A 68-year-old retired security guard presented to our office complaining of worsening right knee pain and right shoulder pain. She stated she sustained a motor vehicle accident 3 years ago when her car was rear-ended. She suffered injuries to her right knee and shoulder.
Over the past 2 years, she had tried conservative treatment options. She had 3 gel injections and 2 cortisone injections in her right knee with minimal relief. She tried physical therapy and home exercise program but without a prolonged relief. She underwent a rotator cuff repair of the right shoulder in New Jersey a year ago.
She states the pain in her right knee has worsened to the point that she is unable to walk or get up from a chair without discomfort. She had restricted herself to the first floor unable to climb stairs. Moreover, she felt reclusive and moribund unable to join her friends at the local supermarket and restaurant.
The patient was a nonsmoker and nondrinker. She had a past medical history of asthma, irritable bowel disease, obstructive sleep apnea, and hypertension. Her medical complaints were well controlled with medications. She had a hysterectomy in the past.
She was visibly upset on her office visit describing her daily ordeal with pain. She was using a cane for ambulation. Her gait was antalgic but coordinated. She was well oriented to time place and person. There was no deformity in the knee on supine and standing examination.
There was mild swelling in the right knee with no erythema and no rise in temperature. Tenderness was positive on the medial and lateral joint line. The range of motion was restricted terminally due to pain. There were no signs of any coronal, sagittal, axial plane instability or laxity.
The examination of the bilateral hips and ankles was unremarkable. Distal neurological examination was normal with intact light touch sensation in all dermatomes. There was no bladder bowel abnormality. She had tenderness over the right subacromial bursae and long head of biceps tendon. Abduction and internal rotation of the right shoulder were restricted terminally.
Imaging studies revealed tricompartmental osteoarthritis with degenerative changes. She was advised custom right total knee replacement considering her examination and needs. A preoperative CT was to be obtained a few weeks prior to surgery.
CT scan images provided accurate data on patients’ knee anatomy. Further, disposable cutting blocks were 3D printed for the patient’s unique anatomy. The preoperative plan was made outlining the various surgical steps and bone cuts. Custom patient-specific implants were made to match the patient’s unique anatomy.
Risks, benefits, and alternatives were discussed with the patient in detail. She was advised of both nonsurgical and surgical methods. The patient went ahead with custom total right knee replacement (posterior stabilized).
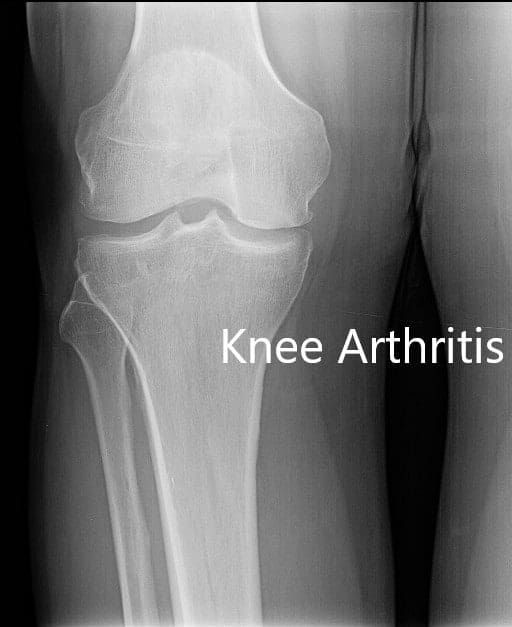
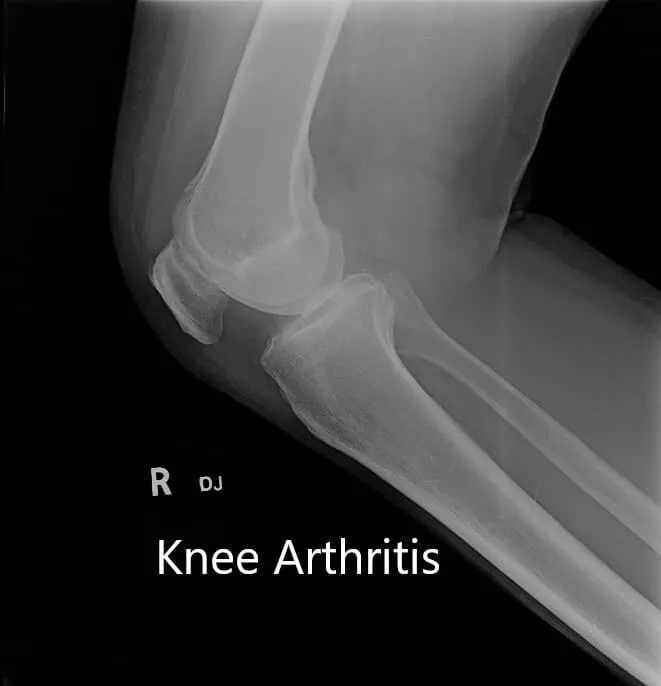
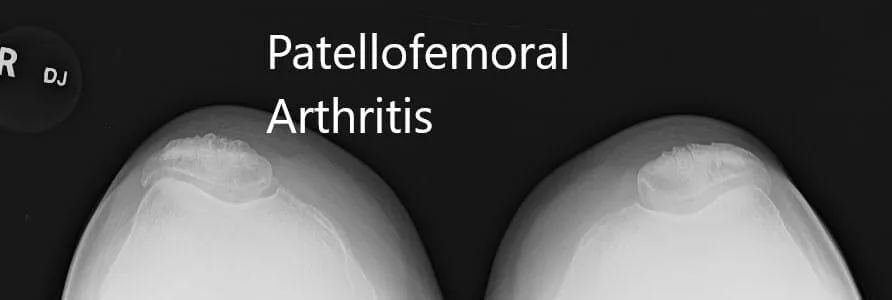
Preoperative X-ray showing AP and lateral view of the right knee joint, and skyline view of both the knee joints.
IMPLANTS USED: Custom femur with a Custom tibia with 10-mm polyethylene insert with a 32-mm x 6-mm patella.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well as the right side of the procedure.
The patient brought to the operating room and anesthesia was obtained by the anesthesiologist. The patient was definitively positioned and the right hip was then draped and prepped in the usual sterile manner. The limb was exsanguinated and the tourniquet was then elevated.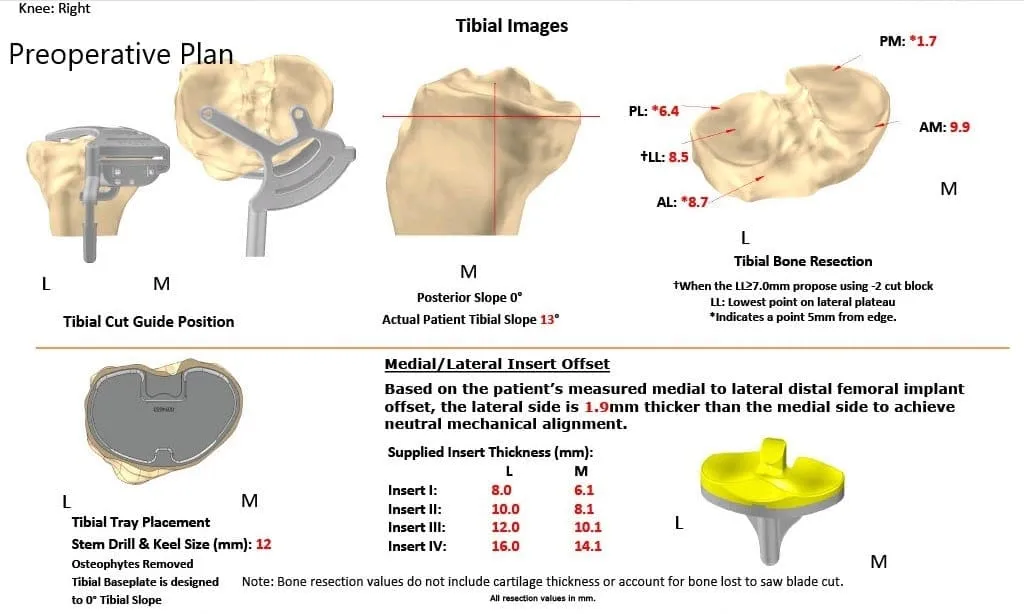
Complete Orthopedics patient-specific surgical plan for a right custom total knee replacement in a 68-year-old female.
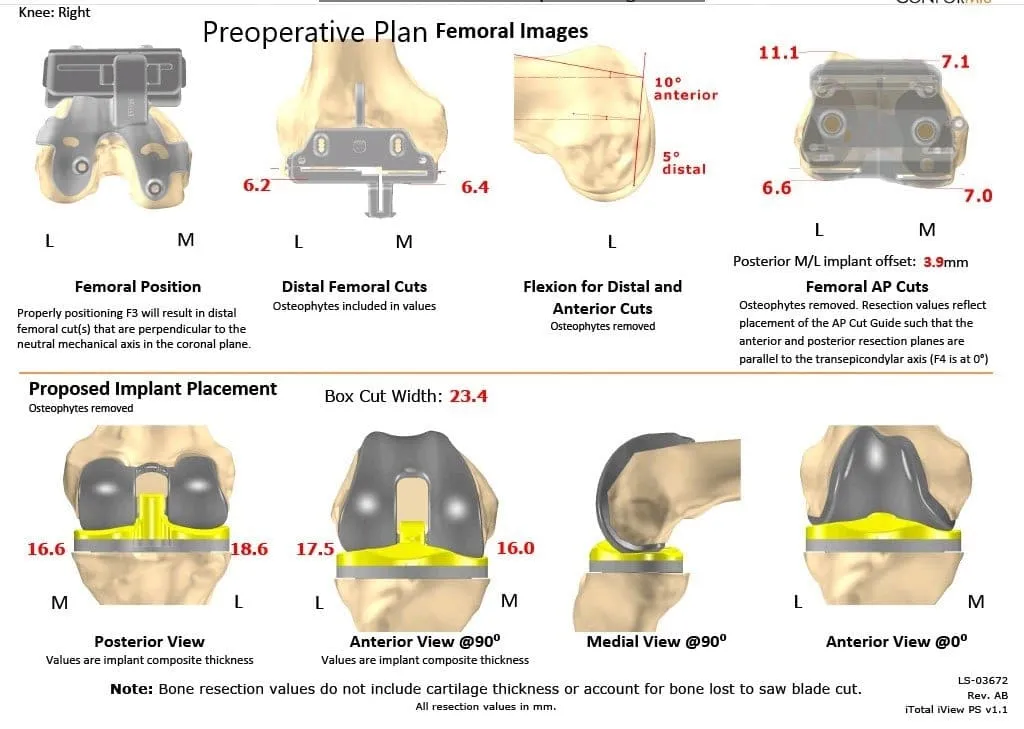
Complete Orthopedics patient-specific surgical plan for a right custom total knee replacement in a 68-year-old female (scan 2)
A straight incision was used for the arthrotomy. Skin and subcutaneous tissue was incised and medial parapatellar arthrotomy was then performed. The knee was then exposed. The femoral distal cut was then performed using the guide.

The anterior, posterior and chamfer cuts were then performed using the guide. The tibia was then repaired using the guide. The alignment of the femur and the tibial cuts were then checked with an alignment guide. Lamina spreaders were used medially and laterally, and meniscus was then debrided.
Posterior osteophytes were then removed. The notch cut was then performed and the patellar cut was then performed and the trial patella was then placed into position after making drill holes in the patella.
The trial femur was placed into position followed by the tibia. The poly was then placed into position. Excellent stability was then achieved.
Trial components were then removed. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. Poly was placed into position and the knee was then reduced and held with a bump under the ankle. The patella was then cemented into position.
After the cement hardened, the tourniquet was let down. Thorough hemostasis was achieved. The wound was then closed in layers. Sterile dressing was then applied to the wound, and the patient was transferred to the postoperative care unit in stable condition.
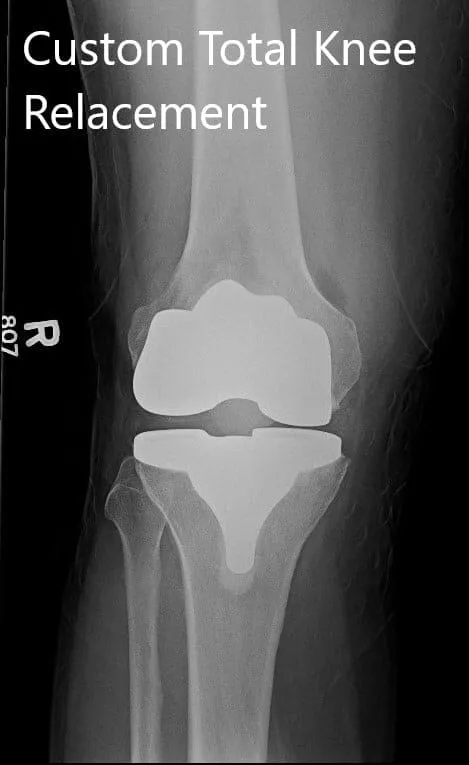
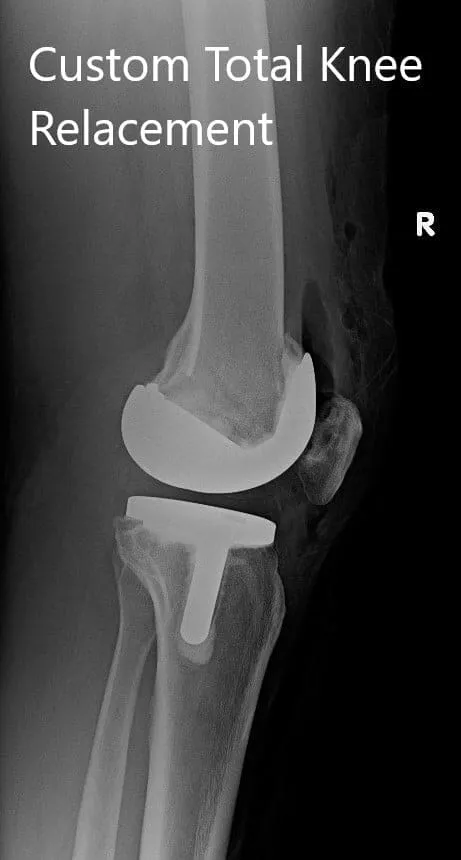
Postoperative X-ray showing AP and lateral images of the right knee
She had an excellent recovery postoperative. She was walking with support the same day of the surgery. The pain was controlled with medications. Deep vein thrombosis prophylaxis was started in the form of compression stockings and aspirin 325mg BID.
Physical therapy focusing on muscle strengthening and increasing range of motion was started. The patient was compliant with physical therapy and a home exercise program. She achieved a pain-free full range of motion in the subsequent visits.
The aspirin was subsequently discontinued. She was happily traveling to Florida to visit her grandson. She was now back to walking and doing her daily activities. She expressed happiness at the outcome of the surgery.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


