Shin splints, or medial tibial stress syndrome, are a common injury, particularly among athletes who engage in running and jumping. This condition causes pain along the inner edge of the shinbone (tibia) and typically results from repetitive stress that exceeds the body’s capacity to repair and strengthen the bone and surrounding tissues. At Complete Orthopedics, we focus on diagnosing and managing shin splints with both conservative and, when necessary, surgical treatments.
How Common It Is and Who Gets It? (Epidemiology)
Shin splints are common among athletes, especially runners, dancers, and military recruits who engage in high-impact physical activities. The condition frequently affects people who suddenly increase their physical activity, particularly runners who may experience shin pain after upping their running distance or intensity. Those with flat feet or improper footwear are also at higher risk.
Why It Happens – Causes (Etiology and Pathophysiology)
Shin splints are caused by repetitive stress on the shinbone, often resulting from overuse. The periosteum, a tough tissue that covers the shinbone, becomes inflamed due to the strain placed on the muscles and tendons attached to the bone. Common contributing factors include sudden increases in activity, running on hard surfaces, improper footwear, and pre-existing conditions like flat feet or weakened arches.
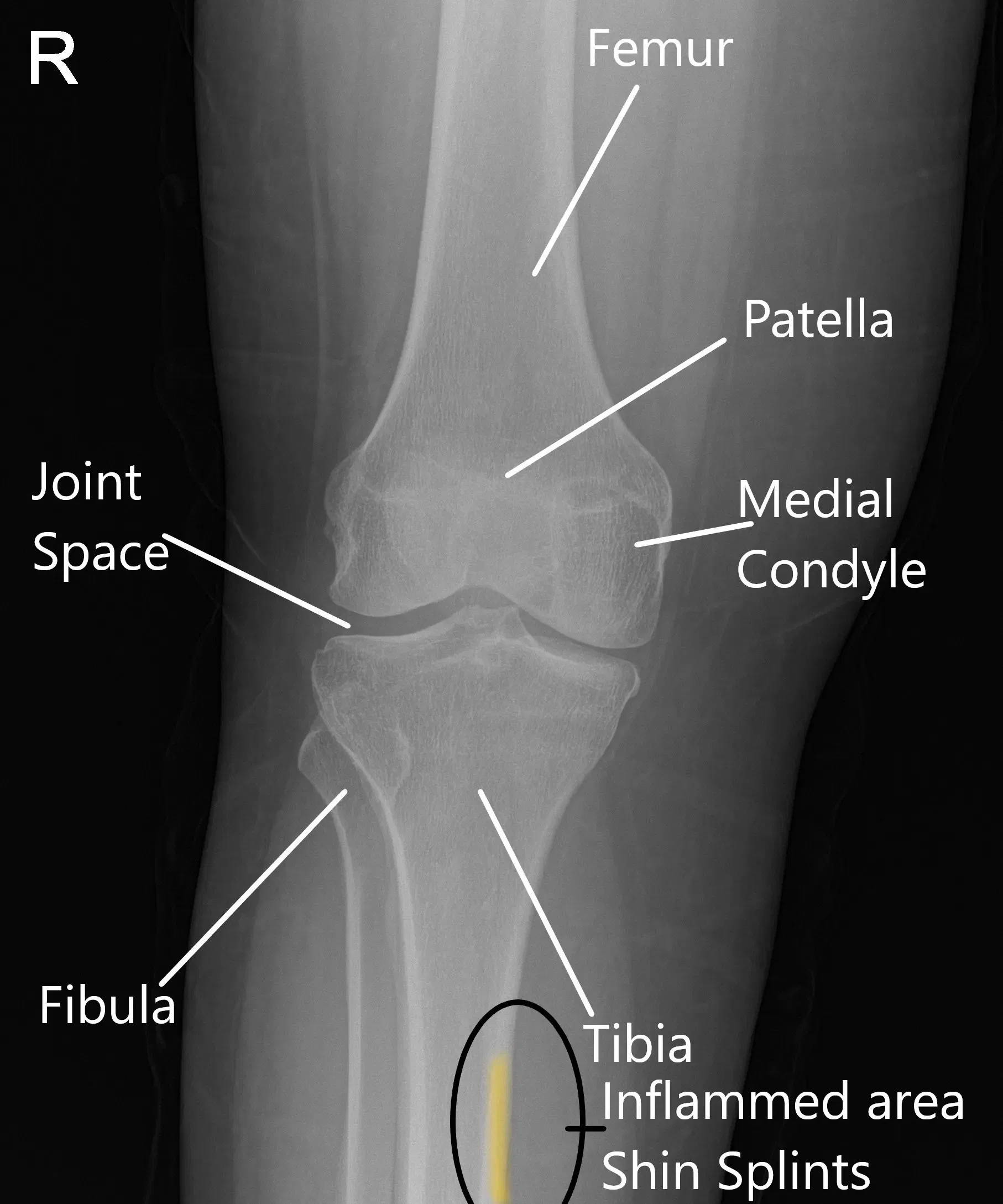
X-ray of a normal knee showing the area of inflammation in shin splints.
How the Body Part Normally Works? (Relevant Anatomy)
The tibia, or shinbone, is the long bone in the lower leg. It is surrounded by muscles, tendons, and the periosteum. The periosteum helps to protect and nourish the bone, while muscles like the calf muscles and the tibialis anterior are responsible for movement. During activities like running or jumping, these muscles contract and apply force to the shinbone. If the muscles and tendons are overstressed, it can lead to inflammation and pain along the inner edge of the tibia.
What You Might Feel – Symptoms (Clinical Presentation)
The main symptom of shin splints is pain along the inner side of the shinbone. This pain may start as a dull ache and intensify to sharp pain, often associated with mild swelling. The pain typically worsens during activity, especially activities that involve bending the knee or high-impact motions such as running or jumping. Rest usually alleviates the pain, but over time, the discomfort can become more persistent and intense.
How Doctors Find the Problem? (Diagnosis and Imaging)
The diagnosis of shin splints begins with a detailed history of physical activity, including any changes in training intensity or volume. A physical examination focuses on tenderness along the inner part of the shinbone, and the doctor may assess the alignment of the feet and legs to identify any contributing factors. X-rays are often used to rule out stress fractures, while MRI or bone scans may be requested if the physician suspects a more serious underlying condition.
Classification
Shin splints can be classified by severity:
- Grade 1: Mild discomfort with activity, typically relieved with rest.
- Grade 2: More significant pain during activity that may persist for a longer period.
- Grade 3: Severe pain that limits participation in physical activities, often requiring more intensive treatment.
Other Problems That Can Feel Similar (Differential Diagnosis)
Conditions that may present with symptoms similar to shin splints include:
- Stress fractures: Small, hairline fractures caused by overuse, typically diagnosed with MRI or bone scan.
- Tendonitis: Inflammation of the tendons, which may mimic shin splints but is localized to the tendons themselves.
- Chronic compartment syndrome: A rare condition involving increased pressure within the muscle compartments of the leg.
Treatment Options
Non-Surgical Care
Most cases of shin splints can be managed with conservative treatments:
- Rest: Avoiding activities that stress the shin and allow the inflammation to subside.
- Ice and Compression: Applying ice packs to reduce swelling and using compression bandages for support.
- Medications: NSAIDs like ibuprofen or naproxen help manage pain and inflammation.
- Physical Therapy: Stretching and strengthening exercises to improve flexibility and muscle balance around the knee, ankle, and foot.
- Proper Footwear: Wearing shoes with proper arch support or using orthotics, especially for those with flat feet.
Surgical Care
Surgery is typically only considered if conservative measures fail to relieve symptoms, or if a stress fracture is present. In rare cases, surgical intervention may involve addressing any underlying tendonitis or other anatomical issues contributing to the condition.
Recovery and What to Expect After Treatment
Recovery from shin splints varies depending on the severity of the injury:
- Rest and Rehab: Most patients recover with a period of rest, followed by a rehabilitation program designed to restore strength and flexibility to the muscles and tendons.
- Gradual Return to Activity: Once pain subsides, it is important to gradually return to physical activity to avoid re-injury. Cross-training with lower-impact activities such as swimming or cycling can help maintain fitness while avoiding stress on the shin.
- Rehabilitation: Physical therapy may continue for several weeks to ensure full recovery and to prevent recurrence.
Possible Risks or Side Effects (Complications)
Without appropriate management, shin splints can lead to more severe conditions, such as stress fractures or chronic tendonitis. Overuse and continued high-impact activity without sufficient recovery can also cause the pain to become chronic, limiting participation in sports or daily activities.
Long-Term Outlook (Prognosis)
Most people recover fully from shin splints with proper management. The prognosis is generally excellent if the condition is treated early and conservative measures are followed. Athletes who maintain good training habits and focus on muscle strengthening and proper footwear are less likely to experience recurrence.
Out-of-Pocket Costs
Medicare
CPT Code 27600 – Fasciotomy / Compartment Release: $95.07
CPT Code 27601 – Fasciotomy / Compartment Release (if bilateral): $103.87
CPT Code 27752 – Tibial Stress Fracture ORIF (if present): $129.62
CPT Code 27680 – Tendon Debridement/Repair (if associated tendonitis): $99.83
CPT Code 27681 – Tendon Debridement/Repair (if associated tendonitis, if bilateral): $120.36
Under Medicare, 80% of the approved amount for these procedures is covered once the annual deductible has been met. The remaining 20% is typically the patient’s responsibility. Supplemental insurance plans—such as Medigap, AARP, or Blue Cross Blue Shield—generally cover this 20%, leaving most patients with little to no out-of-pocket expenses for Medicare-approved surgeries. These supplemental plans work directly with Medicare to ensure full coverage for the procedures.
If you have secondary insurance—such as Employer-Based coverage, TRICARE, or Veterans Health Administration (VHA)—it functions as a secondary payer once Medicare processes the claim. After your deductible is satisfied, these secondary plans may cover any remaining balance, including coinsurance or small residual charges. Secondary plans typically have a modest deductible, ranging from $100 to $300, depending on the specific policy and network status.
Workers’ Compensation
If your fasciotomy, tibial stress fracture ORIF, or tendon surgery is work-related, Workers’ Compensation will fully cover all treatment-related costs, including surgery, hospitalization, and rehabilitation. You will have no out-of-pocket expenses under an accepted Workers’ Compensation claim.
No-Fault Insurance
If your leg or tendon injury resulting in surgery is caused by a motor vehicle accident, No-Fault Insurance will cover all medical and surgical expenses, including the procedures listed. The only possible out-of-pocket cost may be a small deductible depending on your individual policy terms.
Example
Michael, a 50-year-old patient with a tibial stress fracture and associated tendonitis, underwent tibial stress fracture ORIF (CPT 27752) and tendon debridement/repair (CPT 27680). His estimated Medicare out-of-pocket costs were $129.62 for the ORIF and $99.83 for the tendon debridement. Since Michael had supplemental insurance through Blue Cross Blue Shield, the 20% that Medicare did not cover was fully paid, leaving him with no out-of-pocket expenses for the surgeries.
Frequently Asked Questions (FAQ)
Q. What causes shin splints?
A. Shin splints are caused by repetitive stress on the shinbone, often due to sudden increases in activity, improper footwear, or muscle imbalances.
Q. Can shin splints be prevented?
A. Yes, preventing shin splints involves gradual increases in physical activity, wearing proper footwear, using orthotics for flat feet, and incorporating strength training exercises.
Q. How long does it take to recover from shin splints?
A. Recovery time can vary, but most people recover within 2-6 weeks with rest, ice, and rehabilitation exercises. More severe cases may require longer recovery periods.
Q. Can I continue to exercise with shin splints?
A. It’s important to avoid high-impact activities that stress the shin, but low-impact exercises like swimming or cycling can help maintain fitness without exacerbating the condition.
Q. Is surgery necessary for shin splints?
A. Surgery is rarely required for shin splints. Most cases resolve with conservative treatments like rest, physical therapy, and proper footwear.
Summary and Takeaway
Shin splints are a common condition, especially for athletes, caused by repetitive stress on the shinbone. The condition is typically manageable with rest, ice, and rehabilitation. Preventive measures such as proper footwear, strength training, and gradual increases in activity can help reduce the risk of developing shin splints. Most individuals recover fully with appropriate care, but persistent cases may require further intervention.
Clinical Insight & Recent Findings
A recent study explored the misdiagnosis of medial tibial stress syndrome (shin splints) in a patient who had been suffering from chronic anteromedial shin pain for years.
The investigation revealed that the underlying issue was not shin splints but a mixed neuropathy of the L4 spinal nerve due to dynamic stenosis of the L4-5 intervertebral foramen. Despite extensive treatments aimed at shin splints, the pain persisted until the correct diagnosis was made through detailed sensory testing and imaging.
After spinal manipulation therapy targeting the L4-5 foramen, the patient’s symptoms resolved, highlighting the importance of considering peripheral nerve involvement in cases of persistent shin pain that do not respond to standard shin splint treatments (“Study of partial mixed neuropathy of the fourth lumbar spinal nerve – See PubMed“).
Who Performs This Treatment? (Specialists and Team Involved)
Orthopedic surgeons and sports medicine specialists typically manage shin splints. A rehabilitation team, including physical therapists, may also be involved in the recovery process.
When to See a Specialist?
You should consult a specialist if your shin pain persists despite rest and self-care treatments or if the pain interferes with your ability to perform daily activities.
When to Go to the Emergency Room?
Go to the emergency room if you experience severe pain, swelling, or bruising in the lower leg, especially if there is concern for a stress fracture or other serious injury.
What Recovery Really Looks Like?
Recovery from shin splints typically involves rest, physical therapy, and gradual return to activity. Most individuals resume normal activities after a few weeks to months, depending on the severity of the condition.
What Happens If You Ignore It?
Ignoring shin splints can lead to more severe injuries, such as stress fractures or chronic pain, which may require more invasive treatments. Early intervention is key to preventing long-term complications.
How to Prevent It?
Prevent shin splints by gradually increasing physical activity, strengthening the muscles around the shin, wearing proper footwear, and using orthotics if necessary. Regular stretching and cross-training can also help maintain balance and prevent overuse injuries.
Nutrition and Bone or Joint Health
Maintaining a healthy diet rich in calcium and vitamin D can support bone health and help prevent injuries like shin splints. Proper nutrition also aids in muscle recovery and joint function.
Activity and Lifestyle Modifications
Engage in low-impact activities such as swimming or cycling during recovery, and be mindful of gradual increases in activity levels. Proper warm-up and cool-down exercises are essential to prevent overuse injuries.
Do you have more questions?
What exactly causes the pain in shin splints?
The pain in shin splints is caused by inflammation of the muscles, tendons, and the thin layer of tissue covering the shinbone due to overuse or stress.
How can I differentiate shin splint pain from other leg pains?
Shin splint pain is typically localized along the inner edge of the shinbone, is exacerbated by physical activity, and improves with rest. Other leg pains might not follow this pattern and could be due to different causes.
Is it safe to keep running if I think I have shin splints?
It is not safe to continue running with shin splints as it can lead to worsening of the symptoms or more serious injuries. Rest and treatment are recommended.
Are there specific stretching exercises that prevent shin splints?
Specific stretching exercises targeting the calf muscles, like standing calf stretches and seated shin stretches, can help prevent shin splints.
How long do shin splints typically last?
The duration of shin splints varies but typically resolves with proper rest and treatment within a few weeks to a couple of months.
Can shin splints lead to permanent damage?
While shin splints themselves do not cause permanent damage, neglecting them can lead to more severe conditions like stress fractures.
What are the best types of footwear to prevent shin splints?
Footwear that provides good arch support, cushioning, and fits well is best for preventing shin splints.
How effective are orthotic devices in treating shin splints?
Orthotic devices can be effective in treating shin splints, especially for individuals with biomechanical issues like flat feet.
Are children at risk for shin splints?
Children, particularly those in sports involving running and jumping, can develop shin splints, though it’s less common than in adults.
What role does diet play in the prevention and management of shin splints?
A balanced diet rich in calcium and vitamin D can support bone health and may help in the management and prevention of shin splints.
Can shin splints recur after they have healed?
Yes, shin splints can recur if preventive measures are not followed or if there is a return to high-impact activities too quickly.
Are there any alternative therapies for shin splints?
Alternative therapies like acupuncture, massage therapy, and the use of compression sleeves may provide relief for some individuals
How do I know if my shin splints have healed enough to resume activity?
Resumption of activity should be gradual after the pain has completely subsided and with no signs of swelling.
What is the best way to apply ice to shin splints?
Ice should be applied in a cloth-covered pack to the affected area for 15-20 minutes every two to three hours during the initial days after symptoms appear.
Is there a correlation between shin splints and flat feet?
There is a strong correlation between flat feet and shin splints due to the increased stress on the lower leg muscles and tendons.
How can I adjust my running technique to avoid shin splints?
Adjusting your running technique to include shorter strides and ensuring your foot strikes below your hips can help avoid shin splints.
Are there any specific medications recommended for shin splints?
Over-the-counter anti-inflammatory medications, such as ibuprofen or aspirin, can be used to reduce pain and inflammation.
Can shin splints be completely cured?
With appropriate treatment and preventive strategies, shin splints can usually be completely resolved.
What preventive measures can be taken during high-impact sports?
Wearing appropriate footwear, ensuring proper technique, and maintaining astrength training in your routine can all help prevent shin splints during high-impact sports.
How often should I replace my running shoes to prevent shin splints?
Running shoes should be replaced every 300-500 miles to ensure adequate cushioning and support, reducing the risk of shin splints.
Can walking cause shin splints as well as running?
While less common, walking—especially if excessive or on hard surfaces—can also lead to shin splints, particularly if footwear is inadequate.
Are shin splints a sign of a more serious condition?
Generally, shin splints are not a sign of a more serious condition, but if left untreated, they can lead to complications like stress fractures.
How does body weight impact the recovery from shin splints?
Higher body weight can extend recovery time as more stress is placed on the shins during recovery, necessitating more cautious management.
What are the signs that I should seek professional help for shin splints
You should seek professional help if the pain persists despite rest and self-care, if there is severe swelling, or if you suspect a fracture.


