A 74-year-old female presented to our office complaining of worsening pain in the left knee. She stated she had been dealing with the pain in both her knees (left greater than right). She reported that around last winter the pain got worse in her left knee. She underwent cortisone injections, but the relief didn’t last beyond a few days.
She also tried other conservative options such as physical therapy and heat pads but with minimum relief. The patient is a retired security guard. She is currently living with her daughter. The pain has reportedly decreased her daily activities. She expressed anguish being not able to play with her grandkids.
The pain was described as a dull ache located more on the inner side of the left knee. The intensity varied from moderate to severe occurring with activities. She found difficulty in doing daily activities such as standing, walking, sitting, using stairs, kneeling, bending, turning and twisting.
She was a former smoker having quit ten years ago. Her medical history was positive for hypertension and dyslipidemia, both well controlled with medications. She reported seasonal allergies. She previously had a hysterectomy done 20 years ago.
Her physical examination was revealed an antalgic gait with a decreased stance phase on the left side. There was no evidence of genu varum or valgus deformity. There was a presence of mild bilateral knee swelling. There were no scars, sinus or redness on the skin overlying the left knee.
The range of motion was painful terminally ( 5-120 degrees on the left and 5-125 degrees on the right). There was joint crepitus with positive patellofemoral tenderness. Medial and lateral joint line tenderness was positive. Tests for instability in the coronal, sagittal and axial plane were negative.
Right hip demonstrated tenderness at the right greater trochanter suggesting bursitis. Left hip, bilateral ankle examination was normal. Examination of the sensory dermatomes of both lower extremities to light touch was intact. Motor examination of the great toe and ankle plantar flexors and dorsiflexors were normal. The distal pulses were palpable and good volume.
Imaging studies revealed severe osteoarthritis of the left knee. The patient was informed of treatment options in the form of surgical and nonsurgical methods. In view of lifestyle limiting left knee arthritis, she agreed to go for left knee total arthroplasty.
Risks, benefits, and alternatives were discussed at length. She was deemed as a candidate for custom knee replacement. The patient agreed with the plan. A few weeks prior CT of the patient’s lower extremities was obtained. Accurate planning of the bone cuts and offsets was made possible with data from the CT scan.
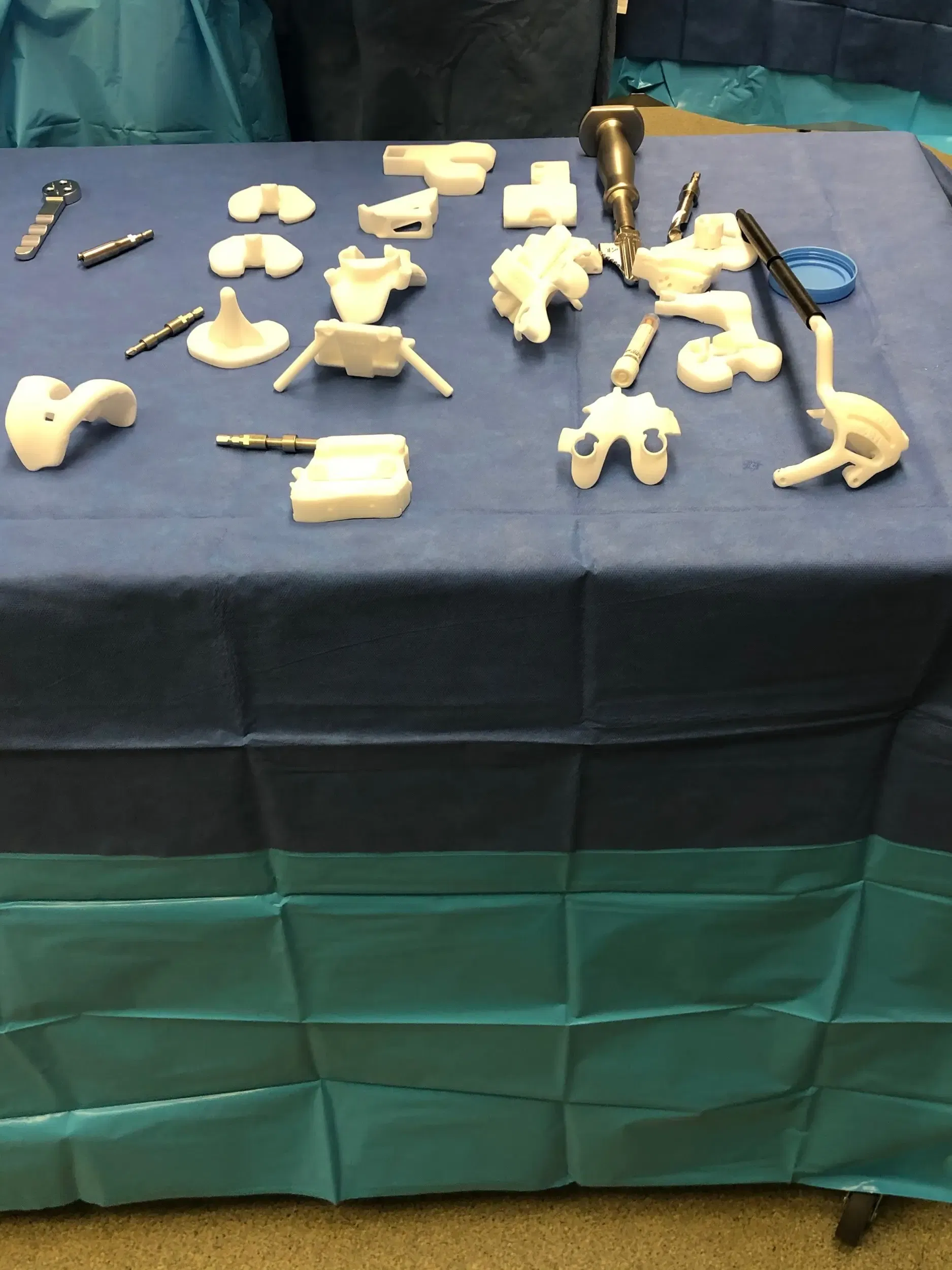
Patient-specific implants were made unique for the patient’s anatomy. Customized disposable jigs were constructed using 3D printers. A preoperative plan was formulated outlining the surgical steps.
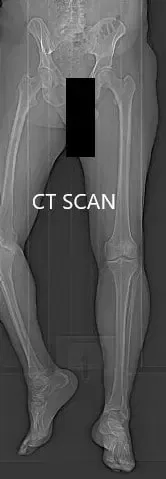
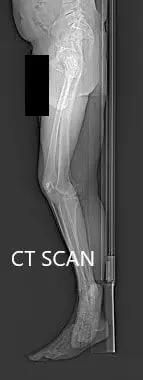
Preoperative CT scan topography images.
OPERATION: Left total knee arthroplasty using custom knee implants. Implants used were femoral implant with a custom tibial tray with 16 mm polyethylene insert with
29-mm x 6-mm patellar implant.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent and signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure
The patient was brought to the operating room, and anesthesia was obtained by the anesthesiologist.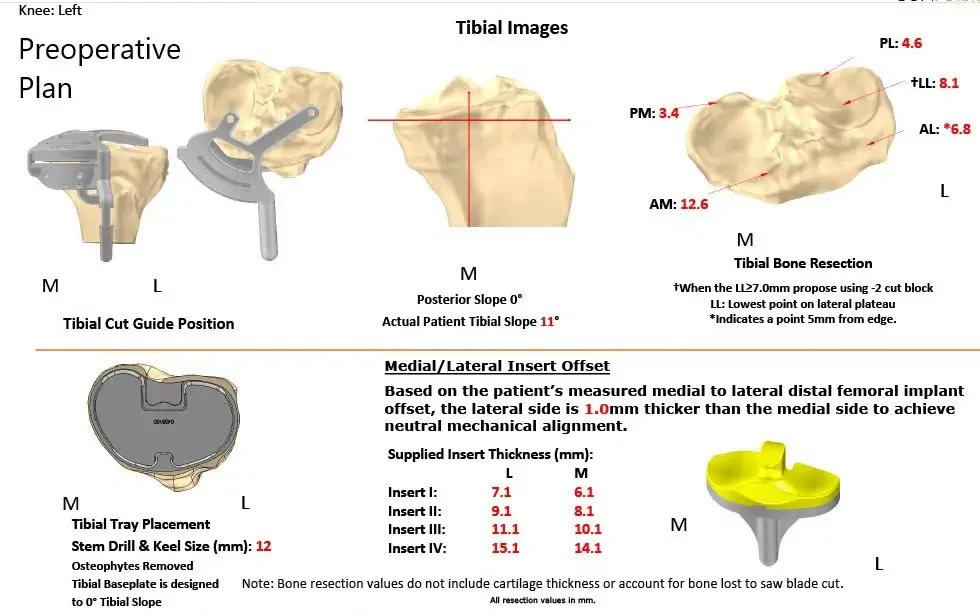
Complete Orthopedics patient-specific surgical plan for a left custom total knee replacement in a 74-year-old female.
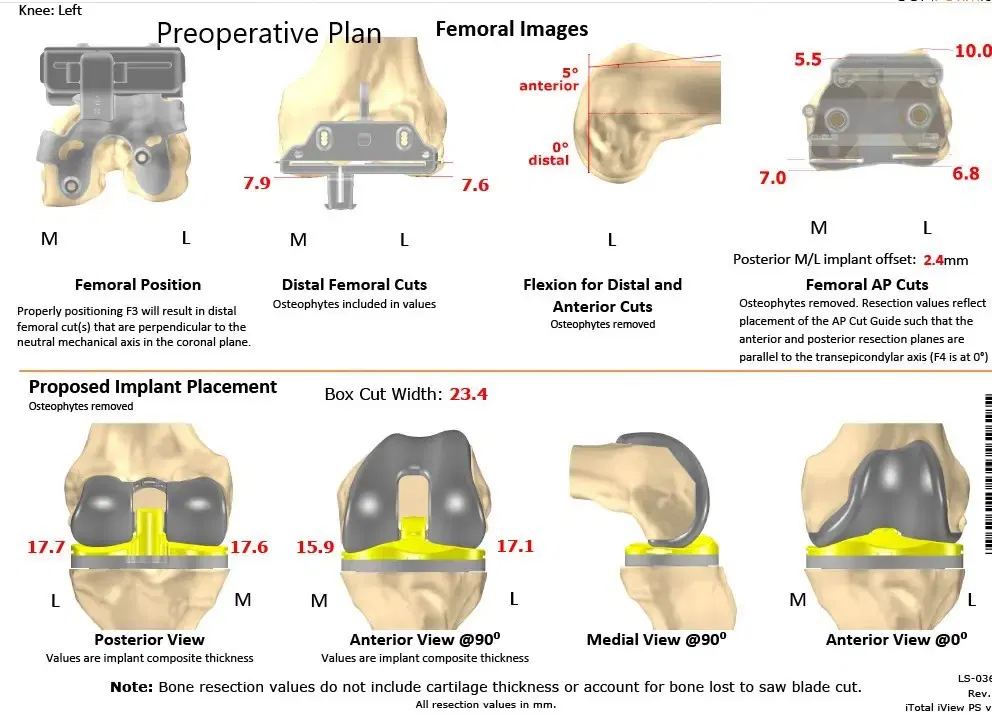
Complete Orthopedics patient-specific surgical plan for a left custom total knee replacement in a 74-year-old female (scan 2)
The patient was then definitively positioned, and a cuff was placed over the left thigh. The left lower extremity was draped and prepped in the usual sterile manner. An Esmarch was used to exsanguinate the extremity, and the tourniquet was elevated.
A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were incised. A medial parapatellar arthrotomy was performed. The tibia was exposed, and the tibial resection was performed using the cutting guides.
Attention was then turned towards the femur. The distal femur was cut using cut customized guide followed by the anterior, posterior, and the chamfer cuts. The notch cut was then performed.
Gap balancing was performed and was found to be correct. Attention was then turned towards the patella. Patellar resection was performed. Drill holes were made in the patella. The trial patella was then placed into position. Attention was then turned towards the femur. A trial femur was placed into position.
Attention was then turned towards the tibia. The tibial preparation was made. The trial tibia was placed into position, and the poly was then placed into position. The knee was then reduced.
The knee was trialed to a full range of motion. The patellar tracking was excellent. Trial components were then removed.
Thorough lavage was given. The injection was given. The femur was cemented into position. Excess cement was removed. The tibia was cemented into position. Excess cement was removed. Poly was then placed into position. The knee was then reduced and was held in full extension with a bump under the ankle. The patella was then cemented into position. Excess cement was removed. The patella was then held into position with a clamp.
After the cement hardened, the clamp was removed. A thorough lavage was given. Medial parapatellar arthrotomy was closed with O Viqryl and with StrataflX. Cutaneous tissues were closed with 0 Vicryl.
Subcuticulartissues was closed with 2-0 Vicryl. The skin was closed using staples. The tourniquet was let down. Sterile dressing was then applied, and the patient was then transferred to the postoperative care unit in stable condition.
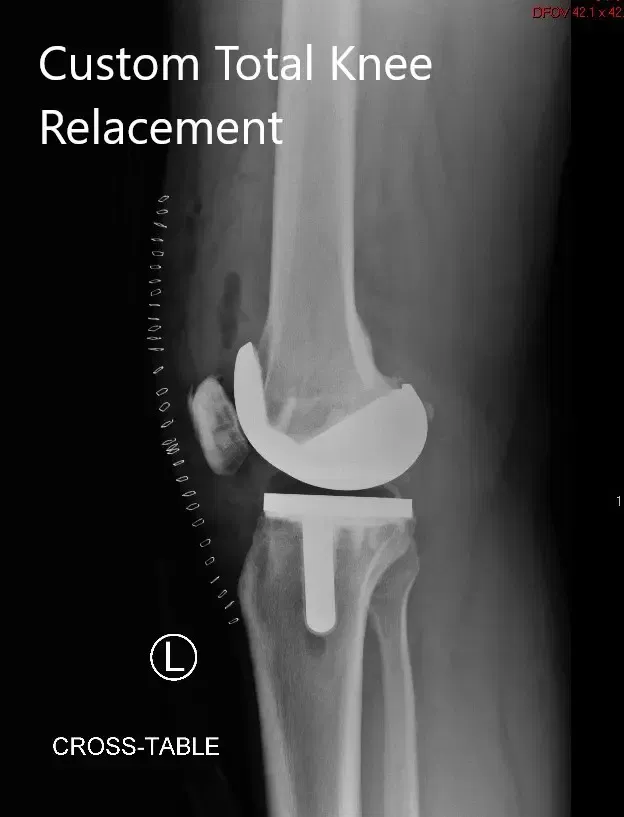
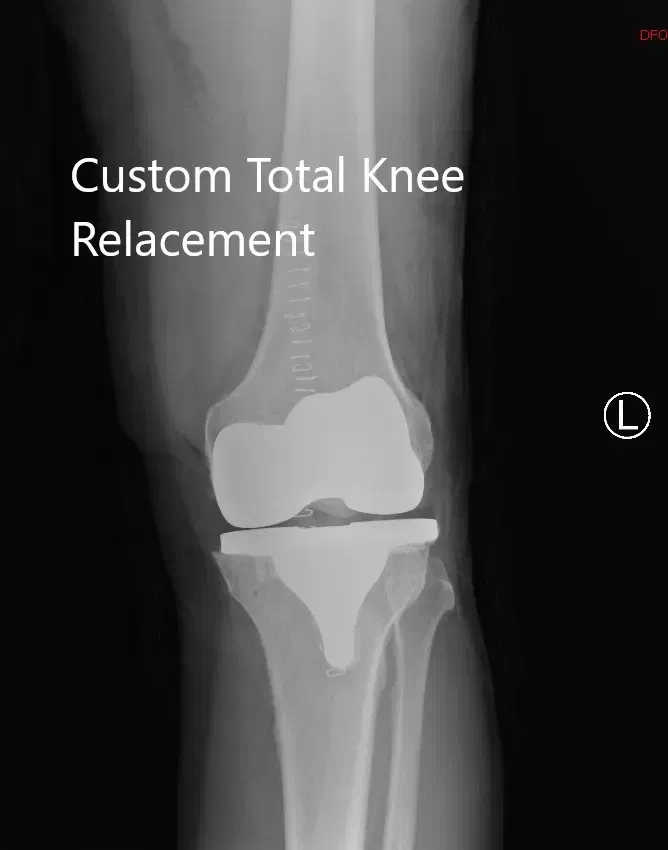
Postoperative X-ray of the left knee showing lateral and AP views
The pain was managed with medications and the patient was able to walk on the day of the surgery. She was started on aspirin for DVT prophylaxis. Range of motion and muscle strengthening exercises were utilized. Sutures were removed uneventfully.
The patient demonstrated excellent recovery and achieved a full range of motion in 4 weeks. She continued physical therapy. The aspirin was discontinued after 3 months. She was now back to her physical state before knee pain. She was extremely happy with the outcome of the surgery.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


