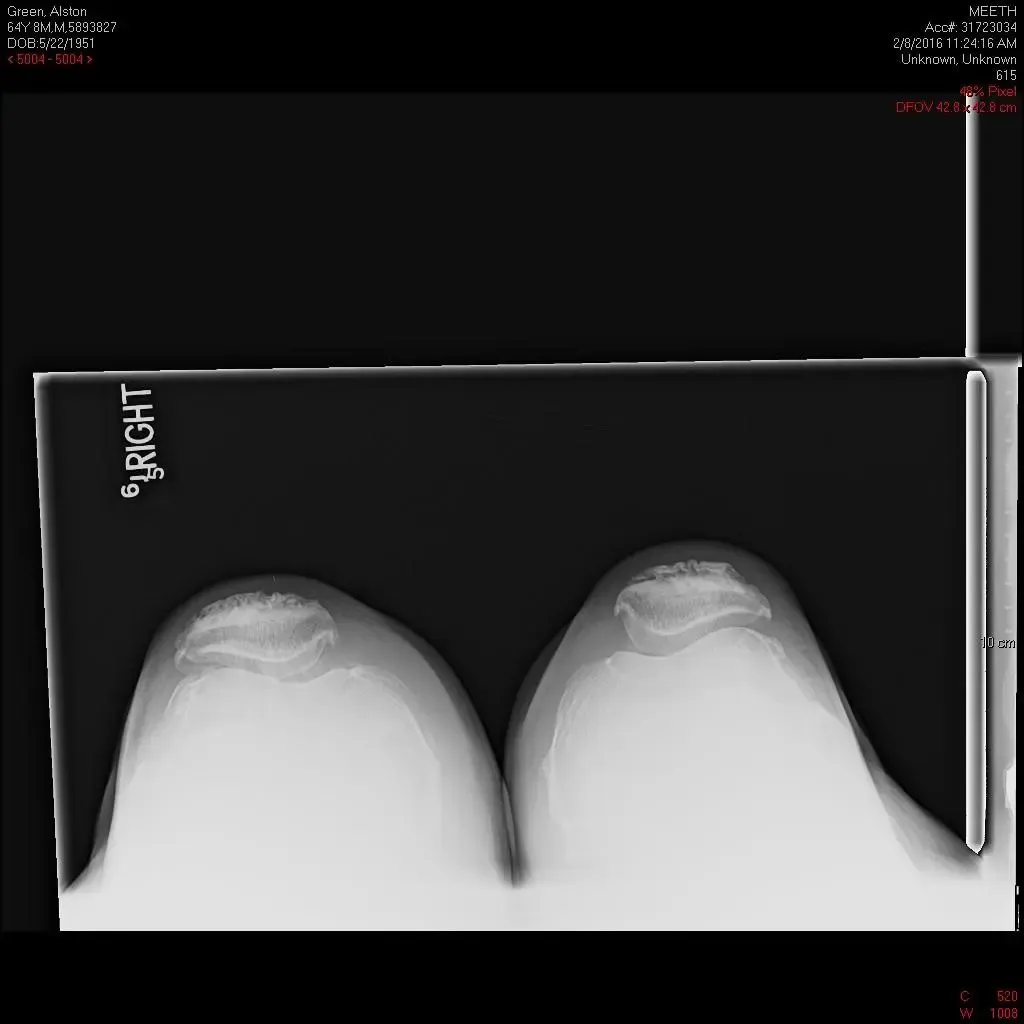
Preoperative X-ray of the right knee in lateral view and skyline view.
OPERATION: Right total knee arthroplasty.
IMPLANTS USED: Posterior stabilized femur size 11 with tibia size F with a tapered stem with 12-mm constrained posterior stabilized polyethylene.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent signing in the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure. The patient understands that she is at a significantly increased risk for complications.
The patient was brought to the operating room, and anesthesia was obtained by the anesthesiologist. The right knee was then draped and prepped in the usual sterile manner with a cuff over the right thigh. Time-out was then performed, and the extremity was then exsanguinated. Tourniquet was then elevated.
A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were then incised. The medial parapatellar arthrotomy was then performed. The fat pad was then resected. The medial soft tissue sleeve was then developed.
The femoral patient-specific guide was then placed into position and pinned into position. The distal cut was then performed followed by the anterior, posterior, and the chamfer cuts. The tibial resection was then performed. Laminar spreaders were then used medially and laterally and the meniscus and the cruciates were then debrided. The notch cut was then performed.
The extension, flexion space was found to be well balanced. The trial femur was placed into position followed by the trial tibia and the poly. The patella was then resected. and the trial patella was then placed into position.
The knee was trialed through a full range of motion, and the range was found to be excellent. Patellar tracking was found to be excellent. The flexion and extension gap was found to be well balanced.
The trial components were then removed. Thorough lavage was given, and intraarticular injection was given. The femur was cemented into position followed by the tibia, and the poly was then placed into position.
The knee was then held in full extension after removing the cement. and the patella was then placed into position. and excess cement was then removed. After the cement hardened, the patellar clamp was then removed.
At this point, it was noticed that the knee was balanced, but the polyethylene size was smaller. The patellar size was therefore increased to 12 mm from a 10 mm polyethylene.
After the new polyethylene was placed into position, the knee was stable. Flexion and extension gaps were found to be well balanced. A thorough lavage was given. The medial parapatellar arthrotomy was closed with Ethibond.
Cutaneous tissues were closed with O Vicryl. Subcuticular tissues were closed with 2 O Vicryl. The skin was closed using staples. Sterile dressing was then applied over the wound, and the patient was then transferred to the postoperative care unit in stable condition.
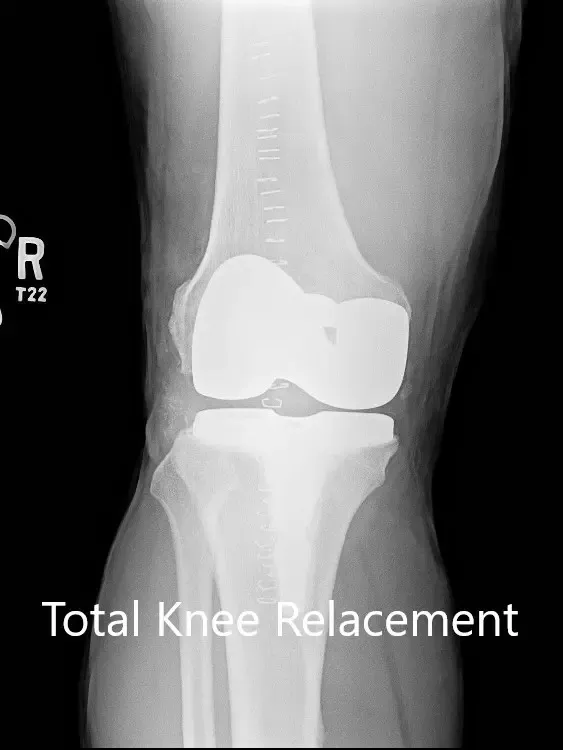
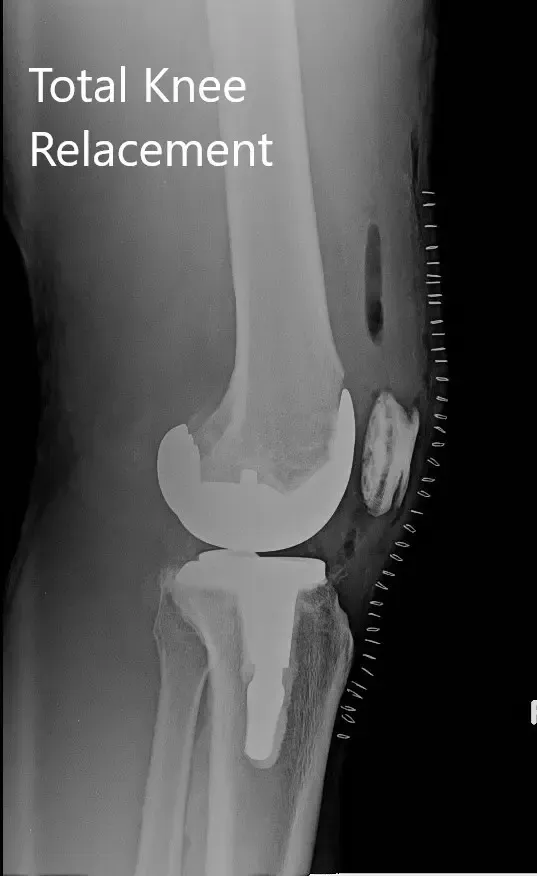
Postoperative X-ray of the right knee with a prosthesis in anteroposterior and lateral views.
Post-op the patient’s recovery was good with normal vitals. She was able to walk with support on the same day. She was given oral medications for pain and aspirin for deep vein thrombosis prophylaxis.
She was advised physical therapy as she was discharged the following day. The sutures were removed uneventfully. Two months post-op she demonstrated a full range of motion of the right knee with no pain. She was back to her baseline and expressed satisfaction on the outcome of the procedure.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


