A 62-year-old male presented for evaluation of his left knee. Over the last seven months, he has had increasing knee pain and discomfort. He stated that in April he got up from a seated position and felt a “crack” within his knee.
He had earlier seen another physician who diagnosed him with a torn meniscus. He underwent a surgical arthroscopy, and following the procedure, his pain increased in severity. He saw another physician in August and was treated with a gel injection. He still had persistent pain and discomfort diffusely about his left knee joint.
He stated that he also gets some swelling in the back of the knee. The pain was sharp with weight-bearing and activities. He got a buckling sensation, clicking and limited range of motion. He described pain with transfers, his walking tolerance was less than a block. He used a cane as an assistive device.
He negotiated stairs one at a time with the use of the banister. He was on Percocet as well as Mobic. He also had a prior right total knee replacement a few years ago. He developed an infection three years after the procedure and underwent a two-staged revision with final reimplantation by an outside physician.
Currently, the right knee was minimally symptomatic, but he did develop a postoperative DVT (deep vein thrombosis) and pulmonary embolism requiring placement of an inferior vena cava filter three years ago. He had been on Coumadin therapy which was recently discontinued by her vascular surgeon. He had a history of low back pain and was going to pain management.
He was a retired school bus driver and currently lives with his wife. The patient was dismayed with the left knee pain and limited mobility secondary to pain. He was unable to do even basic tasks without pain and was apprehensive about climbing stairs. He was exploring the possibility of total knee replacement.
He was a past smoker having quit 30 years ago. Earlier he also had a trial of conservative management in the form of physical therapy and gel injections with minimal relief. He had a known drug allergy to Biaxin.
On his office visit, he was calm, conscious, cooperative and well oriented to time place and person. He walked with an antalgic gait with a reduced stance phase on the left side. The skin overlying the left skin demonstrated a well-healed scar suggestive of prior arthroscopic surgery.
There was mild swelling in the left knee. Pain and crepitus were present throughout the arch of motion. The range of movements was present from 10 degrees to 90 degrees. There was tenderness on the medial and lateral joint lines. Tenderness was also present on patellar facets.
There was mild genu varum deformity. There were no signs of instability or laxity in coronal, sagittal, and axial planes. The examination of the right knee revealed a well-healed anterior scar. The range of motion was full with no pain or stiffness.
The examination of the bilateral hip and ankle was normal. The neurological examination of the lower extremities was normal. The bulk and tone of both lower limbs were normal. The bilateral lower extremity pulses were palpable and comparable.
Imaging revealed severe tricompartmental osteoarthritis of the left knee with joint space reduction and osteophytes.
Considering the lifestyle limiting left knee pain, the patient was advised left knee total replacement. Risks, benefits, and alternatives were discussed with the patient at length. He agreed to undergo left total knee arthroplasty.
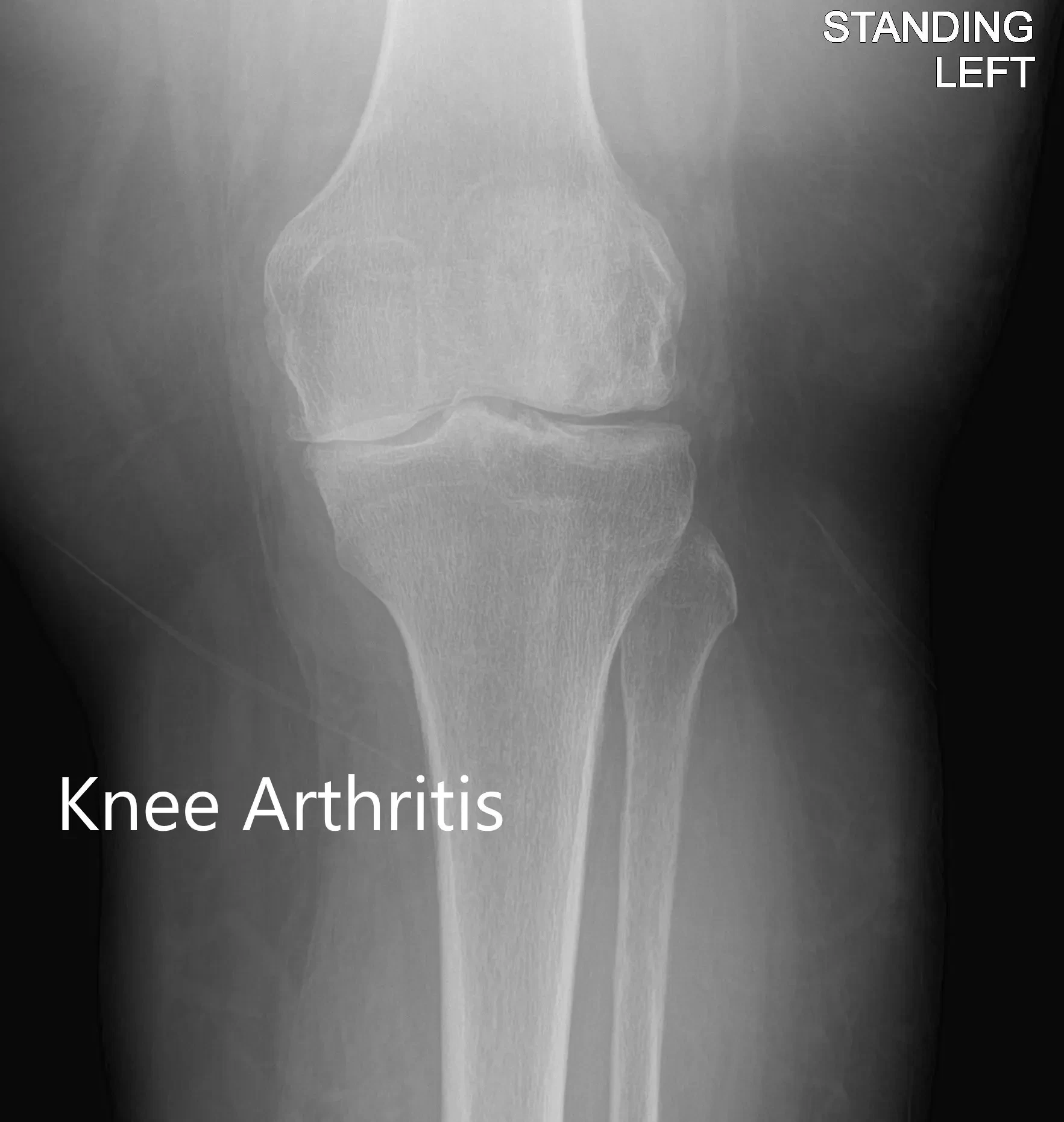
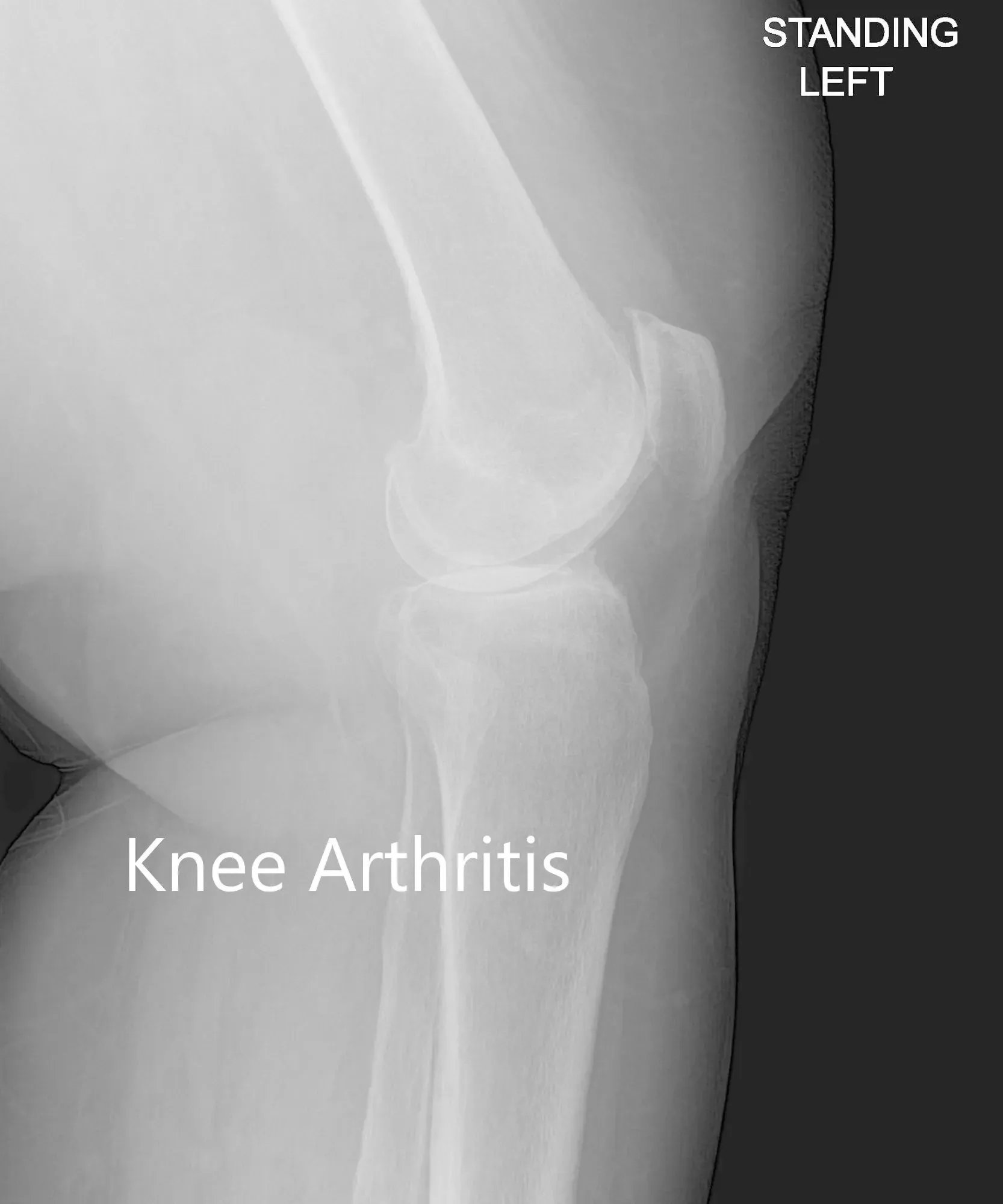
Anteroposterior and lateral view of the left knee
OPERATION: Left total knee replacement.
IMPLANTS USED: Posterior stabilized 8 left standard femoral component left-sided with tibia E left cemented with 14 x 30 stem with poly 16 mm with a 29-mm diameter poly patella.
DESCRIPTION OF PROCEDURE: The patient was brought to the operating room after obtaining informed consent, signing the correct surgical site. The risks, benefits, and alternatives were extensively discussed with the patient prior to the procedure.
The patient, as well as the family, understood that he had increased risk of complications including, but not limited to infection and deep vein thrombosis and pulmonary embolism.
Anesthesia was obtained by the anesthesiologist. The patient was then definitely positioned, and the left knee was then draped and prepped in the usual sterile manner. A straight incision centered over the patella was used for the arthrotomy.
Skin and subcutaneous tissues were then incised. A medial parapatellar arthrotomy was then performed. The knee was then exposed and the femoral cutting guide was then placed into position. The distal cut was then performed. The anterior, posterior, and then the chamfer cuts were then performed.
Attention was then turned towards the tibia. The tibial cut was then performed. Lamina spreaders were used medially and laterally, and the remainder of the meniscus was then debrided. The notch cut was then performed and the femur was then placed into position followed by the tibia.
The tibia was then broached and the trial poly was then placed into position. The gap balancing was performed before the final broaching and was found to be correct. The patella was then resected. The drill holes were made in the patella and then the trial patella was then placed into position.
The knee was then reduced. The knee was then ranged through a full range of motion and the patellar tracking was found to be normal, and the gap balancing was then again checked and was found to be satisfactory.
The trial components were then removed. Thorough lavage was given. The femur was cemented into position. Excess cement was then removed. The tibia was then cemented into position. Excess cement was then removed. Poly was then placed over the tibia. The knee was then reduced.
The knee was then held in full extension and then the patella was cemented into position and held in position with a patellar clamp. The excess cement was removed after the cement hardened. The knee was injected with intraarticular injection and thorough lavage was given.
Medial parapatellar arthrotomy was closed with Ethibond, cutaneous tissues were closed with 0 Vicryl, subcuticular tissues were closed with 2-0 Vicryl, and skin was closed using staples. Sterile dressing was then applied, and the patient was then transferred to the postoperative care unit in stable condition.
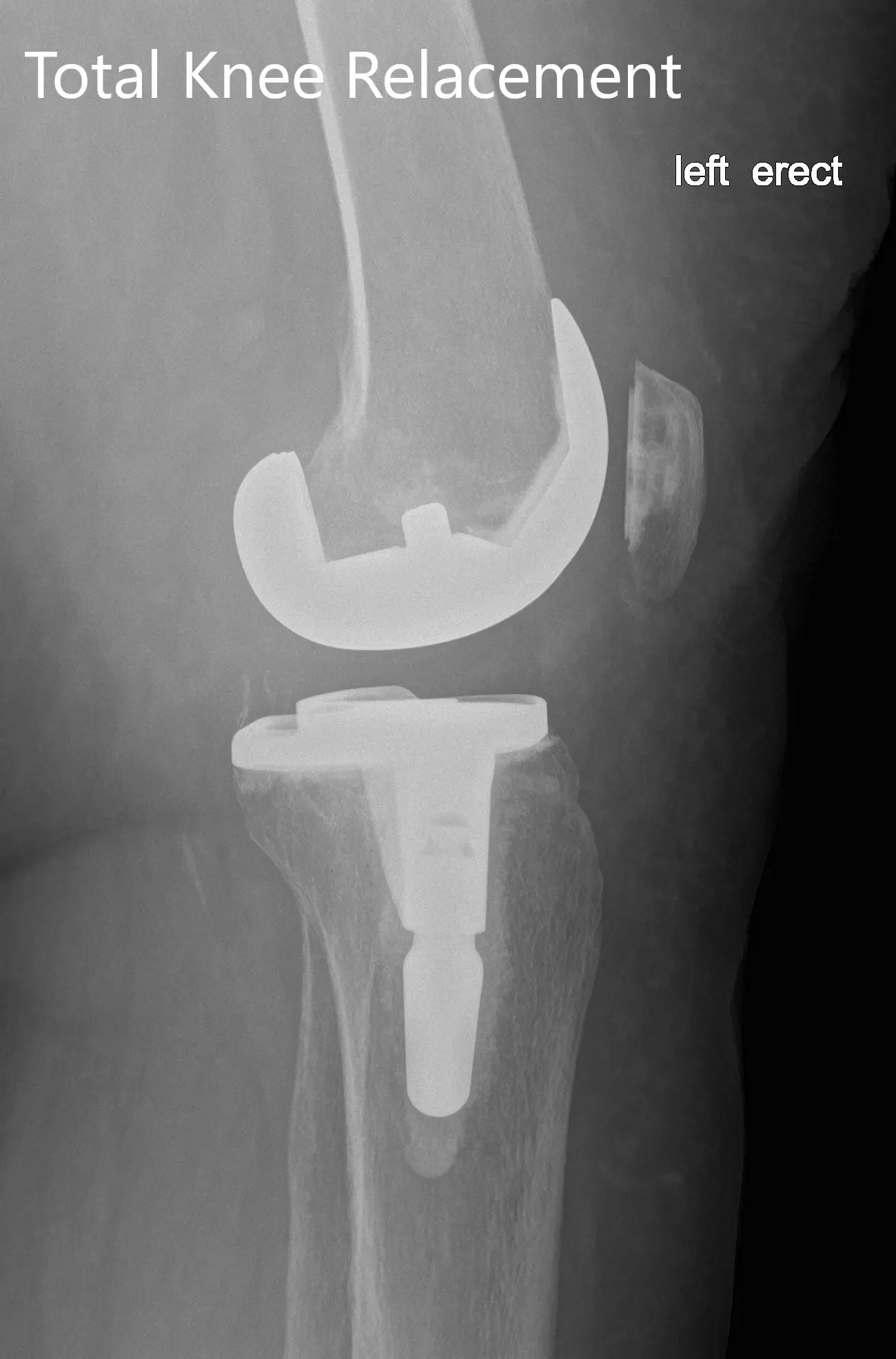
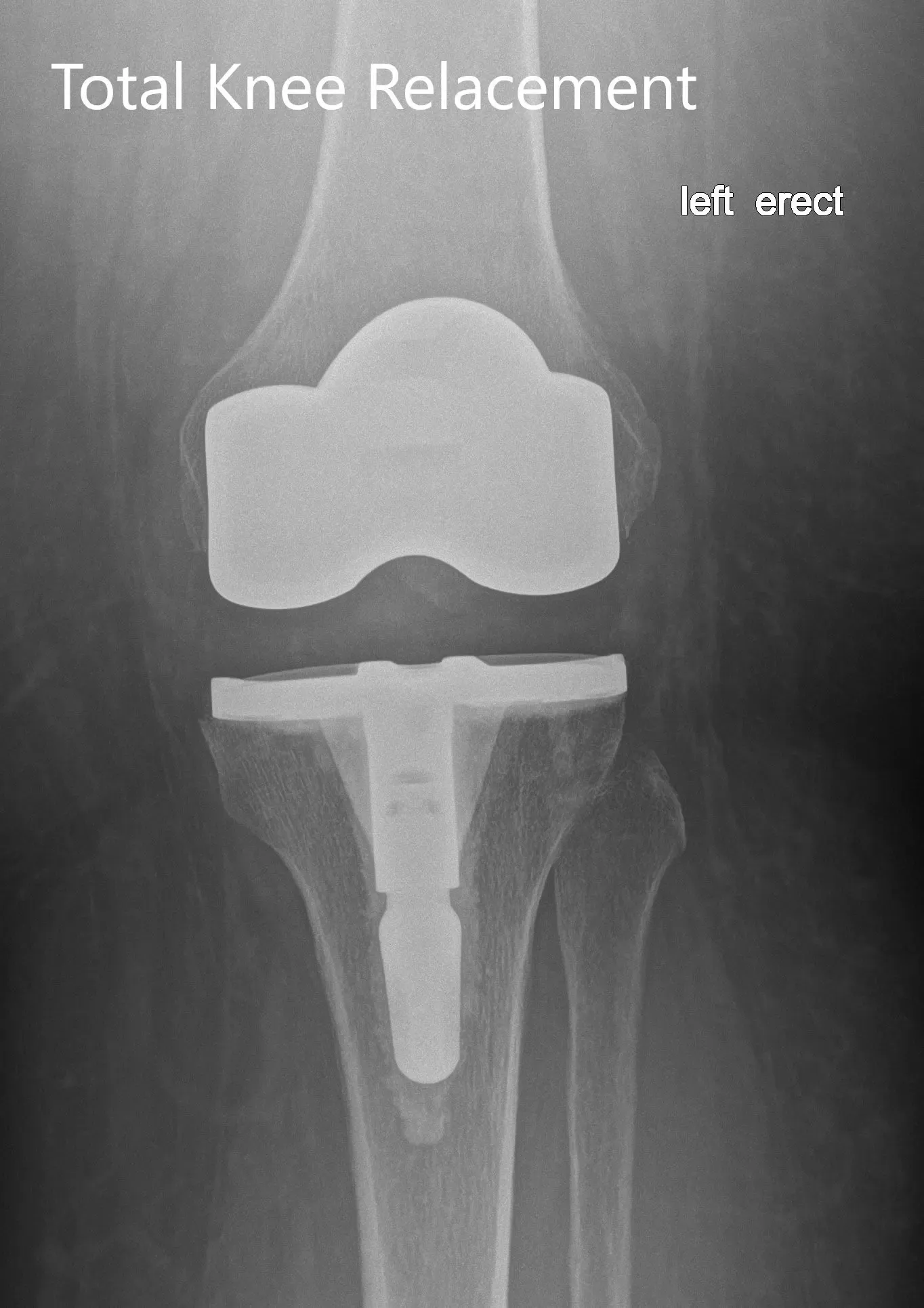
Postoperative X-ray of the left showing the anteroposterior and lateral view with total knee prosthesis in position
The patient had an excellent recovery post-op, his pain was managed well with medications. He was started on Aspirin 325 mg BID for deep vein thrombosis prophylaxis. He was able to walk 100 feet on the same day of the procedure. He was discharged the following day.
The sutures were taken off 14th-day post-op with no complications. There was no swelling of the calves and no neurological deficit of the lower extremities. The patient underwent physical therapy to strengthen muscles and increase range of motion of the joint.
Three months post-op, the patient was able to walk with no pain and a full range of motion. He was extremely happy with the outcome of the procedure and was back to his baseline activities.
Disclaimer – Patient’s name, age, sex, dates, events have been changed or modified to protect patient privacy.


