A 72-year-old male presented to our office with complaints of bilateral knee pain for the past 6 years. The patient was a retired construction worker. He had been in construction for the past 40 years. He was currently staying with his son and loved to ride bicycles and walk his dog.
The pain was first noticed 8 years ago having an insidious onset. The patient feels his long career as a construction worker has led to arthritis in his knees. His construction work involved bending, pushing, pulling, twisting, and lifting of heavy objects.
The patient describes the pain as moderate to severe in intensity. The pain was located in both the knees without any radiation. He described it as a dull ache that was precipitated to sharp upon activities such as climbing stairs, bending, kneeling or getting up from a chair after a long time.
He was using a cane as a walking aid and recently, was unable to perform even basic tasks such as doing his laundry without pain. He was even more distressed about the fact he was unable to play with his grandkids during their summer break.
He was a former smoker with a medical history of benign prostate hypertrophy, hypertension, and asthma. His medical conditions were all well controlled with medications. His surgical history included an appendectomy, laparoscopic hernia repair and right with ganglion cyst removal.
His physical examination revealed severe arthritis of the bilateral knees. There was mild swelling bilaterally with no rise in temperature or erythema. The overlying skin of bilateral knees was normal. There was tenderness on the medial joint line and patellar facet (right greater than left).
Genu varus deformity was present with a restricted range of motion due to pain (right – 0 to 95 degrees and left – 0 to 100 degrees). There was no coronal, sagittal or rotational plane instability or laxity. The distal neurological examination was normal bilateral. Distal lower extremity pulses were 2+ and palpable.
Examination of the right hip revealed tenderness along with the greater trochanteric suggesting bursitis. Bilateral ankle and bilateral hip examination were otherwise unremarkable. The patient denied any known drug allergies. He had previously tried conservative management in the form of physical therapy, cortisone injections, and gel Injections but without any sustained relief.
His imaging studies revealed severe tricompartmental osteoarthritis of the bilateral knee joint. After careful consideration of his medical conditions and needs, he was advised bilateral custom total knee replacement. He was made aware of the increased risk associated with bilateral surgery. Alternatives, risks, and benefits were discussed in detail with him and his son. They agreed for the procedure.

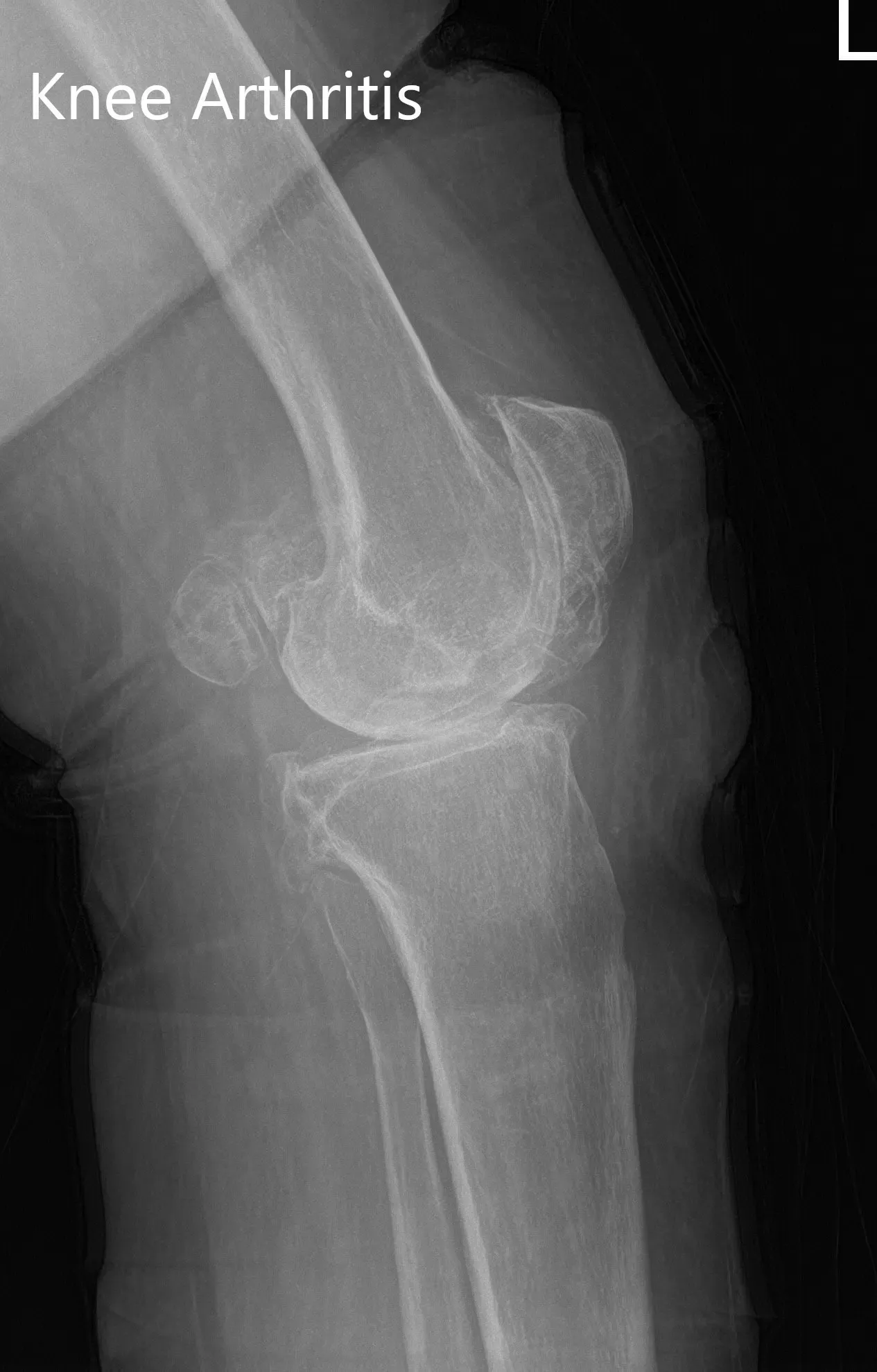
Preoperative X-ray of the left knee showing AP and lateral views
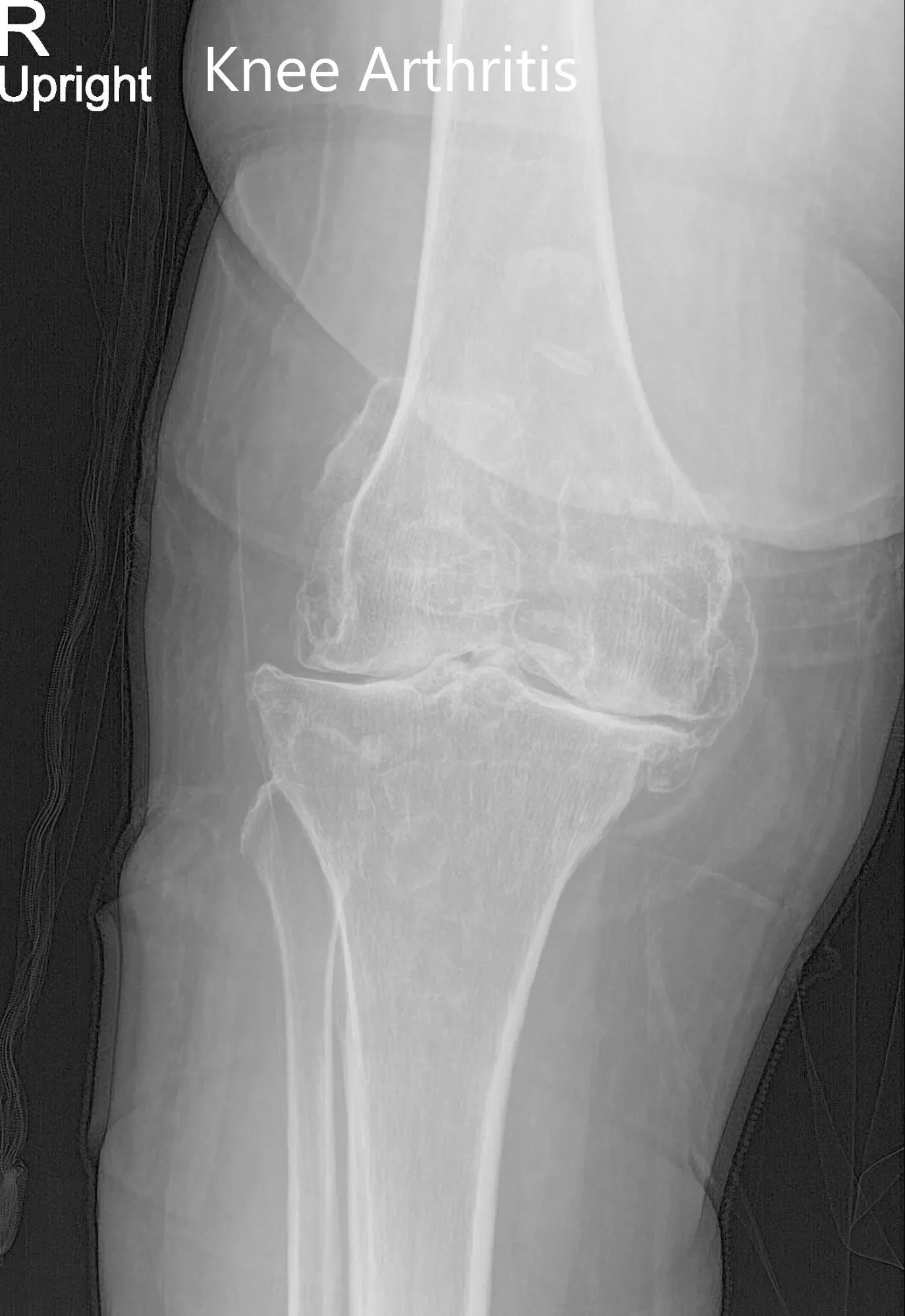
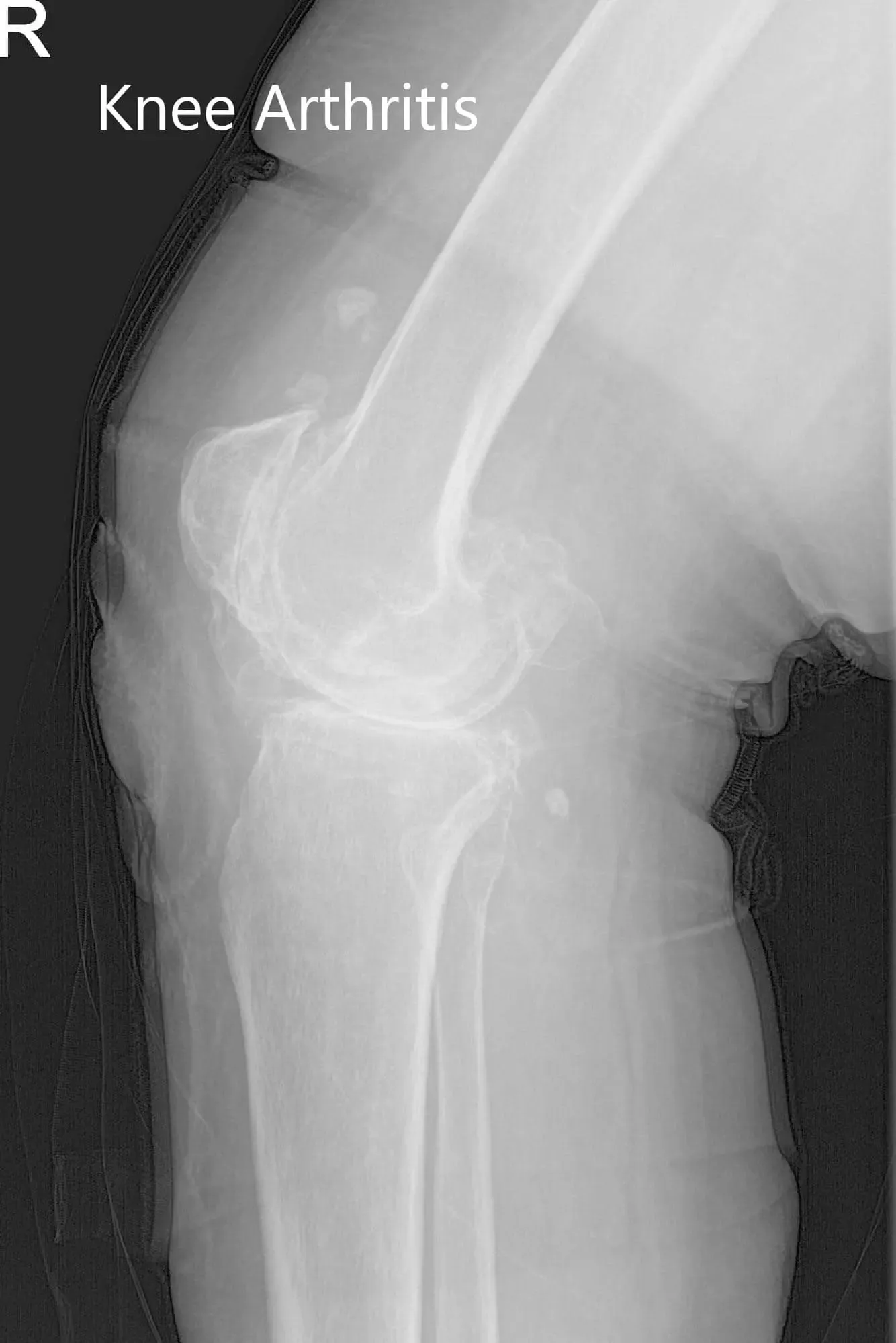
Preoperative X-ray of the right knee showing AP and lateral views
A preoperative CT scan of both the knees including hips and ankles was obtained. Scanogram images were utilized in preoperative planning of the correction of the mechanical axis. Patient-specific unique disposable jigs were 3D printed according to the patient’s anatomy. Custom implants were constructed which would replicate the natural joint with minimal bone cuts. A preoperative plan was made outlining the bone cuts and femoral offsets.


Preoperative merchant views of the bilateral patella showing severe osteoarthritis of the patellofemoral compartment.
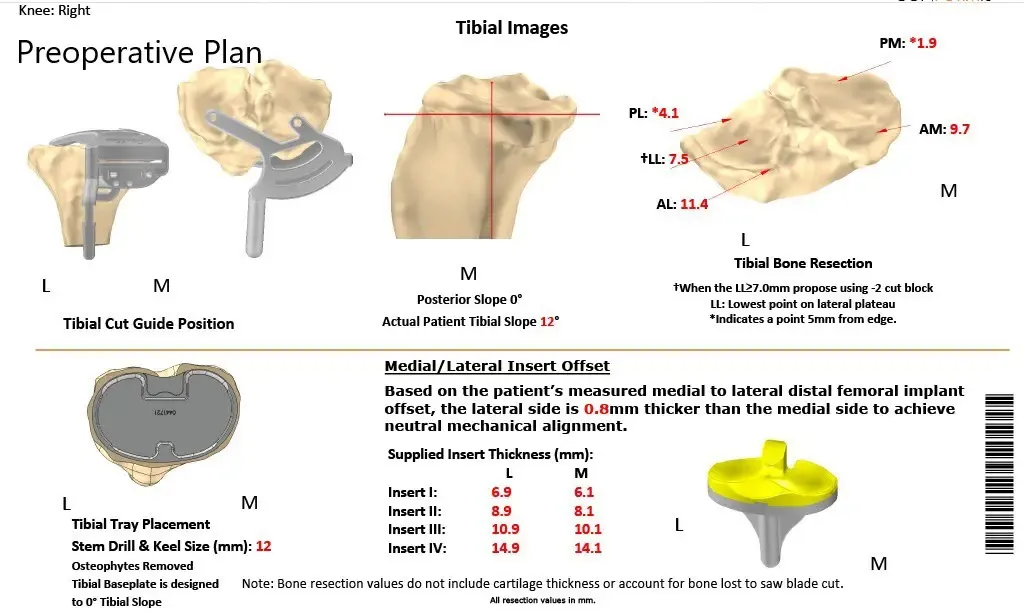
A patient-specific surgical plan for a patient at Complete Orthopedics in New York.
A patient-specific surgical plan for a patient at Complete Orthopedics in New York (scan 2)
A patient-specific surgical plan for a patient at Complete Orthopedics in New York (scan 3)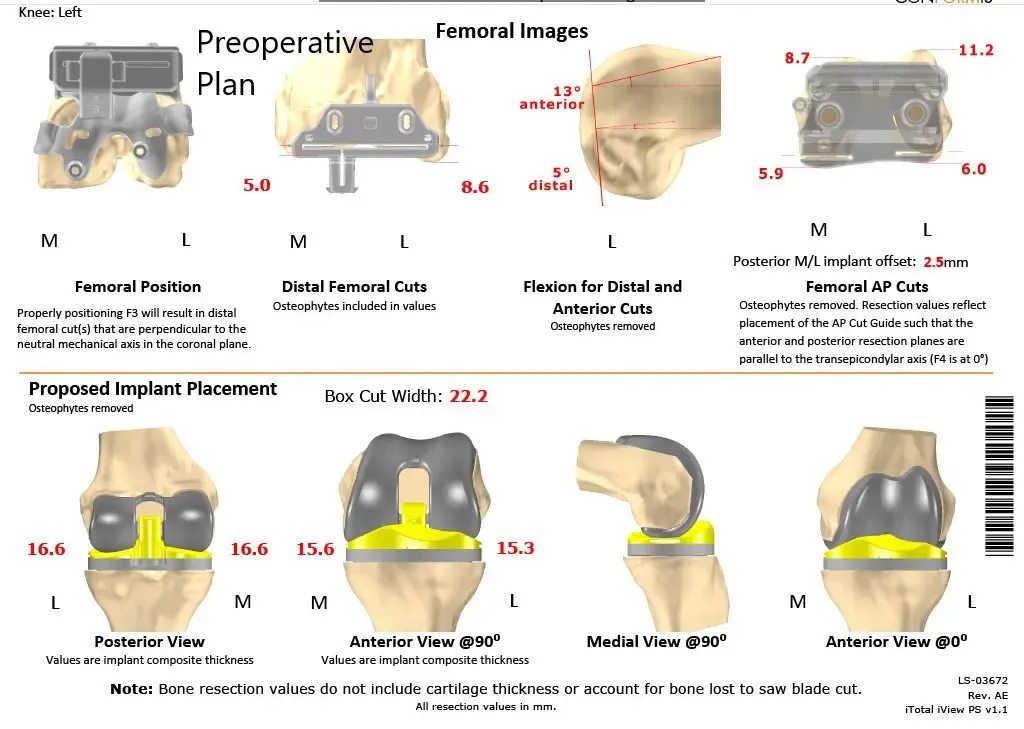
A patient-specific surgical plan for a patient at Complete Orthopedics in New York (scan 4)
IMPLANTS USED: Custom femur and tibia bilaterally, with 10 mm polyethylene bilaterally. Right 29 mm x 6 mm patella and left 32 mm x 6 mm patella.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room and anesthesia was obtained by the anesthesiologist. Risks, benefits, and alternatives were discussed with the patient prior to the procedure. The right knee was more painful than the left and it was decided to do the right knee before the left.
After draping and prepping bilateral lower extremities, the right lower extremity was then exsanguinated and the tourniquet was elevated. A straight incision was used for arthrotomy. Skin and subcutaneous tissues were incised. Medial parapatellar arthrotomy was performed.
The tibia was then exposed and the tibial cutting guide was then used for making the tibial resection. The tibial resection was made. The tibia was then prepared. Attention was then turned towards the femur. The femur was then prepared using the distal cutting guide for the distal cut.
The chamfer cuts were made using cutting guide and the notch cut was made using cutting guides. Laminar spreaders were used medially and laterally and the remainder of the meniscus and cruciates were then debrided. Posterior osteophytes were then removed.
Attention was then turned to the patella. The patellar resection was then performed. Drill holes were made in the patellar. The trial patella was placed in position. Trial femur was placed in position followed by the trial tibia and poly. The knee was then reduced. Patellar tracking was excellent. Full-extension was obtained. Full flexion was obtained. The stability was excellent.
The trial components were then removed. The injection was given. The femur was cemented into position followed by the tibia. Excess cement was removed. Poly was then placed into position and the knee was then reduced and held in full extension with a bump under the ankle. The patella was then cemented and excess cement was removed. The patella was held with the patellar clamp.
After the cement hardened, thorough lavage was given. Medial parapatellar arthrotomy was closed with Vicryl and V-Loc. Cutaneous tissues were closed with 0 Vicryl. Subcutaneous tissues were closed with 2-0 Vicryl. The skin was closed using staples. Sterile dressing was then applied over the wound.
After completion of the right knee, attention was then turned towards the left knee. After the tourniquet was deflated on the right side, the tourniquet on the left side was elevated after exsanguinating the extremity. A straight incision was used for the arthrotomy. Skin and subcutaneous tissues were incised.
Medial parapatellar arthrotomy was then performed. The tibial exposure was performed. The tibial resection was made using the tibial cutting jig.b The tibia was then prepared. Attention was then turned towards the femur. In the distal femur, the chamfer cuts and notch cuts were made using the cutting guides. Laminar spreaders were used medially and laterally. The remainder of the meniscus and the cruciates were then divided.
Osteophytes were then removed. The patellar resection was then performed. The drill holes were made in the patella. Trial patella was then placed into position followed by the trial femur, trial tibia, and poly. The knee was then reduced and trialed through a full range of motion. Full extension and full flexion were achieved. Patellar tracking was excellent.
Excellent stability was achieved. Trial components were then removed. The injection was given. The femur was cemented into position. Excess cement was removed. Tibia was cemented into position. Excess cement was removed. The patella was then placed into position. The knee was held in full extension with a bump under the ankle.
Patella was then cemented into positionExcess cement was removed. The patellar clamp was then placed in position and after the cement hardened, thorough lavage was given. Medial arthrotomy was closed with Ethibond and V-Loc. Cutaneous tissues were closed with 0 Vicryl. Subcuticular tissues were closed with 2-0 Vicryl. The skin was closed using staples.
Sterile dressing was then applied over the wound. The patient was then transferred to the postoperative care unit in stable condition.




Postoperative X-ray showing AP and lateral views of the right and the left knee joint
He was started on aspirin 325mg x 3 months for deep vein thrombosis prophylaxis. He was able to walk the same day of the procedure with support. The pain was controlled with medications. The patient was started on physical therapy for a range of motion and muscle strengthening. The staples were removed uneventfully. After 8 weeks follow up, the patient reported no pain with a full range of motion. He was happily back to his baseline activities. He was now happily able to play with his grandkids and ride his bicycle.


