A 60-year-old female complained of worsening right knee pain. She states that the symptoms have been acute non-traumatic and began two years ago. The symptoms occur constantly. The pain is described as a dull ache and discomforting. The patient previously had a right meniscal repair done by an outside physician 3 years ago.
The pain was moderate to severe in intensity and disturbed her sleep. She described a sensation of giving away of her right knee. The pain was located on the inner side of the knee and was non-radiating.
The patient was unable to perform her daily activities. She described exacerbation of pain with walking, bending, kneeling, sitting, standing and climbing stairs. She was unable to walk for more than 3 blocks and negotiated stairs one step at a time.
She was employed as a manager at a grocery store but was currently not working secondary to pain. She was emotionally stressed about the pain. She stated she avoided getting out of her bed due to apprehension of pain. She used a cane as an assistive device.
She tried physical therapy and home exercise program with minimal to no relief. She received three cortisone injections in the right knee. Initially, she described significant relief with the injection for a month. But subsequently, her last injection only lasted for less than a week. She also tried heat pads and gel injections without any significant relief.
She described a previous intake of steroids for lupus. She was currently not taking any steroids or immunosuppressants. She was a non-smoker and non-drinker. She was currently taking Tylenol for pain and Crestor for dyslipidemia.
On physical examination, she had marked pain in her arch of motion. Her gait was antalgic with a reduced stance phase on the right side. There was mild swelling of the right knee. The patellofemoral crepitus was present. There was tenderness on the medial joint line and patellar facet.
The Mcmurray test was positive for medial meniscus. There was no laxity or instability on valgus and varus stress testing at 0 degrees, 30 degrees and 60 degrees. There was no laxity in the sagittal and axial planes.
The examination of the left knee, bilateral hip and ankles were normal. There was no distal neurological deficit. The bilateral pulses were palpable and comparable. There was no bladder bowel dysfunction.
Imaging studies revealed severe osteoarthritis of the medial compartment of the right knee along with patellofemoral arthritis. MRI revealed progression of previous subchondral fracture at the medial femoral condyle now resulting in a region of avascular necrosis and prominent fluid-filled subchondral fracture line measuring up to 2.8 cm. There was a mild collapse of the articular margin and severe surrounding bone marrow edema.
There was a progression of the medial meniscal tear now with a high-grade tear at the posterior root attachment. Considering lifestyle limiting knee pain with avascular necrosis and arthritis of the right knee. The patient was advised right total knee replacement with custom instruments. She agreed with the plan.
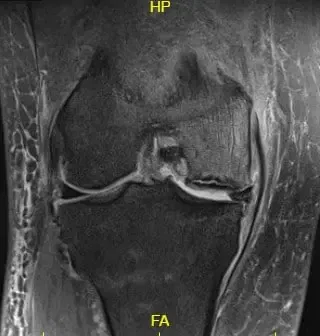
T2 weighted image showing the coronal section of the knee with altered bone marrow signal and rim sign.
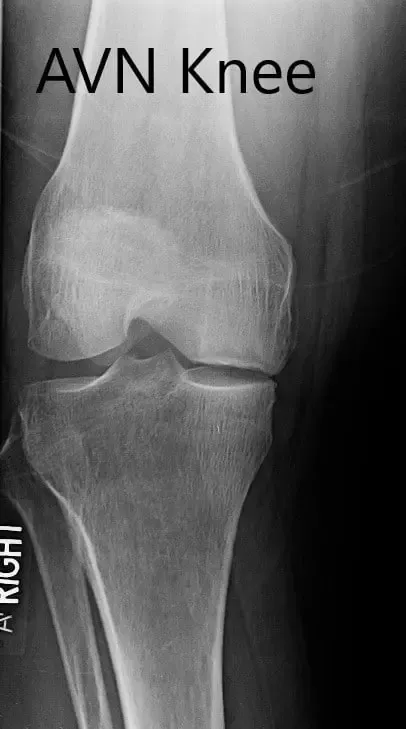
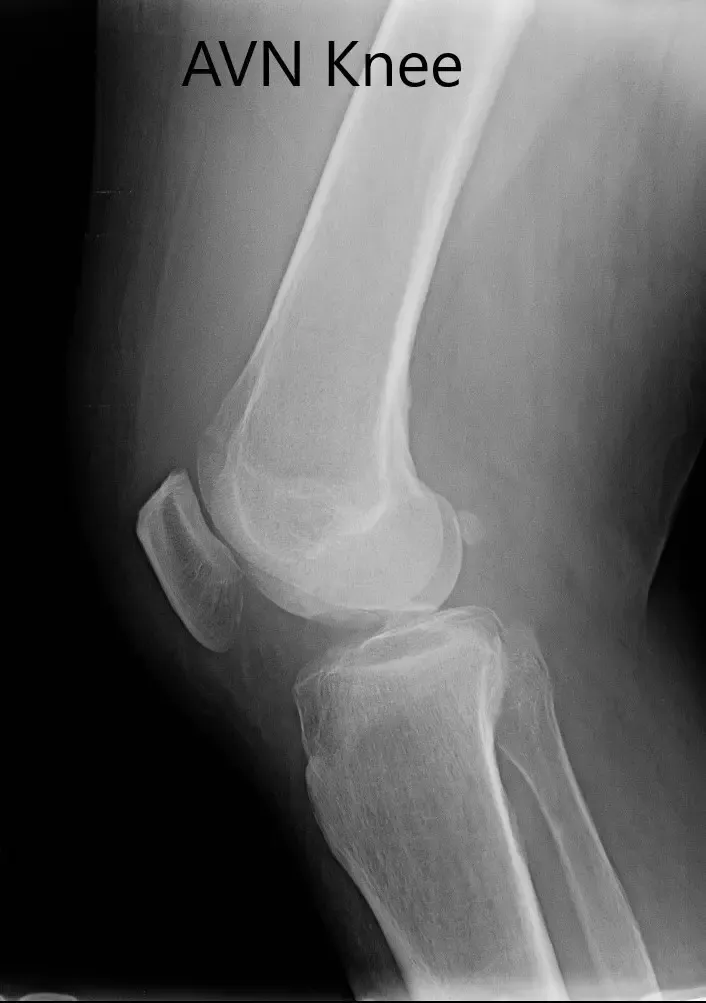
Preoperative X-ray of the right knee in anteroposterior and lateral views.
PREOPERATIVE DIAGNOSIS(ES): Right knee arthritis with osteonecrosis.
OPERATION: Right posterior stabilized total knee replacement
.
IMPLANTS USED: Tibia stemmed size E with a stem extension with highly cross-linked polyethylene patella 35 mm with femur size 11 with 10-mm posterior stabilized polyethylene.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient as well•as with his wife prior to the procedure.
The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist. The patient was definitely positioned and the right lower extremity was then draped and prepped in the usual sterile manner. The time-out was performed and after antibiotics were given, the limb was then exsanguinated.
A straight incision was used for the arthrotomy. Skin and subcutaneous tissue were incised, medial parapatellar arthrotomy was performed. The knee was then exposed. The tibial cutting guide was used for making the tibial resection. The tibial resection was then made and the bone was then removed.
The alignment guides were used for checking the alignment of the cut. Attention was then turned towards the femur. The distal femur was then drilled and distal cutting guide was then placed into position. The distal cut was then made followed by the chamfer cuts and the notch cut.
Lamina spreaders were used medially and laterally and the remainder of the meniscus and the cruciate were then debrided. The flexion and extension gaps were then checked and were found to be correct. Patellar resection was then made.
Drill holes were then made in the patella. The patellar prosthesis was then placed into position. After placing the femur and the tibia and the poly trials, the knee was then trialed through a full range of motion and the stability was found to be excellent. The trial components were then removed. Thorough lavage was given.
The femur was cemented into position. Excess cement was removed. The tibia was cemented into position, excess cement was removed. Poly was placed into position and the knee was then reduced and then held in extension with the bump under the ankle. The patella was then cemented into position.
Excess cement was then removed. The patellar clamp was then placed into position until the cement hardened and after the cement hardened, the most thorough lavage was given. An injection was used for local anesthetic and the wound was then closed in layers. Sterile dressing was then applied to the wound, and the patient was transferred to the postanesthesia care unit in stable condition.
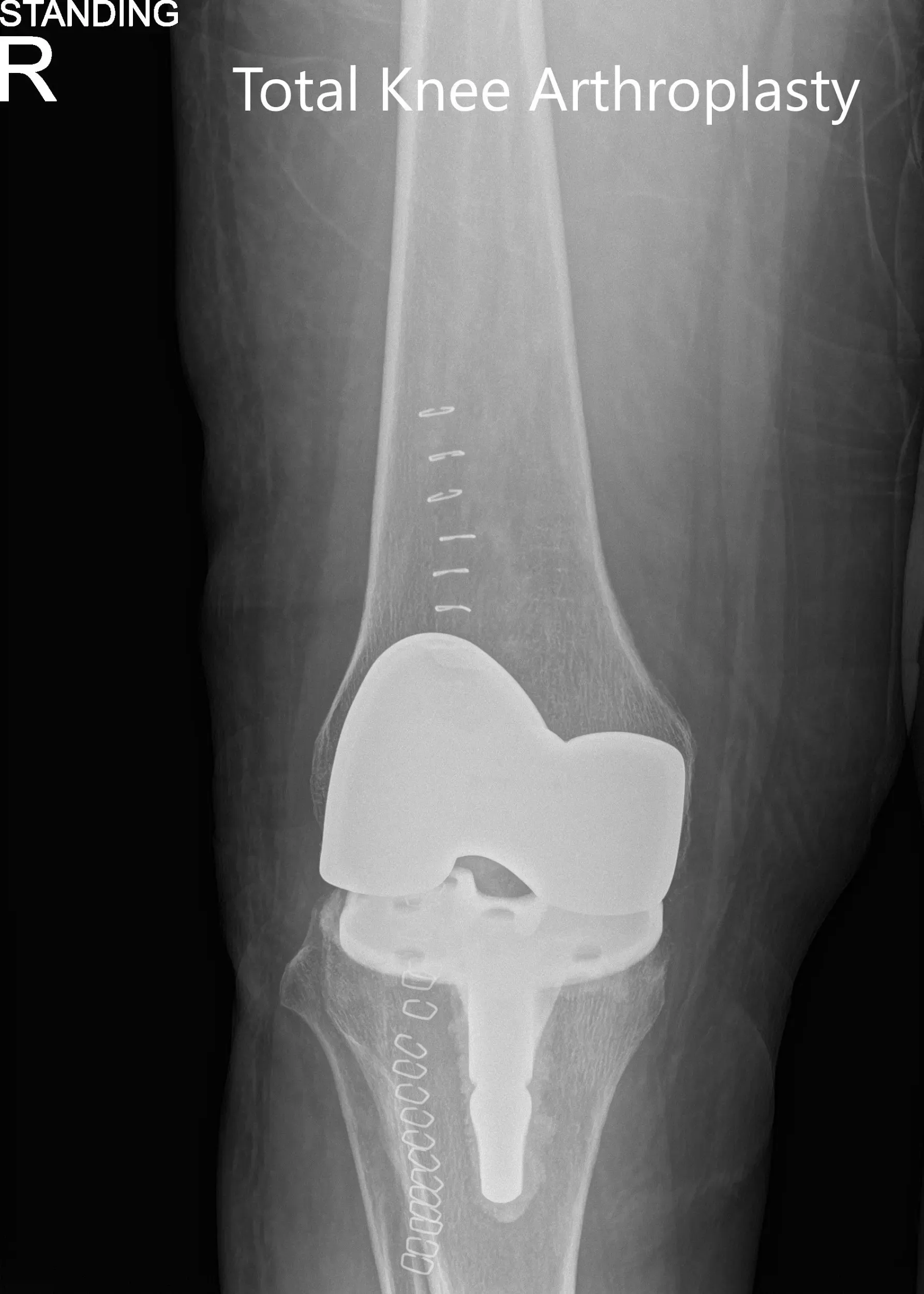
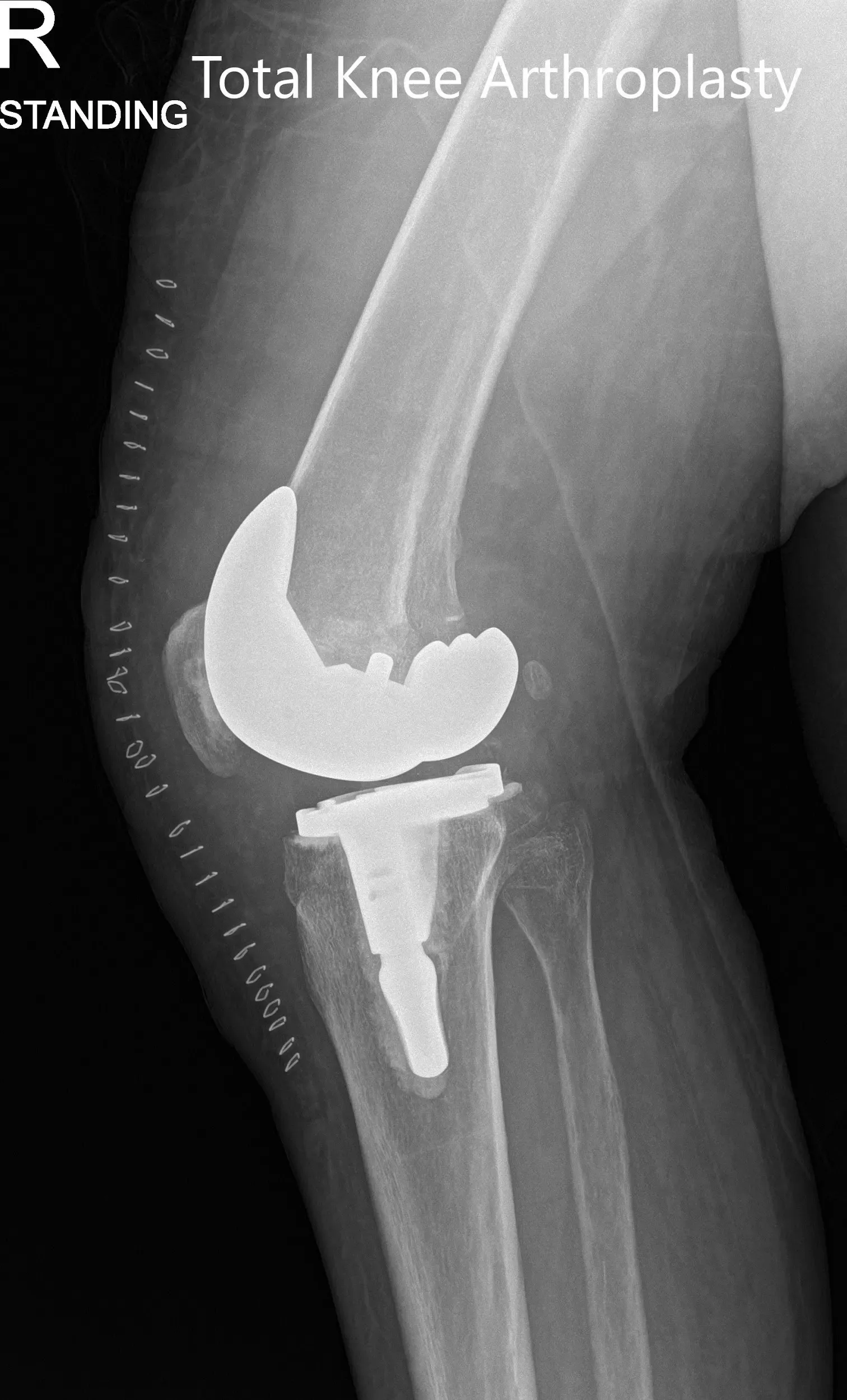
Postoperative x-ray showing the anteroposterior and lateral views of the right knee.
Post-op she had an excellent recovery. She was able to stand and walk the same day of the procedure. The pain was managed well with medications. She received outpatient physical therapy and was compliant with the home exercise program. Aspirin was given for deep vein thrombosis prophylaxis.
Three months post-op she demonstrated a full range of motion with no pain. She was walking without the support and reported her status back to her baseline. She was extremely happy with the outcome.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


